Anesthesia for Emergency Surgery

On this page
🚨 Emergency Surgery Anesthesia: The Critical Hour Command Center
Emergency surgery anesthesia compresses decisions that normally unfold over hours into minutes, where aspiration risk meets hypovolemia, full stomachs collide with empty vasculature, and the luxury of optimization vanishes. You'll master the 90-second assessment that captures what matters, deploy rapid-sequence techniques that protect the airway while circulatory collapse looms, and orchestrate hemodynamic resuscitation concurrent with anesthetic induction. This lesson builds your command of the critical decision architecture that transforms chaos into controlled intervention when seconds determine survival.
📌 Remember: CRASH - Critical assessment, Rapid sequence induction, Airway security, Stabilization priorities, Hemodynamic support. Every emergency case follows this systematic approach within the first 3-5 minutes of patient arrival.
The emergency anesthesia framework operates on three fundamental pillars: rapid physiological assessment (<2 minutes), immediate life-threatening intervention (<5 minutes), and continuous adaptive management throughout the procedure. Understanding these principles transforms chaotic emergency scenarios into systematic, life-saving interventions.
⭐ Clinical Pearl: Emergency surgery patients have 3-5 times higher mortality risk compared to elective cases, with anesthetic complications contributing to 15-20% of preventable deaths. Mastering rapid assessment protocols reduces this risk by 40-60%.
| Emergency Type | Time to OR | Mortality Risk | Key Anesthetic Challenge | Success Rate |
|---|---|---|---|---|
| Trauma Surgery | <30 min | 15-25% | Hemorrhagic shock + full stomach | 75-85% |
| Ruptured AAA | <15 min | 40-60% | Hemodynamic instability | 60-70% |
| Acute Abdomen | <60 min | 5-15% | Sepsis + volume depletion | 85-95% |
| Emergency C-Section | <10 min | 2-5% | Maternal-fetal physiology | 95-98% |
| Airway Emergency | <5 min | 20-40% | Cannot intubate/ventilate | 80-90% |
- Hemorrhage Protocol: Massive transfusion capability with 1:1:1 ratio (RBC:FFP:Platelets)
- Type O negative blood immediately available (<3 minutes)
- Rapid infusion devices capable of 500-1000 mL/min delivery
- Point-of-care coagulation testing (<10 minutes results)
- Airway Crisis Management: Multiple backup plans with <30 seconds between attempts
- Video laryngoscopy as primary tool (85-95% first-pass success)
- Supraglottic airways immediately accessible
- Surgical airway capability within 2-3 minutes
- Hemodynamic Support: Vasoactive drugs pre-drawn and calculated
- Norepinephrine 0.1-0.5 mcg/kg/min for distributive shock
- Epinephrine 0.01-0.1 mcg/kg/min for cardiogenic shock
- Vasopressin 0.01-0.04 units/min for refractory hypotension
💡 Master This: Emergency anesthesia transforms unpredictable crises into systematic protocols. Every successful outcome depends on pre-crisis preparation, rapid pattern recognition, and adaptive decision-making based on real-time physiological feedback.
Connect these foundational emergency principles through rapid assessment frameworks to understand systematic patient evaluation patterns.
🚨 Emergency Surgery Anesthesia: The Critical Hour Command Center
⚡ Rapid Assessment Mastery: The 90-Second Evaluation Engine

Airway Assessment requires multi-dimensional evaluation beyond simple patency:
- Anatomical Predictors: Mallampati III-IV increases difficult intubation risk by 300-400%
- Thyromental distance <6 cm predicts difficult laryngoscopy (sensitivity 85%)
- Neck mobility <35 degrees extension complicates visualization
- Mouth opening <3 cm limits laryngoscope insertion
- Physiological Compromise: Respiratory distress patterns indicate urgency level
- Respiratory rate >30/min suggests impending failure
- Oxygen saturation <90% on room air demands immediate intervention
- Accessory muscle use indicates work of breathing >150% normal
📌 Remember: LEMON assessment - Look externally, Evaluate 3-3-2 rule, Mallampati, Obstruction, Neck mobility. Complete evaluation requires <30 seconds but predicts 90% of difficult airways when systematically applied.
