Cardiovascular Anesthesia

On this page
🎯 Cardiovascular Anesthesia: The Cardiac Operating Theater
Cardiovascular anesthesia demands split-second decisions where hemodynamic precision separates success from catastrophe. You'll master the monitoring systems that reveal real-time cardiac function, build a pharmacologic arsenal for manipulating preload, afterload, and contractility, and learn risk stratification tools that predict which patients will decompensate. Through systematic algorithms and multi-system integration strategies, you'll develop the clinical judgment to orchestrate complex cases-from routine valve replacements to emergent aortic dissections-with confidence and control.
Cardiovascular anesthesia represents the pinnacle of perioperative medicine, requiring mastery of cardiac physiology, advanced monitoring techniques, complex pharmacology, and intricate surgical procedures. Every decision impacts myocardial oxygen supply-demand balance, systemic perfusion, and patient outcomes.
📌 Remember: CARDIAC - Coronary perfusion, Afterload management, Rhythm control, Drug interactions, Ischemia prevention, Anticoagulation, Cardiopulmonary bypass
The cardiac anesthesiologist must understand how anesthetic agents affect cardiac contractility, vascular tone, and conduction systems while managing complex comorbidities. Mortality rates for cardiac surgery range from 1-3% for elective procedures to 15-25% for emergency operations, making precise anesthetic management crucial.
⭐ Clinical Pearl: Cardiac output decreases by 20-40% with most volatile anesthetics, requiring careful titration and hemodynamic support in patients with compromised ventricular function.
| Parameter | Normal Range | Critical Threshold | Intervention Point | Monitoring Method | Clinical Significance |
|---|---|---|---|---|---|
| CVP | 2-8 mmHg | >15 mmHg | >12 mmHg | Central line | Preload assessment |
| PCWP | 6-12 mmHg | >18 mmHg | >15 mmHg | Swan-Ganz | LV filling pressure |
| CI | 2.5-4.0 L/min/m² | <2.0 L/min/m² | <2.2 L/min/m² | Thermodilution | Cardiac performance |
| SVR | 800-1200 dynes | >1500 dynes | >1400 dynes | Calculated | Afterload |
| SvO₂ | 65-75% | <60% | <65% | Mixed venous | O₂ supply/demand |
- Functional capacity evaluation using METs (>4 METs indicates good reserve)
- Cardiac catheterization data: EF <40% increases perioperative risk 3-fold
- Stress testing: >1mm ST depression suggests significant CAD
- Exercise tolerance: <4 METs predicts complications
- Pharmacologic stress: Dobutamine preferred in β-blocked patients
- Nuclear imaging: Reversible defects indicate viable myocardium
💡 Master This: Perioperative β-blockade reduces cardiac events by 30% when started >7 days preoperatively in high-risk patients, but increases stroke risk if initiated <24 hours before surgery.
Understanding cardiovascular anesthesia principles enables prediction of hemodynamic responses and guides therapeutic interventions throughout the perioperative period.
🎯 Cardiovascular Anesthesia: The Cardiac Operating Theater
⚡ Hemodynamic Command Center: Monitoring Mastery
📌 Remember: FRANK-STARLING - Filling pressure determines, Return affects preload, Afterload opposes ejection, Neurohormonal activation, Kinetic energy transfer, Stroke volume optimization, Timing of interventions, Arrhythmia effects, Regional wall motion, Length-tension relationship, Inotropic state, Nitric oxide effects, Gradient-driven flow
| Monitoring Method | Parameters | Normal Values | Accuracy | Invasiveness | Clinical Applications |
|---|---|---|---|---|---|
| Arterial Line | BP, SVV, PPV | MAP 65-100 | ±2 mmHg | Moderate | Beat-to-beat BP, blood sampling |
| CVP | RAP, trends | 2-8 mmHg | ±2 mmHg | Moderate | Preload assessment, fluid status |
| Swan-Ganz | CO, PCWP, SVR | CI 2.5-4.0 | ±10% | High | Complex hemodynamics |
| TEE | EF, wall motion | EF >55% | ±5% | Moderate | Real-time cardiac function |
| FloTrac | CO, SVV | CI 2.5-4.0 | ±15% | Low | Minimally invasive CO |
- Pulse pressure variation >13% predicts fluid responsiveness with 85% accuracy
- Stroke volume variation >10% indicates preload dependence
- Mixed venous oxygen saturation <65% suggests inadequate oxygen delivery
- Central venous O₂ saturation typically 3-5% higher than mixed venous
- Lactate levels >2 mmol/L indicate tissue hypoperfusion
- Base deficit >-5 mEq/L suggests significant metabolic acidosis
⭐ Clinical Pearl: TEE provides real-time assessment of ventricular function, with Grade 4 wall motion abnormalities indicating >50% reduction in regional contractility and requiring immediate intervention.
