Extended-Release LAs - Long‑Lasting Blocks
- Goal: Prolong analgesia (up to 72+ hours), ↓ opioid use, ↓ catheter need.
- Mechanisms & Formulations:
- Liposomal encapsulation (e.g., Exparel)
- Polymer-based systems (microspheres, hydrogels)
- Nanoparticles, prodrugs
- Key Example: Exparel (Liposomal Bupivacaine)
- Bupivacaine in DepoFoam (multivesicular liposomes).
- Approved: Surgical site infiltration, interscalene block.
- Duration: Up to 72 hours.
- Caution: Avoid mixing with lidocaine/other LAs (disrupts liposomes); specific bupivacaine HCl ratios allowed.
⭐ Exparel (liposomal bupivacaine) offers analgesia for up to 72 hours via slow release from DepoFoam technology.
- Advantages:
- Sustained pain relief, ↓ opioid needs.
- ↓ systemic toxicity risk (lower $C_{max}$).
- Improved patient satisfaction.
- Challenges:
- Higher cost.
- Fixed dose (no easy titration).
- Risk of prolonged motor block if not precisely placed.

Novel LA Agents - Safer & Targeted
- Primary Goals:
- Enhanced safety: ↓Systemic toxicity (cardiac, CNS), ↓Neurotoxicity.
- Improved efficacy: Prolonged duration, site-specificity.
- Key Approaches & Examples:
- Liposomal Formulations (e.g., Exparel - Liposomal Bupivacaine):
- Mechanism: Slow drug release from lipid vesicles.
- Benefits: Extended analgesia (up to 72 hrs), ↓peak plasma levels, ↓systemic toxicity.
- Use: Post-op pain, nerve blocks.
- Site-Specific/Activated Agents:
- Prodrugs: Activated by local conditions (inflammation, enzymes).
- Targeted delivery: Nanoparticles, microspheres.
- $Na_v$ Subtype-Specific Blockers:
- Target pain-transmitting $Na_v$ channels (e.g., $Na_v$1.7, $Na_v$1.8).
- Potential: Analgesia without motor block or cardiotoxicity; largely investigational.
- Long-Acting Toxins (e.g., Neosaxitoxin):
- Potent, ultra-long duration. Research ongoing for safety.
- Liposomal Formulations (e.g., Exparel - Liposomal Bupivacaine):
⭐ Exparel (liposomal bupivacaine) can provide analgesia for up to 72 hours, significantly reducing post-operative opioid requirements. oka
Emerging Technologies - Anesthesia's New Wave
- Liposomal Formulations (e.g., Exparel):
- Prolonged action (up to 72 hrs).
- ↓ Systemic toxicity.
- Site-specific delivery.
⭐ Liposomal bupivacaine (Exparel) offers extended analgesia up to 72 hours, reducing opioid needs.
- Stimulus-Responsive Systems:
- LA release by pH, temp, ultrasound, light.
- On-demand pain relief.
- E.g., Ultrasound-triggered release.
- Nanotechnology Delivery:
- Nanoparticles, nanoemulsions.
- ↑ Solubility, stability, penetration.
- Targeted delivery, ↓ side effects.
