Pre-Anesthetic Assessment - Cardiac Checkpoint
- History & Symptoms:
- Cardiac status: NYHA class, angina (CCS), prior MI/PCI/CABG.
- Exercise tolerance: METs (>4 desirable).
- Key symptoms: Dyspnea, orthopnea, PND, syncope.
- Comorbidities & Medications:
- HTN, DM, CKD, OSA, PVD.
- Antiplatelets (Aspirin, Clopidogrel, Ticagrelor), Anticoagulants (Warfarin, NOACs) - crucial management plan needed.
- β-blockers, ACEi/ARBs.
- Allergies: Especially contrast dye.
- Essential Investigations:
- ECG: Baseline rhythm, ischemia, LVH, old MI signs.
- Echocardiography (recent): LVEF (EF <35-40% = ↑risk), valvular function (esp. AS, MR), PAH, RWMA.
- Labs: Hb, Platelets, PT/INR, aPTT, Creatinine, K+.
- Risk Stratification:
- RCRI (Revised Cardiac Risk Index).
- Functional capacity assessment.
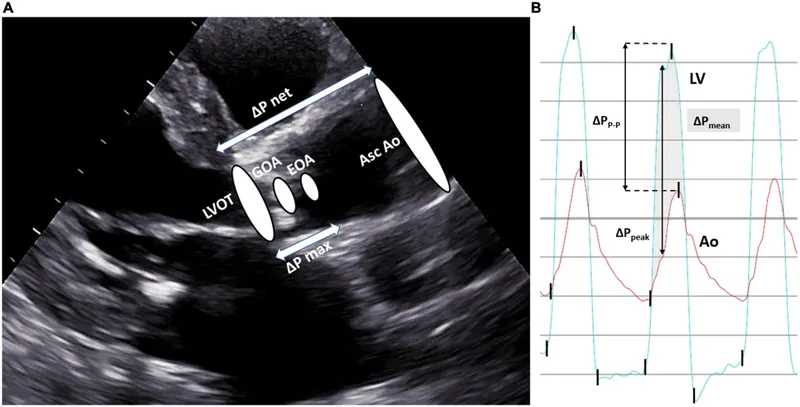
⭐ Severe Aortic Stenosis (AS) (valve area <1.0 cm², mean gradient >40 mmHg, or jet velocity >4.0 m/s) significantly increases peri-procedural risk; meticulous hemodynamic management is paramount during interventional cardiology procedures.
Anesthesia Techniques - Cath Lab Calm
- Anesthesia Spectrum: MAC vs. GA
- MAC (Monitored Anesthesia Care): Preferred for cooperative patients.
- Agents: Propofol (TCI/bolus), Remifentanil, Dexmedetomidine.
- 📌 Dexmed: Delivers Dreamy sedation, Doesn't Depress Dreathing.
- GA (General Anesthesia): For uncooperative, long procedures, airway risk.
- Agents: Volatiles or TIVA (Total Intravenous Anesthesia).
- MAC (Monitored Anesthesia Care): Preferred for cooperative patients.
- Vigilant Monitoring
- Standard ASA: ECG, NIBP, SpO₂, EtCO₂, Temp.
- Invasive Lines: Arterial (complex cases), CVP.
- TEE: For structural interventions (e.g., TAVI, MitraClip).
- Cath Lab Caveats
- Radiation Safety: Lead protection, dosimeters.
- Contrast: Vigilance for reactions.
- Anticoagulation: Heparin (ACT >250-300s).
