Postoperative Care - PACU Priorities!
- PACU: Initial Assessment (ABCDE)
- Airway: Patency, SpO2 > 92%.
- Breathing: Rate, depth, air entry.
- Circulation: HR, BP (±20% baseline), rhythm.
- Disability: LOC, Aldrete Score (target ≥ 9).
- Environment: Temp > 36°C; pain (VAS < 4), PONV, surgical site.
- Monitor for: Key Concerns
- Hypoxemia, hypotension/hypertension.
- Pain, PONV, shivering.
- PACU Discharge Criteria
- Aldrete Score ≥ 9 (or pre-op baseline).
- Stable vital signs.
- Pain & PONV controlled.
- No active bleeding or new surgical issues.
⭐ Aldrete Score components: Activity, Respiration, Circulation, Consciousness, O2 Saturation (each 0-2; total 10). Target ≥ 9 for discharge.

Postoperative Care - Complication Combat
- PACU Priorities
- Airway: Obstruction (tongue, spasm), hypoxemia (atelectasis).
- Hemodynamics: Hypotension (bleed, vasodilation), hypertension (pain), arrhythmias.
- Hypothermia: Shivering (↑O₂ demand).
- Ward Watch-outs
- Pain: Multimodal analgesia.
- PONV: Prophylaxis & treatment (e.g., ondansetron).
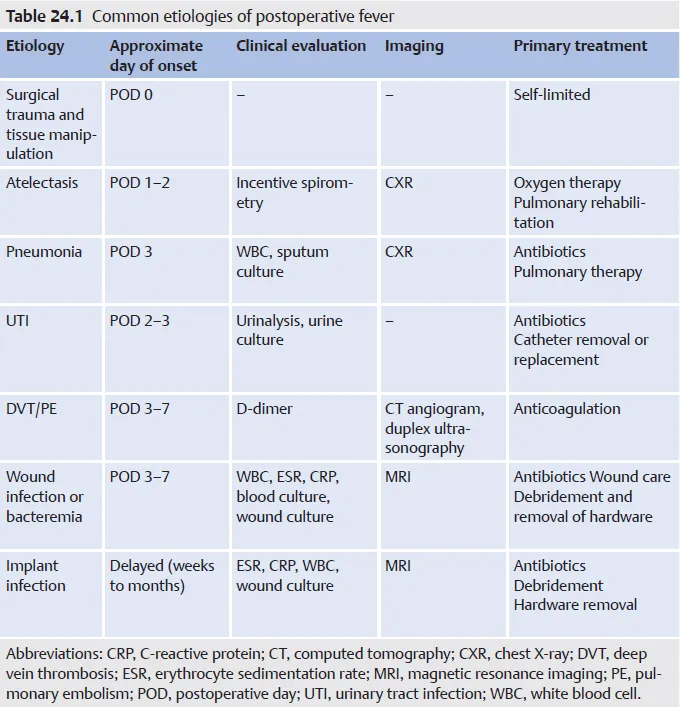
- Fever: 📌 5 W's
- Wind (atelectasis, pneumonia): Day 1-2
- Water (UTI): Day 3-5
- Wound (infection): Day 5-7
- Walking (DVT/PE): Day 7+
- Wonder drugs (drug fever)
- Oliguria: Assess volume status, catheter.
- Ileus: NGT for distension.
- Delayed Dangers
- Surgical Site Infection (SSI).
- DVT/PE: Prophylaxis (LMWH, SCDs), early ambulation.
⭐ Atelectasis is the most common cause of fever in the first 24-48 hours post-operatively.
Postoperative Care - Pain Relief Playbook
- Goal: Optimal pain relief for early mobilization & ↓ complications.
- Assessment: Regular pain scores (VAS, NRS).
- Multimodal Analgesia: Core strategy. Combine agents with different mechanisms.
- Paracetamol: Max 4g/day.
- NSAIDs: e.g., Diclofenac. Caution: Renal, GI, bleeding risk.
- Opioids: e.g., Morphine, Fentanyl. Monitor sedation, respiratory depression, PONV.
- Regional Anesthesia: Epidural, nerve blocks (e.g., TAP block).
- PCA (Patient-Controlled Analgesia): Opioids, empowers patient.
- WHO Ladder Adaptation: Stepwise approach.
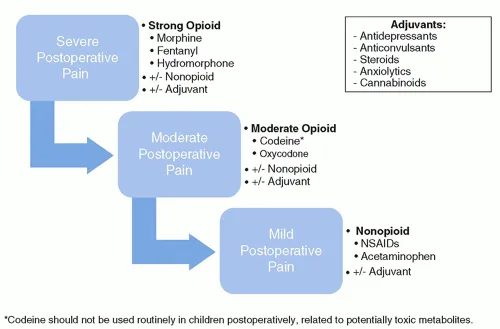
⭐ Multimodal analgesia aims to provide superior pain relief with fewer side effects by combining different analgesic agents acting on various pain pathways.
Postoperative Care - ERAS & Discharge Dash
- ERAS (Enhanced Recovery After Surgery) Protocols: Multimodal approach to ↓ surgical stress & accelerate recovery.
- Key elements: Preoperative counselling, optimal nutrition, opioid-sparing analgesia, early mobilization.
⭐ Core ERAS principle: Early oral intake (within hours post-op) reduces ileus & hospital stay.
- Discharge Criteria (Post-Anesthesia Discharge Scoring System - PADSS):
- Vital signs stable (e.g., Aldrete score ≥ 9)
- Pain controlled
- Nausea/vomiting minimal
- Surgical bleeding minimal
- Able to ambulate & void
High‑Yield Points - ⚡ Biggest Takeaways
- Prioritize airway maintenance and oxygenation immediately post-op.
- Employ multimodal analgesia for optimal pain control and faster recovery.
- Manage Postoperative Nausea and Vomiting (PONV) with prophylaxis and timely treatment.
- Monitor closely for hemorrhage, respiratory depression, and early infection signs.
- Implement early mobilization and DVT prophylaxis to prevent clots.
- Manage postoperative shivering promptly to prevent ↑O2 consumption.
- Assess for PACU discharge using criteria like Aldrete score (vitals, activity, respiration, consciousness, O2 saturation).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

