Neck

On this page
🏗️ Neck Architecture: The Cervical Command Center
The neck is a densely packed corridor where millimeters matter-arteries supplying the brain, nerves controlling speech and swallowing, and lymph nodes signaling disease all navigate through precisely defined triangular zones bounded by muscle and fascia. You'll master the architectural logic that organizes this complex region, trace vascular and neural pathways that make the neck a clinical crossroads, and learn how anatomical relationships predict where infections spread, tumors metastasize, and surgical planes open safely. This knowledge transforms the neck from an intimidating tangle into a readable map that guides diagnosis and intervention.
The cervical region extends from the mandible superiorly to the thoracic inlet inferiorly, bounded by the trapezius posteriorly and midline anteriorly. This 360-degree cylindrical space houses the body's most critical transit routes: the carotid arteries delivering 750ml/min to the brain, the jugular veins returning 85% of cerebral venous blood, and the vagus nerves controlling 75% of parasympathetic function.
📌 Remember: SCALP for neck boundaries - Superior (mandible), Caudal (thoracic inlet), Anterior (midline), Lateral (SCM), Posterior (trapezius)
Cervical Vertebral Framework
The 7 cervical vertebrae form the neck's structural backbone, with C1-C2 providing 50% of total cervical rotation and C5-C6 being the most mobile segment. The cervical lordosis maintains a 20-40 degree anterior curve, distributing 4.5-5.4kg of head weight across the vertebral column.
- Atlas (C1): Ring-shaped vertebra with no body, supporting 100% of cranial weight
- Lateral masses articulate with occipital condyles
- Transverse ligament prevents atlantoaxial dislocation
- Vertebral arteries pass through transverse foramina
- Axis (C2): Features the odontoid process (dens) projecting superiorly
- Dens acts as pivot point for 50% of cervical rotation
- Fracture risk highest at base of dens in elderly patients
- Type II dens fractures have 15-20% nonunion rate
- C3-C7: Typical cervical vertebrae with bifid spinous processes
- Uncovertebral joints develop after age 10 years
- C5-C6 level accounts for 60% of cervical disc herniations
- C6-C7 most common level for degenerative changes
⭐ Clinical Pearl: C5-C6 disc herniation presents with C6 radiculopathy (thumb and index finger numbness), while C6-C7 herniation causes C7 radiculopathy (middle finger numbness and triceps weakness)
| Vertebral Level | Key Features | Clinical Significance | Injury Pattern | Mobility % |
|---|---|---|---|---|
| C1 (Atlas) | No body, lateral masses | Occipital neuralgia, vertebral artery injury | Jefferson fracture | 25% flexion/extension |
| C2 (Axis) | Odontoid process | Hangman's fracture, atlantoaxial instability | Dens fracture | 50% rotation |
| C3-C4 | Hyoid level | Epiglottitis, thyroid surgery landmark | Hyperextension injury | 15% total motion |
| C5-C6 | Most mobile | Disc herniation, radiculopathy | Whiplash, facet dislocation | 60% disc disease |
| C7 | Vertebra prominens | Thoracic outlet, lower trunk plexus | Swimmer's shoulder | Transition zone |
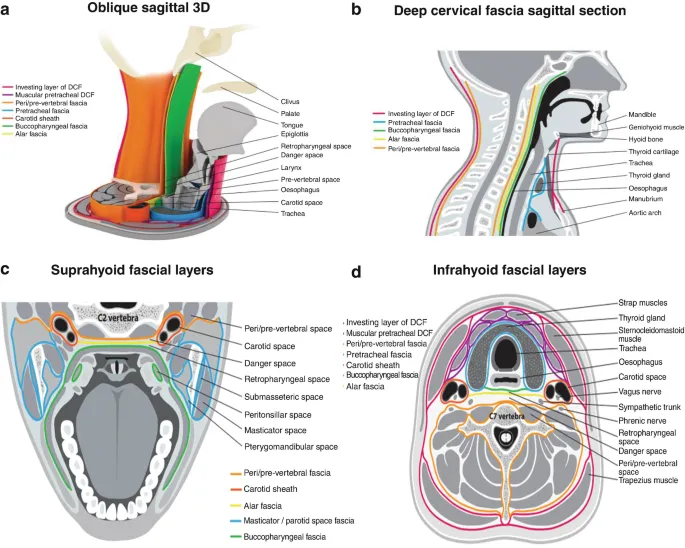
The deep cervical fascia creates 4 distinct layers that compartmentalize neck structures and direct infection spread patterns. Understanding fascial planes predicts 90% of deep neck infection pathways and surgical approach strategies.
