Clinical Uses: LA Application Routes - Numbness Delivery
- Topical Anesthesia:
- Applied to skin or mucous membranes (cornea, throat, urethra).
- Forms: Sprays, gels, creams, ointments.
- Agents: Lidocaine, tetracaine, benzocaine.
⭐ EMLA (Eutectic Mixture of Local Anesthetics): Lidocaine 2.5% + Prilocaine 2.5%. Minimum application time: 60 minutes on intact skin.
- Infiltration Anesthesia:
- Direct injection into tissues for localized numbness.
- Uses: Suturing, wound cleaning, minor excisions, dental procedures.
- Field block: LA injected around the target area.
- Intravenous Regional Anesthesia (IVRA - Bier's Block):
- LA injected into an exsanguinated limb, isolated by a tourniquet.
- Provides anesthesia for limb surgery (e.g., forearm, hand).
oka
Clinical Uses: Nerve Block Techniques - Pinpoint Anesthesia
- Peripheral Nerve Blocks (PNBs): Target specific nerves/plexuses for localized anesthesia & analgesia.
- Upper Limb: Brachial plexus (Interscalene, Supraclavicular, Axillary); Median, Ulnar, Radial nn.
- Lower Limb: Femoral, Sciatic (Popliteal, Ankle), Obturator nn.
- Trunk: Intercostal, Paravertebral, TAP blocks.
- Head & Neck: Trigeminal branches, Cervical plexus.
- Guidance Techniques:
- Landmark-based: Relies on anatomical knowledge.
- Peripheral Nerve Stimulator (PNS): Elicits motor response to confirm proximity.
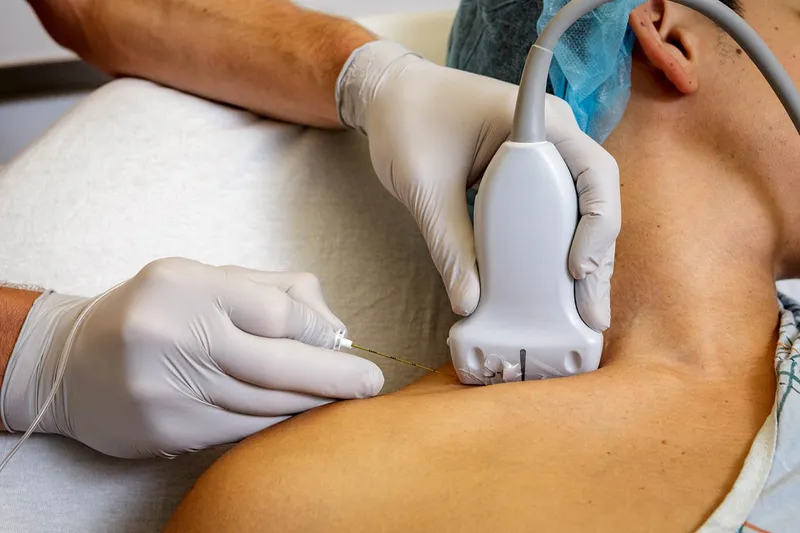
- Ultrasound Guidance (USG): Real-time visualization of nerve & needle; ↑success, ↓complications. Gold Standard.
- Central Neuraxial Blocks (CNBs): More regional; can be targeted (e.g., segmental spinal/epidural).
- Spinal: Anesthesia via subarachnoid LA injection.
- Epidural: Analgesia/anesthesia via epidural LA; catheter for continuous/bolus.
⭐ Order of sensory/functional loss in PNBs: Sympathetic block (vasodilation, temp ↑) → Pain & Temperature (Aδ, C fibers) → Proprioception (Aγ) → Touch & Pressure (Aβ) → Motor function (Aα). 📌 Mnemonic: Some People Prefer Touching Motors.
Clinical Uses: Beyond Surgical Fields - LA's Versatile Roles
- Acute & Chronic Pain Management:
- Post-operative analgesia: wound infiltration, continuous nerve blocks.
- Chronic pain: neuropathic pain, cancer pain (nerve/epidural blocks).
- Labor analgesia: epidural, spinal.
- Cardiac Arrhythmias:
- Ventricular tachyarrhythmias.
⭐ Lidocaine is a Class Ib antiarrhythmic, used for ventricular tachycardia. Typical IV bolus: 1-1.5 mg/kg, followed by infusion 1-4 mg/min.
- Diagnostic Procedures:
- Nerve blocks to pinpoint pain origin.
- Other Specialized Uses:
- Topical anesthesia: mucous membranes (e.g., bronchoscopy).
- Sympathetic blockade: e.g., Complex Regional Pain Syndrome (CRPS).
- Antitussive: nebulized lidocaine for intractable cough.
- Anti-inflammatory properties (emerging evidence).
Clinical Uses: Clinical Safety Net - LA Caveats & Care
- ⚠️ Max Dose Adherence: Critical. Calculate per LA, weight, site.
- Vasoconstrictors (Epinephrine):
- Pros: Prolongs action, ↓systemic absorption & bleeding.
- Cons: Risk of ischemia in end-arterial zones (fingers, toes, nose, penis); systemic effects.
- Patient Factors:
- Liver disease: Impairs amide metabolism.
- Pseudocholinesterase deficiency: Prolongs ester LA action.
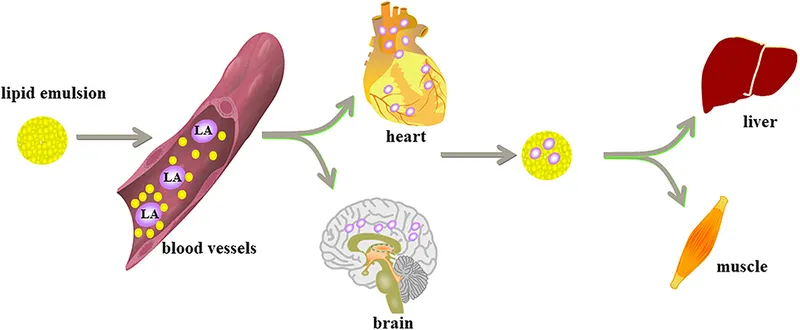
- LAST (Local Anesthetic Systemic Toxicity):
- CNS excitation (tinnitus, seizures) → CNS depression → CVS toxicity.
⭐ Initial bolus dose of lipid emulsion (20%) for LAST: 1.5 mL/kg over 1 min. Max total 3 mL/kg.
- Other Complications:
- Allergy: Rare (esters > amides; PABA).
- Methemoglobinemia: Prilocaine, Benzocaine. Tx: Methylene Blue.
High‑Yield Points - ⚡ Biggest Takeaways
- Topical anesthesia: For mucous membranes (airway) & skin (EMLA).
- Infiltration: Direct tissue injection for minor surgeries.
- Peripheral Nerve Blocks: Target specific nerves/plexuses for limb surgery.
- Spinal Anesthesia: Subarachnoid injection for rapid, dense surgical block.
- Epidural Anesthesia: For labor analgesia & post-op pain control.
- IVRA (Bier's Block): For short limb surgeries using a tourniquet.
- Lidocaine: Systemically for ventricular arrhythmias; also in chronic pain blocks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