Breathing Evaluation focuses on ventilation adequacy and oxygenation reserve:
- Ventilation Mechanics: Tidal volume assessment through chest wall movement
- Normal tidal volume 6-8 mL/kg produces visible chest rise
- Paradoxical breathing suggests diaphragmatic injury or pneumothorax
- Unilateral chest movement indicates tension pneumothorax (mortality 40-60% if untreated)
- Oxygenation Status: Pulse oximetry with clinical correlation
- SpO2 >95% generally adequate for short transport
- SpO2 90-95% requires supplemental oxygen and close monitoring
- SpO2 <90% demands immediate ventilatory support

Circulation Assessment integrates perfusion indicators with volume status:
| Parameter | Normal | Compensated Shock | Decompensated Shock | Critical |
|---|---|---|---|---|
| Heart Rate | 60-100 | 100-120 | 120-140 | >140 |
| Blood Pressure | >90 mmHg | 80-90 mmHg | 70-80 mmHg | <70 mmHg |
| Pulse Pressure | >25 mmHg | 20-25 mmHg | 15-20 mmHg | <15 mmHg |
| Capillary Refill | <2 sec | 2-3 sec | 3-4 sec | >4 sec |
| Mental Status | Alert | Anxious | Confused | Obtunded |
Disability Assessment evaluates neurological function and spinal integrity:
- Glasgow Coma Scale: Rapid assessment with anesthetic implications
- GCS 13-15: Standard induction techniques appropriate
- GCS 9-12: Modified rapid sequence with neuroprotection
- GCS <8: Immediate intubation with ICP management
- Spinal Precautions: C-spine immobilization until cleared
- Manual in-line stabilization during intubation
- Fiberoptic intubation for unstable C-spine injuries
- Methylprednisolone 30 mg/kg within 8 hours for cord injury
💡 Master This: Emergency assessment transforms complex pathophysiology into systematic evaluation protocols. Master the 90-second framework, and you possess the foundation for rapid clinical decision-making that directly impacts patient survival in critical scenarios.
Connect this systematic assessment approach through anesthetic planning strategies to understand drug selection and dosing modifications for emergency scenarios.
⚡ Rapid Assessment Mastery: The 90-Second Evaluation Engine
🎯 Emergency Anesthetic Arsenal: The Pharmacological Precision Strike

Induction Agent Selection depends on hemodynamic status and clinical urgency:
- Etomidate: Hemodynamically stable choice for unstable patients
- Dose: 0.2-0.3 mg/kg (reduce 50% in shock states)
- Maintains blood pressure in 85-90% of hypotensive patients
- Adrenal suppression risk: 24-48 hours duration
- Avoid in septic shock due to cortisol suppression
- Ketamine: Sympathomimetic properties for cardiogenic shock
- Dose: 1-2 mg/kg IV (maintain 0.5-1 mg/kg in elderly)
- Increases heart rate 15-25% and blood pressure 10-15%
- Bronchodilation benefit in reactive airway disease
- Contraindicated in elevated ICP or coronary artery disease
- Propofol: Limited use in hemodynamically stable patients
- Dose: 1-2 mg/kg (reduce to 0.5-1 mg/kg if hypotensive)
- Causes 20-30% decrease in blood pressure
- Rapid onset <60 seconds with smooth induction
- Reserve for stable patients or controlled hypotension
📌 Remember: SHOCK drug selection - Stable patients get propofol, Hypotensive get etomidate, Obstructive lung disease gets ketamine, Cardiac patients avoid ketamine, Keep doses low in elderly. Hemodynamic status determines 80% of induction agent choice.
