Upper Limb

On this page
🗺️ Vascular Lifelines: The Upper Limb's Blood Highway System
The upper limb's arterial network transforms a single axillary trunk into fingertip perfusion through seven major arterial segments and countless anastomoses. Master this vascular geography, and you predict collateral flow patterns, identify bleeding sources, and understand ischemic territories with precision. Every pulse point, every anastomotic pathway, and every clinical measurement depends on understanding this three-dimensional arterial architecture from subclavian origin to digital termination.
The arterial supply to the upper limb follows a remarkably consistent pattern: the subclavian artery becomes the axillary artery at the lateral border of the first rib, transforms into the brachial artery at the lower border of teres major, and bifurcates into radial and ulnar arteries at the level of the radial neck (1 cm distal to the bicipital aponeurosis). This sequential transformation creates predictable injury patterns and collateral pathways that define clinical presentations.
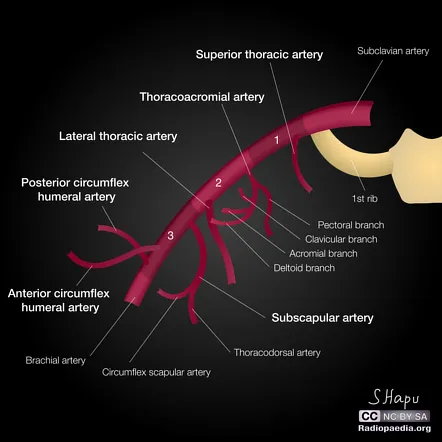
Axillary Artery: The Central Distribution Hub
The axillary artery extends from the lateral border of the first rib to the lower border of teres major, spanning approximately 12-15 cm in length. Pectoralis minor divides it into three anatomical parts with escalating branch complexity: 1 branch from the first part, 2 branches from the second part, and 3 branches from the third part.
📌 Remember: "Screw The Lawyers, Save A Patient" maps axillary branches from proximal to distal:
- Superior thoracic (first part)
- Thoracoacromial and Lateral thoracic (second part)
- Subscapular, Anterior circumflex humeral, Posterior circumflex humeral (third part) This mnemonic predicts 100% of major axillary branches and their sequence, critical for identifying bleeding sources during axillary surgery.
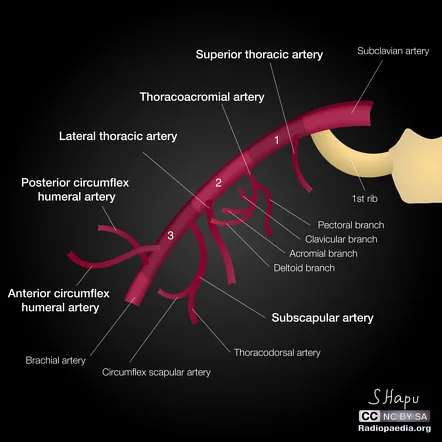
First Part Relations (medial to pectoralis minor):
- Anteriorly: Pectoralis major, clavipectoral fascia, lateral pectoral nerve
- Posteriorly: Long thoracic nerve on serratus anterior, medial pectoral nerve
- Medially: Axillary vein (separated by medial cord of brachial plexus)
- Laterally: Lateral, posterior, and medial cords of brachial plexus surround the artery
- Single branch: Superior thoracic artery supplies upper 2 intercostal spaces
Second Part Relations (deep to pectoralis minor):
- Anteriorly: Pectoralis minor and major muscles
- Posteriorly: Posterior cord and subscapularis muscle
- Medially: Medial cord and axillary vein
- Laterally: Lateral cord
- Two branches: Thoracoacromial (pierces clavipectoral fascia with 4 terminal branches: pectoral, acromial, clavicular, deltoid) and lateral thoracic (follows lower border of pectoralis minor)
⭐ Clinical Pearl: The thoracoacromial artery's four terminal branches create a vascular "square" around the shoulder, providing collateral flow when the axillary artery is compromised. In 85% of axillary artery injuries, this collateral network maintains distal perfusion if the injury occurs proximal to the third part.
Third Part Relations (lateral to pectoralis minor):
- Anteriorly: Pectoralis major (its lower border marks the surgical landmark)
- Posteriorly: Subscapularis, latissimus dorsi, teres major
- Medially: Medial cutaneous nerve of arm and forearm, ulnar nerve, axillary vein
- Laterally: Coracobrachialis, musculocutaneous nerve (enters coracobrachialis at this level), median nerve
- Three branches: Subscapular (largest branch, 10-12 mm diameter, divides into circumflex scapular and thoracodorsal), anterior circumflex humeral (3-4 mm, passes anterior to surgical neck), posterior circumflex humeral (passes through quadrangular space with axillary nerve)
| Axillary Part | Pectoralis Minor Relation | Number of Branches | Key Branch(es) | Diameter (mm) | Collateral Potential |
|---|---|---|---|---|---|
| First | Medial | 1 | Superior thoracic | 4-5 | Minimal |
| Second | Posterior | 2 | Thoracoacromial, Lateral thoracic | 5-6, 3-4 | Moderate (60% flow) |
| Third | Lateral | 3 | Subscapular, Circumflex humeral (A/P) | 10-12, 3-4 | Excellent (90% flow) |
💡 Master This: The axillary artery's three-part division predicts collateral adequacy in proximal occlusion. First-part occlusion has minimal collateral support; second-part occlusion receives moderate collateral flow (60% of normal) via thoracoacromial connections; third-part occlusion maintains excellent collateral flow (>90%) through subscapular and circumflex humeral anastomoses. This explains why first-part injuries cause immediate ischemia while third-part injuries may remain asymptomatic.
