Neuroanesthesia

On this page
🧠 Neuroanesthesia: The Brain's Guardian Protocol
Neuroanesthesia demands you master a paradox: your drugs must render the brain unconscious while simultaneously protecting its fragile perfusion, metabolism, and structure during surgery. You'll learn how cerebral blood flow responds to anesthetic agents, why positioning can catastrophically alter intracranial pressure, and how to monitor a patient whose neurological exam you've deliberately abolished. This lesson builds your framework for managing the body's most unforgiving organ-where small missteps cascade into irreversible damage, and where vigilance from induction through emergence separates excellent outcomes from disaster.
Neuroanesthesia represents the pinnacle of perioperative medicine, where anesthetic decisions directly influence cerebral perfusion pressure, intracranial pressure dynamics, and neurological outcomes. Every drug choice, every ventilation parameter, and every hemodynamic adjustment reverberates through the brain's delicate physiology.
📌 Remember: BRAIN for neuroanesthesia priorities - Blood pressure control, Respiratory management, Anesthetic depth, ICP monitoring, Neurological assessment
The neuroanesthetic approach fundamentally differs from general anesthesia through its focus on cerebral protection, rapid emergence, and immediate neurological assessment. Understanding these principles unlocks the logic behind every neuroanesthetic decision.
⭐ Clinical Pearl: Neuroanesthesia maintains CPP >70 mmHg while keeping ICP <20 mmHg - the golden ratio for cerebral perfusion
| Parameter | Target Range | Critical Threshold | Monitoring Method | Clinical Significance |
|---|---|---|---|---|
| CPP | 70-100 mmHg | <60 mmHg | Arterial line + ICP | Brain perfusion adequacy |
| ICP | <15 mmHg | >20 mmHg | Direct monitoring | Herniation risk |
| PaCO2 | 35-40 mmHg | <30 or >45 | ABG analysis | CBF regulation |
| MAP | 80-100 mmHg | <65 mmHg | Arterial monitoring | Autoregulation zone |
| Temperature | 36-37°C | >38°C | Core monitoring | Neuroprotection |
🧠 Neuroanesthesia: The Brain's Guardian Protocol
⚡ Cerebral Hemodynamics: The Brain's Circulation Command Center
Cerebral Blood Flow (CBF) averages 50 mL/100g/min in gray matter and 20 mL/100g/min in white matter, totaling approximately 750 mL/min or 15% of cardiac output. This massive perfusion requirement reflects the brain's 20% share of total body oxygen consumption despite representing only 2% of body weight.
📌 Remember: FLOW determines CBF - Factor responsiveness (CO2, O2), Location autoregulation, Oxygen consumption coupling, Wave pressure relationships
Autoregulation Mechanisms:
- Myogenic Response: Vascular smooth muscle responds to transmural pressure changes within 15-30 seconds
- Pressure ↑ → vasoconstriction → CBF maintained
- Pressure ↓ → vasodilation → CBF preserved
- Critical threshold: Fails below MAP 50 mmHg or above 150 mmHg
- Metabolic Coupling: CMRO2 directly correlates with CBF through adenosine and lactate signaling
- Normal CMRO2: 3.5 mL O2/100g/min
- Ischemic threshold: CBF <18-20 mL/100g/min
- Chemical Regulation: PaCO2 provides most potent CBF control
- CO2 reactivity: 2-4% CBF change per mmHg PaCO2
- Hyperventilation: PaCO2 25-30 mmHg reduces CBF by 30-40%
⭐ Clinical Pearl: Hyperventilation provides rapid ICP reduction but risks cerebral ischemia - limit to PaCO2 30-35 mmHg and duration <30 minutes
💡 Master This: Monroe-Kellie Doctrine governs intracranial dynamics - brain (80%) + blood (10%) + CSF (10%) = constant volume. Any increase in one component demands compensatory reduction in others.
Understanding cerebral hemodynamics transforms your approach to neuroanesthetic management, providing the physiological foundation for every intervention from positioning to pharmacological manipulation.
