Preoperative Evaluation: Goals & Components - Setting the Stage
- Goals:
- Identify patient risks, optimize conditions.
- Formulate anesthetic strategy.
- Obtain informed consent.
- Reduce patient anxiety.
- Minimize perioperative morbidity & mortality.
- Components:
- History: Medical, surgical, anesthesia, drugs (📌AMPLE: Allergies, Medications, Past medical Hx, Last meal, Events leading to surgery), allergies.
- Physical Exam: Systemic, vitals, airway (e.g., Mallampati).
- Investigations: Indicated, not routine.
- Risk Assessment: ASA status, functional capacity (METs).
- Premedication & fasting guidelines.
⭐ ASA Physical Status Classification is a key predictor of perioperative risk and guides management.
Preoperative Evaluation: Patient Assessment - History & Exam Secrets
- History:
- 📌 AMPLE: Allergies, Medications (anticoagulants, insulin, steroids, MAOIs), Past medical Hx (cardiac, resp, renal, hepatic, endocrine), Last meal (solids 6-8h, clear fluids 2h prior), Events leading to surgery.
- Anesthetic Hx: Prior difficult intubation, Postoperative Nausea & Vomiting (PONV). Family Hx: Malignant hyperthermia, suxamethonium apnoea.
- Functional Capacity: Metabolic Equivalents (METs); < 4 METs (e.g., cannot climb 1 flight of stairs) indicates poor reserve.
- Habits: Smoking (advise cessation 4-8 weeks prior), alcohol, drug abuse.
- Examination:
- Vitals (BP, HR, RR, Temp), BMI. Systemic: Cardiovascular (murmurs, JVP), Respiratory (air entry, wheeze).
- Airway Assessment (Crucial for Safety):
- 📌 LEMON:
- Look externally (facial trauma, large incisors, beard, macroglossia).
- Evaluate 3-3-2 rule: Inter-incisor gap (3 fingers), Hyoid-mental distance (3 fingers), Thyrohyoid distance/Thyroid cartilage to floor of mouth (2 fingers).
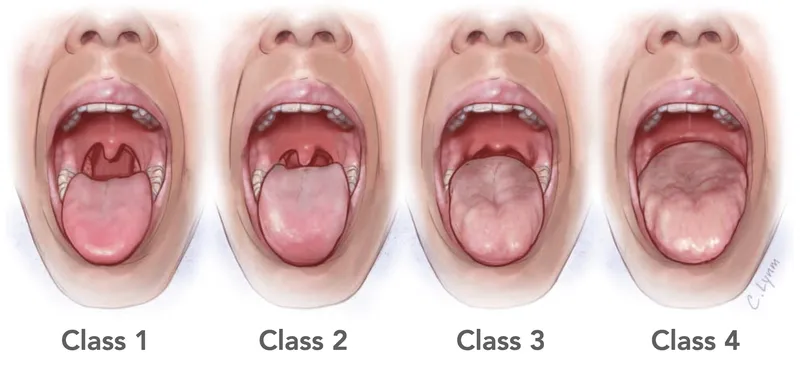
- Mallampati classification (I-IV): Assesses tongue vs. pharyngeal space.
- Obstruction (e.g., goiter, tumor, Ludwig’s angina, stridor).
- Neck mobility: Full flexion & extension (atlanto-occipital joint extension >35°).
- Thyromental Distance (TMD): Normal > 6.5 cm. If < 6 cm, suspect difficult laryngoscopy.
- Inter-incisor Gap (Mouth Opening): Normal > 3 cm (or 2 large finger breadths).
- Upper Lip Bite Test (ULBT): Class I (can bite upper lip above vermilion line), II (below vermilion), III (cannot bite).
- 📌 LEMON:
⭐ A combination of Mallampati Class III/IV, Thyromental Distance (TMD) < 6 cm, and reduced neck movement (especially extension < 35°) significantly increases the likelihood of difficult intubation.
Preoperative Evaluation: Investigations & Risk - Numbers Game
-
Selective Investigations (Not Routine):
- ECG: Age >50y, cardiac Hx/disease, mod-high risk surgery.
- Hb: Major blood loss expected; transfuse if <7-8 g/dL.
- Creatinine: Baseline for RCRI.
- Coagulation: Bleeding Hx, anticoagulants.
-
Cardiac Risk:
- Functional Capacity: METS <4 (e.g., can't climb stairs) = poor.
- RCRI (Revised Cardiac Risk Index) - 1 point each:
- High-risk surgery (vascular, intraperitoneal, intrathoracic)
- Hx IHD
- Hx CHF
- Hx CVA/TIA
- Preoperative Insulin Rx
- Preoperative Creatinine >2 mg/dL
- Stratify MACE risk using RCRI score:
- Pulmonary Risk:
- Factors: Age, SpO2 <96%, recent RTI, anemia (Hb <10 g/dL), site (thoracic/upper abd.), duration >2h, emergency.
- 📌 Smoking cessation: 4-8 weeks prior.
⭐ RCRI ≥1: Consider beta-blockers for high-risk surgery (start days before, not day-of).
Preoperative Evaluation: Fasting & Premeds - Final Prep Rally
- NPO Guidelines (📌 2-4-6-8 Rule): Clear liquids 2 hrs; Breast milk 4 hrs; Infant formula/Light meal 6 hrs; Fatty/Fried meal/Meat 8 hrs.
- Premed Goals: Anxiolysis, sedation, analgesia, amnesia, antisialagogue, aspiration prophylaxis (↑pH, ↓volume), blunt reflexes.
- Common Premeds:
- Anxiolytics: Benzodiazepines (e.g., Midazolam).
- Analgesics: Opioids (e.g., Fentanyl), NSAIDs.
- Anticholinergics: Glycopyrrolate (↓secretions).
- Antiemetics: Ondansetron.
- Aspiration Prophylaxis: H2 blockers (Ranitidine), PPIs (Omeprazole), Sod. Citrate.
- Informed Consent: Essential; covers procedure, risks, benefits, alternatives. Patient capacity vital.
- Final Pre-op Check: Patient ID, surgical site, IV access, allergies reviewed.
⭐ Sodium citrate (0.3M solution, 15-30 mL) given 15-30 minutes before induction rapidly increases gastric pH without increasing volume, reducing aspiration risk.
High‑Yield Points - ⚡ Biggest Takeaways
- ASA physical status is vital for perioperative risk stratification.
- Mallampati score (I-IV) helps predict difficult intubation.
- NPO guidelines: 2h (clears), 4h (breast milk), 6h (light meal), 8h (fatty meal).
- Pre-op ECG if >50 yrs or with cardiac risk factors.
- Critical history: prior anesthetic complications (e.g., MH), allergies.
- Assess functional capacity (METs); >4 METs is generally good.
- Manage anticoagulants/antiplatelets balancing thrombotic vs. bleeding risks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

