Thyroid Anatomy - Neck's Butterfly
- Location: Anterior neck, C5-T1 vertebrae.
- Structure:
- Two lateral lobes, central isthmus.
- Pyramidal lobe (~50%): superior extension from isthmus.
- Capsules:
- True: Inner, fibrous, adherent.
- False: Outer, pretracheal fascia.
- Key Relations:
- Anterior: Strap muscles (sternohyoid, sternothyroid).
- Medial: Larynx, trachea, esophagus, recurrent laryngeal nerve (RLN).
- Posterolateral: Carotid sheath (CCA, IJV, Vagus n.), parathyroids.
- Berry's Ligament: Thickened pretracheal fascia; tethers thyroid to cricoid & upper tracheal rings.
⭐ Berry's ligament tethers the thyroid gland to the trachea, making it move with swallowing.

Thyroid Lifelines - Blood & Nerves
- Arterial Supply:
- Superior thyroid a. (from ECA)
- Inferior thyroid a. (from thyrocervical trunk)
- Thyroidea ima a. (variable origin, ~3-10%)
- Venous Drainage:
- Superior & Middle thyroid vv. → IJV
- Inferior thyroid vv. → Brachiocephalic vv.
- Lymphatics: Prelaryngeal, pretracheal, paratracheal → deep cervical nodes.
- Nerve Supply:
- Sympathetic: Cervical ganglia (vasomotor).
- Parasympathetic (Vagus): Fibers with arteries; RLN & SLN vulnerable in surgery.

⭐ The superior thyroid artery is typically the first branch of the external carotid artery.
Thyroid Genesis - Cells & Origins
- Embryology:
- Origin: Median endodermal thickening (primitive pharynx floor), 1st/2nd pharyngeal arches junction → Foramen cecum (tongue base).
- Descent: Migrates inferiorly, anterior to hyoid bone & laryngeal cartilages.
- Thyroglossal Duct: Epithelial tract of descent; usually obliterates.
- Remnants: Pyramidal lobe (superior to isthmus), thyroglossal duct cysts (midline neck swelling).
- Ectopic Thyroid: Lingual (most common), sublingual, prelaryngeal.
- Histology:
- Follicular cells (cuboidal): Synthesize $T_3$/$T_4$; form follicles containing colloid (storage).
- Parafollicular (C) cells: Neural crest origin; secrete calcitonin (↓ serum $Ca^{2+}$).
⭐ The thyroid gland originates from the foramen cecum at the base of the tongue.
Parathyroids - Calcium's Captains
- Number: Usually 4 (range 2-6).
- Location: Posterior thyroid lobes, within capsule/sheath. Superior more constant; inferior variable.
- Size/Appearance: 3-6 mm, ovoid, yellowish-brown.
- Arterial Supply: Mainly inferior thyroid arteries.
- Venous/Lymphatic Drainage: Follows thyroid vessels/nodes.
- Embryology: 📌 "3rd for Inferior, 4th for Superior"
- Superior: 4th pharyngeal pouch.
- Inferior: 3rd pharyngeal pouch (descends with thymus).
- Histology: Chief cells (PTH); Oxyphil cells (older, function unclear).

⭐ Inferior parathyroid glands (from 3rd pharyngeal pouch) are more variable in location due to descent with the thymus.
Clinical Hotspots - Glandular Dangers
- Recurrent Laryngeal Nerve (RLN): In tracheoesophageal groove; near Berry's ligament. Variable relation to inferior thyroid artery. Injury: unilateral → hoarseness; bilateral → stridor/aphonia.
- External Branch of Superior Laryngeal Nerve (EBSLN): Near superior pole, innervates cricothyroid. Injury → voice fatigue, ↓pitch, cannot hit high notes.
- Thyroglossal Duct Cyst: Midline neck swelling, moves with tongue protrusion.
- Ectopic Thyroid: Lingual (common), sublingual. Substernal goiter.
- Surgery: Preserve parathyroids (blood supply) to prevent hypoparathyroidism. Identify RLN.
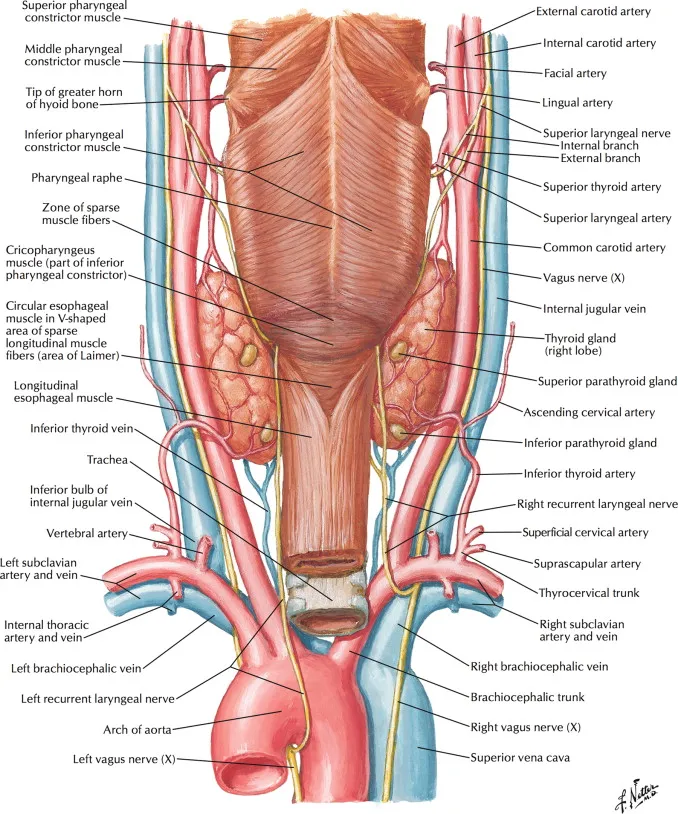
⭐ The recurrent laryngeal nerve is most commonly found in the tracheoesophageal groove; its relationship to the inferior thyroid artery is highly variable.
High-Yield Points - ⚡ Biggest Takeaways
- Thyroid develops from the foramen cecum, descending via the thyroglossal duct.
- Key arterial supply: Superior thyroid artery (from ECA) and Inferior thyroid artery (from thyrocervical trunk).
- Critical nerve relations: External laryngeal nerve near superior thyroid artery; Recurrent laryngeal nerve near inferior thyroid artery.
- Typically four parathyroid glands are posterior to the thyroid; inferior glands (from 3rd pharyngeal pouch) show variable positions.
- Inferior thyroid arteries are the primary blood supply to all parathyroid glands.
- Thyroid parafollicular (C) cells produce calcitonin; Parathyroid chief cells secrete PTH.
- Berry's ligament attaches the thyroid to the trachea, causing it to move with swallowing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