Neuromuscular Blocking Agent Strategy balances onset time with duration requirements:
| Agent | Onset Time | Duration | Intubating Dose | Emergency Advantage |
|---|---|---|---|---|
| Succinylcholine | 45-60 sec | 5-10 min | 1-1.5 mg/kg | Fastest onset, short duration |
| Rocuronium | 60-90 sec | 45-60 min | 1.2-1.5 mg/kg | Reversible with sugammadex |
| Vecuronium | 90-120 sec | 30-45 min | 0.1-0.15 mg/kg | Hemodynamically neutral |
| Atracurium | 120-180 sec | 30-40 min | 0.5-0.6 mg/kg | Organ-independent elimination |
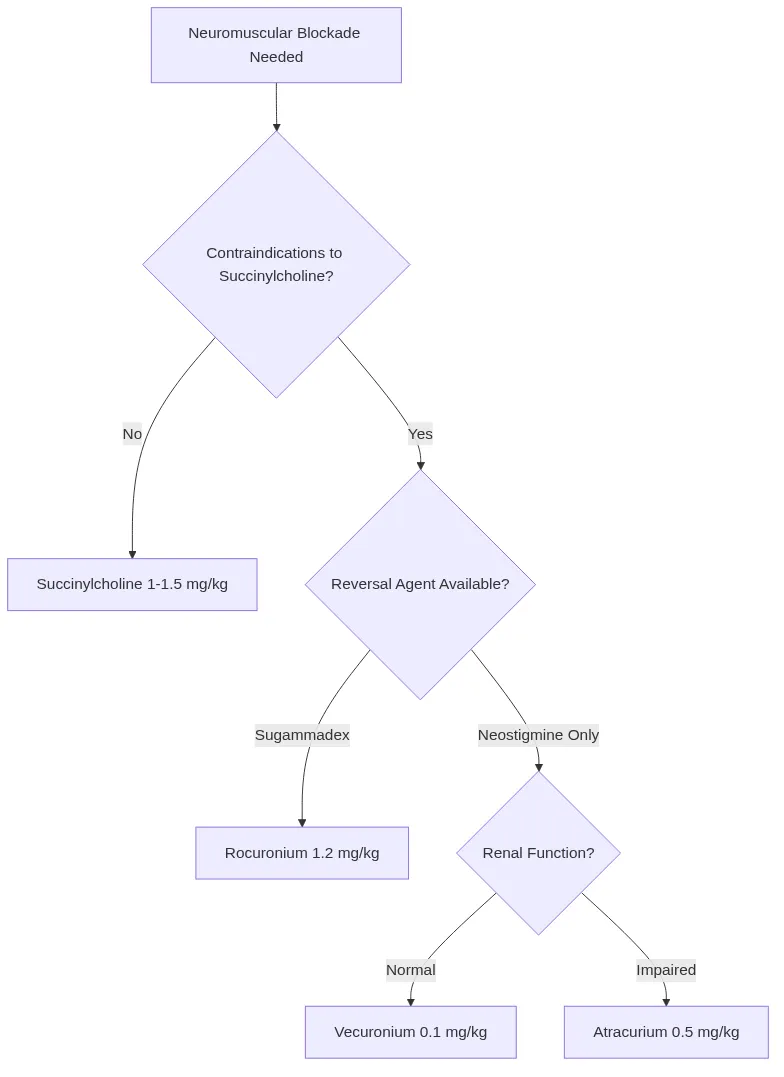
Succinylcholine Contraindications require absolute avoidance in specific scenarios:
- Hyperkalemia Risk: Baseline K+ >5.5 mEq/L or risk factors
- Burns >24 hours old (risk up to 1 year)
- Spinal cord injury >72 hours (permanent contraindication)
- Muscular dystrophy or neuromuscular disease
- Massive tissue trauma >48 hours old
- Malignant Hyperthermia: Personal or family history
- Incidence 1:15,000 in pediatric patients
- Mortality <5% with early dantrolene treatment
- Alternative: rocuronium + sugammadex reversal strategy

Analgesic Strategy addresses pain control while maintaining hemodynamic stability:
- Fentanyl: Short-acting opioid for hemodynamically unstable patients
- Dose: 1-3 mcg/kg (reduce 50% in elderly or shocked patients)
- Onset 1-2 minutes, duration 30-60 minutes
- Minimal hemodynamic effects at standard doses
- Chest wall rigidity risk at doses >5 mcg/kg
- Morphine: Longer-acting option for stable patients
- Dose: 0.1-0.2 mg/kg IV (titrate to effect)
- Histamine release causes vasodilation and hypotension
- Duration 2-4 hours with active metabolites
- Avoid in renal failure due to morphine-6-glucuronide accumulation
⭐ Clinical Pearl: Emergency drug dosing requires context-sensitive adjustments. Reduce all drug doses by 30-50% in shock states due to decreased volume of distribution and altered protein binding. Standard dosing in unstable patients causes overdose in 60-70% of cases.
Vasoactive Drug Preparation ensures immediate hemodynamic support:
- Norepinephrine: First-line vasopressor for distributive shock
- Concentration: 16 mg in 250 mL (64 mcg/mL standard)
- Starting dose: 0.1-0.5 mcg/kg/min (titrate to MAP >65 mmHg)
- Alpha-1 agonist with minimal beta effects
- Preferred in septic shock and neurogenic shock
- Epinephrine: Mixed alpha/beta agonist for cardiogenic shock
- Concentration: 4 mg in 250 mL (16 mcg/mL standard)
- Starting dose: 0.01-0.1 mcg/kg/min (titrate to effect)
- Increases heart rate, contractility, and vascular tone
- First-line in anaphylaxis and cardiac arrest
💡 Master This: Emergency pharmacology transforms standard protocols into patient-specific interventions. Master context-sensitive dosing and hemodynamic-guided selection, and you possess the precision tools for safe anesthetic management in the most challenging clinical scenarios.
