Bronchoscopy Basics & Pre-op Prep - Scope Scope Hooray!
- Types & Indications:
- Flexible Bronchoscopy (FOB): Diagnostic (biopsy, BAL, brushings), difficult intubation aid. Smaller, ↑maneuverability, wider reach.
- Rigid Bronchoscopy: Therapeutic (foreign body removal, stent placement, laser ablation, debulking tumors, managing massive hemoptysis), central airway obstruction. Larger lumen, better airway control & suction/ventilation options.
- Pre-operative Preparation:
- Assessment: Detailed history (bleeding disorders, drug allergies), airway examination (Mallampati, TMD), cardiorespiratory status.
- Investigations: Baseline Hb, coagulation profile, CXR. PFTs if severe respiratory disease. Group & save if high bleeding risk.
- Fasting: 6-8 hrs for solids, 2 hrs for clear fluids.
- Premedication: Antisialagogue (e.g., Glycopyrrolate 0.2 mg IV/IM), Anxiolytic (e.g., Midazolam 1-2 mg IV). Consider nebulized lignocaine.
- Informed consent detailing risks (bleeding, pneumothorax, hypoxemia).
⭐ Rigid bronchoscopy is preferred for foreign body removal and massive hemoptysis.

Anesthetic Goals & Techniques - Snooze & Cruise Views
-
Goals:
- Amnesia, anxiolysis, analgesia
- Suppress cough/gag reflexes
- Maintain oxygenation (SpO₂ > 90%) & ventilation
- Hemodynamic stability
- Rapid recovery & return to baseline
-
Techniques Overview:
- Topical Anesthesia + Monitored Anesthesia Care (MAC):
- Lidocaine (spray/nebulized/transtracheal) + Sedatives (Midazolam, Fentanyl, Propofol).
- Common for flexible bronchoscopy.
- General Anesthesia (GA):
- Required for rigid bronchoscopy; sometimes for complex flexible cases.
- Methods:
- Total Intravenous Anesthesia (TIVA): Propofol, Remifentanil.
- Inhalational (less common due to leaks/pollution).
- Airway: Endotracheal Tube (ETT), Laryngeal Mask Airway (LMA), or specialized jet ventilation (rigid).
- Topical Anesthesia + Monitored Anesthesia Care (MAC):
⭐ Total Intravenous Anesthesia (TIVA) with propofol and remifentanil is commonly preferred for flexible bronchoscopy to allow for rapid recovery and precise titration.
Airway Matters & Ventilation - Breathe Easy Breezy
- Shared Airway: Critical! Constant team communication. Anticipate obstruction.
- Pre-oxygenation: 100% O2 for 3-5 min vital.
⭐ Apneic oxygenation (e.g., via nasal cannula at 5-10 L/min) is crucial during periods of airway manipulation to prolong safe apnea time and prevent desaturation.
- Ventilation Choices:
- Spontaneous Respiration (IV sedation).
- Controlled (GA): ETT (size for scope & ventilation), LMA (bronchoscopy-specific), High-Frequency Jet Ventilation (HFJV).
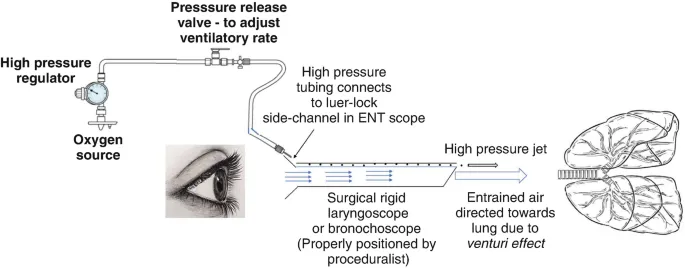
- HFJV: Venturi principle (Sanders injector). Risks: barotrauma, air trapping. Ensure patent exhalation.
- Monitoring: Continuous SpO2, ECG, NIBP. EtCO2 often difficult.
- ⚠️ Key Risks: Hypoxemia, hypercapnia, laryngospasm, bronchospasm.
Monitoring & Crisis Control - Oopsie Whoopsie Scope!
- Monitoring: Standard ASA (ECG, NIBP, SpO2) + EtCO2. Continuous vigilance for desaturation, airway obstruction, or inadequate anesthesia.
- Common Crises & Initial Steps: 📌 LBBBA (Laryngospasm, Bronchospasm, Bleeding, Barotrauma, Arrhythmias)
- Hypoxemia: Immediately give 100% O2, check airway/circuit integrity, suction secretions, deepen anesthesia. Pause procedure.
- Laryngospasm: Apply 100% O2 with PPV, deepen anesthesia, give suxamethonium (0.5-1 mg/kg IV). Larson's maneuver.
- Bronchospasm: Administer 100% O2, ↑volatile/propofol, use IV/inhaled β2-agonists. Consider steroids.
- Bleeding: Vigorous suction, topical adrenaline (1:10,000-1:20,000), cold saline lavage. Inform surgeon promptly.
- Cough/Bucking: Deepen level of anesthesia, administer IV lidocaine (1-1.5 mg/kg).
⭐ Topical or intravenous lidocaine is effective in suppressing cough reflex and reducing airway reactivity, minimizing patient movement and complications.
High‑Yield Points - ⚡ Biggest Takeaways
- Shared airway is a core challenge, demanding excellent team communication with the proceduralist.
- Topical anesthesia of the airway (e.g., lignocaine) is vital to suppress reflexes and improve patient tolerance.
- Sedation spectrum: conscious sedation (midazolam, fentanyl) to deep sedation/general anesthesia (propofol, remifentanil).
- Ventilation options include spontaneous breathing, jet ventilation, or controlled ventilation via LMA/ETT.
- Key complications: laryngospasm, bronchospasm, hypoxemia, arrhythmias, and hemorrhage post-procedure.
- Rigid bronchoscopy typically requires general anesthesia with muscle relaxation; flexible bronchoscopy often uses sedation techniques alone or with GA.
- Pre-operative assessment should focus on airway examination and cardiopulmonary reserve to anticipate difficulties and risks during the procedure and recovery period for the patient.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