- Investing Layer: Outermost fascial envelope
- Encircles entire neck like a collar
- Splits to enclose SCM and trapezius muscles
- Forms roof of anterior and posterior triangles
- Infection here spreads circumferentially around neck
- Pretracheal Layer: Surrounds anterior visceral structures
- Encloses thyroid, trachea, esophagus
- Extends from hyoid to superior mediastinum
- Thyroid infections spread along this plane to mediastinum
- Forms false capsule around thyroid gland
- Prevertebral Layer: Covers posterior neck structures
- Extends from skull base to T3 vertebra
- Encloses vertebrae, paraspinal muscles
- Retropharyngeal space lies anterior to this layer
- Danger space allows infection spread to posterior mediastinum
💡 Master This: Retropharyngeal space infections can descend to the posterior mediastinum within 6-12 hours, making early recognition and drainage critical for preventing necrotizing mediastinitis with 40% mortality
📌 Remember: IPPC for fascial layers - Investing (outermost), Pretracheal (visceral), Prevertebral (deepest), Carotid sheath (neurovascular)
The carotid sheath forms a specialized fascial tube containing the carotid artery, internal jugular vein, and vagus nerve. This neurovascular bundle travels from the skull base to the thoracic inlet, with the vagus nerve positioned posteriorly between the vessels.
Understanding neck architecture transforms complex clinical presentations into predictable anatomical patterns. The cervical region's compartmentalized organization explains why thyroid masses move with swallowing, why carotid bruits radiate to specific locations, and why deep neck infections follow characteristic spread patterns. Connect this structural foundation through triangular organization to understand the neck's functional territories.
🏗️ Neck Architecture: The Cervical Command Center
🗺️ Triangular Territories: The Neck's Geographic Zones
Anterior Triangle: The Vital Front Zone
The anterior triangle contains the neck's most critical visceral structures, bounded by the mandible superiorly, SCM laterally, and midline medially. This high-stakes real estate houses 80% of neck pathology and 90% of surgical emergencies.
- Submandibular Triangle: Bounded by mandible and digastric muscle
- Contains submandibular gland and facial artery
- Ludwig's angina spreads through this space
- Wharton's duct courses 2-3cm medial to gland
- Lingual nerve provides parasympathetic innervation
- Submental Triangle: Between anterior bellies of digastric muscles
- Contains submental lymph nodes draining chin and lower lip
- Floor of mouth infections present here
- Mylohyoid muscle forms the floor
- Ranula may extend into this space
- Carotid Triangle: Most clinically significant subdivision
- Bounded by SCM, omohyoid, digastric muscles
- Contains carotid bifurcation at C3-C4 level
- Carotid body chemoreceptors located at bifurcation
- Hypoglossal nerve crosses superficially
⭐ Clinical Pearl: Carotid massage at the bifurcation can terminate SVT in 80% of cases, but carries 0.5% risk of stroke in patients over 65 years with carotid disease
| Triangle | Key Contents | Clinical Pathology | Surgical Access | Danger Zones |
|---|---|---|---|---|
| Submandibular | Submandibular gland, facial artery | Ludwig's angina, sialolithiasis | Transcervical approach | Marginal mandibular nerve |
| Submental | Submental nodes, anterior jugular | Floor of mouth cellulitis | Submental incision | Airway compromise |
| Carotid | Carotid bifurcation, vagus nerve | Carotid stenosis, paraganglioma | Standard neck dissection | Hypoglossal nerve |
| Muscular | Thyroid, parathyroids, trachea | Thyroid cancer, hyperparathyroidism | Collar incision | Recurrent laryngeal nerve |
The posterior triangle serves as the neck's neural and vascular superhighway, bounded by SCM anteriorly, trapezius posteriorly, and clavicle inferiorly. This anatomical corridor contains the brachial plexus, subclavian vessels, and accessory nerve.