Connect these pharmacological principles through airway management strategies to understand emergency intubation techniques and backup planning.
🎯 Emergency Anesthetic Arsenal: The Pharmacological Precision Strike
🛡️ Emergency Airway Command: The Life-Saving Gateway Protocol
Rapid Sequence Induction (RSI) represents the gold standard for emergency airway management, designed to minimize aspiration risk while ensuring rapid airway control:
Preoxygenation Strategy maximizes oxygen reserves before apnea period:
- Standard Technique: 100% oxygen for 3-5 minutes via face mask
- Achieves functional residual capacity saturation >95%
- Provides safe apnea time of 6-8 minutes in healthy adults
- Reduces to 2-3 minutes in obese or pregnant patients
- Rapid Technique: 8 vital capacity breaths over 60 seconds
- Alternative when time is critical (<3 minutes available)
- Achieves 85-90% of standard preoxygenation benefit
- Requires patient cooperation and adequate respiratory effort
- Apneic Oxygenation: Nasal cannula 15 L/min during laryngoscopy
- Extends safe apnea time by 2-3 minutes
- Particularly beneficial in obese patients (BMI >35)
- Reduces desaturation rate by 40-50%
📌 Remember: STOP preoxygenation goals - Saturation >95%, Time 3-5 minutes, Oxygen 100%, Patient positioning optimized. Adequate preoxygenation provides life-saving oxygen reserves during difficult airway scenarios.
Video Laryngoscopy has become the primary technique for emergency intubation, offering superior visualization and higher first-pass success rates:
| Laryngoscope Type | First-Pass Success | Cormack-Lehane Grade | Learning Curve |
|---|---|---|---|
| Direct Laryngoscopy | 70-80% | Grade 3-4: 15-20% | Extensive experience required |
| Video Laryngoscopy | 85-95% | Grade 3-4: 5-10% | Moderate experience required |
| Fiberoptic Scope | 95-98% | All grades manageable | Extensive training required |
| Supraglottic Airways | 90-95% | Not applicable | Minimal training required |
- Enhanced Visualization: 30-40% improvement in glottic view
- Reduces Cormack-Lehane Grade 3-4 views by 60-70%
- Allows indirect visualization without direct line-of-sight
- Facilitates teaching and assistance from colleagues
- Cervical Spine Protection: Reduced neck extension requirements
- 50% less cervical movement compared to direct laryngoscopy
- Maintains manual in-line stabilization effectiveness
- Critical for trauma patients with potential C-spine injury
- Improved Success Rates: First-pass success increases significantly
- Emergency department: 84% vs 70% with direct laryngoscopy
- Operating room: 94% vs 85% with direct laryngoscopy
- ICU setting: 89% vs 75% with direct laryngoscopy

Backup Airway Strategy follows systematic escalation when primary intubation fails:
- Optimization Techniques for second attempt:
- BURP maneuver: Backward, upward, rightward pressure on thyroid
- External laryngeal manipulation: Improves view in 65-75% of cases
- Bougie-assisted intubation: Tactile confirmation of tracheal placement
- Different blade: Switch between curved and straight blades
- Supraglottic Airway Devices: Rescue ventilation when intubation fails
- LMA Classic: Success rate 85-90% in emergency scenarios
- i-gel: Faster insertion with gastric access port
- King LT: Dual-cuff design for difficult anatomy
- Provides adequate ventilation in 90-95% of failed intubation cases
Surgical Airway Indications represent the final rescue technique:
- Cannot Intubate, Cannot Ventilate (CICV): Absolute indication
- Incidence: 1:10,000 elective cases, 1:1,000 emergency cases
- Mortality >80% if surgical airway delayed >10 minutes
- Cricothyrotomy preferred over tracheostomy in emergency
- Technique Requirements: Scalpel-bougie-tube approach
- Vertical skin incision through cricothyroid membrane
- Horizontal membrane incision with scalpel blade
- Bougie insertion followed by 6.0 ETT advancement
- Success rate >95% when performed systematically
⭐ Clinical Pearl: Emergency airway management follows the 3-3-3 rule: 3 attempts at intubation, 3 minutes maximum per attempt, 3 backup plans always prepared. First-pass success is critical - each additional attempt increases complications by 25-30% and mortality by 5-10%.
