OPCAB Fundamentals - Heart Beating Feats
Off-Pump Coronary Artery Bypass (OPCAB) is cardiac surgery performed on the native beating heart, avoiding cardiopulmonary bypass (CPB).
- Core Principle: Maintain physiological circulation while enabling coronary anastomosis.
- Key Advantages:
- ↓ Systemic inflammatory response (SIRS)
- ↓ Stroke risk (especially with aortic atheroma/calcification)
- ↓ Renal dysfunction & coagulopathy
- ↓ Need for blood transfusion
- Potentially faster recovery & shorter ICU stay
- Key Disadvantages/Challenges:
- Technically more demanding for surgeon
- Hemodynamic instability during cardiac positioning/stabilization
- Risk of incomplete revascularization
- Possible urgent conversion to CPB
- Patient Selection Considerations:
- Proximal, easily accessible coronary lesions
- Patients with high risk for CPB (e.g., porcelain aorta, severe PVD, prior stroke)
- Elderly or frail patients
⭐ OPCAB significantly reduces neurological complications like stroke, particularly in patients with a heavily calcified ('porcelain') aorta, by avoiding aortic cannulation and cross-clamping associated with CPB.
Anesthetic Blueprint - Guiding the Beat
- Goals: Hemodynamic stability, myocardial protection, early extubation.
- Premedication: Anxiolysis (Midazolam), aspiration prophylaxis. Continue β-blockers.
- Induction:
- Balanced: Opioids (Fentanyl/Sufentanil) + Etomidate/Propofol (cautious).
- Maintain normotension, avoid tachycardia.
- Maintenance:
- Volatiles (Iso/Sevo) or TIVA. High-dose opioids.
- Muscle relaxation.
- Normothermia.
- Monitoring:
- Standard + Invasive BP, CVP.
- TEE: Crucial for RWMA, ventricular function. ⭐
- ACT: Target >250s (if heparinized).
- BIS for depth.
- Key Challenges:
- Heart displacement → Hypotension, arrhythmias.
- Regional ischemia during anastomosis.
⭐ TEE is indispensable for detecting acute regional wall motion abnormalities (RWMA) during coronary anastomosis, guiding immediate surgical or anesthetic intervention.
Intraop Challenges - Navigating Turbulence
- Hemodynamic Instability: Primary challenge from cardiac displacement.
- Causes: ↓ Preload, ↓ CO, hypotension.
- Risks: Arrhythmias (bradycardia, VT/VF), myocardial ischemia (ECG/TEE).
- Anesthetic Responses:
- Surgeon communication: Key.
- Volume optimization; Trendelenburg (transient).
- Vasopressors (e.g., phenylephrine) & inotropes (e.g., dobutamine).
- Severe instability: Request cardiac repositioning.
- Critical Monitoring:
- Continuous invasive BP.
- TEE: Detects RWMA, assesses filling/contractility.
- Multi-lead ECG: ST segment analysis.
- ACT: Maintain target (e.g., >250-300s).
⭐ TEE is invaluable for early detection of regional wall motion abnormalities (RWMA) indicating ischemia during cardiac displacement, often before ECG changes.

Complications & Recovery - The Afterbeat
- Key OPCAB Complications:
- Arrhythmias: Atrial fibrillation (AF) common; manage rate/rhythm.
- Bleeding: Monitor chest drain output (< 100-200 ml/hr).
- Renal: AKI risk; ensure good Mean Arterial Pressure (MAP).
- Respiratory: Atelectasis, effusions. Promote early physiotherapy.
- Neuro: Stroke (↓ incidence vs CPB), Postoperative Cognitive Dysfunction (POCD), delirium.
- Graft failure: Often technical; monitor for signs of ischemia.
- Shivering: Increases $O_2$ demand; warm actively, consider meperidine.
- Pain Control Strategy:
- Multimodal: Opioids (IV/PCA), NSAIDs (cautious use), paracetamol.
- Regional: Paravertebral or Erector Spinae Plane (ESP) blocks aid recovery.
- Goal: Facilitate early mobilization, effective cough, deep breathing.
- Extubation Criteria (Fast-Track):
- Hemodynamics: Stable, minimal/no inotropes or vasopressors.
- Temperature: Normothermic (> 36°C).
- Oxygenation: PaO2 > 60 mmHg on FiO2 ≤ 0.4, PEEP ≤ 5 cmH2O.
- Neurological: Awake, cooperative, adequate muscle strength (e.g., head lift).
- Bleeding: Minimal (< 50 ml/hr) chest tube output.
⭐ Postoperative atrial fibrillation (POAF) is the most common arrhythmia (20-40% in OPCAB), increasing stroke risk and length of stay.
High‑Yield Points - ⚡ Biggest Takeaways
- OPCAB avoids cardiopulmonary bypass (CPB), significantly reducing systemic inflammation, coagulopathy, and stroke.
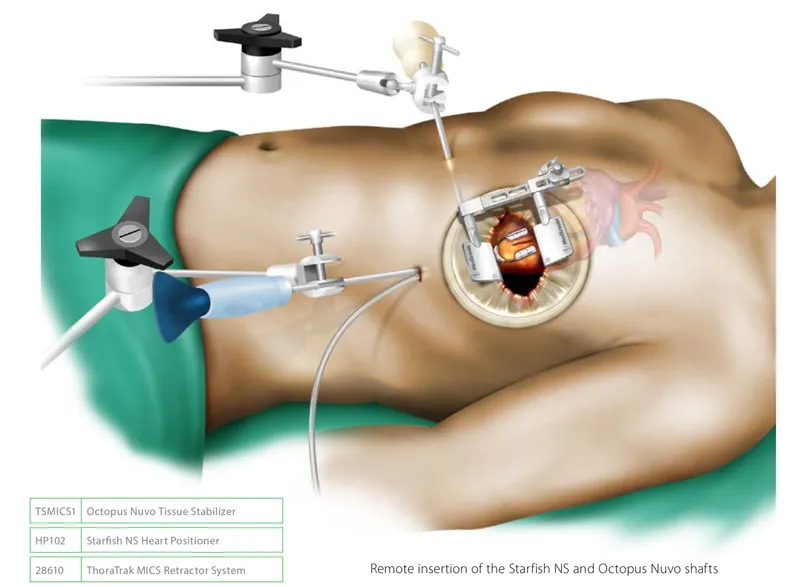
- Mechanical stabilizers (e.g., Octopus, Starfish) are crucial for precise coronary anastomosis on a beating heart.
- Intracoronary shunts are vital to maintain distal myocardial perfusion during grafting.
- Hemodynamic stability is a primary concern; requires meticulous monitoring and proactive management.
- Lower risk of certain complications like renal failure and atrial fibrillation post-surgery.
- Indicated for high-risk patients, such as elderly or those with porcelain aorta or severe comorbidities.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