- Occipital Triangle: Superior portion above omohyoid muscle
- Contains accessory nerve crossing at Erb's point
- Cervical plexus emerges along SCM posterior border
- Levator scapulae and splenius capitis form floor
- Lymph node levels II, III, and V located here
- Supraclavicular Triangle: Inferior portion below omohyoid
- Contains subclavian artery and brachial plexus trunks
- Phrenic nerve crosses anterior scalene muscle
- Thoracic duct enters venous system at left venous angle
- Stellate ganglion lies deep to prevertebral fascia
💡 Master This: The accessory nerve lies superficially in the posterior triangle, making it vulnerable during lymph node biopsies. Injury causes trapezius paralysis with shoulder drop and inability to shrug against resistance
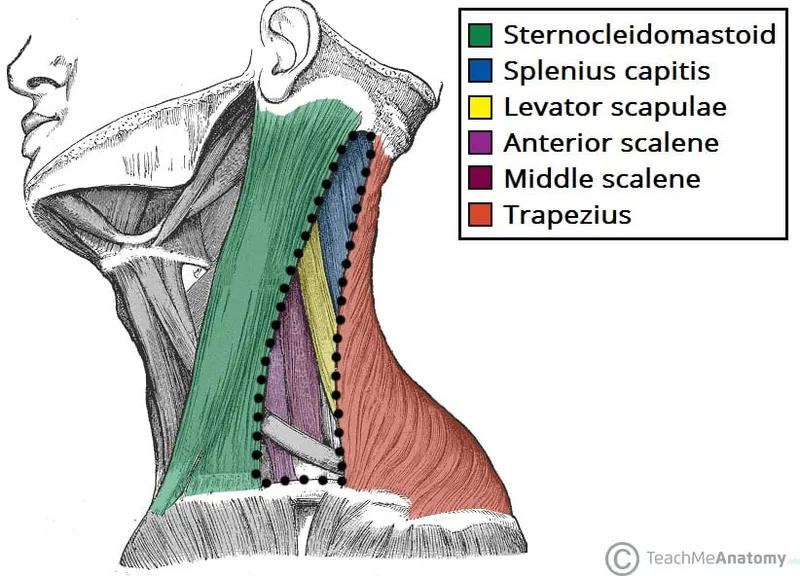
Scalene Triangle: The Thoracic Outlet Gateway
The scalene triangle represents a critical neurovascular bottleneck where the subclavian artery and brachial plexus pass between the anterior and middle scalene muscles. This anatomical chokepoint is the primary site of thoracic outlet syndrome.
- Boundaries: Anterior scalene, middle scalene, first rib
- Contents: Subclavian artery, brachial plexus trunks
- Clinical significance: Cervical ribs narrow this space in 0.5% of population
- Compression patterns: Neurogenic (95%) vs vascular (5%) symptoms
📌 Remember: SAM for scalene triangle contents - Subclavian artery, Anterior scalene (boundary), Middle scalene (boundary). The subclavian vein passes anterior to the anterior scalene, not through the triangle.
Clinical Navigation Principles
The triangular system provides anatomical coordinates for clinical localization. Anterior triangle masses suggest thyroid, lymph node, or salivary gland pathology, while posterior triangle masses indicate lymphadenopathy or neural tumors. Level-based lymph node classification follows triangular boundaries, with levels I-III in the anterior triangle and levels IV-V in the posterior triangle.
- Palpation sequence: Systematic examination follows triangular boundaries
- Imaging correlation: CT/MRI findings map to specific triangular zones
- Surgical planning: Incision placement respects triangular anatomy
- Complication prediction: Nerve injury patterns follow triangular distributions
Understanding triangular territories transforms neck examination from random palpation into systematic anatomical exploration. Each triangle contains predictable structures with characteristic pathology patterns, enabling rapid localization and targeted investigation. Connect this geographic framework through fascial organization to understand how infections spread and surgical planes develop.
🗺️ Triangular Territories: The Neck's Geographic Zones
🚗 Vascular Superhighways: The Neck's Circulatory Network
Arterial Supply Architecture
The neck receives arterial supply from 4 primary sources: bilateral common carotids and bilateral vertebral arteries, delivering 85% of cerebral blood flow and 100% of facial circulation.
- Common Carotid Arteries: Primary cerebral supply vessels
- Right CCA: Arises from brachiocephalic trunk
- Left CCA: Arises directly from aortic arch
- Bifurcation level: C3-C4 vertebral level (thyroid cartilage)
- Carotid sinus: Baroreceptor zone with vagal innervation
- Flow rate: 350ml/min per vessel (700ml/min total)
⭐ Clinical Pearl: Carotid stenosis >70% reduces ipsilateral cerebral perfusion by 40-60%, but Circle of Willis collaterals can maintain adequate flow in 60% of patients
Internal Carotid System: Brain's VIP Access
The internal carotid arteries provide anterior circulation to 80% of cerebral tissue, traveling through the carotid canal and cavernous sinus before forming the Circle of Willis.