⚡ Cerebral Hemodynamics: The Brain's Circulation Command Center
🎯 Anesthetic Agents: The Neurochemical Arsenal
Intravenous Anesthetic Effects on CBF and CMRO2:
📌 Remember: GABA agents for neuroprotection - Good CBF reduction, Anticonvulsant properties, Brain protection, Autoregulation preserved
-
Propofol: The neuroanesthetic gold standard
- CBF reduction: 30-50% dose-dependent
- CMRO2 reduction: 35-60% with burst suppression at >4 mg/kg/hr
- ICP reduction: 25-40% through vasoconstriction
- Neuroprotection: Antioxidant properties + GABA enhancement
- Emergence: Context-sensitive half-time increases from 10 minutes (2 hours) to 50 minutes (8+ hours)
-
Etomidate: Hemodynamic stability champion
- CBF reduction: 35-45% with autoregulation preserved
- Cardiovascular stability: Minimal MAP changes even in shock states
- Limitation: Adrenal suppression lasting 6-24 hours
- Indication: Hemodynamically unstable patients requiring neuroprotection
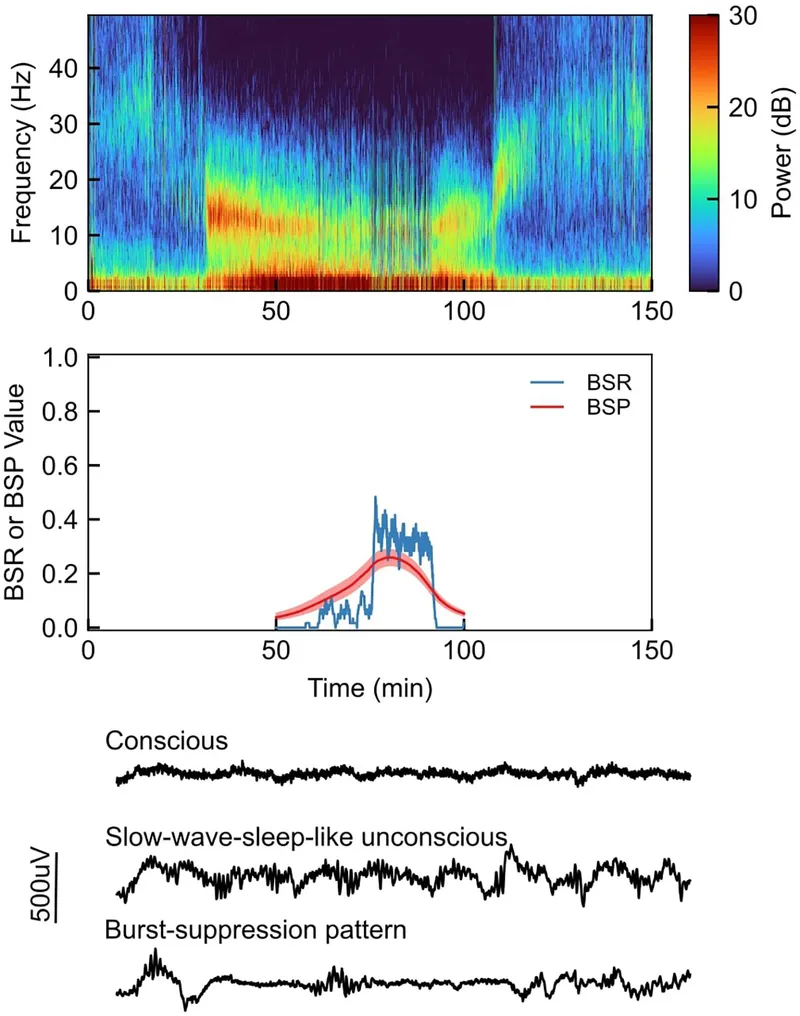
Volatile Anesthetic Considerations:
| Agent | CBF Effect | CMRO2 Effect | ICP Impact | MAC-Awake | Neuroprotection |
|---|---|---|---|---|---|
| Sevoflurane | ↑20-40% | ↓30-50% | ↑Mild | 0.3-0.5 | Preconditioning |
| Isoflurane | ↑50-80% | ↓45-65% | ↑Moderate | 0.25-0.4 | Controversial |
| Desflurane | ↑60-100% | ↓40-60% | ↑Significant | 0.3-0.5 | Limited data |
Neuromuscular Blocking Considerations:
- Rocuronium: Onset 60-90 seconds, duration 30-60 minutes, sugammadex reversible
- Intubating dose: 0.6-1.2 mg/kg for rapid sequence
- Maintenance: 0.15 mg/kg every 20-30 minutes
- Vecuronium: Onset 90-120 seconds, duration 25-45 minutes, hepatic elimination
- Preferred in renal dysfunction due to hepatic metabolism
- Avoid succinylcholine: ICP increase of 5-15 mmHg lasting 5-10 minutes
💡 Master This: Total intravenous anesthesia (TIVA) with propofol + remifentanil provides optimal ICP control, rapid emergence, and immediate neurological assessment - the neuroanesthetic technique of choice.
