Pelvic Overview - His vs. Hers Blueprint
- General Form: Male pelvis heavier, thicker, prominent bone markings. Female pelvis lighter, thinner, smoother.
- Pelvic Inlet (Brim): Male - heart-shaped, narrow. Female - oval/rounded, wider.
- Pelvic Outlet: Male - smaller. Female - larger, for childbirth.
- Subpubic Angle: Male - acute (< 70°). Female - obtuse (> 80°).
- Greater Sciatic Notch: Male - narrow, J-shaped. Female - wide, L-shaped.
- Sacrum: Male - longer, narrower, more curved. Female - shorter, wider, less curved.
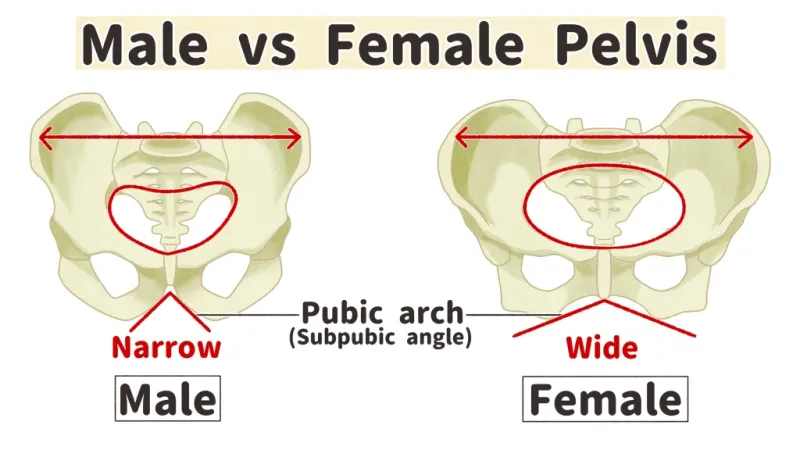
⭐ Pelvic dimorphism is primarily driven by the female's role in parturition, adapting for fetal passage during birth.
Bony Pelvis - Skeletal Showdown

| Feature | Male | Female |
|---|---|---|
| General Structure | Heavy, thick, prominent muscle markings | Light, thin, smooth |
| Pelvic Inlet | Heart-shaped, narrow | Oval/rounded, wider |
| Pelvic Outlet | Smaller | Larger |
| Subpubic Angle | Acute, <70° | Obtuse, >80-85° |
| Ischial Spines | Prominent, point inward | Everted, less prominent |
| Obturator Foramen | Round | Oval |
| Sacrum | Longer, narrower, more curved | Shorter, wider, less curved |
| Greater Sciatic Notch | Narrow, J-shaped | Wider, L-shaped (almost 90°) |
- Subpubic Angle: Men <70° (acute); Women >80-85° (obtuse).
- Greater Sciatic Notch: Male J-shape; Female L-shape.
⭐ The subpubic angle (acute in males, typically <70°; obtuse in females, typically >80°) is a cardinal sign for differentiating male and female pelves.
Pelvic Soft Parts - Gendered Guts & Guards
- Pelvic Diaphragm (Levator Ani & Coccygeus):
- Female: Broader, shallower basin; larger urogenital hiatus (for vagina) → ↑risk of weakness/prolapse.
- Male: Narrower, deeper funnel.
- Urogenital Diaphragm (UGD) / Perineal Membrane:
- Female: Pierced by urethra & vagina.
- Male: More developed; pierced by urethra.
- Perineal Body:
- Female: Larger, more critical for pelvic floor integrity, especially post-childbirth.
- Male: Smaller.
- Pelvic Viscera Positioning:
- Common: Bladder (anterior), Rectum (posterior).
- Female: Uterus, ovaries, vagina (between bladder & rectum).
- Male: Prostate, seminal vesicles (inferior/posterior to bladder).
- Distinctive Ligaments:
- Female: Broad, Round, Ovarian, Cardinal, Uterosacral (uterine & ovarian support).
- Male: Puboprostatic ligaments.

⭐ The female urogenital hiatus is significantly larger to accommodate the vagina, making the female pelvic floor more susceptible to weakness and prolapse.
Clinical Significance - Pelvic Puzzles in Practice
- Obstetric Significance:
- Pelvic Types & Labor Implications:
- Gynecoid: Round/oval inlet, wide subpubic angle. Most common, ideal for birth.
- Android: Heart-shaped inlet, narrow subpubic angle. ↑Instrumental delivery/C-section.
- Anthropoid: AP oval inlet, narrow subpubic angle. Favors Occipito-Posterior delivery.
- Platypelloid: Transverse oval, flat. ↑Arrest, C-section often needed.
- Pelvimetry: Obstetric conjugate ≈ 11 cm; Diagonal conjugate ≈ 12.5 cm (clinical estimate).
- Mechanism of Labor: Pelvic architecture critically influences fetal passage.
- Pelvic Types & Labor Implications:
- Surgical Implications:
- Nerve Injury Risk: Pudendal, obturator, sciatic nerves vulnerable during pelvic surgery.
- Surgical Access: Approaches differ for male (e.g., prostate) vs. female (e.g., uterus) organs.
- Urological & Gynecological Conditions:
- Female: Anatomical factors contribute to ↑Stress Urinary Incontinence (SUI) & Pelvic Organ Prolapse (POP) risk.
- Male: Benign Prostatic Hyperplasia (BPH) commonly affects bladder outlet function.
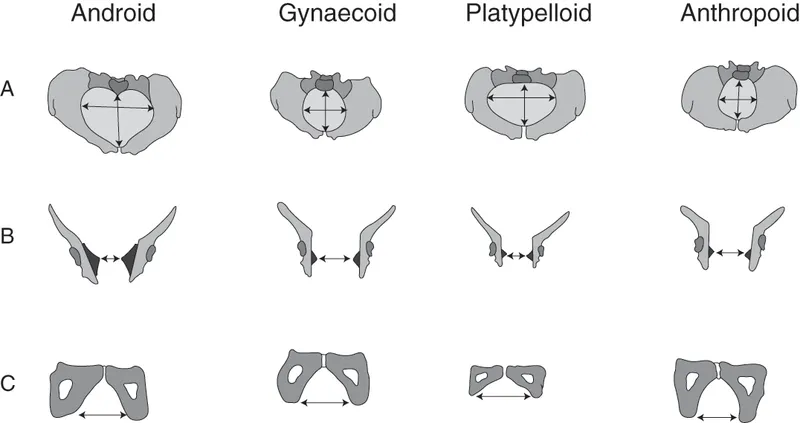
⭐ The Gynecoid pelvis, with its round to transverse oval inlet and wide subpubic angle, is the most common female pelvic type and is considered ideal for vaginal childbirth.
High‑Yield Points - ⚡ Biggest Takeaways
- Female pelvis: Lighter, wider, shallower for parturition; Male pelvis: Heavier, thicker, more marked bone features.
- Pelvic inlet: Female - transversely oval or rounded, spacious; Male - heart-shaped, narrower.
- Subpubic angle: Female - wide and rounded (>80°-85°); Male - narrow and acute (<70°).
- Greater sciatic notch: Female - wide (almost 90°); Male - narrow (~70°), J-shaped.
- Sacrum: Female - shorter, wider, less curved anteriorly; Male - longer, narrower, more uniformly curved.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

