Primary Survey & Resuscitation - Trauma Tango
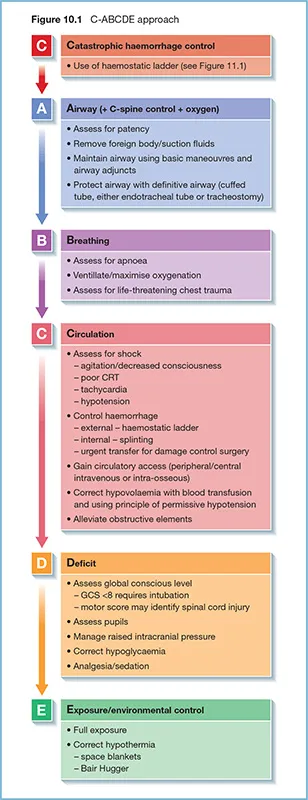
Systematic ABCDE approach: rapid ID & management of life-threatening injuries. Simultaneous resuscitation. 📌 Airway, Breathing, Circulation, Disability, Exposure.
- Airway & C-Spine:
- Assess patency, clear. Secure airway (intubate if GCS ≤ 8).
- C-spine immobilization.
- Breathing & Ventilation:
- Assess rate, depth. Oxygenation (SpO₂ > 94%).
- Manage tension pneumothorax, open pneumothorax.
- Circulation & Hemorrhage:
- Control external bleed. IV access (2 large-bore).
- Fluids/blood. Permissive hypotension (SBP 80-90 mmHg) if no TBI.
- Disability (Neuro):
- GCS, pupils.
- Exposure & Environment:
- Undress fully. Prevent hypothermia (warm blankets/fluids).
⭐ Lethal Triad in trauma: hypothermia, acidosis, coagulopathy. Early, aggressive management is crucial for survival.
Trauma Airway Management - Breath Guardian
- C-spine immobilization: MILS during airway maneuvers.
- Rapid Sequence Intubation (RSI): For unprotected airway.
- Preoxygenate: 100% O2, 3-5 min.
- Drugs: Ketamine (1-2 mg/kg IV) / Etomidate (0.2-0.3 mg/kg IV); Succinylcholine (1-1.5 mg/kg IV) / Rocuronium (1.2 mg/kg IV).
- Difficult Airway: LEMON assessment.
- Backups: SGA, Video Laryngoscopy.
- Failed: Surgical Cricothyroidotomy.
- "Breath Guardian" - Post-Intubation:
- Confirm: EtCO2 (gold standard), chest rise.
- Secure tube.
- Ventilate: LPS ($V_T$ 6-8 mL/kg IBW, PEEP).
- Monitor: SpO2, EtCO2. Prevent hypoxia/hypercapnia.
⭐ Ketamine is often favored in hypotensive trauma patients for RSI due to its sympathomimetic properties, maintaining hemodynamic stability.
Hemorrhagic Shock & MTP - Red River Rally
-
Hemorrhagic Shock: Blood loss → ↓perfusion.
- ATLS Classes I-IV guide resuscitation. Key examples:
- Class III: 30-40% loss, HR >120, BP ↓, UO 5-15ml/hr.
- Class IV: >40% loss, HR >140, BP markedly ↓, UO negligible.
- Management: Stop bleed, restore volume, permissive hypotension (SBP 80-90 mmHg pre-control, not TBI).
- ⚠️ Avoid "Lethal Triad": Hypothermia, Acidosis, Coagulopathy.
- ATLS Classes I-IV guide resuscitation. Key examples:
-
Massive Transfusion Protocol (MTP):
- Triggered by e.g., >4 units PRBCs in 1 hr.
- Ratio: 1:1:1 (PRBC:FFP:Platelets). 📌 Mnemonic: "Red River Rally".
- Goals: Hb >7 g/dL, Plt >50,000/µL, Fibrinogen >1.5-2 g/L, normothermia, normocalcemia.
⭐ TXA: 1g IV within 3 hrs of injury, then 1g IV over 8 hrs. Reduces mortality in bleeding trauma.
Anesthetic Management & DCS - Damage Control Dance
- Core Goals: Rapid physiological stabilization & surgical control.
- Address "Lethal Triad":
- Hypothermia (<35°C): Aggressive warming (warm fluids, forced air warmers).
- Acidosis (pH <7.2, BE <-6): Optimize ventilation/perfusion, judicious bicarbonate.
- Coagulopathy (INR >1.5, PTT >60s, Platelets <50,000): Tranexamic acid (TXA), 1:1:1 PRBC:FFP:Platelets. (📌 "Trauma triad is a bad cascade")
- Permissive Hypotension: Target SBP 80-90 mmHg (unless TBI: MAP >80 mmHg).
- Address "Lethal Triad":
- Anesthetic Choices:
- Induction: Ketamine (hemodynamically stable), Etomidate (cardio-stable, adrenal suppression risk).
- Maintenance: Low MAC volatiles (e.g., Sevoflurane <1 MAC) or TIVA. Avoid N₂O.
- Damage Control Surgery (DCS) - "The Dance":
- Phase 1 (OR): Abbreviated surgery (control hemorrhage/contamination).
- Phase 2 (ICU): Physiological restoration (correct lethal triad).
- Phase 3 (OR): Planned re-operation for definitive repair.
⭐ Early administration of Tranexamic Acid (TXA) within 3 hours of injury significantly improves survival in bleeding trauma patients.

High‑Yield Points - ⚡ Biggest Takeaways
- Airway management is paramount; assume cervical spine injury until cleared.
- Rapid Sequence Intubation (RSI) is standard for securing the trauma airway.
- Manage hemorrhagic shock with permissive hypotension (SBP 80-90 mmHg) and 1:1:1 balanced transfusion.
- Prioritize Damage Control Resuscitation (DCR) and early Damage Control Surgery (DCS).
- Prevent and treat the lethal triad: hypothermia, acidosis, and coagulopathy.
- Ketamine is preferred for induction in hemodynamically unstable patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