Scapular Anastomosis: The Shoulder's Safety Network
The scapular anastomosis represents one of the body's most robust collateral networks, connecting thyrocervical trunk branches (from subclavian) with axillary artery branches around the scapula. This network can maintain up to 80% of normal upper limb perfusion when the axillary artery is occluded between thyrocervical and subscapular branches.
Anastomotic Connections:
- Suprascapular artery (from thyrocervical trunk) → Circumflex scapular artery (from subscapular)
- Connect around scapular neck through suprascapular notch and spinoglenoid notch
- Provides primary collateral pathway in axillary artery occlusion
- Maintains 70-80% of resting blood flow to upper limb
- Dorsal scapular artery (from subclavian or thyrocervical) → Subscapular artery
- Runs along medial scapular border
- Supplies rhomboids and levator scapulae
- Provides secondary collateral pathway (40-50% flow capacity)
- Posterior circumflex humeral → Anterior circumflex humeral
- Form complete ring around surgical neck of humerus
- Critical for humeral head perfusion
- Compromise in displaced surgical neck fractures causes avascular necrosis in 15-20% of cases
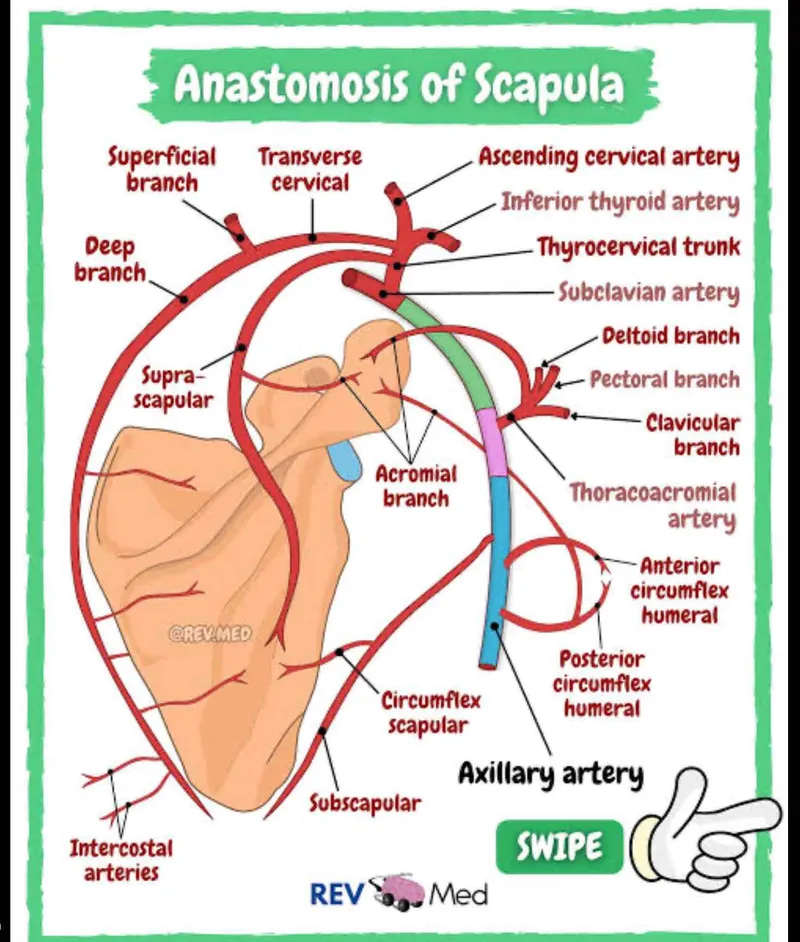
⭐ Clinical Pearl: The scapular anastomosis explains why gradual axillary artery occlusion (atherosclerosis) rarely causes limb-threatening ischemia, while acute occlusion (trauma, embolism) causes severe ischemia in >90% of cases. Collateral development requires 2-3 weeks of progressive stenosis to achieve adequate compensatory flow.
The scapular anastomosis creates a vascular "watershed" around the scapula, connecting four arterial sources: subclavian (via thyrocervical), axillary (via subscapular and circumflex humeral), internal thoracic (via intercostal perforators), and thoracic aorta (via posterior intercostals). This redundancy ensures shoulder perfusion even with multiple arterial injuries.
Connect these axillary patterns through to understand how neurovascular relationships predict injury patterns, then advance to brachial artery anatomy to see how this single-vessel territory creates unique vulnerability patterns.
🗺️ Vascular Lifelines: The Upper Limb's Blood Highway System
📚 The Brachial Pipeline: Arm's Singular Arterial Conduit
The brachial artery represents a critical transition from the rich collateral network of the shoulder to a single-vessel system supplying the entire forearm and hand. Extending from the lower border of teres major to 1 cm distal to the bicipital aponeurosis (at the level of the radial neck), this 12-15 cm segment carries the entire arterial supply with minimal collateral support, making injuries potentially limb-threatening.