💡 Master This: Dynamic parameters (SVV, PPV) are superior to static parameters (CVP, PCWP) for predicting fluid responsiveness, with >90% accuracy in mechanically ventilated patients with normal sinus rhythm.
The integration of multiple monitoring modalities creates a comprehensive hemodynamic picture, enabling precise management of complex cardiac patients and optimization of perioperative outcomes.
⚡ Hemodynamic Command Center: Monitoring Mastery
🧬 Cardiac Pharmacology Arsenal: Drug Precision Targeting
📌 Remember: RECEPTORS - Renin-angiotensin effects, Epinephrine α/β actions, Calcium channel blocking, Endothelial NO release, Phosphodiesterase inhibition, Thromboxane synthesis, Opioid receptor binding, Ryanodine channel effects, Sodium channel blockade
| Drug Class | Mechanism | Onset | Duration | Hemodynamic Effects | Clinical Applications |
|---|---|---|---|---|---|
| β-Blockers | β₁/β₂ antagonism | 2-5 min | 3-6 hours | ↓HR, ↓BP, ↓CO | Rate control, ischemia prevention |
| Vasodilators | Various | 1-3 min | 15-60 min | ↓SVR, ↓BP | Afterload reduction |
| Inotropes | β₁ agonism | 1-2 min | 5-10 min | ↑CO, ↑HR | Low output states |
| Vasopressors | α₁ agonism | <1 min | 2-5 min | ↑SVR, ↑BP | Hypotension, shock |
| Antiarrhythmics | Na⁺/K⁺ channels | 2-15 min | 6-24 hours | Variable | Rhythm control |
- Dobutamine: 2.5-15 μg/kg/min, primarily β₁ agonist, increases contractility 30-50%
- Milrinone: 0.375-0.75 μg/kg/min, PDE-III inhibitor, improves diastolic function
- Epinephrine: 0.01-0.1 μg/kg/min, mixed α/β effects, dose-dependent responses
- Low dose (<0.05 μg/kg/min): predominantly β effects
- High dose (>0.1 μg/kg/min): α effects predominate
- Increases myocardial oxygen consumption by 15-25%
⭐ Clinical Pearl: Milrinone provides lusitropic effects (improved relaxation) independent of β-receptors, making it ideal for patients with β-blockade or receptor downregulation.