- Cervical segment: No branches in the neck
- Travels posterolateral to external carotid
- Larger diameter than external carotid
- Carotid body at bifurcation monitors O2/CO2
- Atherosclerosis most common at bifurcation
- Petrous segment: Through temporal bone
- Caroticotympanic arteries to middle ear
- Vidian artery to nasal cavity
- Cavernous segment: Through cavernous sinus
- Ophthalmic artery origin
- Anterior choroidal artery to internal capsule
| ICA Segment | Anatomical Course | Branch Pattern | Clinical Significance | Pathology Risk |
|---|---|---|---|---|
| Cervical | Carotid sheath | No branches | Atherosclerosis, dissection | 70% stenosis threshold |
| Petrous | Carotid canal | Caroticotympanic | Temporal bone fracture | Hemorrhage risk |
| Cavernous | Cavernous sinus | Ophthalmic | Aneurysm formation | Mass effect |
| Supraclinoid | Subarachnoid space | ACA, MCA | Stroke territory | Embolic events |
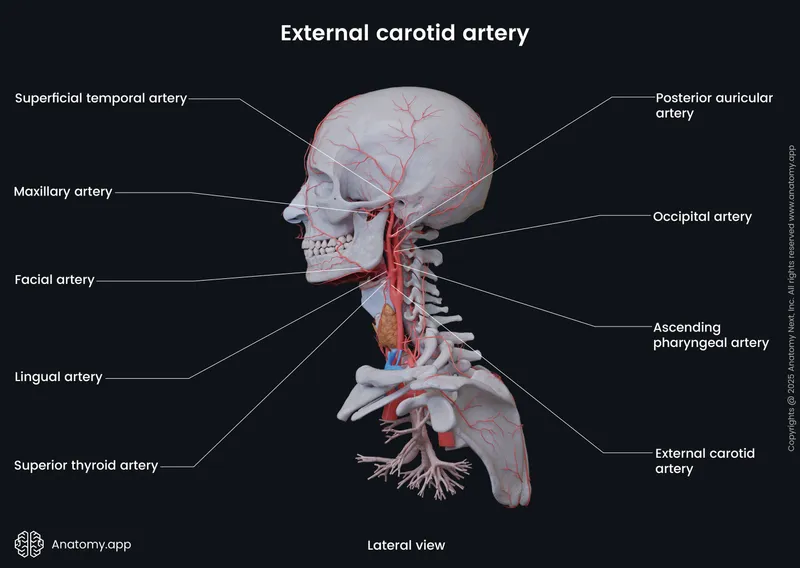
The external carotid artery provides comprehensive facial circulation through 8 major branches, supplying scalp, face, neck viscera, and oral cavity.
- Anterior branches: Superior thyroid, lingual, facial
- Superior thyroid: First branch, supplies thyroid gland
- Lingual: Supplies tongue via deep lingual artery
- Facial: Crosses mandible at anterior masseter
- Posterior branches: Occipital, posterior auricular
- Occipital: Supplies posterior scalp
- Posterior auricular: Supplies external ear
- Terminal branches: Maxillary, superficial temporal
- Maxillary: Deep facial circulation
- Superficial temporal: Temporal artery biopsy site
📌 Remember: SALFOP-MT for ECA branches - Superior thyroid, Ascending pharyngeal, Lingual, Facial, Occipital, Posterior auricular, Maxillary, Temporal
Vertebral Artery System: Posterior Circulation
The vertebral arteries provide posterior circulation to the brainstem, cerebellum, and posterior cerebrum, contributing 20% of total cerebral blood flow.
- V1 segment: Subclavian to C6 transverse foramen
- Most common atherosclerosis site
- Subclavian steal occurs with proximal stenosis
- V2 segment: Through C6-C2 transverse foramina
- Protected by bony canal
- Cervical spine manipulation risk zone
- V3 segment: C2 to foramen magnum
- Most mobile segment
- Dissection risk with neck rotation
- V4 segment: Intracranial to basilar artery
- PICA origin
- Lateral medullary syndrome territory
💡 Master This: Vertebral artery dissection accounts for 20% of strokes in patients <45 years, often triggered by neck manipulation or sudden rotation. V3 segment is most vulnerable due to atlantoaxial mobility
Venous Drainage Networks
The neck's venous system manages cerebral venous return through multiple parallel pathways, with the internal jugular veins handling 85% of brain drainage.
