Vasodilators Overview - Pressure Plungers
- Mechanism: Relax vascular smooth muscle → ↓ vascular resistance (SVR), ↓ venous tone.
- Hemodynamic Goals:
- Afterload Reduction: ↓ resistance to LV ejection.
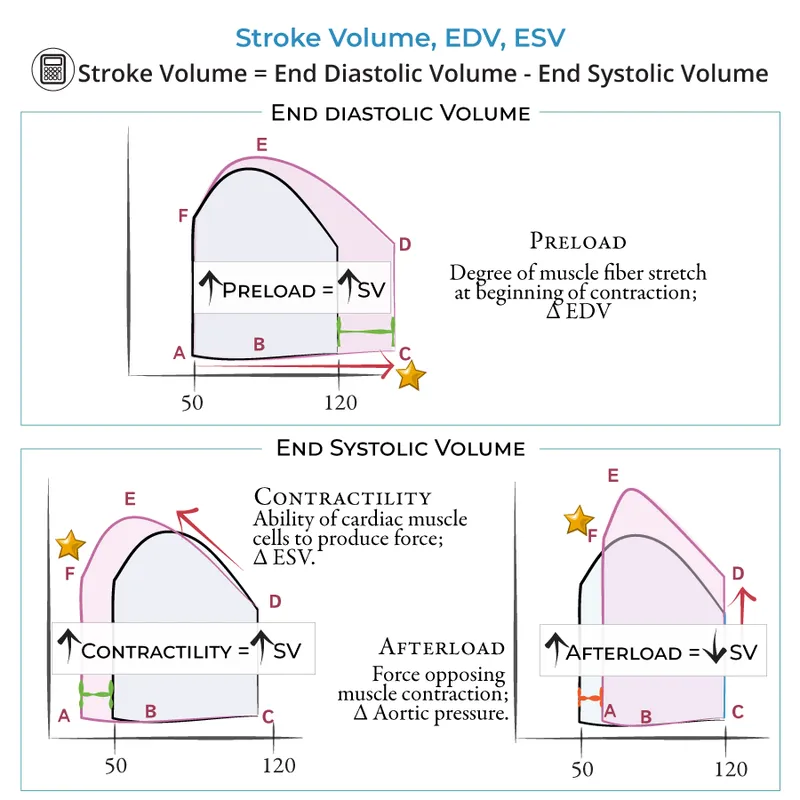
- Benefits: ↓ myocardial oxygen demand ($MVO_2$), ↑ stroke volume.
- Indications: Hypertension, LV dysfunction, valvular regurgitation.
- Preload Reduction: ↓ venous return & ventricular filling pressures.
- Benefits: ↓ myocardial wall stress, ↓ pulmonary congestion.
- Indications: Heart failure, fluid overload.
- Afterload Reduction: ↓ resistance to LV ejection.
- Key Types:
- Arterial dominant (e.g., Hydralazine)
- Venous dominant (e.g., Nitroglycerin - low dose)
- Mixed (e.g., Sodium Nitroprusside, ACEIs)
- Calcium Channel Blockers (CCBs) (e.g., Nicardipine)
⭐ Sodium Nitroprusside (SNP) is a potent arterial and venous vasodilator; monitor for cyanide toxicity with prolonged use or high doses, especially in renal impairment.
Nitrovasodilators - The NO Donors
- Release Nitric Oxide (NO) → ↑cyclic GMP (cGMP) → vascular smooth muscle relaxation → vasodilation.
- Nitroglycerin (NTG):
- Primarily venodilator (↓preload); coronary artery dilator. 💡Reduces myocardial O2 demand.
- Uses: Angina, acute MI, CHF, controlled hypotension.
- Dose: IV infusion 5-200 mcg/min.
- ⚠️ Tachyphylaxis common with prolonged use (>24-48h). Side effects: Headache, hypotension, reflex tachycardia.
- Sodium Nitroprusside (SNP):
- Potent, direct, balanced arterial & venous dilator (↓preload & ↓afterload).
- Uses: Hypertensive emergencies, acute aortic regurgitation, controlled hypotension, severe CHF.
- Dose: IV infusion 0.3-2 mcg/kg/min (max 10 mcg/kg/min for <10 minutes).
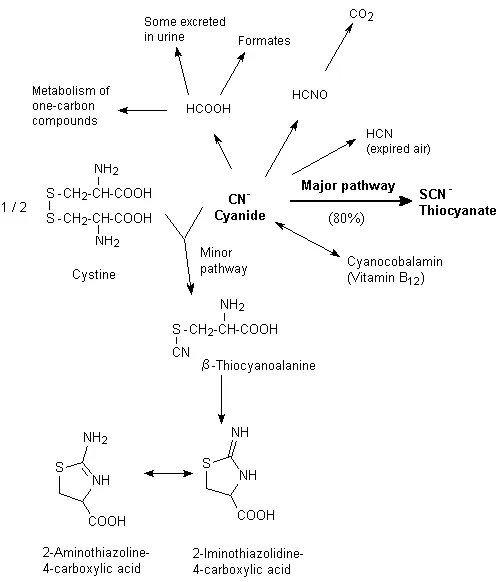
- ⚠️ Cyanide Toxicity: Risk with doses >2 mcg/kg/min, prolonged infusions (>24-48h), or renal impairment.
- Features: Unexplained metabolic acidosis, arrhythmias, ↑mixed venous O2 saturation (SvO2) (tissue hypoxia).
- Antidotes: Sodium thiosulfate, hydroxocobalamin.
- Protect from light. Thiocyanate toxicity (slower onset, with renal failure): confusion, psychosis.