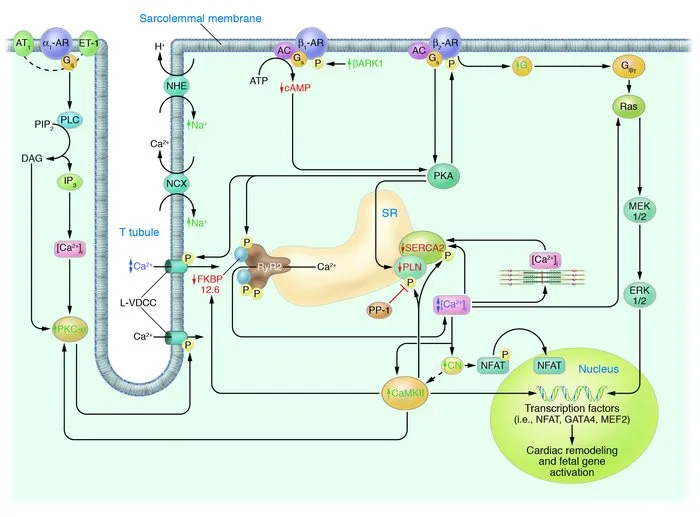
- Vasodilator Precision
- Nitroglycerin: 0.5-10 μg/kg/min, venous > arterial dilation, reduces preload 20-40%
- Nicardipine: 5-15 mg/hour, calcium channel blocker, coronary vasodilation
- Clevidipine: 1-32 mg/hour, ultra-short acting, t½ = 1 minute
- Metabolized by plasma esterases, predictable offset
- No renal or hepatic metabolism required
- Reduces afterload without reflex tachycardia
💡 Master This: Vasodilator selection depends on primary pathophysiology: nitroglycerin for preload reduction in heart failure, nicardipine for controlled hypotension, clevidipine for precise BP control with rapid reversibility.
Understanding cardiovascular pharmacology enables rational drug selection and dosing strategies, optimizing hemodynamic management while minimizing adverse effects and drug interactions.
🧬 Cardiac Pharmacology Arsenal: Drug Precision Targeting
🔍 Perioperative Risk Stratification: The Prediction Matrix
📌 Remember: RISK SCORES - Revised cardiac risk index, Institutional factors, Surgical complexity, Kidney function (creatinine), Stress testing results, Clinical presentation, Objective measures, Recent events, Ejection fraction, Symptom severity
| Risk Score | Variables | Low Risk | Intermediate | High Risk | Mortality Prediction |
|---|---|---|---|---|---|
| RCRI | 6 factors | 0-1 points | 2 points | ≥3 points | 0.4%, 0.9%, 6.6% |
| EuroSCORE II | 18 variables | <2% | 2-5% | >5% | Logistic model |
| STS Score | 40+ variables | <1% | 1-3% | >3% | 30-day mortality |
| NSQIP | 21 factors | <1% | 1-5% | >5% | Morbidity/mortality |
| METS | Functional | >10 METs | 4-10 METs | <4 METs | Exercise tolerance |
- High-risk surgery (intraperitoneal, intrathoracic, suprainguinal vascular)
- Ischemic heart disease (MI, positive stress test, chest pain with ischemia)
- Congestive heart failure (clinical CHF, pulmonary edema, S3 gallop, CXR findings)
- Cerebrovascular disease (TIA, stroke)
- Diabetes mellitus requiring insulin therapy
- Chronic kidney disease (creatinine >2.0 mg/dL)
⭐ Clinical Pearl: Patients with ≥3 RCRI factors have >6% risk of major cardiac events, warranting intensive perioperative monitoring and possible preoperative optimization.
- Biomarker Integration
- Troponin elevation >0.03 ng/mL increases 30-day mortality 3-fold
- BNP >100 pg/mL or NT-proBNP >300 pg/mL predicts cardiac events
- Creatinine >1.5 mg/dL doubles perioperative mortality risk
- eGFR <60 mL/min/1.73m² requires dose adjustments
- Proteinuria indicates increased cardiovascular risk
- Cystatin C provides more accurate GFR estimation
💡 Master This: Preoperative troponin elevation, even without clinical symptoms, increases perioperative cardiac event risk by 300% and warrants cardiology consultation and optimization.
Risk stratification enables personalized perioperative care plans, optimizing resource allocation while improving patient outcomes through targeted interventions and monitoring strategies.