- Internal jugular veins: Primary cerebral drainage
- Flow rate: 400ml/min per vessel
- Valve-free system allows bidirectional flow
- Central line access point at cricothyroid level
- Thrombosis risk with central catheters
- External jugular veins: Superficial drainage
- Facial and scalp venous return
- Visible with Valsalva maneuver
- Compression indicates SVC obstruction
- Vertebral venous plexus: Deep cervical drainage
- Valve-free communication with intracranial veins
- Infection spread pathway to epidural space
- Metastasis route for prostate/breast cancer
The neck's vascular architecture creates predictable flow patterns and collateral pathways that determine clinical presentations. Carotid stenosis produces anterior circulation strokes, while vertebral disease causes posterior circulation symptoms. Venous obstruction patterns follow anatomical drainage territories, enabling rapid localization of vascular pathology. Connect this circulatory framework through neural networks to understand how blood supply supports nerve function.
🚗 Vascular Superhighways: The Neck's Circulatory Network
⚡ Neural Networks: The Neck's Electrical Grid
Cervical Plexus: The Regional Command Center
The cervical plexus forms from C1-C4 nerve roots, creating sensory and motor branches that innervate the neck, shoulder, and diaphragm. This neural network provides 100% of neck sensation and critical respiratory control.
- Sensory branches: 4 major cutaneous nerves
- Lesser occipital (C2): Posterior scalp sensation
- Great auricular (C2-C3): Ear and angle of mandible
- Transverse cervical (C2-C3): Anterior neck sensation
- Supraclavicular (C3-C4): Shoulder and upper chest
- Motor branches: Critical functional control
- Phrenic nerve (C3-C5): Diaphragm innervation
- Ansa cervicalis (C1-C3): Infrahyoid muscles
- Segmental branches: Deep neck muscles
⭐ Clinical Pearl: Phrenic nerve injury during cardiac surgery occurs in 5-10% of cases, causing hemidiaphragm paralysis with 25-30% reduction in vital capacity
Cranial Nerve Superhighway
8 cranial nerves traverse the neck, controlling swallowing, phonation, facial expression, and autonomic functions. These neural pathways create predictable deficit patterns when injured.
| Cranial Nerve | Neck Course | Function | Injury Pattern | Clinical Test |
|---|---|---|---|---|
| VII (Facial) | Stylomastoid foramen | Facial expression | Facial paralysis | Smile asymmetry |
| IX (Glossopharyngeal) | Jugular foramen | Swallowing, taste | Dysphagia | Gag reflex |
| X (Vagus) | Carotid sheath | Phonation, autonomic | Hoarseness | Voice quality |
| XI (Accessory) | Posterior triangle | Trapezius, SCM | Shoulder drop | Shrug strength |
| XII (Hypoglossal) | Submandibular triangle | Tongue movement | Tongue deviation | Protrusion test |
The vagus nerve represents the neck's most critical autonomic pathway, controlling 75% of parasympathetic function and 100% of laryngeal innervation.
- Superior laryngeal nerve: External and internal branches
- External branch: Cricothyroid muscle innervation
- Internal branch: Supraglottic sensation
- Injury: Voice pitch changes, aspiration risk
- Recurrent laryngeal nerve: Critical voice pathway
- Right RLN: Loops around subclavian artery
- Left RLN: Loops around aortic arch
- Innervates: All intrinsic laryngeal muscles except cricothyroid
- Injury rate: 1-2% in thyroid surgery
💡 Master This: Bilateral RLN injury causes vocal cord paralysis with airway obstruction requiring immediate tracheostomy. Unilateral injury causes hoarseness and aspiration risk but rarely requires surgical intervention
Sympathetic Chain: The Fight-or-Flight Network
The cervical sympathetic chain contains 3 ganglia that control pupillary function, facial sweating, and cardiovascular regulation.