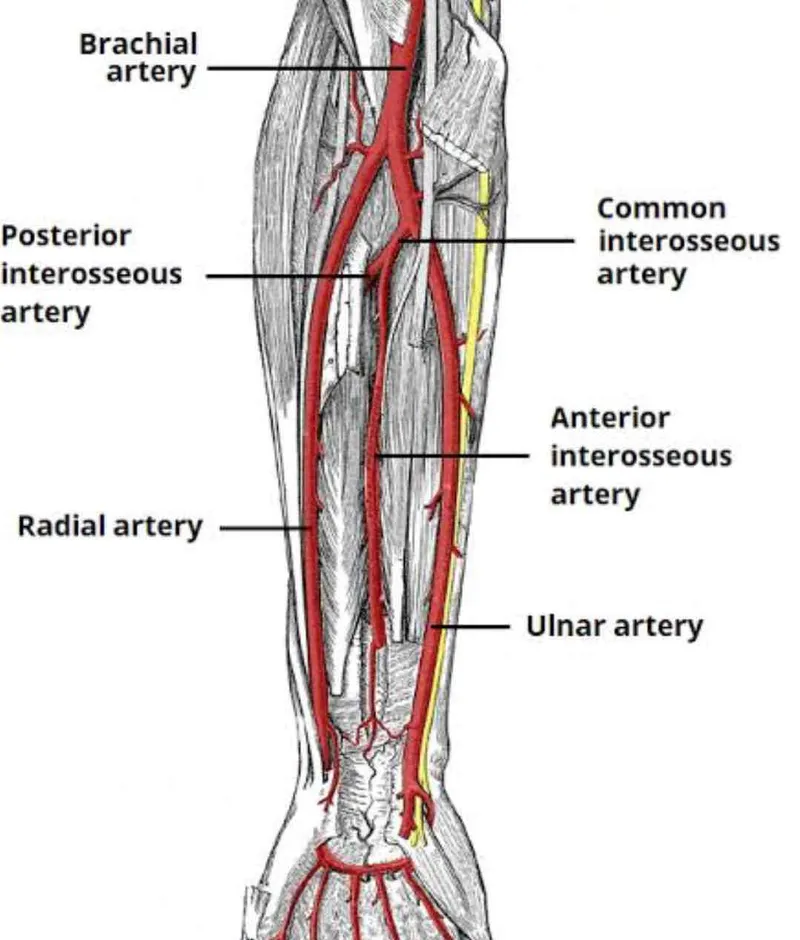
Brachial Artery Anatomical Relations and Clinical Implications
The brachial artery descends through the medial bicipital groove, maintaining consistent relationships that define safe surgical approaches and predict nerve injury patterns in trauma.
Proximal Arm Relations (upper third):
- Anteriorly: Skin, superficial fascia, median nerve (crosses from lateral to medial at mid-arm)
- Posteriorly: Long head of triceps, radial nerve (separated by medial head of triceps)
- Medially: Ulnar nerve and medial cutaneous nerve of forearm (up to mid-arm where ulnar nerve pierces medial intermuscular septum)
- Laterally: Coracobrachialis (proximal), biceps brachii, median nerve (proximal)
- Venae comitantes: Two accompanying veins that frequently communicate across the artery (risk of venous injury during arterial repair)
Mid-Arm Relations (middle third):
- Median nerve crossing: Nerve crosses from lateral to medial at mid-arm level (variable, 35-45% of arm length from acromion)
- Basilic vein: Pierces deep fascia at this level, joining brachial venae comitantes to form axillary vein
- Ulnar nerve departure: Pierces medial intermuscular septum to enter posterior compartment at junction of middle and distal thirds
- Profunda brachii: Already departed proximally (within 3-5 cm of teres major), travels with radial nerve
Distal Arm and Cubital Fossa Relations:
- Anteriorly: Bicipital aponeurosis (protects artery during venipuncture), median cubital vein (superficial to aponeurosis)
- Posteriorly: Brachialis muscle, supinator (at bifurcation level)
- Medially: Median nerve (throughout cubital fossa)
- Laterally: Biceps tendon (proximal), radial nerve between brachialis and brachioradialis (distal)
- Bifurcation point: At level of radial neck, 1 cm distal to bicipital aponeurosis, into radial and ulnar arteries
📌 Remember: "MARBLE" maps medial-to-lateral structures at the cubital fossa from medial to lateral:
- Median nerve
- Artery (brachial)
- Radial nerve (between brachialis and brachioradialis)
- Biceps tendon
- Lateral cutaneous nerve of forearm (terminal branch of musculocutaneous)
- Epicondyle (lateral, as landmark) This sequence predicts 95% of neurovascular injuries during cubital fossa procedures and guides safe antecubital vein access.
Brachial Artery Branches: Minimal Collateral Architecture
Unlike the axillary artery's extensive branching, the brachial artery gives off only 4-5 major branches, creating minimal collateral support and explaining the high risk of distal ischemia with brachial injuries.
- Profunda brachii (deep brachial artery)
- Largest branch (5-7 mm diameter), arises within 3-5 cm of teres major
- Accompanies radial nerve through spiral groove
- Divides into radial collateral (anastomoses with radial recurrent) and middle collateral (anastomoses with interosseous recurrent)
- Provides primary blood supply to posterior compartment and secondary collateral to elbow joint
- Injury in humeral shaft fractures causes posterior compartment ischemia in 5-8% of cases
- Superior ulnar collateral artery
- Arises near mid-arm level
- Accompanies ulnar nerve through medial intermuscular septum
- Anastomoses with posterior ulnar recurrent and inferior ulnar collateral
- Diameter 2-3 mm, provides medial elbow collateral flow
- Inferior ulnar collateral artery
- Arises 5-8 cm proximal to elbow joint
- Passes anterior to medial epicondyle
- Anastomoses with anterior ulnar recurrent
- Contributes to cubital anastomosis with 15-20% of elbow collateral flow
- Nutrient artery to humerus
- Arises at mid-arm level
- Enters nutrient foramen on anteromedial surface of humeral shaft
- Provides primary blood supply to humeral diaphysis
- Compromise in mid-shaft fractures delays union in 10-15% of cases
- Muscular branches
- Multiple small branches (1-2 mm) to biceps, brachialis, coracobrachialis
- Minimal collateral contribution
| Branch | Origin Level | Diameter (mm) | Accompanies | Anastomoses With | Collateral Capacity |
|---|---|---|---|---|---|
| Profunda brachii | Proximal (3-5 cm from teres major) | 5-7 | Radial nerve | Radial recurrent, interosseous recurrent | 40-50% |
| Superior ulnar collateral | Mid-arm | 2-3 | Ulnar nerve | Posterior ulnar recurrent | 15-20% |
| Inferior ulnar collateral | Distal (5-8 cm from elbow) | 2-3 | None | Anterior ulnar recurrent | 15-20% |
| Nutrient artery | Mid-arm | 1-2 | None | Intramedullary network | Minimal |
| Muscular branches | Throughout | 1-2 | None | Minimal | Minimal |
⭐ Clinical Pearl: The brachial artery's limited collateral network means that occlusion at any level risks distal ischemia. The profunda brachii provides the only significant collateral pathway (40-50% of resting flow), explaining why supracondylar humeral fractures with brachial artery injury cause acute hand ischemia in >95% of cases when profunda collaterals are insufficient.
