ERAS & Fasting Basics - Hunger Games Shift
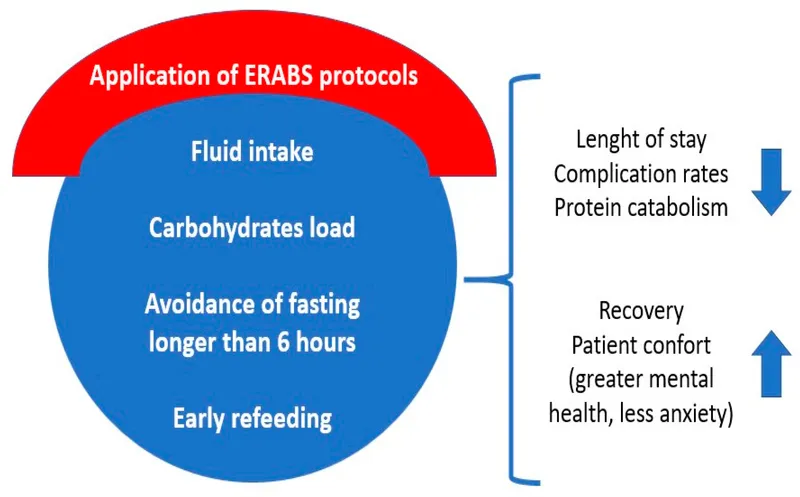
- ERAS: Evidence-based, multimodal care to reduce surgical stress & hasten recovery.
- Traditional NPO: Prolonged fasting → dehydration, insulin resistance, patient distress.
- ERAS Goal: Minimize fasting for:
- Better hydration, ↓PONV.
- Improved insulin sensitivity.
- Enhanced patient comfort.
- Key Pre-op Times:
- Clear fluids: up to 2 hrs.
- Light meal: 6 hrs.
⭐ ERAS protocols allow clear carbohydrate drinks up to 2 hours before surgery, reducing postoperative insulin resistance and improving patient comfort without increasing aspiration risk in most patients.
Current Fasting Rules - Sip, Sip, Hooray!
- ASA/ISA Consensus (Adults & Children):
- Clear Fluids: 2 hours (water, no-pulp juice, black tea/coffee)
- Breast Milk: 4 hours
- Infant Formula / Non-human Milk: 6 hours
- Light Meal (e.g., toast): 6 hours
- Heavy/Fried Meal: 8 hours
- 📌 "2-4-6-8 Rule": Clear fluids → Breast milk → Formula/Light meal → Heavy meal.
- Oral medications: Typically with sips of water up to 1 hour pre-op.
⭐ Preoperative oral carbohydrate drinks (e.g., maltodextrin) 2 hours before surgery can ↓PONV & ↓insulin resistance, improving patient comfort and recovery under ERAS protocols.
Physiology of Shorter Fasts - Gut Feelings & Gains
- Shorter Fasts: Physiological Wins
- Maintains hydration & crucial liver glycogen stores.
- Reduces surgical stress response, ↓ catabolism.
- ↓ Insulin resistance: Pre-op carbs (e.g., maltodextrin 2-3 hours prior) prevent starvation-induced resistance.
- Better glycemic control: Avoids fasting hypoglycemia & stress hyperglycemia.
- ↑ Patient comfort: Significantly less hunger, thirst, anxiety.
- ↓ PONV: Linked to better hydration & reduced ketosis.
- Earlier gut function return: Gentle gut stimulation.
- Prolonged Fasts: Physiological Toll
- Induces insulin resistance, mimics a starved state.
- ↑ Protein breakdown, dehydration, electrolyte disturbances.
⭐ Allowing clear fluids up to 2 hours before surgery significantly reduces patient-reported thirst and anxiety, improving overall experience.
Fasting in Special Groups - Tricky Tummies & Alerts
Modify ERAS fasting for special groups. Balance aspiration risk vs. minimal fasting benefits.
- Diabetes Mellitus:
- Risks: Hypo/hyperglycemia.
- Mgmt: Monitor glucose. Adjust meds. Morning list preferred.
- GERD/Gastroparesis/Hiatus Hernia/Bowel Obstruction:
- ↑ Aspiration risk.
- Mgmt: PPI, H2 blockers, prokinetics. RSI. Solids >6-8h, clears >2-4h (case-by-case).
- Obesity (BMI >35 kg/m²):
- ↑ Gastric volume & pressure.
- Mgmt: ERAS often safe. Individualize. Consider RSI.
- Obstetrics:
- Elective C-Section (non-laboring): ERAS (solids 6h, clears 2h).
- Laboring/Emergency: Assume full stomach. NPO. RSI.
- ⭐ > Parturients in active labor are always considered to have a full stomach.
- Emergency Surgery:
- Assume full stomach. NPO. RSI mandatory.
Pre-Op Carb Drinks - Sweet Surge Strategy
- Goal: Transition from fasted to fed metabolic state before surgery.
- Key effect: ↓ postoperative insulin resistance.
- Protocol: 50g CHO (e.g., maltodextrin) in clear liquid.
- Given 2 hours before anesthesia induction.
- Benefits: ↓ thirst, hunger, anxiety; ↓ PONV; preserves muscle.
- Improves patient comfort & glycemic control.
⭐ Preoperative CHO loading can reduce postoperative insulin resistance by up to 50%.
- Caution: Gastroparesis, severe reflux, emergency surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Clear fluids (water, pulp-free juice) allowed up to 2 hours before surgery.
- Solids (light meal) permitted up to 6 hours before surgery.
- Preoperative carbohydrate drinks (e.g., maltodextrin) 2 hours preoperatively reduce insulin resistance.
- Prolonged fasting offers no benefit; increases PONV and insulin resistance.
- Infants: breast milk 4 hours, formula 6 hours fasting.
- Goal: Enhance patient comfort, reduce catabolic state, improve glycemic control.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more