Connect these pharmacological principles through positioning strategies to understand how anesthetic choices integrate with surgical requirements and patient safety.
🎯 Anesthetic Agents: The Neurochemical Arsenal
🔄 Positioning Protocols: The Spatial Strategy Matrix
Position-Specific Physiological Impacts:
📌 Remember: HEADS for positioning priorities - Hemodynamics, Eye protection, Airway security, Drainage optimization, Safety monitoring
-
Supine Position: Foundation for supratentorial procedures
- Head elevation: 15-30 degrees improves venous drainage by 20-30%
- Neck rotation: Limit to <45 degrees to prevent jugular compression
- CPP maintenance: Minimal hydrostatic gradient preserves cerebral perfusion
- Complications: Macroglossia risk with prolonged procedures >6 hours
-
Lateral Position: Temporal and parietal access optimization
- Dependent ear protection: Gel padding prevents pressure necrosis
- Axillary roll: Prevents brachial plexus compression and vascular compromise
- Venous drainage: Operative side up enhances gravitational drainage
- Monitoring: Dependent eye requires frequent assessment

High-Risk Positioning Considerations:
| Position | Primary Risk | Monitoring Priority | Prevention Strategy | Complication Rate |
|---|---|---|---|---|
| Prone | VAE | Precordial Doppler | CVP monitoring | 2-5% |
| Sitting | VAE + Hypotension | TEE + Arterial line | Volume loading | 10-25% |
| Lateral | Pressure injuries | Pulse checks | Padding protocols | 1-3% |
| Supine | Macroglossia | Tongue assessment | Bite block | <1% |
- Venous Air Embolism (VAE): Incidence 2-5% due to negative venous pressure
- Cardiovascular effects: Decreased venous return and cardiac output ↓15-25%
- Respiratory changes: FRC reduction and V/Q mismatch
- Monitoring essentials: Precordial Doppler, ETCO2, CVP access
⭐ Clinical Pearl: Sitting position carries VAE risk up to 25% but provides optimal surgical access for posterior fossa - requires TEE monitoring and immediate VAE management protocols
Venous Air Embolism Management Protocol:
- Recognition: Mill-wheel murmur, ETCO2 ↓, hypotension, arrhythmias
- Immediate actions: 100% O2, flood surgical field, left lateral Trendelenburg
- Advanced management: Central line aspiration, vasopressor support
- Prevention: PEEP 5-10 cmH2O, adequate hydration, CVP >5 mmHg
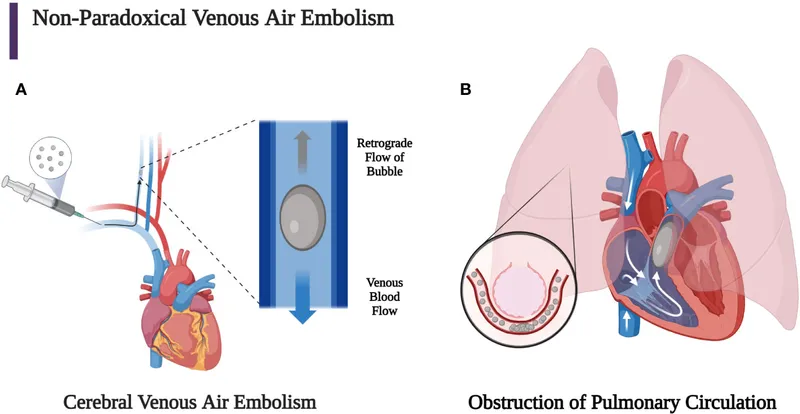
💡 Master This: Position-related complications account for 15-20% of neuroanesthetic morbidity - meticulous pressure point padding, physiological monitoring, and VAE vigilance prevent most adverse outcomes.
