CCL Setup & Pre-Flight Checks - Cath Lab Conquest
- Unique CCL Environment: Radiation, remote location, shared airway, limited space/access.
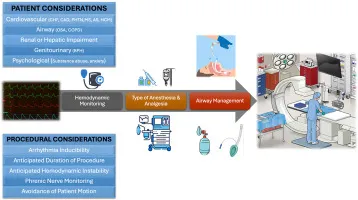
- Pre-Procedural Assessment (📌 CATH):
- Cardiac: IHD, valvular lesions, LV function (e.g., EF < 35%), arrhythmias.
- Allergies: Esp. to contrast media (note previous contrast reaction).
- Tests: ECG, Echo, Renal function (e.g., Serum Creatinine > 1.5 mg/dL).
- Haemorrhage Risk: Coagulopathy; review antiplatelets, anticoagulants.
- Comorbidities (renal, diabetes), ASA status, informed consent.
- NPO Guidelines: Solids 6-8 hrs, clear fluids 2 hrs pre-procedure.
⭐ Patients with significant renal dysfunction (e.g., eGFR < 30 mL/min/1.73 square meters) require careful consideration for contrast volume and nephroprotective strategies.
Anesthetic Modalities - Potions & Protocols
- Goals: Patient safety, comfort, immobility, hemodynamic stability, rapid recovery. 📌 SEDATe (MAC): Safety, Equilibrium (hemodynamic), Discomfort relief, Amnesia, Titratability, Emesis prevention.
- Monitored Anesthesia Care (MAC): Most common. Agents:
- Midazolam: Anxiolysis, amnesia (0.02-0.1 mg/kg).
- Fentanyl/Remifentanil: Analgesia.
- Propofol: Sedation, antiemetic (Bolus: 0.25-0.5 mg/kg; Infusion: $25-75 \text{ mcg/kg/min}$). Risks: apnea, hypotension.
- Dexmedetomidine: Sedation, minimal respiratory depression, sympatholysis.
- General Anesthesia (GA) Indications: Uncooperative/pediatric patients, prolonged/complex procedures (structural heart), hemodynamic instability, MAC refusal, difficult airway.
- Airway (GA): Remote setting considerations.
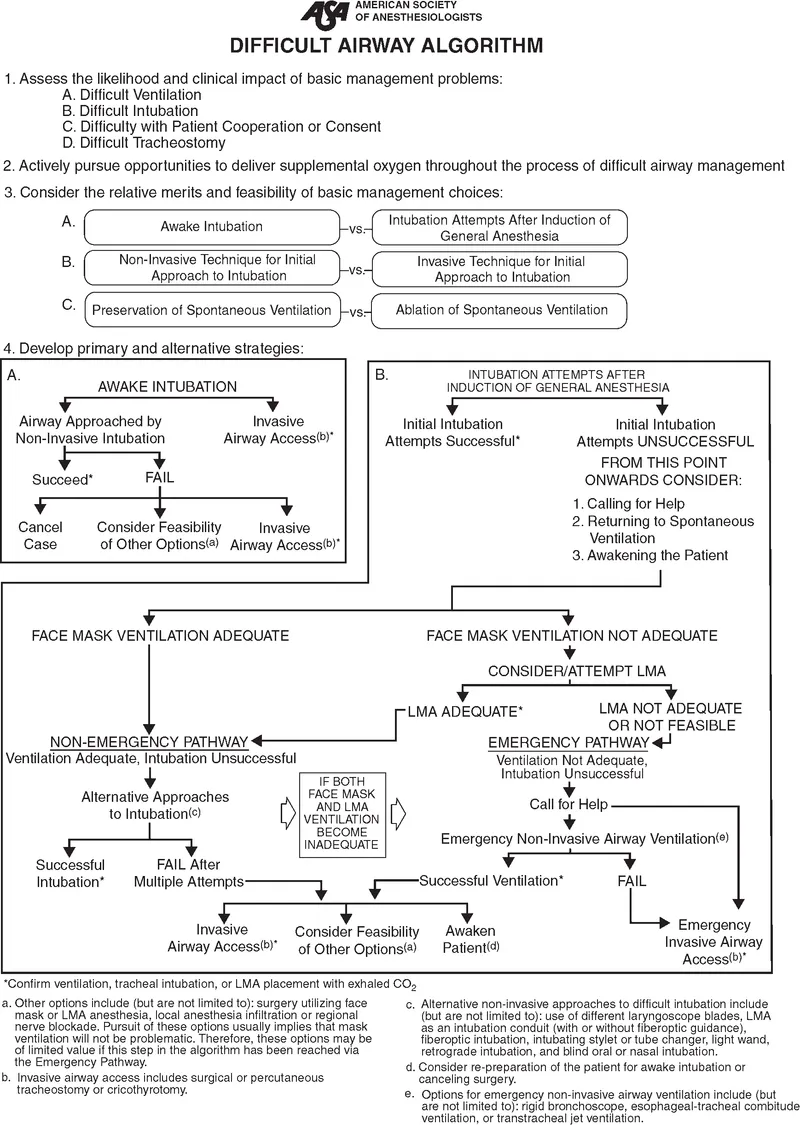
⭐ Dexmedetomidine is particularly useful in patients where respiratory depression is a major concern (e.g., severe COPD, OSA) undergoing procedures under MAC.