🔍 Perioperative Risk Stratification: The Prediction Matrix
⚖️ Anesthetic Management Algorithms: Precision Protocol Navigation
📌 Remember: INDUCTION - Intravenous access secured, Nitrous oxide avoided, Dose reduction needed, Unstable hemodynamics anticipated, Cardiac output preserved, Timing coordinated, Inotropes ready, Oxygen delivery maintained, Narcotics titrated
| Anesthetic Phase | Goals | Monitoring | Drug Choices | Hemodynamic Targets | Complications |
|---|---|---|---|---|---|
| Induction | Smooth transition | A-line, 5-lead ECG | Etomidate, fentanyl | MAP >65, HR <100 | Hypotension, arrhythmias |
| Maintenance | Hemodynamic stability | TEE, Swan-Ganz | Isoflurane, sufentanil | CI >2.0, SVR 800-1200 | Ischemia, bleeding |
| CPB | Organ protection | ACT, blood gases | Propofol, midazolam | Flow >2.4 L/min/m² | Emboli, inflammation |
| Separation | Cardiac function | Mixed venous O₂ | Inotropes, vasodilators | PCWP <18, CI >2.2 | Low output, arrhythmias |
| Emergence | Controlled awakening | Neurologic exam | Reversal agents | Stable hemodynamics | Hypertension, bleeding |
- High-dose opioid technique: Sufentanil 10-30 μg/kg provides hemodynamic stability
- Balanced technique: Fentanyl 10-50 μg/kg with volatile agents for faster emergence
- Etomidate 0.1-0.3 mg/kg: minimal cardiovascular depression, ideal for unstable patients
- Maintains cardiac output and blood pressure
- May cause adrenal suppression with single dose
- Preferred in patients with severe LV dysfunction
⭐ Clinical Pearl: Avoid succinylcholine in patients with recent MI (<72 hours) due to risk of hyperkalemia from muscle membrane changes, potentially causing cardiac arrest.
- Maintenance Protocols
- Volatile agents: 0.5-1.5 MAC with opioid supplementation
- TIVA: Propofol 50-150 μg/kg/min with sufentanil 0.5-2 μg/kg/hour
- Muscle relaxation: Vecuronium 0.1 mg/kg or rocuronium 0.6 mg/kg
- Avoid pancuronium in CAD patients (tachycardia risk)
- Cisatracurium preferred in renal/hepatic dysfunction
- Monitor neuromuscular function with TOF ratio >0.9
💡 Master This: Fast-track cardiac anesthesia uses lower opioid doses (fentanyl <20 μg/kg) and shorter-acting agents to enable same-day extubation, reducing ICU stay by 24-48 hours without increasing complications.
Systematic anesthetic protocols ensure consistent, high-quality care while enabling rapid response to hemodynamic changes and surgical complications throughout the perioperative period.
⚖️ Anesthetic Management Algorithms: Precision Protocol Navigation
🔗 Advanced Integration: Multi-System Orchestration
📌 Remember: INTEGRATION - Inflammatory response, Neurologic protection, Tissue perfusion, Endothelial function, Glycemic control, Renal preservation, Anticoagulation balance, Temperature management, Immune modulation, Oxygen delivery, Nutritional support
| System Integration | Monitoring | Targets | Interventions | Outcomes | Evidence Level |
|---|---|---|---|---|---|
| Cardiopulmonary | TEE, Swan-Ganz | CI >2.2, PCWP <18 | Inotropes, IABP | Reduced LOS | Class I |
| Neurologic | NIRS, EEG | rSO₂ >50%, BIS 40-60 | Cerebral perfusion | Stroke prevention | Class IIa |
| Renal | Creatinine, UOP | UOP >0.5 mL/kg/hr | Goal-directed therapy | AKI reduction | Class I |
| Coagulation | TEG, ACT | ACT >480s on CPB | Heparin, protamine | Bleeding control | Class I |
| Metabolic | Glucose, lactate | Glucose 140-180 mg/dL | Insulin protocols | Infection reduction | Class I |
- Myocardial protection: Cold blood cardioplegia reduces enzyme release by 60%
- Cerebral protection: NIRS monitoring detects desaturation >20% from baseline
- Renal protection: Goal-directed therapy reduces AKI incidence by 35%
- Maintain MAP >65 mmHg during CPB
- Avoid nephrotoxic agents (NSAIDs, aminoglycosides)
- Consider RIPC (remote ischemic preconditioning)
⭐ Clinical Pearl: Tight glycemic control (140-180 mg/dL) reduces deep sternal wound infections by 50% without increasing hypoglycemia risk, using insulin protocols with hourly glucose monitoring.