- Superior cervical ganglion: C1-C4 level
- Pupillary dilation via long ciliary nerves
- Facial sweating control
- Müller's muscle innervation (eyelid elevation)
- Middle cervical ganglion: C6 level (often absent)
- Thyroid and cardiac innervation
- Variable anatomy in 50% of population
- Stellate ganglion: C7-T1 level
- Upper extremity sympathetic supply
- Cardiac acceleration pathways
- Stellate ganglion block treats CRPS
📌 Remember: Horner's syndrome triad - Ptosis, Miosis, Anhidrosis from sympathetic chain injury. Central (brainstem), preganglionic (spinal cord), or postganglionic (neck) lesions
Brachial Plexus: Upper Extremity Command
The brachial plexus originates from C5-T1 nerve roots, forming trunks, divisions, cords, and terminal branches that innervate the entire upper extremity.
- Nerve roots: C5-T1 exit through intervertebral foramina
- C5-C6: Upper trunk formation
- C7: Middle trunk (isolated)
- C8-T1: Lower trunk formation
- Erb's point: C5-C6 junction at SCM posterior border
- Most vulnerable to traction injury
- Erb's palsy: Waiter's tip deformity
- Obstetric injury in 0.5-2 per 1000 births
Clinical Integration Patterns
Neural network understanding enables rapid localization of neck pathology. Upper cervical lesions affect occipital sensation and neck movement, while lower cervical pathology impacts shoulder function and upper extremity sensation. Cranial nerve deficits follow predictable anatomical patterns, enabling targeted investigation and surgical planning.
- Systematic examination: Cranial nerves V, VII, IX-XII
- Functional testing: Swallowing, phonation, facial expression
- Sensory mapping: Cervical dermatomes C2-C4
- Motor assessment: Neck flexion, shoulder elevation
The neck's neural architecture creates integrated control systems that coordinate complex functions through parallel pathways. Injury patterns follow anatomical distributions, enabling precise localization and targeted treatment. Connect this neural framework through lymphatic drainage to understand how the neck's immune surveillance system protects these critical pathways.
⚡ Neural Networks: The Neck's Electrical Grid
🛡️ Lymphatic Surveillance: The Neck's Immune Highway System
Lymph Node Level Classification
The 6-level system organizes cervical lymph nodes into anatomically defined territories that correspond to predictable drainage patterns and surgical approaches.
- Level I: Submental and submandibular triangles
- Submental (IA): Between anterior digastric bellies
- Submandibular (IB): Submandibular triangle contents
- Primary drainage: Oral cavity, anterior tongue, floor of mouth
- Clinical significance: Oral cancer staging, Ludwig's angina
- Level II: Upper jugular chain (skull base to hyoid)
- IIA: Anterior to spinal accessory nerve
- IIB: Posterior to spinal accessory nerve
- Primary drainage: Oropharynx, nasopharynx, parotid
- Surgical risk: Spinal accessory nerve injury
⭐ Clinical Pearl: Level IIB lymph nodes are rarely involved in oral cavity cancers but commonly affected in oropharyngeal and nasopharyngeal malignancies, influencing surgical planning
| Level | Anatomical Boundaries | Primary Drainage | Malignancy Risk | Surgical Approach |
|---|---|---|---|---|
| I | Mandible to hyoid | Oral cavity, anterior tongue | 85% oral cavity mets | Supraomohyoid dissection |
| II | Skull base to hyoid | Oropharynx, nasopharynx | 70% oropharynx mets | Modified radical dissection |
| III | Hyoid to cricoid | Hypopharynx, larynx | 60% hypopharynx mets | Selective dissection |
| IV | Cricoid to clavicle | Hypopharynx, thyroid | 40% thyroid mets | Extended dissection |
| V | Posterior triangle | Nasopharynx, thyroid | 30% nasopharynx mets | Posterolateral approach |
| VI | Hyoid to innominate | Thyroid, trachea, esophagus | 90% thyroid mets | Central compartment |
Lymphatic drainage follows predictable anatomical pathways that determine metastatic spread patterns and surgical staging requirements.
- Oral cavity: Bilateral drainage to levels I-III
- Anterior tongue: Level I predominance
- Posterior tongue: Bilateral levels II-IV
- Floor of mouth: Level I with skip metastases to level III
- Oropharynx: Bilateral drainage to levels II-IV
- Tonsil: Ipsilateral levels II-III (85%)
- Base of tongue: Bilateral levels II-IV (60%)
- Soft palate: Bilateral levels II-III
- Larynx: Compartment-specific drainage
- Supraglottis: Bilateral levels II-IV (40% bilateral)
- Glottis: Minimal drainage (<5% nodal metastases)
- Subglottis: Levels III-VI with paratracheal involvement
Thyroid Lymphatic System
The thyroid gland has extensive lymphatic drainage through central and lateral compartments, with metastatic patterns determining surgical extent.