💡 Master This: Brachial artery pulse assessment reveals three critical zones: Proximal arm pulse (axillary-to-profunda segment), mid-arm pulse (main trunk), and cubital fossa pulse (pre-bifurcation). Loss of proximal pulse with preserved distal pulses suggests collateral flow via profunda brachii; loss of all pulses indicates main trunk occlusion requiring immediate intervention. In traumatic brachial injury, presence of radial pulse does NOT exclude significant arterial injury-15-20% of patients with brachial intimal tears maintain distal pulses via collaterals until thrombosis propagates.
Cubital Anastomosis: The Elbow's Collateral Network
The cubital anastomosis forms a rich vascular network around the elbow joint, connecting brachial artery branches with radial, ulnar, and interosseous recurrent arteries. This network maintains forearm perfusion when the brachial artery is occluded proximal to its bifurcation.
Anastomotic Components:
- Radial collateral (from profunda brachii) ↔ Radial recurrent (from radial artery)
- Anastomose anterior to lateral epicondyle
- Provide lateral elbow collateral flow
- Contribute 25-30% of total cubital anastomotic capacity
- Middle collateral (from profunda brachii) ↔ Interosseous recurrent (from posterior interosseous artery)
- Anastomose posterior to lateral epicondyle
- Provide posterior elbow collateral flow
- Contribute 20-25% of cubital anastomotic capacity
- Superior ulnar collateral ↔ Posterior ulnar recurrent (from ulnar artery)
- Anastomose posterior to medial epicondyle
- Provide medial posterior collateral flow
- Contribute 20-25% of cubital anastomotic capacity
- Inferior ulnar collateral ↔ Anterior ulnar recurrent (from ulnar artery)
- Anastomose anterior to medial epicondyle
- Provide medial anterior collateral flow
- Contribute 15-20% of cubital anastomotic capacity
⭐ Clinical Pearl: The cubital anastomosis can maintain up to 70% of resting forearm blood flow when the brachial artery is occluded proximal to the bifurcation but distal to profunda brachii origin. However, if occlusion occurs proximal to profunda origin, collateral flow drops to <30%, causing forearm claudication and hand ischemia in >80% of cases.
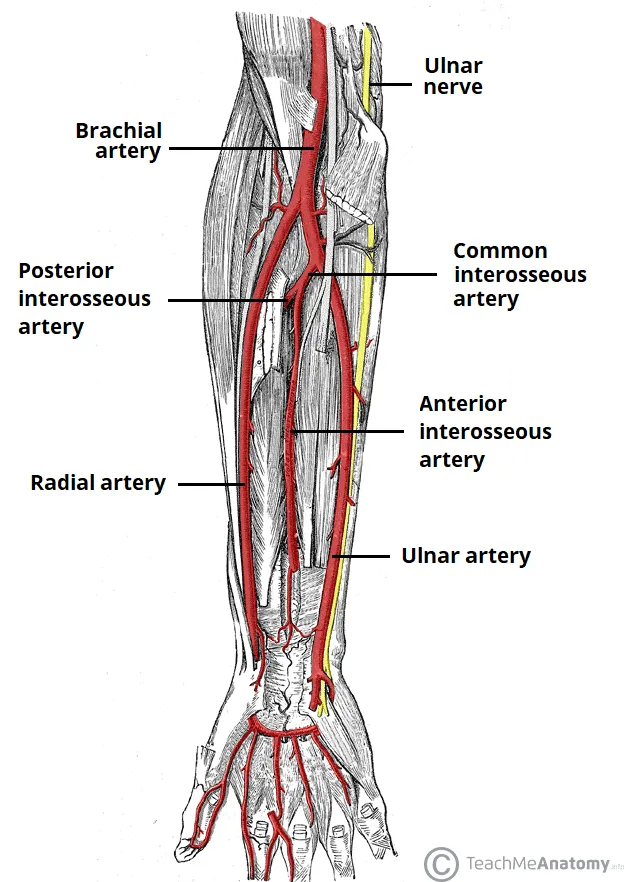
The cubital anastomosis creates a circumferential vascular ring around the elbow, explaining why isolated radial or ulnar artery injuries at the forearm rarely cause hand ischemia-the intact vessel maintains perfusion via palmar arch connections. However, combined brachial artery injury with elbow dislocation disrupts this network, causing acute forearm compartment syndrome in 30-40% of cases due to collateral vessel stretching and tearing.
Connect these brachial patterns through to understand how single-vessel anatomy creates unique injury vulnerabilities, then advance to forearm arterial anatomy to master the dual-vessel perfusion system and palmar arch architecture.
📚 The Brachial Pipeline: Arm's Singular Arterial Conduit
🔬 Forearm's Dual Highways: Radial and Ulnar Arterial Territories
The brachial artery bifurcates at the level of the radial neck (1 cm distal to bicipital aponeurosis) into radial and ulnar arteries, creating a dual-vessel system that provides redundancy and maintains hand perfusion even when one vessel is compromised. This anatomical redundancy explains why isolated radial or ulnar artery injuries rarely cause hand ischemia-the intact vessel maintains 70-85% of normal palmar perfusion via rich palmar arch anastomoses.