These positioning principles connect directly with intraoperative monitoring strategies, where continuous assessment ensures patient safety throughout complex neurosurgical procedures.
🔄 Positioning Protocols: The Spatial Strategy Matrix
📊 Monitoring Mastery: The Neurological Surveillance Network
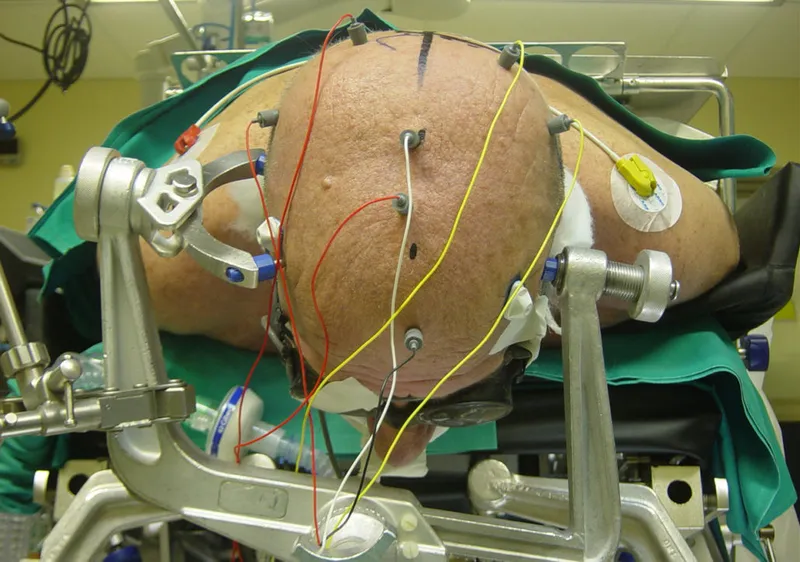
Essential Neuroanesthetic Monitoring Parameters:
📌 Remember: MONITOR for comprehensive surveillance - MAP/CPP, Oxygenation, Neurological function, ICP, Temperature, Output, Respiratory
-
Intracranial Pressure (ICP) Monitoring:
- Normal values: 5-15 mmHg supine, <20 mmHg critical threshold
- Waveform analysis: P1 > P2 > P3 indicates normal compliance
- Pathological patterns: P2 > P1 suggests decreased compliance
- CPP calculation: MAP - ICP with target >70 mmHg
- Monitoring duration: Continuous for elevated ICP risk procedures
-
Processed EEG Monitoring:
- Bispectral Index (BIS): Target 40-60 for adequate anesthesia
- Burst suppression: >80% indicates excessive depth
- Seizure detection: High-frequency activity with amplitude changes
- Ischemia recognition: Slow wave activity and amplitude reduction
Advanced Neuromonitoring Techniques:
| Modality | Parameter | Normal Range | Abnormal Threshold | Clinical Significance |
|---|---|---|---|---|
| SSEP | Latency | <10% increase | >10% increase | Spinal cord function |
| MEP | Amplitude | >50% baseline | <50% baseline | Motor pathway integrity |
| BAER | Wave V | <0.5ms delay | >0.5ms delay | Brainstem function |
| Near-IR | rSO2 | >60% | <50% | Cerebral oxygenation |
- Somatosensory (SSEP): Dorsal column and sensory pathway assessment
- Latency increase >10% or amplitude decrease >50% = significant change
- Anesthetic effects: Volatile agents cause dose-dependent suppression
- Motor Evoked Potentials (MEP): Corticospinal tract monitoring
- Amplitude reduction >50% indicates motor pathway compromise
- Anesthetic sensitivity: Neuromuscular blockade must be minimal
- Brainstem Auditory (BAER): Posterior fossa procedure essential
- Wave V latency >0.5ms suggests brainstem dysfunction
⭐ Clinical Pearl: TIVA with propofol + remifentanil provides stable evoked potentials while volatile agents >0.5 MAC can suppress MEPs by 80-90%
Cerebral Oxygenation Monitoring:
- Near-Infrared Spectroscopy (NIRS):
- Regional oxygen saturation (rSO2): Normal 60-80%
- Critical threshold: <50% or >20% decrease from baseline
- Bilateral monitoring: Asymmetry >10% suggests unilateral pathology
- Trending capability: Real-time ischemia detection during vascular procedures

💡 Master This: Multimodal monitoring combining ICP, EEG, evoked potentials, and cerebral oximetry provides 360-degree neurological surveillance - essential for complex neurovascular and spine procedures with neurological risk.