⭐ SNP provides rapid, potent, and balanced vasodilation but carries a significant risk of cyanide toxicity, particularly at infusion rates >2 mcg/kg/min or with renal dysfunction.
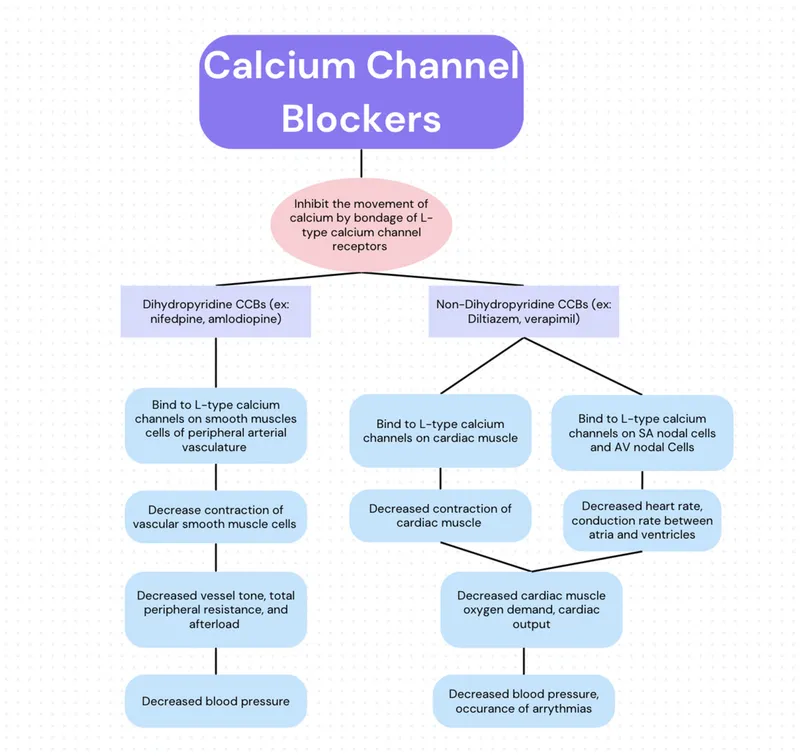
Calcium Channel Blockers - Calcium Controllers
- Mechanism: Block L-type Ca²⁺ channels in vascular smooth muscle → ↓ intracellular Ca²⁺ → smooth muscle relaxation → vasodilation.
- Primary Effect: Arterial vasodilation → ↓ Systemic Vascular Resistance (SVR) & ↓ Blood Pressure (BP).
- Key IV Agents (Dihydropyridines):
- Nicardipine:
- Arterial > venous dilator.
- Onset: 5-15 min; Duration: 1-4 hrs.
- Useful for sustained BP control.
- Clevidipine:
- Ultra-short acting; metabolized by blood/tissue esterases.
- Onset: 2-4 min; Half-life: ~1 min.
- Dosing: Start 1-2 mg/hr IV, titrate q 90s by doubling dose; max 16 mg/hr (briefly up to 32 mg/hr).
- ⚠️ Lipid emulsion: Caution in severe egg/soy allergy, defective lipid metabolism (e.g., pancreatitis, hyperlipidemia).
- Nicardipine:
⭐ Clevidipine's rapid onset and offset allow for precise, beat-to-beat BP management, especially valuable in cardiac surgery for acute hypertension control during critical periods like aortic cannulation or sternotomy.
Other Key Vasodilators - Diverse Dilators
- Milrinone (PDE3 Inhibitor)
- Mechanism: ↑ cAMP → inotropy & vasodilation (arterial & venous).
- Use: Acute HF, cardiogenic shock, weaning from CPB.
- Dose: Loading 25-75 mcg/kg over 10-20 min; Infusion 0.25-0.75 mcg/kg/min.
- Side effects: Hypotension, arrhythmias, thrombocytopenia.
- Hydralazine (Direct Arterial Vasodilator)
- Mechanism: Directly relaxes arterial smooth muscle; minimal venodilation.
- Use: Hypertensive emergencies, afterload reduction in HF.
- Dose: 5-20 mg IV q4-6h.
- Side effects: Reflex tachycardia, lupus-like syndrome (chronic use).
- Fenoldopam (Dopamine D1 Agonist)
- Mechanism: Selective D1 receptor agonist → renal, mesenteric, coronary vasodilation.
- Use: Hypertensive emergencies, renal protection during cardiac surgery (controversial).
- Dose: Infusion 0.01-0.3 mcg/kg/min.
- Side effects: Hypotension, tachycardia, ↑IOP.
⭐ Milrinone is an "inodilator", providing both positive inotropic support and vasodilation, particularly useful in patients with low cardiac output and high systemic vascular resistance after cardiac surgery. It does not rely on beta-receptors, making it effective in patients on beta-blockers. 📌 Remember "Mighty Milly dilates & contracts!"
High‑Yield Points - ⚡ Biggest Takeaways
- Nitroglycerin (NTG): Primarily venodilates, reduces preload; treats myocardial ischemia, hypertension.
- Sodium Nitroprusside (SNP): Balanced arterial/venous dilator (↓preload/↓afterload). Risks: cyanide toxicity, coronary steal.
- Fenoldopam: Selective D1 agonist; renal vasodilation, manages hypertension, offers renal protection.
- Hydralazine: Direct arterial vasodilator (↓afterload); watch for reflex tachycardia.
- CCBs (Nicardipine, Clevidipine): Potent arterial vasodilators for acute hypertension; Clevidipine: ultra-short acting.
- Milrinone (PDE3 inhibitor): Inodilator (vasodilation, ↑contractility); for heart failure, pulmonary hypertension.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