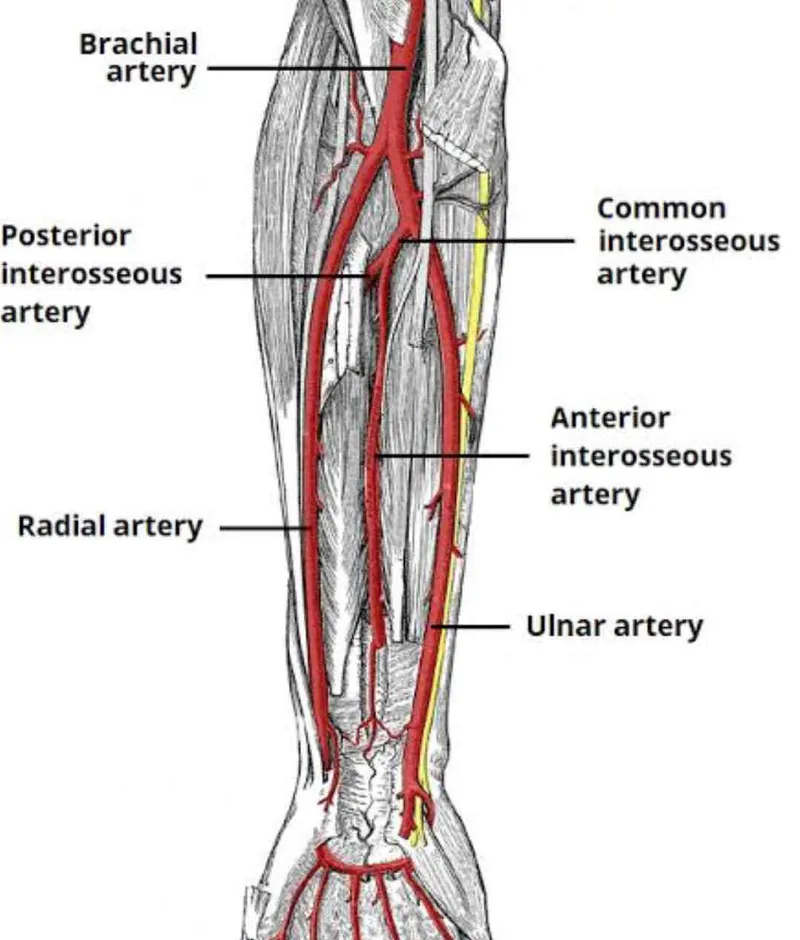
Radial Artery: The Lateral Forearm Conduit
The radial artery represents the smaller of the two forearm vessels (diameter 2.5-3.5 mm vs ulnar 3-4 mm), but provides the dominant blood supply to the thumb and lateral hand via the deep palmar arch in >80% of individuals. Its superficial course in the distal forearm makes it the preferred site for pulse assessment, arterial blood gas sampling, and radial artery catheterization.
Radial Artery Course and Relations:
- Proximal forearm (upper third):
- Lies on biceps tendon, then passes between brachioradialis (laterally) and pronator teres (medially)
- Covered by brachioradialis muscle belly
- Lateral cutaneous nerve of forearm lies immediately lateral
- Gives off radial recurrent artery (ascends to anastomose with radial collateral)
- Mid-forearm (middle third):
- Lies on flexor digitorum superficialis, flexor pollicis longus, pronator quadratus
- Covered only by brachioradialis tendon and deep fascia
- Superficial branch of radial nerve crosses from lateral to posterior at junction of middle and distal thirds
- Accompanied by two venae comitantes
- Distal forearm (lower third):
- Becomes subcutaneous between brachioradialis and flexor carpi radialis tendons
- Lies on pronator quadratus and distal radius
- Most accessible site for pulse palpation and arterial cannulation
- Superficial branch of radial nerve now lies posterior (risk of injury during arterial access)
- Wrist and hand:
- Passes dorsally around radial styloid in anatomical snuffbox
- Pierces first dorsal interosseous muscle to enter palm
- Forms deep palmar arch with deep branch of ulnar artery
📌 Remember: "BFPP" maps radial artery's posterior relations from proximal to distal:
- Biceps tendon (proximal)
- Flexor digitorum superficialis (proximal-mid)
- Flexor pollicis longus (mid)
- Pronator quadratus (distal) This sequence predicts the four zones of radial artery exposure for surgical access and guides identification during trauma exploration.
Radial Artery Branches:
- Radial recurrent artery (proximal)
- Arises 2-3 cm distal to bifurcation
- Ascends between brachioradialis and brachialis
- Anastomoses with radial collateral (from profunda brachii)
- Contributes 25-30% of cubital anastomotic flow
- Diameter 1.5-2 mm
- Muscular branches (throughout)
- Supply brachioradialis, radial flexors, extensors
- Minimal collateral contribution
- Palmar carpal branch (distal)
- Arises at distal radius level
- Anastomoses with palmar carpal branch of ulnar to form palmar carpal arch
- Provides carpal bone perfusion
- Diameter 0.5-1 mm
- Superficial palmar branch (distal)
- Arises at radial styloid level
- Passes through thenar muscles
- Completes superficial palmar arch in 30-40% of individuals
- When absent, superficial arch is completed by ulnar artery alone
- Diameter 1-2 mm
- Dorsal carpal branch (wrist)
- Arises as radial artery passes dorsally around wrist
- Anastomoses with dorsal carpal branch of ulnar and anterior/posterior interosseous to form dorsal carpal arch
- Gives off dorsal metacarpal arteries
- Diameter 1-1.5 mm
- First dorsal metacarpal artery (hand)
- Arises as radial artery pierces first dorsal interosseous
- Divides into princeps pollicis (thumb) and radialis indicis (lateral index finger)
- Provides dominant blood supply to thumb in >95% of cases
- Diameter 1.5-2 mm
- Deep palmar arch (hand)
- Terminal continuation of radial artery
- Anastomoses with deep branch of ulnar artery
- Gives off palmar metacarpal arteries (supply interossei and contribute to common digital arteries)
- Complete arch in >95% of individuals
- Diameter 2-3 mm
⭐ Clinical Pearl: The radial artery's superficial distal course makes it vulnerable to laceration injuries but ideal for Allen test assessment of palmar arch patency before radial artery harvesting. The test has sensitivity 73-97% and specificity 97% for detecting inadequate ulnar collateral flow. However, false negatives occur in 3-5% due to incomplete palmar arch variants, emphasizing the need for pulse oximetry confirmation during radial artery compression.