- Central compartment (Level VI): Primary drainage
- Pretracheal and paratracheal nodes
- Delphian node: Prelaryngeal sentinel node
- 90% of thyroid cancers involve central nodes
- Prophylactic dissection controversial for T1-T2 tumors
- Lateral compartment (Levels II-V): Secondary drainage
- Levels III-IV most commonly involved
- Level II involvement indicates advanced disease
- Skip metastases to level V in 15% of cases
- Bilateral involvement in 20% of cases
💡 Master This: Papillary thyroid cancer has microscopic nodal metastases in 80% of cases, but clinically apparent nodes in only 30%. Central compartment dissection improves staging accuracy but increases recurrent laryngeal nerve and parathyroid injury risk
Infection Spread Patterns
Lymphatic pathways direct infection spread through predictable routes that follow anatomical boundaries and fascial planes.
- Odontogenic infections: Level I progression
- Dental abscess → submandibular space
- Ludwig's angina: Bilateral submandibular involvement
- Airway compromise in 15-20% of cases
- Pharyngeal infections: Deep neck space involvement
- Retropharyngeal space: Levels II-III drainage
- Parapharyngeal space: Carotid sheath proximity
- Descending necrotizing fasciitis: 40% mortality
- Skin and soft tissue: Superficial lymphatic spread
- Cellulitis: Regional node enlargement
- Lymphangitis: Red streaking along lymphatic channels
- Systemic spread risk with immunocompromise
📌 Remember: SCALP for deep neck infection spaces - Submandibular, Carotid, Anterior visceral, Lateral pharyngeal, Prevertebral/retropharyngeal
Clinical Assessment Framework
Systematic lymph node examination follows anatomical levels with specific palpation techniques and imaging correlation.
- Palpation sequence: Levels I-VI systematic approach
- Bimanual examination for level I nodes
- SCM landmark for levels II-IV localization
- Posterior triangle assessment for level V
- Central compartment palpation for level VI
- Size criteria: >1cm in levels I-II, >1.5cm in levels III-V
- Consistency assessment: Hard, fixed nodes suggest malignancy
- Imaging correlation: CT/MRI for deep nodes and extracapsular extension
The neck's lymphatic architecture creates organized drainage territories that predict disease spread patterns and guide therapeutic decisions. Level-based classification enables precise communication between clinicians and standardized surgical approaches. Understanding drainage pathways transforms random node palpation into systematic anatomical assessment. Connect this immune surveillance framework through clinical integration to understand how neck pathology presents and progresses.
🛡️ Lymphatic Surveillance: The Neck's Immune Highway System
🎯 Clinical Integration: Mastering Neck Pathology Patterns
Systematic Clinical Assessment
Neck examination follows anatomical territories with specific techniques for each structural system, enabling comprehensive evaluation in <5 minutes.
- Inspection phase: Symmetry, masses, skin changes
- Thyroid enlargement: Moves with swallowing
- Lymphadenopathy: Fixed vs mobile characteristics
- Vascular prominence: JVD, carotid pulsations
- Skin changes: Scars, discoloration, lesions
- Palpation sequence: Systematic anatomical approach
- Thyroid: Bimanual technique with swallowing
- Lymph nodes: Level-by-level assessment
- Carotid pulses: Bilateral comparison, no simultaneous palpation
- Trachea: Midline position assessment
- Functional testing: Neural and muscular function
- Cranial nerves: VII, IX, X, XI, XII assessment
- Range of motion: Cervical spine mobility
- Swallowing: Coordination and aspiration risk
- Voice quality: Hoarseness, breathiness evaluation
⭐ Clinical Pearl: Thyroid nodules that are >4cm, fixed to surrounding structures, or associated with vocal cord paralysis have >80% malignancy risk and require immediate surgical evaluation
Pathology Localization Framework
Anatomical location predicts differential diagnosis with 85-90% accuracy, enabling targeted investigation and efficient workup.