💡 Master This: Emergency airway mastery transforms life-threatening scenarios into systematic protocols. Master video laryngoscopy techniques, backup planning, and surgical airway skills, and you possess the complete airway arsenal for managing the most challenging emergency scenarios.
Connect these airway management principles through hemodynamic optimization strategies to understand fluid resuscitation and vasopressor management in emergency surgery.
🛡️ Emergency Airway Command: The Life-Saving Gateway Protocol
⚖️ Hemodynamic Optimization Engine: The Circulation Stabilization Matrix
Shock Classification guides targeted resuscitation strategies based on underlying pathophysiology:
| Shock Type | Mechanism | Heart Rate | Blood Pressure | CVP | Treatment Priority |
|---|---|---|---|---|---|
| Hypovolemic | Volume loss | ↑↑ (>120) | ↓↓ (<80) | ↓ (<5) | Fluid resuscitation |
| Cardiogenic | Pump failure | ↑ (100-120) | ↓ (<90) | ↑↑ (>15) | Inotropic support |
| Distributive | Vasodilation | ↑↑ (>110) | ↓↓ (<70) | ↓ (<8) | Vasopressor therapy |
| Obstructive | Outflow obstruction | ↑↑ (>120) | ↓↓ (<70) | ↑↑ (>15) | Relieve obstruction |
| Neurogenic | Sympathetic loss | ↓ (<60) | ↓ (<80) | ↓ (<5) | Vasopressor + fluid |
- Initial Fluid Challenge: 500 mL crystalloid over 15-30 minutes
- Lactated Ringer's: Preferred for hemorrhagic shock
- Normal Saline: Acceptable but hyperchloremic acidosis risk
- Balanced Solutions: Plasma-Lyte or Normosol reduce AKI risk
- Response assessment: MAP increase >10 mmHg or HR decrease >10 bpm
- Fluid Responsiveness Testing: Passive leg raise or stroke volume variation
- Passive leg raise: >10% increase in stroke volume predicts response
- SVV >12% indicates fluid responsiveness in mechanically ventilated patients
- Pulse pressure variation >13% suggests volume responsiveness
- Static pressures (CVP, PCWP) are poor predictors of fluid responsiveness
Vasopressor Selection depends on shock mechanism and desired physiological effects:
- Norepinephrine: First-line for distributive shock
- Mechanism: Alpha-1 agonist with minimal beta effects
- Dose: 0.1-3.0 mcg/kg/min (titrate to MAP >65 mmHg)
- Effects: Vasoconstriction with preserved cardiac output
- Advantages: Minimal tachycardia, improved renal perfusion
- Epinephrine: Mixed alpha/beta agonist for cardiogenic shock
- Mechanism: Alpha + Beta-1 + Beta-2 receptor activation
- Dose: 0.01-0.5 mcg/kg/min (start low, titrate carefully)
- Effects: Increased HR, contractility, and vasoconstriction
- Indications: Cardiac arrest, anaphylaxis, severe cardiogenic shock
- Vasopressin: Non-catecholamine vasopressor for refractory shock
- Mechanism: V1 receptor activation causing vasoconstriction
- Dose: 0.01-0.04 units/min (fixed dose, not weight-based)
- Advantages: Catecholamine-sparing, effective in acidosis
- Limitations: Coronary vasoconstriction, decreased cardiac output
Inotropic Support addresses cardiac contractility in pump failure scenarios:
- Dobutamine: Beta-1 selective inotrope for cardiogenic shock
- Dose: 2.5-20 mcg/kg/min (titrate to cardiac index >2.2)
- Effects: Increased contractility with mild vasodilation
- Monitoring: Cardiac output, mixed venous saturation
- Limitations: Tachycardia, increased oxygen consumption
- Milrinone: Phosphodiesterase inhibitor for heart failure
- Loading dose: 50 mcg/kg over 10 minutes
- Maintenance: 0.375-0.75 mcg/kg/min
- Effects: Inotropic and vasodilatory properties
- Advantages: No tolerance, improved diastolic function
📌 Remember: SHOCK vasopressor selection - Septic shock gets norepinephrine, Heart failure gets dobutamine, Obstructive shock needs cause treatment, Cardiogenic shock gets epinephrine, Keep vasopressin for refractory cases. Mechanism-based selection improves outcomes by 20-30%.