- Precision Medicine Applications
- Pharmacogenomics: CYP2D6 polymorphisms affect codeine metabolism
- Biomarker-guided therapy: Troponin trends guide intervention timing
- Personalized anticoagulation: Factor V Leiden affects heparin response
- APOE4 genotype increases stroke risk 2-fold
- SLCO1B1 variants affect statin myopathy risk
- CYP2C19 polymorphisms influence clopidogrel efficacy
💡 Master This: Enhanced recovery protocols combining multimodal analgesia, early mobilization, and optimized fluid management reduce hospital stay by 2-3 days and complications by 30% in cardiac surgery patients.
Advanced integration strategies enable personalized perioperative care, optimizing multiple organ systems simultaneously while incorporating cutting-edge technologies and evidence-based protocols for superior patient outcomes.
🔗 Advanced Integration: Multi-System Orchestration
🎯 Clinical Mastery Toolkit: Rapid Decision Framework
📌 Remember: MASTERY - Monitor continuously, Anticipate problems, Systematic approach, Team communication, Evidence-based decisions, Rapid interventions, Yield optimization
| Clinical Scenario | Recognition | Immediate Action | Drug/Dose | Monitoring | Success Criteria |
|---|---|---|---|---|---|
| Acute hypotension | MAP <65 mmHg | Fluid/vasopressor | Phenylephrine 100-200 μg | A-line, UOP | MAP >65 mmHg |
| Low cardiac output | CI <2.0 L/min/m² | Inotropic support | Dobutamine 5-15 μg/kg/min | Swan-Ganz, TEE | CI >2.2 L/min/m² |
| Myocardial ischemia | ST changes >1mm | Optimize supply/demand | Nitroglycerin 0.5-2 μg/kg/min | 12-lead ECG | ST resolution |
| Severe bleeding | >150 mL/15min | Hemostasis protocol | Protamine 1:1 ratio | ACT, TEG | ACT <150s |
| Arrhythmias | Sustained VT/VF | ACLS protocol | Amiodarone 150 mg | Defibrillator | Sinus rhythm |
- Hypotension Algorithm: Assess volume status → vasopressor vs. inotrope → dose titration
- Ischemia Protocol: Increase oxygen supply → decrease demand → anticoagulation
- Bleeding Management: Surgical control → reversal agents → blood products
- Massive transfusion: 1:1:1 ratio (RBC:FFP:platelets)
- Factor concentrates: PCC 25-50 units/kg for warfarin reversal
- Antifibrinolytics: TXA 1g loading, then 1g over 8 hours
⭐ Clinical Pearl: The "Rule of 30s" - MAP <30 mmHg below baseline, urine output <30 mL/hour, or lactate >3.0 mmol/L indicates inadequate perfusion requiring immediate intervention.
- Rapid Assessment Framework
- ABC-D approach: Airway, Breathing, Circulation, Drugs/Devices
- POCUS integration: Point-of-care ultrasound for immediate diagnosis
- Team communication: SBAR format (Situation, Background, Assessment, Recommendation)
- Closed-loop communication: Confirm all orders verbally
- Crisis resource management: Designate roles clearly
- Debriefing protocols: Review critical events within 24 hours
💡 Master This: Successful cardiovascular anesthesia requires anticipatory management - predicting hemodynamic changes 2-3 steps ahead and having interventions ready before problems become critical, reducing morbidity by 40%.
The clinical mastery toolkit provides systematic approaches to complex scenarios, enabling rapid recognition, immediate intervention, and optimal outcomes in cardiovascular anesthesia practice.
🎯 Clinical Mastery Toolkit: Rapid Decision Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























