Urinary Bladder & Urethra - Bladder & Urethra Blueprint
- Urinary Bladder:
- Hollow muscular organ; urothelium.
- Parts: Apex, body, fundus, neck. Trigone: smooth.
- Detrusor: Smooth muscle for micturition.
- Capacity: 400-600 mL. Urge: 150-200 mL.
- Innervation:
- Parasympathetic (S2-S4): Micturition (contracts detrusor).
- Sympathetic (T11-L2): Storage (relaxes detrusor).
- Somatic (Pudendal n.): External sphincter (voluntary).
- Arteries: Sup. & Inf. vesical aa. (internal iliac a.).

- Urethra:
- Male Urethra (~20 cm):
- Parts: Pre-prostatic, Prostatic (widest), Membranous (narrowest, ext. sphincter), Spongy (longest). (PPMMS)
- 📌 Mnemonic: "Prostitutes Prefer Making Money Standing".
- Female Urethra (~4 cm):
- Shorter, anterior to vagina; ↑UTI risk.
- Skene's glands (prostate homologue).
⭐ The membranous urethra in males is the narrowest and least distensible part, most prone to rupture during instrumentation.
- Male Urethra (~20 cm):
Male Urogenital Organs - Gents' Gear & Ducts
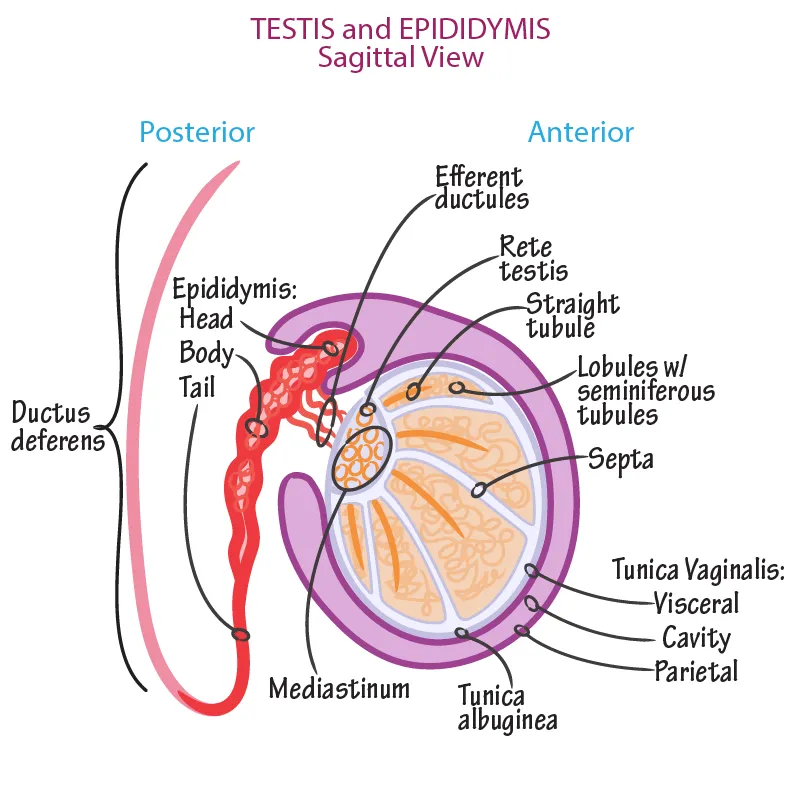
- Testes & Epididymis
- Testes: Paired oval glands in scrotum; produce sperm & testosterone. Tunica albuginea (fibrous capsule), septa divide into lobules containing seminiferous tubules.
- Epididymis: Coiled tube on posterior testis; sperm maturation & storage. Head, body, tail (continuous with ductus deferens).
- Blood Supply: Testicular artery (from aorta).
- Innervation: Testicular plexus.
- Ductus (Vas) Deferens
- Muscular tube; transports sperm from epididymis to ejaculatory duct.
- Part of spermatic cord.
- Seminal Vesicles
- Paired glands posterior to bladder; produce ~70% of seminal fluid (alkaline, fructose-rich).
- Duct joins ductus deferens to form ejaculatory duct.
