Anesthesia for Interventional Radiology - Suite Spot Secrets
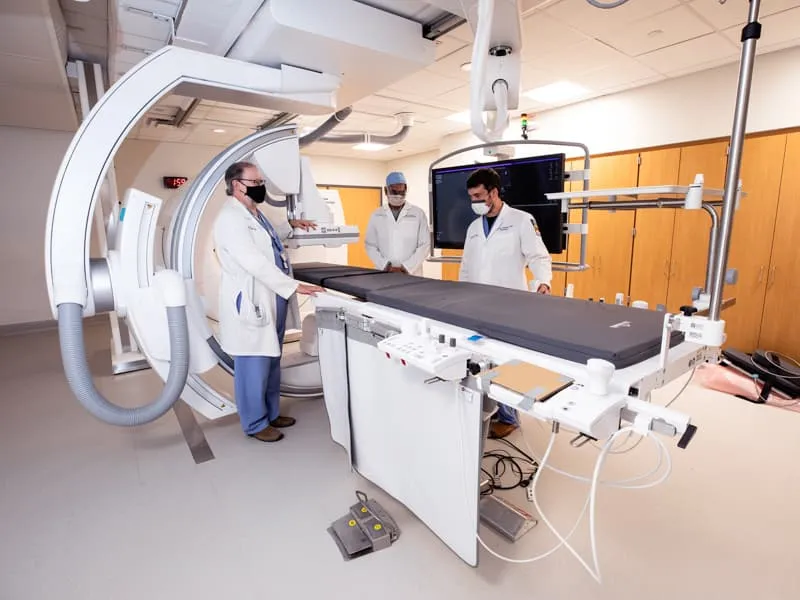
- NORA Challenges: Remote location, unfamiliar staff, limited patient access, radiation exposure (📌 ALARA), magnetic fields (MRI).
- Patient Factors: Often sicker, multiple comorbidities, ↑risk.
- Procedure Types:
- Diagnostic: Angiography, biopsy.
- Therapeutic: Embolization, angioplasty, stenting, drainage, TIPS, neurointerventional.
- Radiation Safety: Key concern.
⭐ The ALARA (As Low As Reasonably Achievable) principle is paramount for radiation safety of both patient and personnel in the IR suite.
Anesthesia for Interventional Radiology - Ready, Set, Scan!
- Pre-Scan Checklist:
- Comprehensive H&P: Assess cardiac, respiratory, renal, hepatic function.
- Allergy Screen: Crucial for contrast media; document reactions.
- Medication Review: Focus on anticoagulants/antiplatelets; follow specific management protocols.
- Verify NPO status and informed consent.
- Critical Labs: Aim for INR < 1.5, Platelet count > 50,000/µL (varies by procedure).
⭐ Severe contrast allergy history? Premedicate: Prednisone 50mg PO (13h, 7h, 1h prior) + H1/H2 blockers.
Anesthesia for Interventional Radiology - The Sedation Spectrum
Anesthetic approaches for IR:
| Feature | Monitored Anesthesia Care (MAC) | General Anesthesia (GA) |
|---|---|---|
| Level | Minimal to deep sedation; patient self-maintains airway. | Unconsciousness; loss of reflexes; airway secured. |
| Indications | Shorter, minor procedures; cooperative. | Long/complex; uncooperative; airway risk; neuro IR, TIPS. |
| Pros | Rapid recovery; ↓physiological impact; responsive. | Secure airway; immobility; controlled. |
| Cons | Needs cooperation; airway risk (deep); conversion risk. | Slower recovery; ↑hemodynamic changes; PONV. |
| Agents | Propofol, midazolam, fentanyl, remifentanil, dexmedetomidine. | TIVA (propofol), volatiles, muscle relaxants. |
- Regional Anesthesia (RA): Limited use; for specific peripheral sites.
Anesthesia for Interventional Radiology - Vigilant Vibes
- Monitoring: Standard ASA.
- Invasive BP (arterial line): For major procedures or hemodynamic instability.
- Temperature: Continuous monitoring vital.
- Neuromonitoring (Neuro IR): SSEP, MEP, EEG for specific cases.
- Challenges:
- Limited patient access due to equipment.
- Electromagnetic interference with monitors.
- Radiation exposure (patient, staff). Scatter radiation awareness.
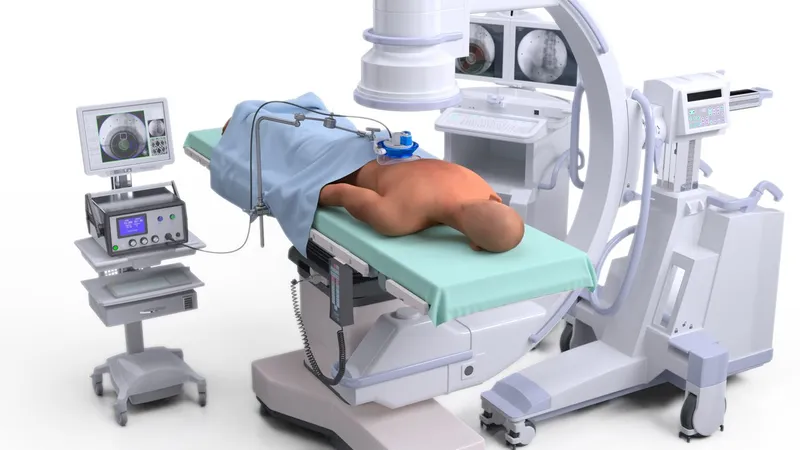
⭐ Maintaining normothermia is crucial as hypothermia can exacerbate coagulopathy and delay recovery, especially in long IR procedures.
Anesthesia for Interventional Radiology - Procedure Pointers
| Common IR Procedure | Key Anesthetic Goals | Potential Complications |
|---|---|---|
| Embolizations | Pain control, manage hemodynamic changes | Pain, bleeding, non-target embolization, post-embolization syndrome |
| Angioplasty/Stenting | Maintain perfusion, manage contrast reactions | Contrast nephropathy/allergy, dissection, thrombosis, hemorrhage |
| TIPS | Secure airway (GA preferred), manage massive hemorrhage | Hemorrhage, arrhythmias, hepatic encephalopathy, ascites |
| Neurointerventional | Controlled hypotension, rapid emergence, neuro-monitoring | Stroke, vasospasm, re-bleed, ↑ICP, contrast issues |
| Biopsies/Drainages | Pain control, manage bleeding, patient immobility | Pain, bleeding, pneumothorax (thoracic), infection |
High‑Yield Points - ⚡ Biggest Takeaways
- IR patients are often high-risk with multiple comorbidities; procedures can be prolonged.
- Monitored Anesthesia Care (MAC) is common; General Anesthesia (GA) for complex procedures or immobility.
- Prioritize radiation safety, manage contrast allergy risks, and address remote location challenges.
- Absolute patient immobility is critical, especially during neurovascular interventions.
- Careful management of anticoagulants/antiplatelets is vital due to bleeding potential.
- Be aware of post-embolization syndrome after TACE or similar embolization procedures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