Hemodynamic Monitoring provides real-time feedback for therapeutic adjustments:
- Arterial Line Monitoring: Beat-to-beat blood pressure assessment
- Indications: Vasopressor therapy, frequent blood sampling
- Complications: Thrombosis 1-2%, infection <1%
- Pulse pressure variation: >13% suggests fluid responsiveness
- Central Venous Pressure: Preload assessment with limitations
- Normal range: 8-12 mmHg in mechanically ventilated patients
- Poor predictor of fluid responsiveness (accuracy <60%)
- Useful for: Trend monitoring and drug administration
- Cardiac Output Monitoring: Advanced hemodynamic assessment
- Thermodilution: Gold standard but invasive
- Pulse contour analysis: Less invasive with good correlation
- Echocardiography: Non-invasive but operator-dependent
⭐ Clinical Pearl: Goal-directed therapy improves emergency surgery outcomes by 15-25%. Target MAP >65 mmHg, cardiac index >2.2 L/min/m², ScvO2 >70%, and lactate clearance >10%/hour. Early aggressive resuscitation within first 6 hours determines long-term survival.
💡 Master This: Hemodynamic optimization transforms shock physiology into systematic resuscitation protocols. Master shock classification, fluid responsiveness testing, and vasopressor selection, and you possess the circulation management tools for successful emergency surgery outcomes.
Connect these hemodynamic principles through perioperative monitoring strategies to understand comprehensive patient surveillance during emergency procedures.
⚖️ Hemodynamic Optimization Engine: The Circulation Stabilization Matrix
🔍 Perioperative Surveillance Matrix: The Multi-System Monitoring Command
Standard Monitoring Enhancement adapts routine protocols for emergency scenarios:
- Electrocardiography: 5-lead configuration with ST-segment analysis
- Lead II: Rhythm monitoring and inferior wall ischemia
- Lead V5: Lateral wall ischemia detection (sensitivity 75%)
- ST-segment changes: >1 mm depression suggests myocardial ischemia
- Arrhythmia detection: Automatic algorithms with 95% sensitivity
- Pulse Oximetry: Enhanced accuracy with perfusion index
- Perfusion index >1%: Reliable readings in most patients
- Plethysmographic variability: Fluid responsiveness indicator
- Methemoglobin detection: Co-oximetry when SpO2 discordant
- Limitations: Poor perfusion, nail polish, ambient light
- Capnography: Continuous CO2 monitoring with waveform analysis
- Normal ETCO2: 35-45 mmHg with rectangular waveform
- Sudden decrease: Cardiac arrest, massive PE, circuit disconnect
- Gradual increase: Hypoventilation, CO2 rebreathing, malignant hyperthermia
- Waveform changes: Bronchospasm (shark fin), partial obstruction (slanted)
Invasive Monitoring Indications expand in emergency scenarios due to increased risk:
- Arterial Line Placement: Lower threshold for emergency cases
- Indications: Vasopressor use, frequent blood sampling, hemodynamic instability
- Sites: Radial (first choice), femoral (emergency), brachial (alternative)
- Complications: Thrombosis 1-2%, infection <1%, nerve injury <0.1%
- Benefits: Beat-to-beat BP, pulse pressure variation, immediate lab access
- Central Venous Access: Multi-purpose monitoring and therapy
- Indications: Large-bore access, vasopressor administration, CVP monitoring
- Sites: Internal jugular (preferred), subclavian (pneumothorax risk), femoral (infection risk)
- Monitoring: CVP trends, central venous saturation, blood sampling
- Complications: Pneumothorax 1-3%, arterial puncture 2-5%, infection 1-2%
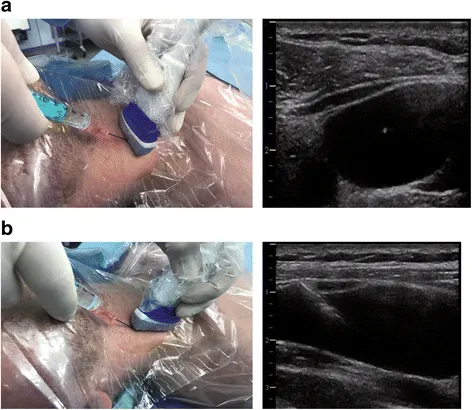