Ulnar Artery: The Dominant Forearm Vessel
The ulnar artery represents the larger of the two forearm vessels (diameter 3-4 mm) and provides the dominant blood supply to the superficial palmar arch in >95% of individuals. Its deep proximal course protects it from injury but complicates surgical access, while its superficial distal course at the wrist creates vulnerability to laceration and thrombosis.
Ulnar Artery Course and Relations:
- Proximal forearm (upper third):
- Passes deep to pronator teres, flexor carpi radialis, palmaris longus, flexor digitorum superficialis (all heads)
- Lies on brachialis and flexor digitorum profundus
- Median nerve lies immediately medial (risk of injury during ulnar artery exposure)
- Gives off anterior and posterior ulnar recurrent arteries (ascend to cubital anastomosis)
- Gives off common interosseous artery at 2-3 cm distal to bifurcation
- Mid-forearm (middle third):
- Emerges from beneath flexor digitorum superficialis
- Lies on flexor digitorum profundus
- Ulnar nerve joins artery at junction of upper and middle thirds, lying medially
- Covered by flexor carpi ulnaris (medially) and flexor digitorum superficialis (laterally)
- Distal forearm (lower third):
- Becomes more superficial between flexor carpi ulnaris and flexor digitorum superficialis
- Ulnar nerve lies immediately medial (neurovascular bundle)
- Lies on flexor digitorum profundus and pronator quadratus
- Covered only by skin, superficial fascia, and deep fascia (vulnerable to laceration)
- Wrist and hand:
- Passes superficial to flexor retinaculum in Guyon's canal with ulnar nerve
- Divides into superficial and deep branches
- Superficial branch forms superficial palmar arch
- Deep branch anastomoses with radial artery to complete deep palmar arch
Ulnar Artery Branches:
- Anterior ulnar recurrent artery (proximal)
- Arises immediately distal to bifurcation
- Ascends anterior to medial epicondyle
- Anastomoses with inferior ulnar collateral
- Contributes 15-20% of cubital anastomotic flow
- Diameter 1.5-2 mm
- Posterior ulnar recurrent artery (proximal)
- Arises 1-2 cm distal to bifurcation
- Ascends posterior to medial epicondyle between two heads of flexor carpi ulnaris
- Anastomoses with superior ulnar collateral
- Contributes 20-25% of cubital anastomotic flow
- Diameter 1.5-2 mm
- Common interosseous artery (proximal)
- Arises 2-3 cm distal to bifurcation (at level of radial tuberosity)
- Travels posteriorly toward interosseous membrane
- Divides into anterior and posterior interosseous arteries after 1-2 cm
- Diameter 2-3 mm (proximal), 1-2 mm (branches)
- Muscular branches (throughout)
- Supply ulnar flexors and profundus
- Minimal collateral contribution
- Palmar carpal branch (distal)
- Arises at distal ulna level
- Anastomoses with palmar carpal branch of radial to form palmar carpal arch
- Provides carpal bone perfusion (especially lunate and scaphoid)
- Diameter 0.5-1 mm
- Dorsal carpal branch (wrist)
- Arises at wrist level, passes dorsally beneath flexor carpi ulnaris tendon
- Anastomoses with dorsal carpal branch of radial and posterior interosseous to form dorsal carpal arch
- Diameter 1-1.5 mm
- Superficial palmar arch (hand)
- Terminal continuation of ulnar artery
- Passes superficial to flexor tendons and lumbricals
- Gives off three common palmar digital arteries (supply medial three web spaces)
- Complete arch (anastomoses with superficial palmar branch of radial) in 30-40%; incomplete in 60-70%
- Diameter 2.5-3.5 mm
- Deep branch (hand)
- Arises in Guyon's canal
- Passes deep with deep branch of ulnar nerve
- Anastomoses with radial artery to complete deep palmar arch
- Diameter 1-2 mm
📌 Remember: "APCI" maps proximal ulnar artery branches in order:
- Anterior ulnar recurrent (first branch, immediate)
- Posterior ulnar recurrent (second branch, 1-2 cm distal)
- Common interosseous (third branch, 2-3 cm distal)
- Interosseous branches (anterior and posterior, from common interosseous) This sequence predicts 100% of proximal ulnar branches and guides surgical ligation during trauma control.
