Pre-op Assessment & Risks - Abdominal Alert!
- Initial Triage (ABCDE): Prioritize ABCs. Address life-threats.
- Focused History: AMPLE. Pain details, vomiting, fever.
- Clinical Exam: Vitals. Abdominal: distension, tenderness, rigidity. Shock/sepsis signs (qSOFA).
- Major Risks:
- Full Stomach: High aspiration risk; RSI standard.
- Hemodynamic Instability: Hypovolemia, septic shock.
- Sepsis & Organ Dysfunction: ↑Lactate, acidosis, organ impairment.
- Electrolyte Imbalance: K⁺, Ca²⁺, Mg²⁺.
- Coagulopathy.
- Investigations: CBC, U&Es, LFTs, coag, G&S/X-match, lactate, ABG. Imaging (USG, X-ray, CT).
- Pre-Anesthetic Optimization (Time Permitting):
- IV fluids: Target MAP >65 mmHg, UO >0.5 ml/kg/hr.
- Broad-spectrum antibiotics.
- Correct severe electrolyte/acid-base.
- NGT decompression.
- Blood if Hb <7-8 g/dL / hemorrhage.
- Consent: Informed; if incapacitated, act in best interest.
⭐ Patients with acute abdomen are ALWAYS considered "full stomach" - RSI is mandatory unless specific contraindications exist (e.g., anticipated difficult airway where awake technique preferred).
Induction & Airway Mgmt - Airway Action!
- Goal: Rapid airway control, prevent aspiration (full stomach). RSI is standard.
- 📌 RSI Steps (The 7 P's):
- Preparation: 📌 "SOAP ME" (Suction, Oxygen, Airway equip, Pharmacology, Monitors, Emergency equip).
- Preoxygenation: 100% O₂ 3-5 min / 4 VC breaths. Target EtO₂ >90%.
- Pre-treatment (consider): Lidocaine 1.5 mg/kg, Fentanyl 1-3 mcg/kg.
- Paralysis with Induction:
- Induction: Ketamine (1-2 mg/kg), Etomidate (0.2-0.3 mg/kg), Propofol (1.5-2.5 mg/kg).
- Relaxant: Succinylcholine (1-1.5 mg/kg) or Rocuronium (0.9-1.2 mg/kg for RSI).
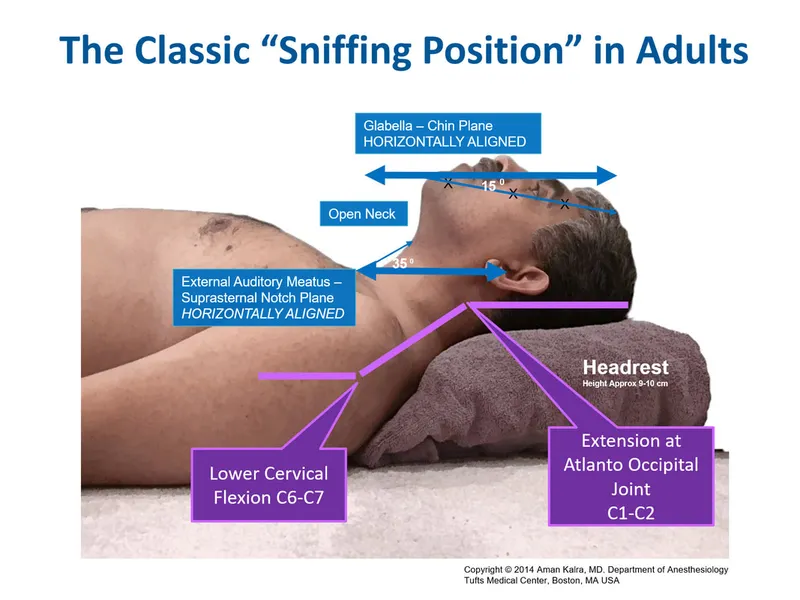
- Positioning: Sniffing position for optimal glottic view.
- Protection: Cricoid pressure (Sellick’s) 30N (apply before LOC, release after ETT cuff inflation; controversial).
- Placement & Proof: Intubate; confirm with capnography (EtCO₂).
⭐ Capnography is the GOLD STANDARD for confirming endotracheal tube placement.
- Difficult Airway: Anticipate! Have backup: VL, SGA (e.g., LMA), surgical airway kit.
Intra-op & Post-op Care - Gut Battle Anesthesia
- Intra-operative Management:
- Monitoring: Standard ASA, IBP, CVP, UO. Temp, EtCO2 monitoring.
- Fluid Resuscitation: Goal-directed therapy (GDT). Balanced crystalloids (RL). Target MAP >65 mmHg, UO >0.5 ml/kg/hr. Blood products ready.
- Ventilation: Lung Protective Strategy (LPSV): $V_T$ 6-8 ml/kg IBW, PEEP 5-8 cmH2O.
- Anesthetic Technique: Balanced: Volatiles, Opioids, NMBs (NeuroMuscular Blockers). TIVA for high-risk (aspiration/MH).
- Specifics: NG/OG for decompression. Active warming. Sepsis: early antibiotics, source control, Noradrenaline (for MAP). MTP (PRBC:FFP:Platelets 1:1:1) if major bleed.
- Post-operative Care & Transition:
- Disposition: PACU/ICU based on stability.
- Pain Control: Multimodal pain relief: IV opioids (PCA), epidural, TAP blocks, NSAIDs (cautious), Paracetamol.
- PONV Prophylaxis: Ondansetron, Dexamethasone.
- Respiratory Support: O2 therapy, chest physio, early mobilization. Monitor atelectasis.
- Gut Management: Monitor for ileus. Early Enteral Nutrition (EEN) when feasible.
- Thromboprophylaxis: DVT prophylaxis (mechanical/pharmacological).
⭐ For septic shock in abdominal emergencies, MAP ≥65 mmHg via early Noradrenaline is key for organ perfusion.
High‑Yield Points - ⚡ Biggest Takeaways
- Full stomach mandates Rapid Sequence Intubation (RSI) to prevent aspiration.
- Hemodynamic instability (hypovolemia, sepsis) requires judicious fluid resuscitation and vasopressor support.
- Prioritize aspiration prophylaxis: pre-oxygenation, cricoid pressure, and prompt Endotracheal Tube (ETT) insertion.
- Multimodal analgesia, including regional blocks (e.g., TAP, epidural), is key for effective pain control.
- Correct electrolyte disturbances (e.g., hypokalemia in bowel obstruction) preoperatively if feasible.
- Be vigilant for complications of ↑ Intra-Abdominal Pressure (IAP), such as respiratory compromise.
- Consider ketamine or etomidate for induction in hemodynamically unstable patients to maintain stability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