Advanced Hemodynamic Monitoring provides detailed cardiovascular assessment:
| Monitor Type | Parameters | Accuracy | Invasiveness | Emergency Utility |
|---|---|---|---|---|
| Pulmonary Artery Catheter | CO, PCWP, SVR, PVR | Gold standard | High | Selected cases |
| Pulse Contour Analysis | CO, SVV, PPV | Good correlation | Moderate | Preferred method |
| Transesophageal Echo | CO, preload, function | Excellent | Moderate | Diagnostic + monitoring |
| Non-invasive CO | CO, SVR | Variable | Low | Limited emergency use |
- Hemodynamic Assessment: Preload, contractility, afterload evaluation
- Left ventricular filling: End-diastolic area >10 cm² suggests adequate preload
- Ejection fraction: Visual estimation with ±5% accuracy
- Wall motion abnormalities: Regional ischemia detection
- Valve function: Regurgitation and stenosis assessment
- Volume Status Evaluation: Superior to static pressures
- IVC diameter: >2 cm with <50% collapse suggests volume overload
- Left ventricular end-diastolic area: Best preload indicator
- Stroke volume variation: >12% indicates fluid responsiveness
- Real-time guidance: Fluid administration and vasopressor titration
Neurological Monitoring becomes critical in emergency scenarios:
- Bispectral Index (BIS): Depth of anesthesia monitoring
- Target range: 40-60 for adequate anesthesia
- Benefits: Reduced awareness, faster emergence, drug optimization
- Limitations: Electrocautery interference, neuromuscular blockade effects
- Emergency value: Anesthetic titration in hemodynamically unstable patients
- Cerebral Oximetry: Regional brain oxygenation
- Normal values: 60-80% baseline cerebral saturation
- Intervention threshold: >20% decrease from baseline
- Applications: Carotid surgery, cardiac surgery, prone positioning
- Limitations: Scalp blood flow, intracranial pathology interference
📌 Remember: MONITOR emergency priorities - Myocardial ischemia (ECG), Oxygenation (pulse ox + ABG), Neurological status (BIS), Invasive pressures (arterial line), Temperature (core), Output (urine), Respiratory (capnography). Comprehensive monitoring detects complications 30-60 minutes before clinical signs.
Laboratory Monitoring provides metabolic and coagulation assessment:
- Point-of-Care Testing: Rapid results for immediate decisions
- Blood gas analysis: pH, lactate, base deficit, electrolytes
- Hemoglobin: Trending for blood loss assessment
- Coagulation: PT/INR, aPTT, platelet function
- Glucose: Stress hyperglycemia management
- Lactate Monitoring: Tissue perfusion and shock severity
- Normal: <2 mmol/L in healthy patients
- Mild elevation: 2-4 mmol/L suggests compensated shock
- Severe elevation: >4 mmol/L indicates tissue hypoperfusion
- Clearance: >10%/hour predicts improved outcomes
⭐ Clinical Pearl: Early warning systems using multiple parameters detect clinical deterioration 2-6 hours before traditional vital signs. Lactate clearance, base deficit improvement, and ScvO2 >70% are better outcome predictors than blood pressure or heart rate alone.
💡 Master This: Perioperative surveillance transforms routine monitoring into comprehensive physiological assessment. Master enhanced monitoring protocols, advanced hemodynamic assessment, and early warning recognition, and you possess the surveillance tools for detecting and preventing emergency surgery complications.
Connect these monitoring principles through rapid mastery frameworks to understand essential clinical decision-making tools for emergency anesthesia practice.