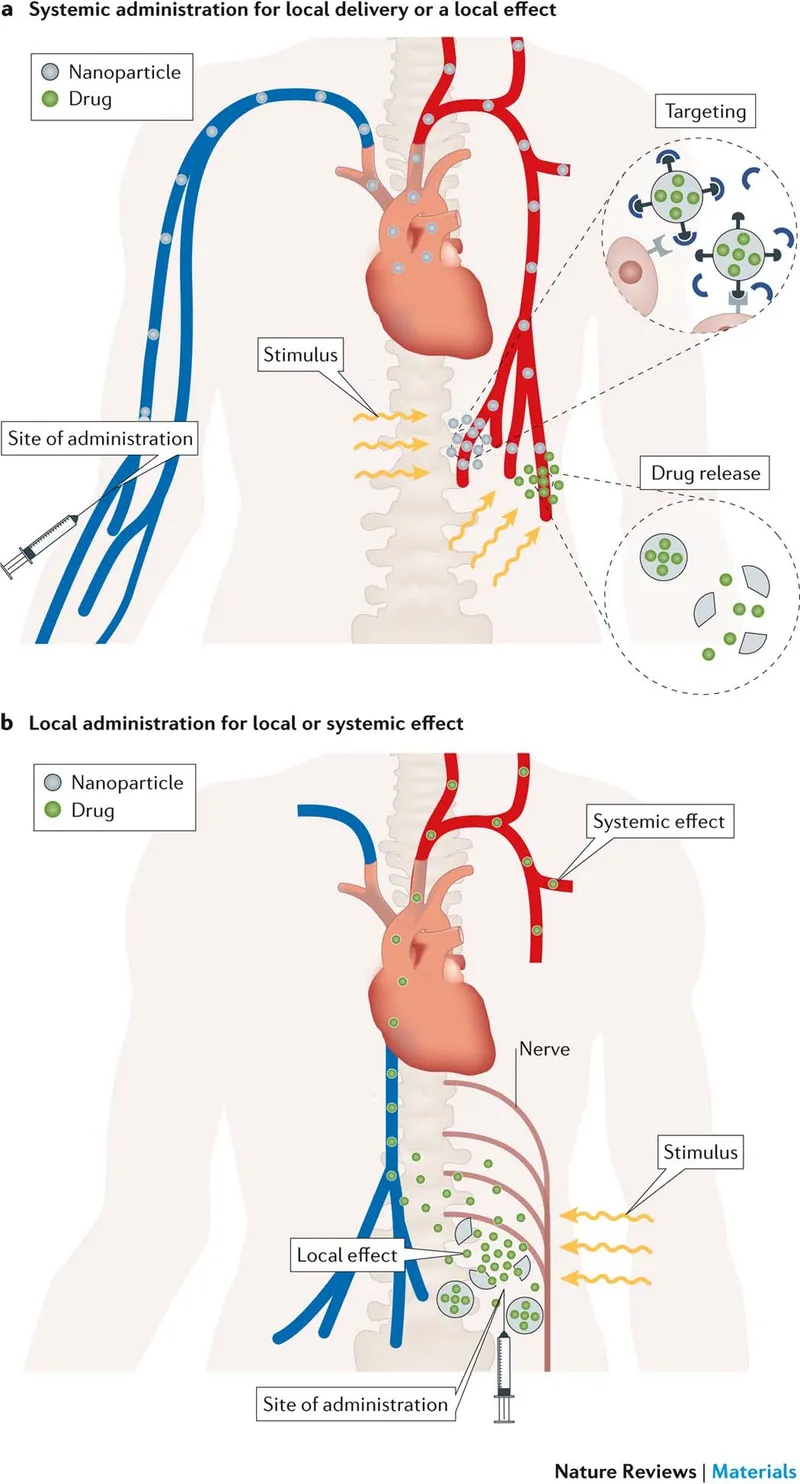
- Site-Specific LA Analogs:
- Target specific Na+ channels (e.g., Nav1.7).
- Aim: Analgesia without motor block.
- Needle-Free Delivery:
- Jet injectors, advanced topical patches.
- ↑ Patient comfort_._
High‑Yield Points - ⚡ Biggest Takeaways
- Liposomal LAs (e.g., Exparel) for prolonged analgesia.
- Nanocarriers (e.g., microspheres) for site-specific delivery, ↑efficacy, ↓toxicity.
- Development of safer LAs with less cardiotoxicity & neurotoxicity.
- Novel adjuvants (e.g., capsaicin analogs) to prolong action, reduce LA dose.
- Nav1.7 inhibitors as subtype-specific blockers for selective analgesia (no motor block).
- Reversible LAs for better control and rapid recovery.
- Needle-free delivery (e.g., jet injectors, patches) for painless application.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

