Pectoral Girdle Joints - Shoulder's Anchor
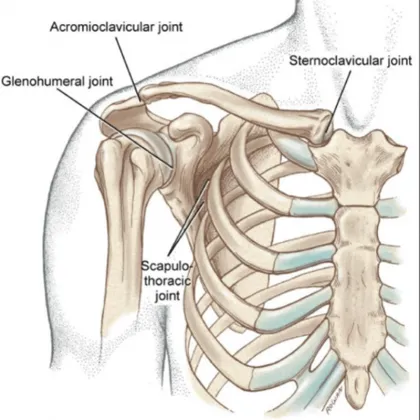
- Sternoclavicular (SC) Joint:
- Type: Saddle synovial; only true bony articulation of upper limb to axial skeleton.
- Components: Medial clavicle, manubrium, 1st costal cartilage. Intra-articular disc present.
- Stability: Strong capsule; Ant/Post Sternoclavicular, Interclavicular, Costoclavicular (primary stabilizer) ligaments.
- Movements: Elevation/depression, protraction/retraction, rotation (~30-35°).
- Acromioclavicular (AC) Joint:
- Type: Plane synovial.
- Components: Lateral clavicle, acromion. Incomplete intra-articular disc.
- Stability: Weak capsule; Acromioclavicular ligament. Coracoclavicular ligament (conoid & trapezoid) is main extrinsic stabilizer, preventing superior displacement of clavicle.
- Movements: Gliding, allows scapular rotation on thoracic cage (scapulothoracic rhythm).
⭐ The SC joint is rarely dislocated due to its strong ligamentous support; posterior dislocation is a medical emergency due to risk to mediastinal structures.
Glenohumeral Joint - Mobile Marvel
- Type: Synovial, ball-and-socket, multiaxial.
- Articular Surfaces: Large, round humeral head & shallow glenoid fossa of scapula.
- Glenoid labrum: fibrocartilaginous rim; deepens fossa by 50%.
- Capsule: Lax inferiorly (allows abduction); attaches to anatomical neck of humerus & glenoid margin.
- Openings: long head of biceps tendon, subscapular bursa.
- Ligaments:
- Glenohumeral (superior, middle, inferior): thickenings of anterior capsule.
- Coracohumeral: superiorly strengthens capsule.
- Transverse humeral: holds biceps tendon in intertubercular groove.
- Stability: Primarily dynamic (muscles) > static (ligaments).
- Rotator cuff muscles (SITS): Supraspinatus, Infraspinatus, Teres minor, Subscapularis.
- Long head of biceps brachii.
- Movements: Flexion, extension, abduction, adduction, medial rotation, lateral rotation, circumduction.

- Blood Supply: Anterior & posterior circumflex humeral arteries, suprascapular artery.
- Nerve Supply: Suprascapular, axillary, lateral pectoral nerves (Hilton's Law).
⭐ Most commonly dislocated large joint in the body; usually anteriorly (anteroinferiorly). Axillary nerve is most commonly injured in anterior dislocation.
📌 SITS for Rotator Cuff muscles: Supraspinatus, Infraspinatus, Teres minor, Subscapularis.
Elbow & Radioulnar Joints - Flexion & Rotation Hub
- Elbow Joint (Synovial Hinge): A complex joint.
- Components:
- Humeroulnar: Trochlea (humerus) with Trochlear notch (ulna). Primary for flexion/extension.
- Humeroradial: Capitulum (humerus) with Head (radius).
- Movements: Flexion (Brachialis, Biceps brachii, Brachioradialis), Extension (Triceps brachii, Anconeus).
- Ligaments: Medial (Ulnar) Collateral Lig. (MCL/UCL), Lateral (Radial) Collateral Lig. (LCL/RCL).
- Carrying Angle: ~5-15° valgus; more pronounced in females.
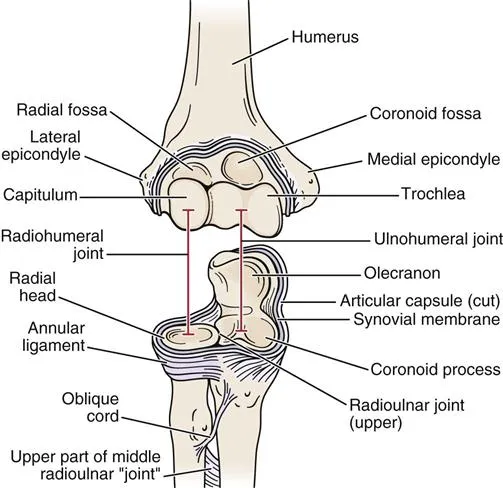
- Components:
- Radioulnar Joints (Synovial Pivot):
- Superior: Head of radius in radial notch of ulna; stabilized by Annular ligament.
- Inferior: Head of ulna in ulnar notch of radius; Triangular Fibrocartilage Complex (TFCC) is key.
- Movements: Pronation (Pronator teres, Pronator quadratus), Supination (Supinator, Biceps brachii).
⭐ Nursemaid's elbow (pulled elbow): Subluxation of radial head under annular ligament in children (typically 1-4 years) due to sudden pull on extended, pronated forearm.
Wrist & Hand Joints - Dexterity's Domain
- Radiocarpal (Wrist): Ellipsoid. Radius & disc with Scaphoid, Lunate, Triquetrum. Ulna excluded. Actions: Flex/Ext, Add/Abd, Circumduction.
- Intercarpal: Plane. Gliding between carpals. Midcarpal joint important.
- **Carpometacarpal (CMC):
- 1st (Thumb): Saddle. Trapezium & 1st Metacarpal. Key for opposition.
- 2nd-5th: Plane. Limited movement.
- Metacarpophalangeal (MCP): Condyloid. Actions: Flex/Ext, Add/Abd.
- Interphalangeal (IP): Hinge. PIP & DIP in fingers. Actions: Flex/Ext only.
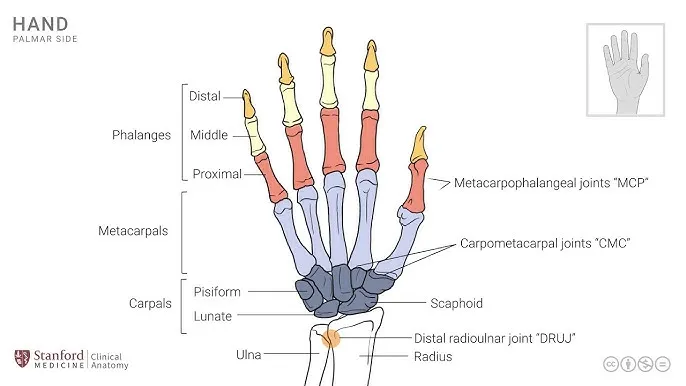
⭐ The 1st CMC joint (thumb), a saddle type, is vital for opposition.
High‑Yield Points - ⚡ Biggest Takeaways
- Shoulder joint: Most mobile, commonest anterior dislocation; rotator cuff for stability.
- Elbow joint: Hinge & pivot functions; site of Nursemaid's elbow and carrying angle.
- Wrist joint: Condyloid type; scaphoid fracture risks avascular necrosis.
- Sternoclavicular joint: Saddle type; sole bony link to axial skeleton.
- Acromioclavicular joint: Plane type; common for separation.
- Axillary nerve vulnerable in shoulder dislocation; Median nerve in carpal tunnel.
- Pronation/supination occurs at radioulnar joints (pivot).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