Vigilant Monitoring - Cath Lab Command
- Standard ASA Monitoring:
- ECG: Continuous, leads II & V5 for ischemia detection (ST depression > 1mm).
- NIBP: Frequent cycling.
- SpO2, Temperature.
- Capnography (ETCO2): Mandatory for General Anesthesia (GA); highly recommended for deep Monitored Anesthesia Care (MAC) to monitor ventilation.
- Invasive Arterial Blood Pressure (IABP):
- Indications: Anticipated large fluid shifts/blood loss, severe LV dysfunction, frequent blood sampling, vasopressor/inotrope use.
- Activated Clotting Time (ACT):
- Crucial for procedures requiring heparinization (e.g., PCI, structural interventions).
- Target ACT typically 250-350 seconds.
- Neuromuscular Monitoring: If muscle relaxants are administered.
- Radiation Safety: 📌 ALARA (As Low As Reasonably Achievable) for personnel - lead aprons, thyroid shields, dosimeters.
⭐ Continuous 5-lead ECG monitoring is preferred over 3-lead for better detection of myocardial ischemia during cardiac catheterization procedures.
Complication Control - Crisis Crew
- Hemodynamic Instability:
- Hypotension: Causes (vasovagal, hypovolemia, ischemia, drugs). Mgmt:
- Hypertension: Causes (pain, anxiety, pre-existing). Mgmt: Analgesics, anxiolytics, antihypertensives (e.g., Labetalol **5-20 mg IV**).
- Arrhythmias: Bradyarrhythmias (Atropine **0.5-1 mg IV**, pacing), Tachyarrhythmias (ACLS guided).
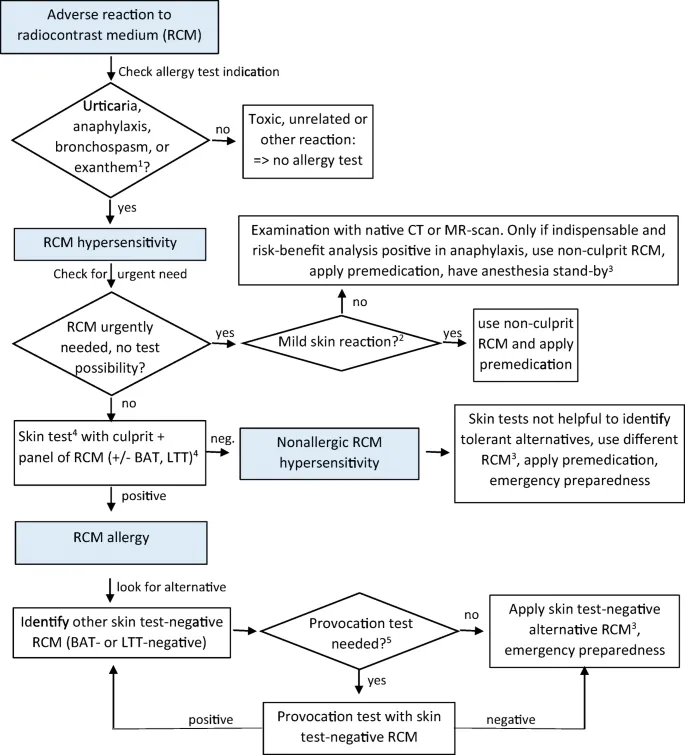
- Contrast Media Reactions:
- Types: Mild (urticaria), Moderate (bronchospasm), Severe/Anaphylactoid (shock).
- Prophylaxis (high-risk): Steroids, antihistamines.
- Mgmt: Mild (antihistamines); Moderate (O2, bronchodilators, steroids); Severe (Epinephrine $0.3-0.5 \text{ mg IM}$ (1:1000) or $0.05-0.1 \text{ mg IV}$ (1:10000), IV fluids, O2, airway support).
- Vascular Access Complications:
- Hematoma, pseudoaneurysm, retroperitoneal hemorrhage.
⭐ Retroperitoneal hemorrhage: rare, life-threatening femoral access complication; presents with hypotension, flank pain, ↓Hb.
- Other Key Complications:
- Thromboembolism/Stroke: Maintain anticoagulation.
- Air Embolism: Left lateral decubitus (LLD), Trendelenburg, 100% O2.
- Local Anesthetic Systemic Toxicity (LAST): If large LA volumes; Mgmt: Lipid emulsion therapy.
- 📌 HHAPPy Mnemonic (Common Complications): Hemorrhage, Hypotension, Arrhythmia, Pseudoaneurysm, Puncture site pain.
- Emergency Preparedness:
- Essential: Difficult airway cart, defibrillator, emergency drugs readily available (e.g., ACLS drugs).
High-Yield Points - ⚡ Biggest Takeaways
- Monitored Anesthesia Care (MAC) is preferred, using midazolam and fentanyl for sedation.
- Vigilant airway monitoring and readiness for intervention are crucial due to sedation risks.
- Systemic heparinization is standard; target Activated Clotting Time (ACT) of 250-300 seconds.
- Key complications: cardiac arrhythmias, vascular access site bleeding, and allergic contrast reactions.
- Ensure immediate availability of reversal agents like naloxone and flumazenil.
- General anesthesia is often necessary for pediatric patients or complex interventions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