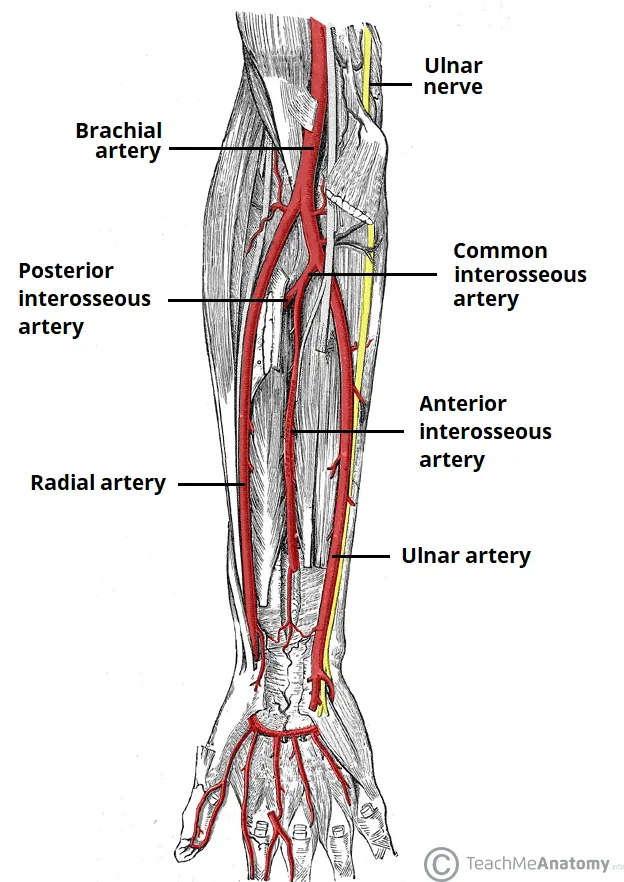
Interosseous Arteries: The Deep Forearm Network
The common interosseous artery arises from the ulnar artery 2-3 cm distal to the brachial bifurcation and divides into anterior and posterior interosseous arteries after 1-2 cm. These vessels provide deep compartment perfusion and contribute to carpal and cubital anastomoses, maintaining forearm viability when both radial and ulnar arteries are compromised.
- Anterior interosseous artery:
- Descends on anterior surface of interosseous membrane
- Lies between flexor digitorum profundus and flexor pollicis longus
- Accompanied by anterior interosseous nerve (from median)
- Supplies deep flexor compartment and median nerve
- Gives off median artery (persistent in 10-15%, accompanies median nerve to hand)
- Pierces interosseous membrane distally to anastomose with posterior interosseous and contribute to dorsal carpal arch
- Diameter 1-2 mm
- Posterior interosseous artery:
- Passes posteriorly above interosseous membrane
- Descends between superficial and deep extensor layers
- Accompanied by posterior interosseous nerve (from radial)
- Supplies extensor compartment
- Gives off interosseous recurrent (ascends to anastomose with middle collateral in cubital anastomosis)
- Anastomoses with anterior interosseous and contributes to dorsal carpal arch
- Diameter 1-2 mm
💡 Master This: The interosseous arteries provide critical collateral pathways when both radial and ulnar arteries are compromised. In combined radial-ulnar artery occlusion, the interosseous system can maintain up to 40% of resting hand blood flow via palmar carpal and dorsal carpal arches. However, this collateral capacity requires intact common interosseous origin-if occlusion occurs proximal to common interosseous takeoff, hand ischemia develops in >90% of cases.
| Forearm Artery | Origin | Diameter (mm) | Course | Terminal Distribution | Collateral Capacity |
|---|---|---|---|---|---|
| Radial | Brachial bifurcation | 2.5-3.5 | Lateral, superficial distally | Deep palmar arch (>80%), thumb | 70-85% (via palmar arches) |
| Ulnar | Brachial bifurcation | 3-4 | Medial, deep proximally | Superficial palmar arch (>95%) | 70-85% (via palmar arches) |
| Anterior interosseous | Common interosseous | 1-2 | Anterior to membrane | Palmar carpal arch, median nerve | 30-40% (via carpal arches) |
| Posterior interosseous | Common interosseous | 1-2 | Posterior to membrane | Dorsal carpal arch, extensors | 20-30% (via carpal arches) |
| Common interosseous | Ulnar (2-3 cm distal) | 2-3 | Posterior toward membrane | Divides into anterior/posterior | Critical for deep collaterals |
Connect these forearm patterns through to understand how dual-vessel anatomy creates redundancy, then advance to palmar arch architecture to master hand perfusion territories and clinical implications of arch variations.
🔬 Forearm's Dual Highways: Radial and Ulnar Arterial Territories
🏥 Palmar Arch Architecture: Hand's Vascular Redundancy System
The hand receives arterial supply through two interconnected arches-the superficial palmar arch (formed primarily by ulnar artery) and the deep palmar arch (formed primarily by radial artery). This dual-arch system creates remarkable vascular redundancy, explaining why isolated digital artery injuries rarely cause finger necrosis and why thumb replantation succeeds with single arterial anastomosis in >85% of cases.
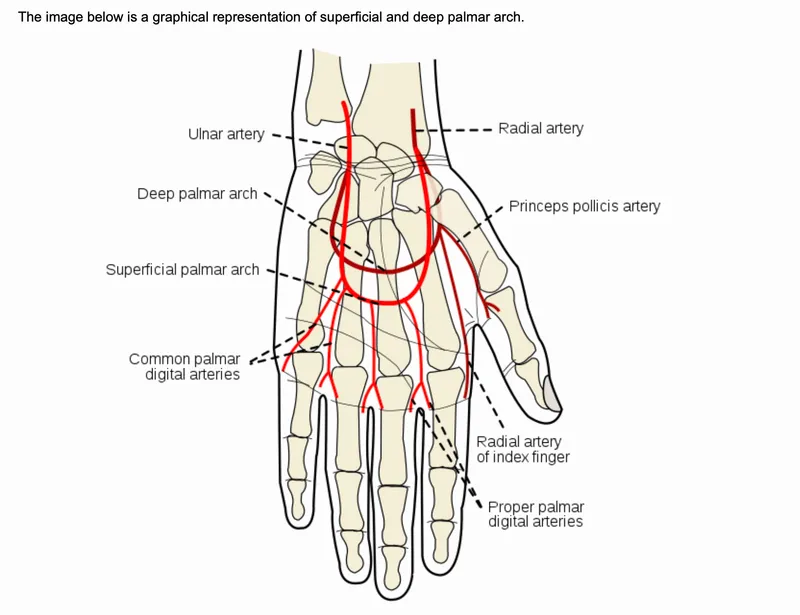
Superficial Palmar Arch: The Digital Arterial Source
The superficial palmar arch lies immediately deep to palmar aponeurosis and superficial to flexor tendons, lumbricals, and digital nerves. Formed by the terminal continuation of the ulnar artery in >95% of cases, it provides the dominant blood supply to the fingers via common and proper palmar digital arteries.