🔍 Perioperative Surveillance Matrix: The Multi-System Monitoring Command
🎯 Emergency Anesthesia Mastery Arsenal: The Critical Decision Command Center
The Emergency Anesthesia Decision Matrix provides systematic approach to complex scenarios:
| Clinical Scenario | Primary Assessment | Immediate Action | Monitoring Priority | Backup Plan |
|---|---|---|---|---|
| Hemorrhagic Shock | Blood loss + vitals | Fluid + blood products | Arterial line + Hgb | Massive transfusion protocol |
| Full Stomach | Aspiration risk | RSI + cricoid pressure | Capnography + SpO2 | Surgical airway |
| Cardiac Emergency | Ischemia + function | Hemodynamic support | ECG + TEE | IABP + ECMO |
| Airway Crisis | Anatomy + physiology | Video laryngoscopy | Continuous SpO2 | Supraglottic + surgical |
| Septic Shock | Infection + perfusion | Antibiotics + pressors | Lactate + ScvO2 | Steroid therapy |
Rapid Assessment Protocol enables 60-second patient evaluation:
- 10-Second Survey: Life-threatening priorities
- Airway: Patent vs. compromised vs. lost
- Breathing: Adequate vs. inadequate vs. absent
- Circulation: Stable vs. unstable vs. arrest
- Disability: Alert vs. altered vs. unresponsive
- 20-Second Vital Signs: Quantitative assessment
- Heart rate: Trend and rhythm analysis
- Blood pressure: Actual values and pulse pressure
- Oxygen saturation: Baseline and response to oxygen
- Respiratory rate: Pattern and work of breathing
- 30-Second History: Critical background information
- Mechanism of injury or presenting complaint
- Allergies and current medications
- Last meal and aspiration risk
- Comorbidities affecting anesthetic management
Drug Dosing Quick Reference provides weight-based calculations for immediate use:
- Induction Agents (per kg body weight):
- Propofol: 1-2 mg/kg (reduce 50% if hypotensive)
- Etomidate: 0.2-0.3 mg/kg (hemodynamically stable)
- Ketamine: 1-2 mg/kg (sympathomimetic effects)
- Midazolam: 0.1-0.3 mg/kg (anxiolysis/amnesia)
- Neuromuscular Blocking Agents:
- Succinylcholine: 1-1.5 mg/kg (rapid onset/offset)
- Rocuronium: 1.2-1.5 mg/kg (sugammadex reversible)
- Vecuronium: 0.1-0.15 mg/kg (intermediate duration)
- Emergency Medications:
- Epinephrine: 10 mcg/kg IV push (cardiac arrest)
- Atropine: 20 mcg/kg IV (minimum 0.5 mg)
- Naloxone: 0.4-2 mg IV (opioid reversal)
- Flumazenil: 0.2 mg IV (benzodiazepine reversal)
Crisis Management Protocols address common emergency scenarios:
- Cannot Intubate, Cannot Ventilate:
- Step 1: Call for help + 100% oxygen
- Step 2: Supraglottic airway insertion
- Step 3: If unsuccessful, surgical airway
- Timeline: <4 minutes to prevent hypoxic brain injury
- Malignant Hyperthermia:
- Step 1: Discontinue triggers + 100% oxygen
- Step 2: Dantrolene 2.5 mg/kg IV (repeat PRN)
- Step 3: Cooling measures + treat complications
- Timeline: Early recognition reduces mortality to <5%
- Anaphylaxis:
- Step 1: Epinephrine 1 mg IV + fluid bolus
- Step 2: Antihistamines + steroids
- Step 3: Bronchodilators if bronchospasm
- Timeline: Immediate treatment prevents cardiovascular collapse
⭐ Clinical Pearl: Cognitive aids and crisis checklists improve emergency performance by 25-40% and reduce medical errors by 50-70%. Memory fails under stress - systematic protocols and visual aids ensure consistent high-quality care during critical scenarios.
Essential Numbers Arsenal for immediate clinical reference:
- Hemodynamic Targets:
- MAP: >65 mmHg (organ perfusion threshold)
- Cardiac Index: >2.2 L/min/m² (adequate output)
- ScvO2: >70% (oxygen delivery/consumption balance)
- Lactate: <2 mmol/L (normal tissue perfusion)
- Ventilation Parameters:
- Tidal Volume: 6-8 mL/kg ideal body weight
- PEEP: 5-10 cmH2O (lung recruitment)
- FiO2: Lowest to maintain SpO2 >95%
- Plateau Pressure: <30 cmH2O (lung protection)
- Transfusion Triggers:
- Hemoglobin: <7 g/dL (stable patients)
- Hemoglobin: <9 g/dL (cardiac disease)
- Platelets: <50,000 (active bleeding)
- INR: >1.5 (surgical bleeding)
💡 Master This: Emergency anesthesia mastery transforms crisis scenarios into systematic protocols. Master rapid assessment frameworks, drug dosing calculations, and crisis management algorithms, and you possess the complete clinical arsenal for safe and effective emergency anesthesia practice under any circumstances.
🎯 Emergency Anesthesia Mastery Arsenal: The Critical Decision Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