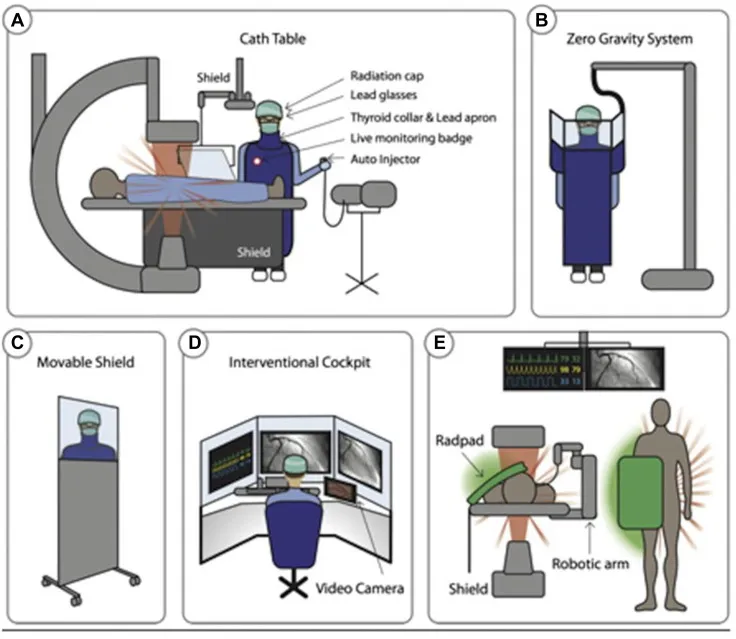
⭐ Dexmedetomidine is ideal for cath lab sedation: provides anxiolysis, analgesia, and sedation with minimal respiratory depression, maintaining spontaneous ventilation.
Intra-Op Issues - Code Cath
Rapid recognition & management of cath lab emergencies. "Code Cath" protocols vital.
- Hemodynamic Instability:
- Hypotension: Fluids, vasopressors (phenylephrine, NE).
- Hypertension: Labetalol, esmolol, NTG.
- Arrhythmias: (Follow ACLS)
- Bradycardia: Atropine 0.5-1mg, pacing.
- Tachyarrhythmias (VT/SVT with pulse): Amiodarone 150mg IV. Unstable: Cardiovert.
- Myocardial Ischemia/Infarction:
- ECG changes, chest pain.
- O2, NTG, aspirin, heparin. PCI/stent.
- Cardiac Tamponade:
- Beck's Triad (hypotension, JVD, muffled sounds).
- ECHO. Emergent pericardiocentesis.
- Contrast Reactions:
- Mild: Antihistamines (diphenhydramine 25-50mg).
- Anaphylaxis: Epinephrine (0.3-0.5mg IM or 0.1mg IV), O2, fluids, steroids.
- Vascular Access Complications:
- Hematoma, pseudoaneurysm, retroperitoneal bleed.
- Compression, US-guided thrombin, surgery.
⭐ For heparin reversal during bleeding, administer protamine sulfate: 1 mg for every 100 units of circulating heparin. Max dose 50 mg.
Post-Cath Care - Recovery Roadmap
- Handover: SBAR (Situation, Background, Assessment, Recommendation).
- Monitoring: Vital signs, access site (hematoma, bleeding), distal pulses.
- Pain Management: Multimodal analgesia; opioids for severe pain.
- Anticoagulation: Continue per protocol (e.g., DAPT post-stent, OAC for AF).
- Neurological Assessment: Especially post-TAVI or carotid interventions.
- Procedure-Specific Considerations:
- TAVI: Monitor for conduction blocks, vascular complications.
- EP Ablation: Groin care, monitor for pericardial effusion signs.
- Discharge Criteria: Stable vitals, no active bleeding, pain controlled.
⭐ Post-PCI, Dual Antiplatelet Therapy (DAPT) with Aspirin and a P2Y12 inhibitor is typically continued for 6-12 months, depending on stent type and patient's bleeding risk.
High-Yield Points - ⚡ Biggest Takeaways
- Conscious sedation (MAC) is common; GA for complex, long procedures or uncooperative patients.
- Crucial anticoagulation management: monitor Activated Clotting Time (ACT), targeting 250-350s with heparin.
- Prevent Contrast-Induced Nephropathy (CIN) via hydration and minimizing contrast volume.
- Strict radiation safety (ALARA principle) for patient and staff is essential.
- Monitor for vascular access site complications: hematoma, pseudoaneurysm, retroperitoneal bleed.
- Maintain hemodynamic stability: manage arrhythmias, hypotension, and potential ischemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

