Cardiac Cycle & PV Loops - Heart's Beat Dance
- Cardiac Cycle (~0.8s): Rhythmic mechanical & electrical events.
- Systole (ventricular contraction, ~0.3s):
- Isovolumetric Contraction: All valves closed, LV pressure ↑ rapidly.
- Ejection: Aortic valve opens, blood ejected.
- Diastole (ventricular relaxation, ~0.5s):
- Isovolumetric Relaxation: All valves closed, LV pressure ↓ rapidly.
- Ventricular Filling: Mitral valve opens, LV fills.
- Heart Sounds: S1 (mitral/tricuspid closure), S2 (aortic/pulmonary closure).
- Systole (ventricular contraction, ~0.3s):
- Pressure-Volume (PV) Loop: Plots LV pressure vs. LV volume for one beat.
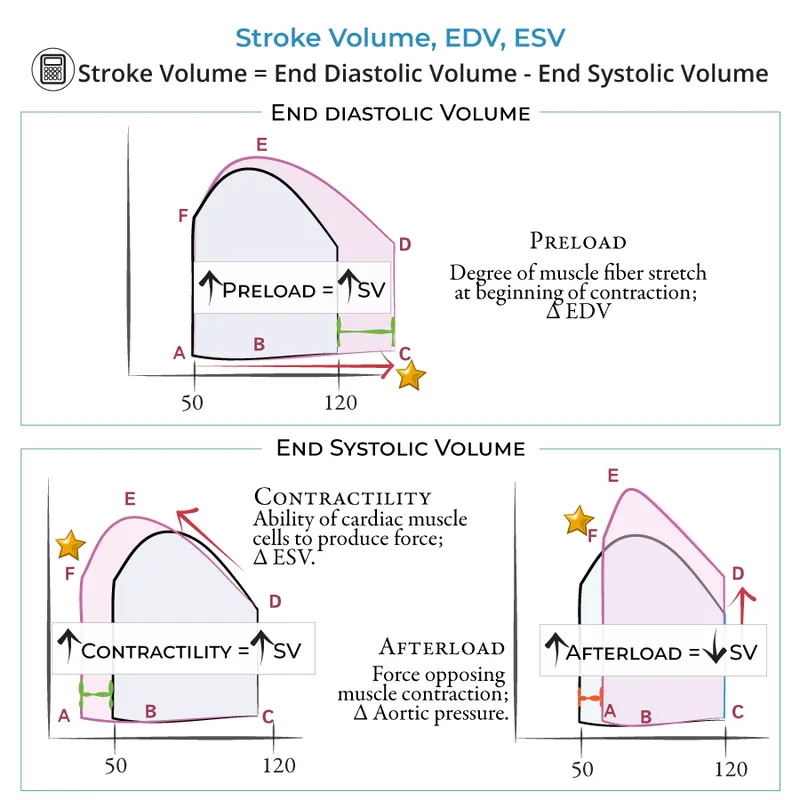
- Width of loop = Stroke Volume ($SV = EDV - ESV$).
- Area within loop = LV Stroke Work.
- Corners represent valve opening/closing points.
⭐ The dicrotic notch (incisura) on the aortic pressure wave, occurring after S2, is caused by the brief backflow of blood into the left ventricle just before aortic valve closure, leading to a transient increase in aortic pressure.
Myocardial Mechanics - Pump Power & Stretch
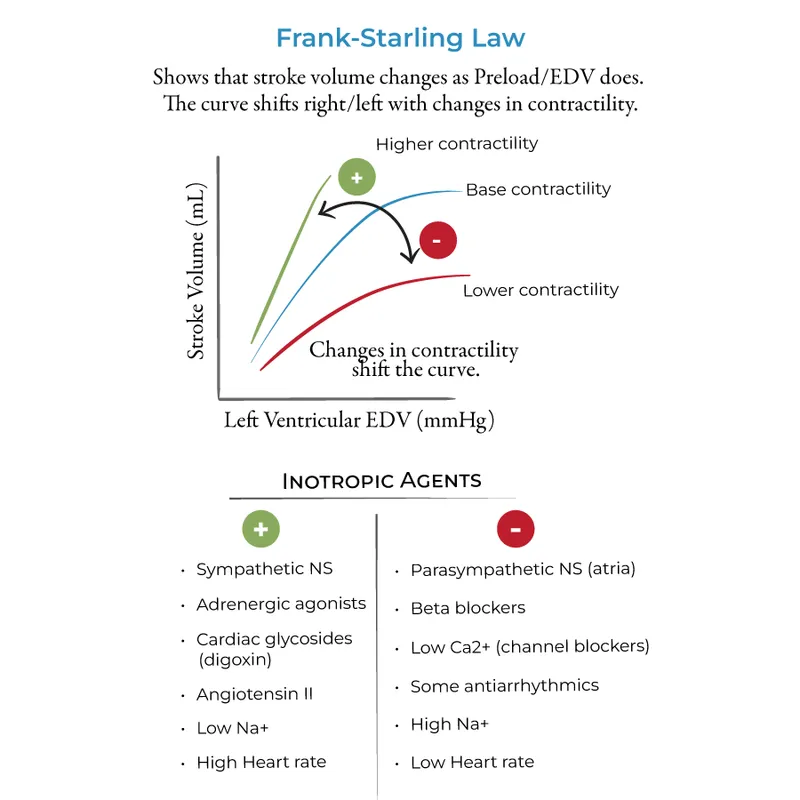
- Frank-Starling Mechanism (Preload/Stretch):
- ↑ End-Diastolic Volume (EDV) → ↑ myocardial stretch → ↑ force of contraction (length-dependent activation).
