Preoperative Assessment & Goals - Brainy Prep Work
- Neurological Status: Baseline GCS, focal deficits, seizure history/control.
- ICP Assessment: Signs of ↑ICP (headache, N/V, papilledema). Cushing's triad (late).
- Airway: Standard assessment; consider difficult airway with ↑ICP or cervical spine issues.
- Systemic Review: CV (HTN, IHD), Respiratory (pulmonary edema risk), Renal function.
- Medications: Continue anticonvulsants. Steroids (e.g., dexamethasone). Manage anticoagulants/antiplatelets.
- Investigations: Recent MRI/CT. Baseline bloods (FBC, U&E, Coags).
- Anesthetic Goals:
- Maintain CPP ($CPP = MAP - ICP$; use CVP if higher). Target >60-70 mmHg.
- Control ICP (target <20 mmHg).
- Smooth induction & emergence.
- Rapid recovery for neuro assessment.
⭐ Patients on long-term phenytoin may exhibit resistance to non-depolarizing muscle relaxants due to enzyme induction.
Induction & Neuromonitoring - Setting the Stage
- Primary Goals:
- Maintain hemodynamic stability (MAP within 20% of baseline).
- Control ICP (target < 20 mmHg).
- Ensure adequate CPP (target 60-70 mmHg; $CPP = MAP - ICP$).
- Induction Protocol:
- Airway & Positioning: Head up 15-30° (promotes venous drainage), neutral neck.
- Essential Monitoring:
- Standard ASA (ECG, NIBP, SpO2, EtCO2, Temp).
- Invasive Arterial BP (A-line): For continuous MAP & ABGs.
- Neuromuscular monitoring (TOF).
- Consider: CVP, EEG/BIS, SSEP/MEP if eloquent areas involved.
⭐ Rapid Sequence Intubation (RSI) is generally avoided due to risk of ICP spike with succinylcholine; a modified rapid sequence with rocuronium is preferred if aspiration risk is high.
Intraoperative Anesthetic Management - Skull Session Secrets
- Brain Relaxation:
- Head elevation: 15-30°.
- Hyperventilation: PaCO₂ 30-35 mmHg.
- Osmotic diuretics: Mannitol (0.25-1 g/kg) or Hypertonic Saline (HTS).
- Loop diuretics: Furosemide (0.5-1 mg/kg).
- CSF drainage (if available).
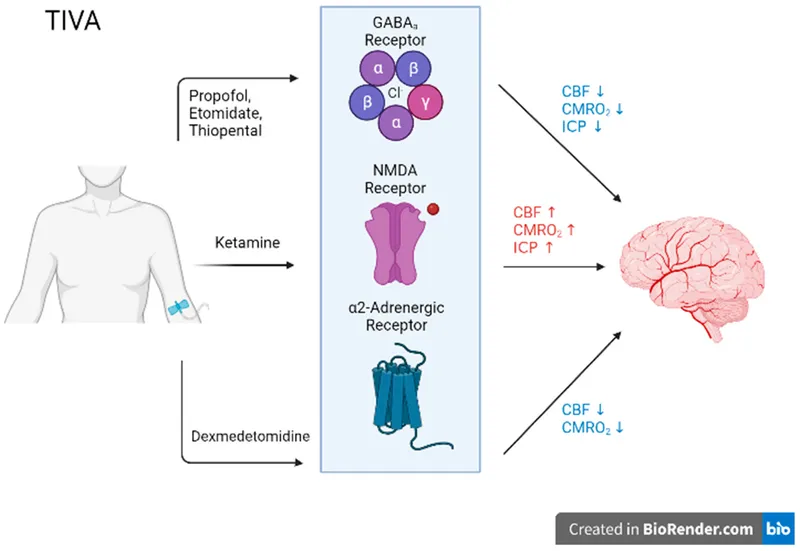
- Anesthetic Choice:
- TIVA (Propofol + Remifentanil) favored: ↓ICP, rapid emergence.
- Volatiles: Maintain <1 MAC if used.
- Hemodynamic Goals:
- Maintain Mean Arterial Pressure (MAP) within 20% of baseline.
- Cerebral Perfusion Pressure (CPP) >60-70 mmHg.
- Fluid Management:
- Isotonic crystalloids (Normal Saline preferred). Avoid hypotonic & glucose solutions.
- ⚠️ Key Complications & Management:
- Venous Air Embolism (VAE): Sudden ↓ETCO₂, ↓SpO₂, hypotension. Mgmt: Notify surgeon, flood field with saline, 100% O₂, aspirate from CVC, left lateral decubitus (Durant's maneuver).
- Intraoperative Seizures: Propofol, thiopental, levetiracetam.
⭐ During craniotomy, a sudden decrease in End-Tidal CO₂ (ETCO₂) accompanied by hypotension should immediately raise suspicion for Venous Air Embolism (VAE).
Emergence & Postoperative Care - Waking Up Well
- Goal: Smooth emergence, stable hemodynamics, early neuro-assessment.
- Smooth Emergence Strategies:
- Lidocaine IV (1-1.5 mg/kg) or LTA.
- Short-acting opioids (e.g., remifentanil, fentanyl).
- Dexmedetomidine infusion.
- Avoid $N_2O$ at closure (prevents pneumocephalus expansion).
- Extubation Criteria: Awake, follows commands, adequate ventilation (TOF > 0.9).
- Immediate Postoperative Care (PACU/Neuro-ICU):
- Frequent neurological checks (GCS, pupils, motor function).
- Strict BP control (e.g., SBP < 140-160 mmHg, avoid hypotension).
- Multimodal analgesia (paracetamol, opioids; NSAIDs with caution).
- Antiemetics (e.g., ondansetron).
- Maintain normothermia, normocapnia, normoglycemia.
- Key Complications to Monitor: Hematoma, seizures, ↑ICP, PONV, delayed awakening.
⭐ Delayed emergence or neurological deterioration post-craniotomy mandates urgent CT scan to exclude intracranial hematoma or acute hydrocephalus.
High‑Yield Points - ⚡ Biggest Takeaways
- ICP management is crucial: target PaCO2 30-35 mmHg, mannitol, and consider CSF drainage.
- Maintain Cerebral Perfusion Pressure (CPP) at 60-70 mmHg by optimizing MAP and ICP.
- Anesthetic choices: TIVA or volatile agents (<1 MAC); strictly avoid Nitrous Oxide.
- Ensure smooth emergence to prevent coughing, straining, and subsequent ICP elevation.
- Key complications: Venous Air Embolism (VAE), seizures, and intracranial hematoma.
- Preoperative: assess neurological deficits, ICP signs, and steroid/anticonvulsant use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