These monitoring principles integrate seamlessly with emergence strategies, where rapid awakening and immediate neurological assessment validate the success of neuroanesthetic management.
📊 Monitoring Mastery: The Neurological Surveillance Network
🚀 Emergence Excellence: The Awakening Architecture
Emergence Timeline and Targets:
📌 Remember: AWAKE for emergence priorities - Airway protection, Wake-up timing, Assessment readiness, Keep hemodynamics stable, Emergence quality
-
Rapid Emergence Protocol (5-15 minutes):
- Anesthetic cessation: Propofol off at dural closure
- Reversal agents: Sugammadex 2-4 mg/kg for rocuronium reversal
- Target timeline: Eye opening <10 minutes, extubation <15 minutes
- Neurological assessment: GCS evaluation within 5 minutes of awakening
-
Hemodynamic Management During Emergence:
- Hypertension control: SBP target <160 mmHg to prevent hemorrhage
- Antihypertensive options: Labetalol 10-20 mg IV or nicardipine 0.5-2 mg IV
- Avoid hypotension: MAP >65 mmHg maintains cerebral perfusion
- Heart rate control: Target 60-100 bpm with beta-blocker if needed
Emergence Complications and Management:
| Complication | Incidence | Recognition | Immediate Management | Prevention Strategy |
|---|---|---|---|---|
| Hypertension | 40-60% | SBP >180 | Labetalol/Nicardipine | Smooth emergence |
| Agitation | 15-25% | Confusion/combative | Propofol bolus | Pain control |
| Delayed awakening | 5-10% | No response >20min | Reversal agents | TIVA technique |
| Respiratory depression | 2-5% | RR <10, SpO2 <95% | Naloxone if needed | Opioid titration |
- Residual anesthetics: Propofol context-sensitive accumulation
- Metabolic causes: Hypoglycemia, electrolyte imbalance, hypothermia
- Neurological causes: Intracranial hemorrhage, cerebral edema, seizure
- Pharmacological: Residual neuromuscular blockade, opioid excess
⭐ Clinical Pearl: Smooth emergence prevents intracranial pressure spikes - maintain anesthetic depth until surgical stimulation ceases, then rapid but controlled awakening
Immediate Neurological Assessment Protocol:
- Level of consciousness: GCS score with motor, verbal, eye opening
- Motor function: Bilateral strength testing and coordination assessment
- Cranial nerves: Pupillary response, facial symmetry, speech clarity
- Cognitive function: Orientation, memory, following commands
- Vital signs: Hemodynamic stability and respiratory adequacy
Quality Emergence Indicators:
- Timeline: Awakening <10 minutes, extubation <15 minutes
- Hemodynamics: MAP 65-100 mmHg, HR 60-100 bpm
- Neurological: Baseline function or expected deficits only
- Respiratory: Adequate ventilation without support
- Comfort: Pain score <4/10, minimal agitation
💡 Master This: Emergence quality directly correlates with anesthetic technique - TIVA with short-acting agents, multimodal analgesia, and hemodynamic optimization throughout the procedure ensure rapid, smooth, and neurologically intact awakening.
This emergence mastery completes the neuroanesthetic journey from preoperative optimization through intraoperative precision to successful awakening - transforming complex neurosurgical procedures into predictable, safe, and successful patient outcomes through evidence-based neuroanesthetic excellence.
🚀 Emergence Excellence: The Awakening Architecture
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