- Mechanism: Optimal actin-myosin filament overlap.
- Foundation for preload management & fluid responsiveness assessment.
- Contractility (Inotropy - Pump Power):
- Myocardium's intrinsic contractile strength; independent of preload/afterload.
- Positive inotropes (e.g., catecholamines, dobutamine, milrinone) ↑ contractility.
- Negative inotropes (e.g., β-blockers, Ca²⁺ channel blockers, severe acidosis, hypoxia) ↓ contractility.
- Afterload:
- Force opposing ventricular ejection (e.g., Systemic Vascular Resistance (SVR) for LV; Pulmonary Vascular Resistance (PVR) for RV).
- Governed by Laplace's Law: Wall Tension $T alsuccessor (P imes r) / (2h)$ (P=pressure, r=radius, h=wall thickness).
- ↑ Afterload → ↓ Stroke Volume (if other factors constant).
⭐ Contractility is best assessed clinically by $dP/dt_{max}$ (maximum rate of ventricular pressure rise during isovolumetric contraction).
Hemodynamic Harmony - Flow, Force, Fill
- Flow (Cardiac Output, CO): Blood pumped/min. $CO = HR \times SV$. Normal: 5-6 L/min.
- HR: Beats/min.
- SV: Volume/beat. 📌 Mnemonic: "PAC" (Preload, Afterload, Contractility).
- Fill (Preload): End-diastolic volume (EDV)/stretch. Frank-Starling: ↑Preload → ↑SV. From Venous Return.
- Force (Afterload): Ejection resistance (mainly SVR). ↑Afterload → ↓SV.
- Contractility: Myocardial pump strength.
- Systemic Vascular Resistance (SVR): Resistance in systemic arteries.
- $SVR = [(MAP - CVP) / CO] \times 80$. Normal: 800-1200 dynes.sec/cm⁵.
- Mean Arterial Pressure (MAP): $MAP \approx CO \times SVR$.
⭐ > Arteriolar radius is key to SVR. Poiseuille's Law ($R \propto 1/r^4$): small radius changes → large SVR & BP changes.
Coronary Circulation - Heart's Fuel Line

- Origin: Left Coronary Artery (LCA) & Right Coronary Artery (RCA) from aortic sinuses.
- Major Arteries & Supply:
- LCA → Left Anterior Descending (LAD): Anterior wall, septum, apex.
- LCA → Circumflex (LCx): Lateral, posterior LV walls.
- RCA → Supplies RV, SA/AV nodes; Posterior Descending Artery (PDA) in ~70% (right dominance) supplies inferior wall, posterior septum.
- Blood Flow Dynamics:
- LV: Predominantly during diastole (systolic compression limits flow).
- RV: Throughout cardiac cycle (lower wall tension).
- Coronary Perfusion Pressure (CPP): $CPP = AoDP - LVEDP$. (AoDP: Aortic Diastolic Pressure; LVEDP: Left Ventricular End-Diastolic Pressure).
- Autoregulation: Maintains constant flow despite MAP changes (60-140 mmHg).
- Myocardial O2 Extraction: Highest in body (~70-80% at rest); increased O2 demand primarily met by increased coronary blood flow.
⭐ The subendocardium of the left ventricle is most vulnerable to ischemia due to higher systolic wall stress and greater distance from epicardial arteries, receiving flow mainly in diastole.
High‑Yield Points - ⚡ Biggest Takeaways
- Coronary Perfusion Pressure (CPP) = DBP - LVEDP; crucial for myocardial oxygen supply.
- Key determinants of myocardial oxygen demand: heart rate, contractility, wall stress.
- Frank-Starling Law: Increased preload (within limits) boosts stroke volume.
- Bainbridge Reflex: ↑ atrial filling (CVP) leads to ↑ heart rate.
- Bezold-Jarisch Reflex: Ventricular stimuli trigger bradycardia, hypotension, and vasodilation.
- Pulmonary Vascular Resistance (PVR) is minimal at Functional Residual Capacity (FRC).
- Hypoxic Pulmonary Vasoconstriction (HPV) diverts blood from hypoxic alveoli, improving V/Q matching.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