Superficial Arch Formation Variants:
- Complete arch (30-40% of individuals):
- Ulnar artery anastomoses with superficial palmar branch of radial
- Forms continuous vascular loop across palm
- Provides optimal collateral flow between radial and ulnar systems
- Maintains >90% of digital perfusion with single vessel occlusion
- Incomplete arch (60-70% of individuals):
- Ulnar artery terminates without anastomosing with radial contribution
- Common digital arteries arise from ulnar terminal branches
- Collateral flow between radial and ulnar systems occurs via deep arch and palmar metacarpal connections
- Maintains 70-85% of digital perfusion with single vessel occlusion
- Median artery contribution (10-15% of individuals):
- Persistent median artery (from anterior interosseous) contributes to arch
- May provide dominant supply to index and middle fingers
- Recognized by artery accompanying median nerve into palm
Superficial Arch Branches:
- Common palmar digital arteries (three vessels):
- Arise from convexity of arch
- Travel distally in 2nd, 3rd, 4th web spaces
- Divide at web space into proper palmar digital arteries (two per finger)
- Supply medial three web spaces (eight digital vessels total)
- Diameter 1-1.5 mm (common), 0.7-1 mm (proper)
- Proper palmar digital artery to ulnar side of little finger:
- Arises directly from ulnar artery (not from common digital)
- Supplies medial aspect of little finger
- Diameter 0.7-1 mm
- Anastomoses with palmar metacarpal arteries (from deep arch):
- Connect at level of web spaces
- Provide collateral flow between superficial and deep arches
- Critical for maintaining digital perfusion when one arch is compromised
- Diameter 0.3-0.5 mm
📌 Remember: The superficial arch supplies "3.5 fingers": complete supply to little, ring, middle fingers and medial half of index finger. The radial side of index finger and entire thumb receive supply from deep arch via princeps pollicis and radialis indicis branches.
Deep Palmar Arch: The Metacarpal Arterial Network
The deep palmar arch lies deep to flexor tendons, on interosseous muscles and metacarpal bases, approximately 1 cm proximal to superficial arch. Formed by the terminal continuation of the radial artery in >95% of cases, it provides primary blood supply to the thumb and contributes to digital perfusion via palmar metacarpal arteries.
Deep Arch Formation:
- Complete arch (>95% of individuals):
- Radial artery (after piercing first dorsal interosseous) anastomoses with deep branch of ulnar artery
- Forms continuous vascular loop at level of metacarpal bases
- Provides collateral flow to both radial and ulnar territories
- Incomplete arch (<5% of individuals):
- Radial artery terminates without anastomosing with ulnar deep branch
- Palmar metacarpal arteries still arise but collateral capacity reduced
- Increases risk of digital ischemia with radial artery injury
Deep Arch Branches:
- Princeps pollicis artery:
- Ar Complete the truncated "Deep Arch Branches" section by finishing the princeps pollicis artery description and adding the remaining branch descriptions:
Deep Arch Branches:
-
Princeps pollicis artery:
- Arises from radial artery as it enters palm
- Descends along medial border of first metacarpal
- Divides into two proper palmar digital arteries for thumb
- Supplies both sides of thumb (ulnar and radial aspects)
- Diameter 1-1.5 mm (main trunk), 0.8-1 mm (digital branches)
- Critical vessel for thumb perfusion and replantation
-
Radialis indicis artery:
- Arises from radial artery or princeps pollicis
- Supplies radial side of index finger
- Travels along radial border of second metacarpal
- Diameter 0.8-1 mm
- May arise as common trunk with princeps pollicis (40% of cases)
-
Palmar metacarpal arteries (three vessels):
- Arise from convexity of deep arch
- Descend in 2nd, 3rd, 4th interosseous spaces
- Anastomose with common digital arteries from superficial arch
- Provide collateral circulation between deep and superficial systems
- Diameter 0.5-0.8 mm
- Critical for digital salvage when superficial arch is compromised
-
Recurrent branches:
- Supply carpal joints and ligaments
- Anastomose with posterior interosseous and anterior interosseous arteries
- Contribute to wrist collateral circulation
Clinical Applications: Allen's Test and Vascular Assessment
The dual-arch architecture enables reliable clinical assessment of hand perfusion through Allen's test and guides surgical decision-making in trauma and reconstructive procedures.
Allen's Test Protocol:
- Compress both radial and ulnar arteries at wrist level
- Patient makes tight fist for 30 seconds to exsanguinate hand
- Release ulnar artery compression while maintaining radial compression
- Normal result: Palm flushes pink within 5-7 seconds (complete superficial arch)
- Abnormal result: Delayed flushing >10 seconds (incomplete arch or ulnar insufficiency)
- Repeat test releasing radial artery to assess deep arch contribution
Surgical Relevance:
- Radial artery harvesting for cardiac bypass: Allen's test ensures adequate ulnar collateral flow
- Digital replantation: Single arterial anastomosis succeeds due to arch redundancy
- Carpal tunnel surgery: Superficial arch lies 2-3mm distal to transverse carpal ligament
- Trauma management: Understanding arch anatomy predicts digital viability
Continue reading on Oncourse
Sign up for free to access the full lesson, plus unlimited questions, flashcards, AI-powered notes, and more.
CONTINUE READING — FREEor get the app
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Practice Questions: Upper Limb
Test your understanding with these related questions
Interosseous membrane of forearm is pierced by?



