Breathing Systems Basics - Circuit Central
- Core Components:
- Fresh Gas Source (FGS): Gases/O2 input.
- Delivery Tubes: Inspiratory/expiratory.
- Reservoir Bag: Tidal volume, manual/spontaneous ventilation.
- APL Valve: Pressure limit, excess gas vent.
- Patient Connection: Mask/ETT/LMA.
and classification overview)
- Classification:
| System Type | Rebreathing | CO2 Absorption | Example(s) |
|---|---|---|---|
| Open | No | No | Open drop |
| Semi-Open | Minimal/No | No | Mapleson A,D |
| Semi-Closed | Partial | Yes | Circle (low) |
| Closed | Total | Yes | Circle (min) |
Mapleson Circuits - Alphabet Soup Fun
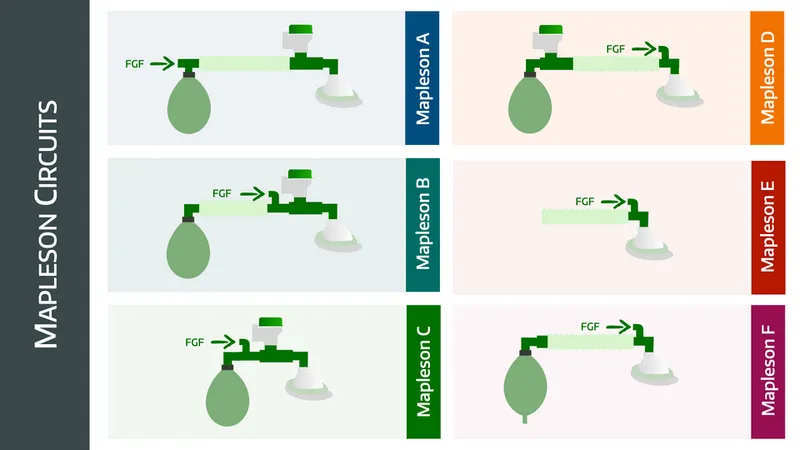
| Circuit | Components | FGF (SV) | FGF (CV) | Efficiency (SV) | Efficiency (CV) | Best Use | Notes |
|---|---|---|---|---|---|---|---|
| Mapleson A (Magill) | FGF, CT, RB, APL (pt end) | $FGF = MV$ | High, 2-3x MV | Most efficient | Least efficient | Adults, SV | APL near patient. |
| Mapleson D | FGF (pt), CT, RB, APL (mach end) | 2-3x MV | 1-2x MV ($70 \text{ ml/kg/min}$) | Good | Most efficient | All ages, SV & CV | Bain: coaxial D. Test inner tube. |
| Mapleson E (Ayre's T) | FGF (pt), CT (exp limb) | 2-3x MV | 2-3x MV | Good | Good | Peds < 25 kg, SV | No RB/APL. Low dead space/resistance. |
| Mapleson F (Jackson-Rees) | FGF (pt), CT, open RB | 2-3x MV | 2-3x MV | Good | Good | Peds, SV & CV | Mod of E. Allows CPAP/PEEP. |
- 📌 Efficiency (CV): 'Dead Babies Can't Assist' (D > B > C > A)
⭐ The Bain circuit, a coaxial Mapleson D, requires integrity testing of the inner fresh gas delivery tube to prevent rebreathing of exhaled gases if it becomes kinked or disconnected.
Circle System - Round & Round We Go
Most common system; allows rebreathing of gases after CO₂ removal.
Components:
- CO₂ absorber (Soda lime)
- Unidirectional inspiratory & expiratory valves
- APL (Adjustable Pressure Limiting) valve
- Reservoir bag
- Y-piece
- Fresh Gas Flow (FGF) inlet
- Corrugated breathing tubes
CO₂ Absorption (Soda Lime):
- Reactions: $CO_2 + 2NaOH \rightarrow Na_2CO_3 + H_2O + Heat$; then $Na_2CO_3 + Ca(OH)_2 \rightarrow CaCO_3 \text{ (s)} + 2NaOH$.
- Granule size: 4-8 mesh.
- Indicator: Ethyl violet (Pink → Violet). 📌 "Violet is Violating" (CO₂ rebreathing).
Advantages:
- Low FGF: Conserves gases & agents.
- Conserves heat & humidity.
- ↓ Operating room pollution.
- Suitable for all patient ages.
Disadvantages:
- Complex; many parts, ↑ failure risk.
- ↑ Resistance to breathing.
- Rebreathing risk (valve/absorber failure).
- Compound A formation (Sevoflurane + dry absorbent).
Simplified Pre-Use Check:
⭐ Channeling in the CO₂ absorber canister can lead to premature exhaustion and rebreathing of CO₂ despite color change indicating otherwise in parts of the absorbent.
Safety & Monitoring - Vigilant Vents
- Hazards: Leaks, disconnections, obstructions, barotrauma, volutrauma, hypoxia, hypercarbia.
- Key Monitoring:
- Airway pressures (Peak, Plateau, PEEP).
- Capnography (ETCO2: normal 35-45 mmHg).
- Inspired O2 (FiO2).
- Spirometry (VT, MV).
- Alarms: Low/High pressure, Apnea.
- Scavenging: Active/passive systems for Waste Anesthetic Gas Disposal (WAGD).

⭐ A sudden drop in ETCO2 to near zero can indicate esophageal intubation, circuit disconnection, or cardiac arrest.
High‑Yield Points - ⚡ Biggest Takeaways
- Mapleson A (Magill) is best for spontaneous ventilation; Mapleson D for controlled ventilation.
- The Bain circuit is a coaxial Mapleson D; check inner tube integrity.
- Circle systems enable low FGF, conserve heat/humidity, and need CO2 absorption.
- Key circle components: unidirectional valves, APL valve, CO2 absorber.
- Minimize apparatus dead space for efficient ventilation and to prevent rebreathing.
- Soda lime exhaustion: color change (ethyl violet), ↑ETCO2, ↑HR, ↑BP.
- Adequate Fresh Gas Flow (FGF) prevents rebreathing in Mapleson systems.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

