Ester LAs - The Quick Spritzers
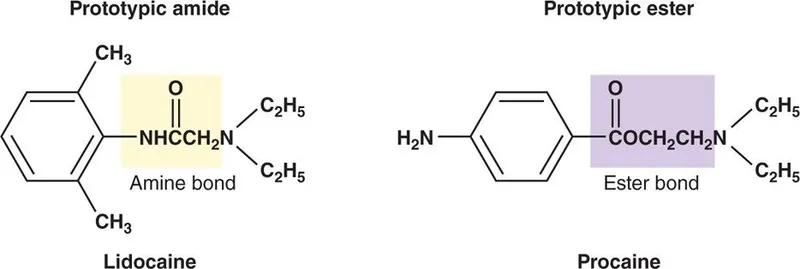
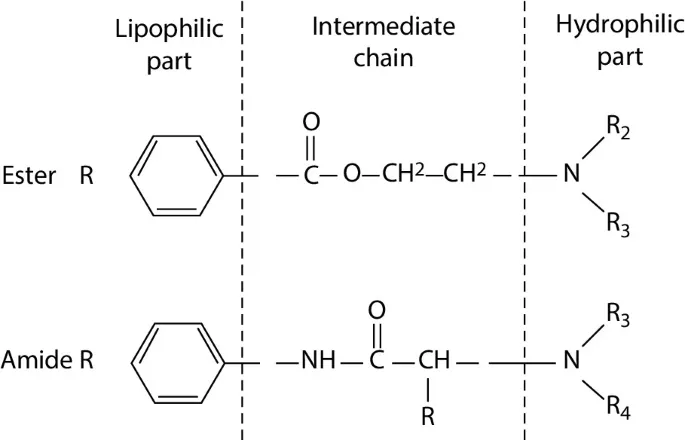
- Contain an ester linkage (-COO-) in their intermediate chain.
- Metabolism: Rapidly hydrolyzed in plasma by pseudocholinesterase.
- Cocaine is an exception (also liver esterases).
- Allergy: Higher potential due to metabolite PABA (para-aminobenzoic acid).
- Cross-allergenicity within the ester group is common.
- Systemic toxicity: Less likely than amides due to rapid breakdown.
- Duration of action: Generally shorter.
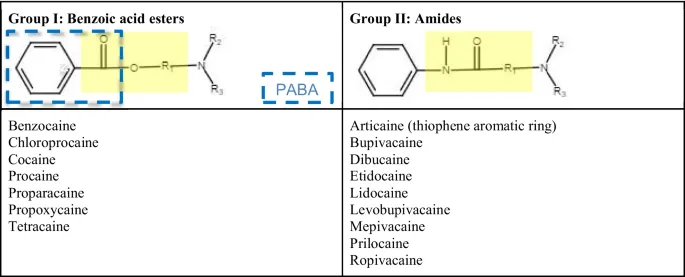
- Examples: Procaine, Cocaine, Tetracaine, Benzocaine, Chloroprocaine.
📌 Mnemonic: Papa Can Take Baby Care.
⭐ Chloroprocaine: shortest duration, rapid metabolism; preferred in obstetrics.
MOA & PK - Block & Vanish
- Mechanism of Action (MOA): Block
- Reversibly block voltage-gated Na+ channels intracellularly.
- Preferentially bind to open/inactivated channels (use-dependency).
- Prevent Na+ influx, blocking nerve impulse conduction.
- Non-ionized form crosses nerve membrane; ionized form is active.
- Pharmacokinetics (PK): Vanish
- Rapidly hydrolyzed by plasma pseudocholinesterases (butyrylcholinesterase).
- Results in characteristically short duration of action.
- Metabolite: Para-aminobenzoic acid (PABA) → potential for allergic reactions. 📌 "Esters are Pests (PABA)"
- Minimal hepatic metabolism (cocaine is an exception, also metabolized by liver esterases).
- Onset: Governed by pKa (↓pKa = ↑non-ionized form = faster onset).
- Duration: ↑ with protein binding & lipid solubility; vasoconstrictors (e.g., adrenaline) prolong duration & ↓ systemic toxicity.
- Rapidly hydrolyzed by plasma pseudocholinesterases (butyrylcholinesterase).
⭐ Allergic reactions to local anesthetics are significantly more common with esters due to their metabolism to PABA (para-aminobenzoic acid) derivatives.
The Ester Crew - Meet the Agents
All esters are hydrolyzed by plasma pseudocholinesterases to para-aminobenzoic acid (PABA), which can cause allergic reactions. They generally have a shorter duration of action than amides.
- 📌 Esters have one 'i' in their name (e.g., Procaine, Cocaine, Tetracaine, Benzocaine, Chloroprocaine).
| Agent | Potency | Onset | Duration | Key Uses / Notes |
|---|---|---|---|---|
| Cocaine | Medium | Medium | Medium | Topical (ENT), potent vasoconstrictor (blocks NE reuptake), Schedule II drug. |
| Procaine | Low | Slow | Short | Infiltration, nerve blocks (largely historical). High PABA metabolite (allergy). |
| Chloroprocaine | High | V. Fast | V. Short | Epidural (obstetrics), spinal. Rapid hydrolysis, low systemic toxicity. |
| Tetracaine | High | Slow | Long | Spinal, topical (corneal). Potent, longer acting ester. |
| Benzocaine | Low | Fast | Short | Topical ONLY (sprays, lozenges). ⚠️ Risk of methemoglobinemia. |
Side Effects & Allergies - The Ester Sting
- Systemic Toxicity (dose-dependent):
- CNS: Early (circumoral numbness, tinnitus, metallic taste); Late (seizures, coma).
- CVS: Hypotension, bradycardia, arrhythmias, cardiac arrest. (Cocaine: unique vasoconstriction, hypertension).
- Management of LA Systemic Toxicity (LAST):
- Stop LA injection, ABCs (Airway, Breathing, Circulation), Oxygen.
- Seizures: Benzodiazepines.
- Lipid Emulsion (20%): Bolus 1.5 mL/kg IV, then 0.25 mL/kg/min infusion.
- Allergic Reactions (📌 PABA = Problem):
- More common with esters due to Para-aminobenzoic acid (PABA) metabolite.
- Range: Skin rash, urticaria, angioedema to anaphylaxis.
- Generally no cross-allergy with amide LAs.
⭐ Allergic reactions to ester local anesthetics are primarily due to their metabolite, para-aminobenzoic acid (PABA), not the parent drug itself.
High‑Yield Points - ⚡ Biggest Takeaways
- Metabolized by plasma pseudocholinesterase; PABA metabolite is responsible for allergic reactions.
- Generally have a shorter duration of action compared to amide local anesthetics.
- Cocaine is unique: causes vasoconstriction (blocks NE reuptake) and CNS stimulation.
- Procaine: Low potency, short duration, high incidence of allergy; prototype.
- Tetracaine: Potent, long-acting ester, commonly used for spinal anesthesia.
- Chloroprocaine: Rapid onset, very short duration, low toxicity; ideal for obstetrics.
- Benzocaine: Used topically only; associated with methemoglobinemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

