Pelvic Nodal Stations - Lymphatic Landmarks
- External Iliac Nodes:
- Lie along the external iliac artery & vein.
- Subgroups: Lateral, medial (intermediate), and anterior (medial lacunar).
- Internal Iliac (Hypogastric) Nodes:
- Cluster around the internal iliac artery & vein, and origins of their branches.
- Drain: Most pelvic viscera, deep perineum, gluteal muscles, posterior thigh.
- Common Iliac Nodes:
- Positioned along the common iliac vessels, up to the aortic bifurcation.
- Receive lymph from: External & internal iliac nodes, some pelvic viscera directly.
- Sacral Nodes:
- Located in the sacral concavity, anterior to the sacrum, near median sacral vessels.
- Drain: Posterior pelvic wall, rectum, prostate, cervix, body of uterus.
- Obturator Node(s):
- Found in the obturator fossa, typically near the obturator nerve & vessels.
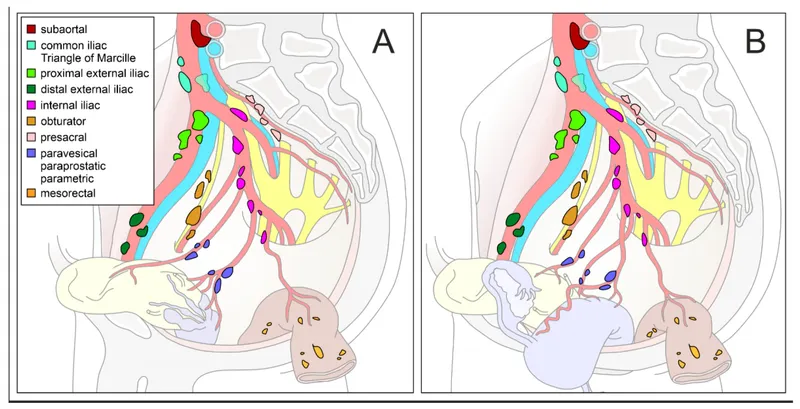
⭐ The obturator node is a crucial sentinel lymph node; its involvement is common in metastases from cancers of the cervix, prostate, bladder, and endometrium. It is often the first pelvic node involved in vulvar/vaginal cancer spreading from inguinal nodes via Cloquet's node pathway (though Cloquet's itself is inguinal).
Organ Drainage Maps - Follow the Flow
Pelvic lymph drainage generally mirrors arterial supply routes. Mapping organ-to-node pathways is crucial for oncology (staging, metastasis).
- Gonads (Ovaries/Testes): Directly to Para-aortic (lumbar) nodes.
⭐ Testicular and ovarian tumors primarily spread to para-aortic nodes, bypassing pelvic nodes initially.
- Upper Pelvic Structures:
- Uterine Fundus/Body (superior), Fallopian Tubes: Para-aortic nodes, some to External iliac nodes.
- Bladder (superior/lateral aspects): External iliac nodes.
- Rectum (proximal/upper): Via Inferior Mesenteric Artery pathway to Para-aortic nodes.
- Mid/Lower Pelvic Structures:
- Cervix, Upper ⅔ Vagina, Prostate, Bladder (base/neck/trigone), Uterus (lower), Mid-Rectum: Primarily Internal iliac nodes (including obturator, presacral, pararectal), some to External iliac & Sacral nodes.
- External Genitalia & Distal Tracts (below Pectinate Line):
- Vulva, Lower ⅓ Vagina, Anal Canal (distal), Perineal skin, Scrotum: Superficial inguinal nodes.
- Glans Penis/Clitoris: May drain to Deep inguinal (Cloquet's node) & External iliac nodes.

Clinical Crossroads - Cancer & Complications
- Metastatic Spread: Key pelvic cancer pathways:
- Cervical: Parametrial → Obturator, Ext/Int Iliac → Common Iliac → Para-aortic.
- Prostate: Obturator → Int Iliac → Presacral → Ext Iliac.
- Bladder: Obturator, Ext/Int Iliac.
- Rectal (upper 2/3): Sup. Rectal → Inf. Mesenteric.
- Rectal (lower 1/3): Int. Iliac; Inguinal (if below dentate line).
- Sentinel Node Biopsy (SLNB): Identifies first draining node(s) for staging; reduces surgical morbidity.
- Lymphedema: Common complication post-lymphadenectomy or radiotherapy; causes chronic limb swelling.

⭐ Virchow's node (left supraclavicular) involvement can indicate metastasis from pelvic/abdominal cancers (e.g., gastric, testicular, ovarian, prostate).
High‑Yield Points - ⚡ Biggest Takeaways
- Internal iliac nodes: Drain most pelvic viscera (bladder, prostate, uterus, vagina, rectum).
- External iliac nodes: Drain anterior pelvis, superior bladder, uterine fundus (via round ligament).
- Para-aortic nodes: Receive direct drainage from gonads (ovaries/testes) and common iliacs.
- Superficial inguinal nodes: Drain perineum, lower vagina, lower anal canal, external genitalia.
- Cloquet's node: Highest deep inguinal node, sentinel for penis/clitoris cancer.
- Common iliac nodes: Collect from internal/external iliacs; drain to para-aortic nodes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