| Location | Common Pathology | Key Features | Investigation Priority | Malignancy Risk |
|---|---|---|---|---|
| Level I | Submandibular gland pathology | Moves with tongue | Sialography, CT | 15% malignant |
| Level II | Metastatic lymphadenopathy | Hard, fixed | Primary site search | 70% malignant |
| Level VI | Thyroid pathology | Moves with swallowing | Ultrasound, FNA | 25% malignant |
| Posterior triangle | Neural tumors, lymphoma | Soft, mobile | MRI, biopsy | 40% malignant |
| Carotid space | Paraganglioma, schwannoma | Pulsatile, mobile | MRA, octreotide scan | 10% malignant |
Life-threatening neck pathology presents with predictable warning signs that demand immediate intervention within minutes to hours.
- Airway emergencies: Stridor, dyspnea, voice changes
- Ludwig's angina: Floor of mouth induration
- Epiglottitis: Muffled voice, drooling
- Retropharyngeal abscess: Neck extension, fever
- Bilateral vocal cord paralysis: Inspiratory stridor
- Vascular emergencies: Hemorrhage, ischemia
- Carotid blowout: Massive bleeding post-radiation
- Carotid dissection: Horner's syndrome, stroke
- Subclavian steal: Arm claudication, syncope
- Neurologic emergencies: Rapid deficit progression
- Cervical spine injury: Quadriplegia risk
- Epidural abscess: Progressive myelopathy
- Cavernous sinus thrombosis: Cranial nerve palsies
💡 Master This: Acute airway obstruction from deep neck infections can progress from mild symptoms to complete obstruction within 2-4 hours. Early intubation or surgical airway prevents catastrophic outcomes
Imaging Strategy Integration
Imaging selection follows anatomical considerations and clinical suspicion, optimizing diagnostic yield while minimizing cost and radiation exposure.
- Ultrasound: First-line for thyroid and superficial masses
- Real-time assessment with Doppler evaluation
- FNA guidance for tissue sampling
- Cost-effective screening tool
- Operator-dependent limitations
- CT with contrast: Comprehensive neck evaluation
- Deep space infection assessment
- Vascular anatomy and pathology
- Lymph node staging and extracapsular extension
- Radiation exposure consideration
- MRI: Soft tissue and neural pathology
- Superior contrast resolution
- Multiplanar imaging capability
- No radiation exposure
- Longer acquisition time and higher cost
Surgical Planning Principles
Anatomical relationships determine surgical approaches, complication risks, and functional outcomes across all neck procedures.
- Incision planning: Cosmetic and functional considerations
- Collar incisions: Thyroid and central compartment
- Utility incisions: Comprehensive neck access
- Skin tension lines: Optimal healing and cosmesis
- Neural preservation: Critical function protection
- Recurrent laryngeal nerve: Voice preservation
- Spinal accessory nerve: Shoulder function
- Marginal mandibular nerve: Facial symmetry
- Phrenic nerve: Respiratory function
- Vascular control: Hemorrhage prevention
- Carotid system: Stroke prevention
- Jugular system: Air embolism risk
- Thyroid vessels: Bleeding control
📌 Remember: NAILS for neck surgery complications - Nerve injury, Airway compromise, Infection, Lymphatic leak, Scar formation
Evidence-Based Management
Treatment decisions integrate anatomical knowledge with evidence-based protocols to optimize patient outcomes and minimize complications.
- Thyroid nodules: ATA guidelines for FNA and surgery
- >1cm nodules with suspicious features
- >1.5cm nodules with intermediate features
- >2cm nodules with benign features
- Lymphadenopathy: Size and character criteria
- >2cm nodes require tissue diagnosis
- Hard, fixed nodes suggest malignancy
- Persistent nodes >4 weeks need evaluation
- Deep neck infections: Antibiotic and surgical management
- Empiric antibiotics: Clindamycin or ampicillin-sulbactam
- Surgical drainage: Airway compromise or failed medical therapy
- ICU monitoring: Airway and hemodynamic stability
The neck's anatomical complexity creates predictable clinical patterns that enable systematic assessment and targeted management. Structure-function relationships guide diagnostic strategies, while anatomical boundaries determine surgical approaches and complication patterns. Mastering neck anatomy transforms complex clinical presentations into manageable diagnostic and therapeutic challenges.
🎯 Clinical Integration: Mastering Neck Pathology Patterns
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