- Ejaculatory Ducts
- Formed by union of ductus deferens & seminal vesicle duct; pass through prostate to empty into prostatic urethra.
- Prostate Gland
- Walnut-sized gland inferior to bladder, surrounds prostatic urethra.
- Produces ~25% of seminal fluid (milky, slightly acidic, contains PSA).
- Zones: Peripheral (common site of cancer), central, transitional (BPH).
⭐ Clinical Pearl: The neurovascular bundles supplying the penis run posterolaterally to the prostate; crucial to preserve during prostatectomy to maintain erectile function.
- Bulbourethral (Cowper's) Glands
- Pea-sized, posterolateral to membranous urethra; secrete pre-ejaculate (lubrication).
- Penis & Urethra
- Penis: Corpora cavernosa (2, dorsal), corpus spongiosum (1, ventral, contains urethra).
- Urethra: Prostatic, membranous, spongy (penile).
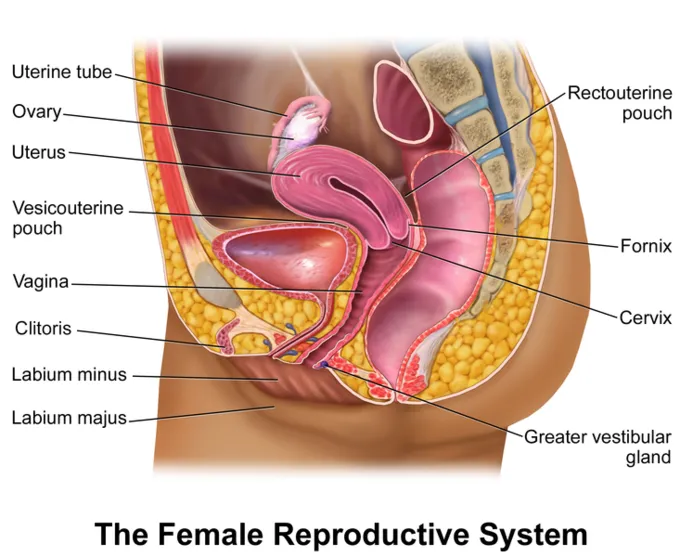
Female Urogenital Organs - Ladies' Layout & Lifeline
- Ovaries: Paired, in ovarian fossa.
- Function: Oogenesis, hormone production (estrogen, progesterone).
- Ligaments: Suspensory (vessels), Ovarian.
- Blood: Ovarian a. (aorta); R vein to IVC, L vein to L renal v.
- Uterine Tubes (Fallopian): ~10 cm.
- Parts: Infundibulum (fimbriae), Ampulla (fertilization), Isthmus, Intramural.
- Uterus: Pear-shaped.
- Parts: Fundus, Body, Cervix. Layers: Peri-, Myo-, Endometrium (cyclic changes).
- Position: Anteverted, anteflexed.
- Supports: Broad lig., Round lig., Cardinal lig. (primary), Uterosacral lig.
- Blood: Uterine a. (internal iliac a.).
⭐ Uterine artery crosses superior to ureter. 📌 "Water (ureter) under the bridge (uterine a.)".
- Vagina: Fibromuscular tube (~8-10 cm); cervix to vestibule. Fornices.
- Vulva: Mons pubis, Labia majora/minora, Clitoris, Vestibule (urethral/vaginal orifices, Bartholin's glands).
- Urethra: Short (~4 cm); opens in vestibule; prone to UTIs.
High‑Yield Points - ⚡ Biggest Takeaways
- Ureter is inferior to uterine artery ("water under bridge") near lateral vaginal fornix.
- Pudendal nerve (S2-S4): main motor/sensory supply to perineum.
- Membranous urethra: shortest, narrowest, least dilatable; prone to rupture.
- Micturition: parasympathetic (S2-S4) stimulates detrusor. Storage: sympathetic (T11-L2).
- Cardinal ligament: strongest support for uterus/cervix.
- Testicular/Ovarian arteries: arise from abdominal aorta (L2).
- Prostatic venous plexus drains to vertebral plexus (Batson's): metastasis route.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

