LAST: Definition & Pathophysiology - Uh Oh, Overdose!
- Definition: LAST: Severe systemic reaction to high plasma LA levels; affects CNS & CVS.
- Primary Cause: Accidental intravascular injection; also excessive dose, rapid absorption, or ↓metabolism.
- Mechanism:
- Dose-dependent blockade of voltage-gated $Na^+$ channels.
- CNS: Initial excitation (perioral numbness, tinnitus, seizures) via blockade of inhibitory pathways, then generalized depression (coma, respiratory arrest).
- CVS: Myocardial depression (↓contractility, bradycardia, hypotension), arrhythmias (VT/VF, asystole).
⭐ Highly lipid-soluble LAs (e.g., bupivacaine) have ↑cardiotoxicity due to slower dissociation from cardiac $Na^+$ channels.
LAST: Clinical Features - Systemic Storm Signals
- CNS Manifestations (Often Biphasic):
- Early Excitation: Metallic taste, perioral numbness, tinnitus, agitation, dizziness, visual disturbances, muscle twitching, tremors.
- Advanced Excitation: Slurred speech, seizures (tonic-clonic).
- Depression (Late): Drowsiness, unconsciousness, coma, respiratory depression/apnea.
- Cardiovascular Manifestations (Can precede, follow, or occur with CNS signs):
- Early (Hyperdynamic): Hypertension, tachycardia, ventricular ectopy.
- Late (Depressant): Hypotension, bradycardia, ↓contractility, conduction blocks (↑PR, ↑QRS duration), ventricular arrhythmias (VT/VF), asystole.
- 📌 Mnemonic: SAMS (Slurred speech, Altered mental status, Muscle twitching, Seizures) for key CNS signs.
⭐ Bupivacaine is notorious for severe cardiotoxicity that can be refractory to standard resuscitation and may occur before or concurrently with CNS signs, often with rapid progression to cardiovascular collapse.
 oka
oka
LAST: Prevention Strategies - Dodging Danger
- Risk Assessment: Identify high-risk patients (elderly, organ dysfunction, pregnancy).
- Dose Minimization: Use lowest effective LA volume & concentration.
- Strictly adhere to maximum recommended doses.
- Safe Technique:
- Frequent aspiration before & during injection.
- Incremental injections: 3-5 mL aliquots.
- Ultrasound guidance (USG) strongly advised.
- Consider epinephrine test dose.
- Preparedness: Ensure immediate availability of lipid emulsion & resuscitation equipment.
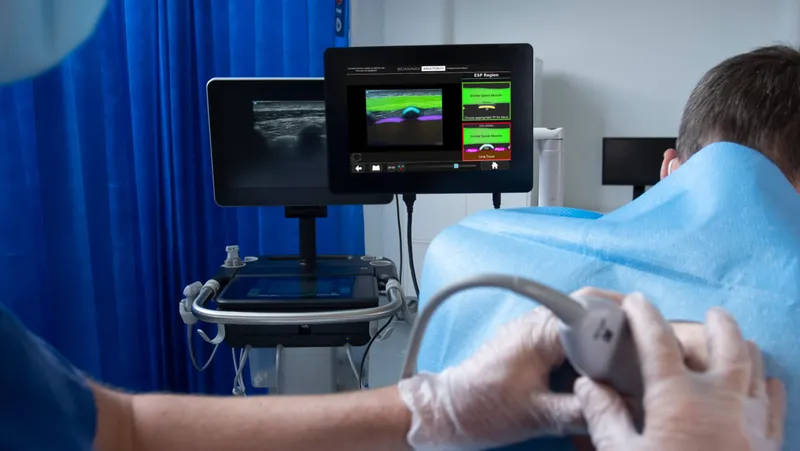
⭐ Ultrasound guidance significantly reduces LAST risk by allowing real-time visualization of needle and injectate spread, minimizing intravascular injection or excessive local spread near sensitive structures.
LAST: Management Protocol - Rescue Mission
Key Steps:
- STOP LA INJECTION & Call for Help.
- Airway: 100% O₂. Intubate if needed.
- Seizures: Benzodiazepines (Midazolam 0.05-0.1 mg/kg). Avoid large propofol doses.
Lipid Emulsion (20%):
- Bolus: 1.5 mL/kg IV over 1 min.
- Infusion: 0.25 mL/kg/min.
- Repeat bolus (1-2x) if unstable. Max: 10-12 mL/kg (first 30 min).
Modified ACLS (if arrest):
- Epinephrine: Small doses (≤1 mcg/kg).
- Amiodarone for VT/VF.
- Avoid: Vasopressin, CCBs, β-blockers.
- Prolonged resuscitation.
⭐ Lipid emulsion therapy is the cornerstone of LAST management, acting as a "lipid sink".
High-Yield Points - ⚡ Biggest Takeaways
- Stop LA injection immediately at first signs of toxicity.
- Secure airway, give 100% O2; manage seizures with benzodiazepines.
- Administer 20% lipid emulsion: 1.5 mL/kg IV bolus, then 0.25 mL/kg/min infusion.
- For cardiac arrest, use modified ACLS: small epinephrine doses (<1 mcg/kg), avoid vasopressin.
- CNS symptoms (e.g., tinnitus, metallic taste, seizures) often precede cardiovascular collapse.
- Avoid propofol for seizures if cardiovascular instability is present; lipid emulsion is preferred treatment for LAST-induced seizures or cardiac arrest.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

