Glomerulus & Bowman's Capsule - Filtration's First Pass
- Glomerulus: Capillary tuft; blood enters via afferent arteriole (wider) & exits via efferent arteriole (narrower), maintaining high filtration pressure.
- Endothelium: Fenestrated (pores 70-100 nm), restricts cells but allows plasma.
- Bowman's Capsule: Double-walled cup surrounding glomerulus.
- Parietal layer: Outer simple squamous epithelium.
- Visceral layer: Inner layer with specialized cells - Podocytes.
- Podocytes: Have foot processes (pedicels) that interdigitate.
- Filtration slits: Spaces between pedicels, bridged by slit diaphragms (key proteins: nephrin, podocin).
- Glomerular Filtration Barrier (GFB): From capillary lumen to Bowman's space:
- Fenestrated endothelium of glomerular capillary.
- Glomerular Basement Membrane (GBM): Fused basal laminae; Type IV collagen, laminin, heparan sulfate (negatively charged, repels albumin).
- Podocyte filtration slits with slit diaphragms.
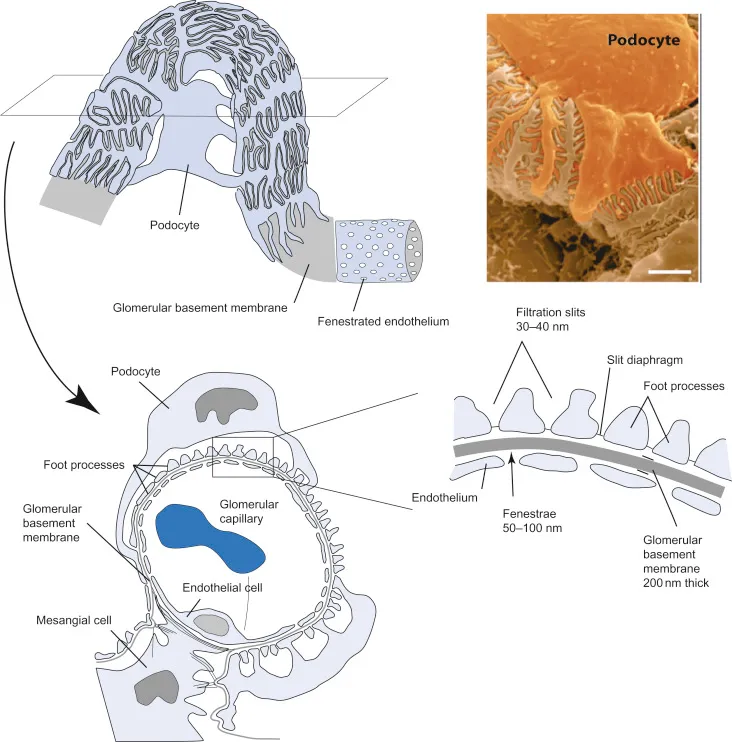
⭐ The Glomerular Basement Membrane (GBM) is the principal barrier to plasma proteins, especially albumin, due to its strong negative charge (from heparan sulfate) and fine porous structure. Damage here leads to proteinuria.
Renal Tubules & Ducts - The Modifying Maze
- Proximal Convoluted Tubule (PCT):
- Cuboidal cells, dense brush border (↑ surface area). Major reabsorption site: ~65% Na+, H2O; 100% glucose, amino acids; HCO3-.
- Secretion: H+, NH4+, organic acids/bases, drugs (📌 SAD PoCahontas: Salicylates, Allopurinol, Diuretics, Penicillin, Cephalosporins).
- Loop of Henle (LOH): Establishes medullary osmotic gradient (countercurrent multiplier).
- Descending Limb: Freely permeable to H2O, impermeable to NaCl. Concentrates filtrate.
- Ascending Limb (TAL - Thick): Actively reabsorbs Na+-K+-2Cl- (NKCC2 cotransporter). Impermeable to H2O. "Diluting segment".
- Distal Convoluted Tubule (DCT):
- Early: Reabsorbs Na+, Cl- (NCC cotransporter). Impermeable to H2O. Ca2+ reabsorption (PTH-regulated).
- Collecting System (Collecting Tubules & Ducts): Fine-tunes urine composition.
- Principal Cells: Reabsorb Na+ & H2O (ADH via Aquaporin-2); Secrete K+ (Aldosterone-regulated).
- Intercalated Cells (α & β): Acid-base balance (H+/HCO3- transport); K+ reabsorption/secretion.
⭐ The Thick Ascending Limb (TAL) of the Loop of Henle is the primary diluting segment of the nephron; it actively reabsorbs Na+, K+, and 2Cl- via the NKCC2 cotransporter but is impermeable to water, thus lowering filtrate osmolality.
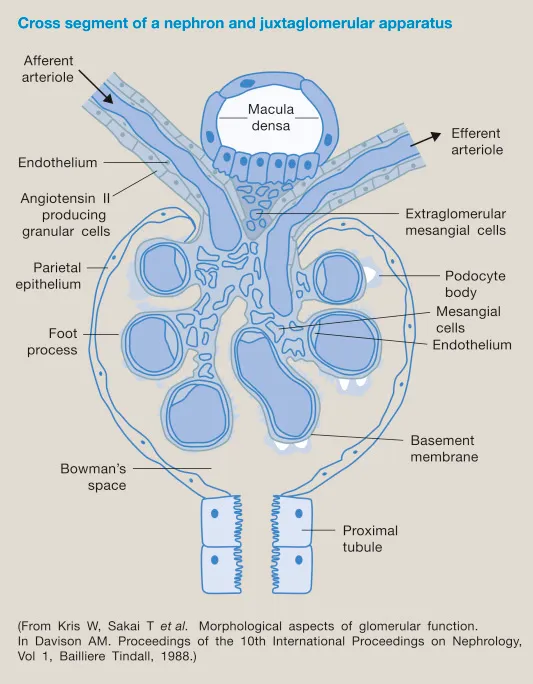
Juxtaglomerular Apparatus - The Regulation Hub
- Location: Vascular pole of glomerulus; where Distal Convoluted Tubule (DCT) contacts afferent arteriole.
- Components:
- Macula Densa: Modified DCT cells; chemoreceptors for tubular $NaCl$.
- Juxtaglomerular (JG) Cells (Granular): Modified smooth muscle (afferent/efferent arterioles); mechanoreceptors; secrete renin.
- Lacis Cells (Extraglomerular Mesangial): Between MD & arterioles; signal transmission.
- Key Functions:
- Blood Pressure (BP) regulation via RAAS.
- Glomerular Filtration Rate (GFR) regulation via TGF.
⭐ JG cells are the primary site of renin production, crucial for RAAS activation.
- Tubuloglomerular Feedback (TGF) Mechanism:
Excretory Passages - The Final Journey
- General Layers: Mucosa, muscularis, adventitia/serosa.
- Mucosa:
- Transitional epithelium (urothelium): Impermeable; superficial umbrella cells with uroplakin plaques.
- Lamina propria: Dense CT.
- Muscularis (Smooth Muscle):
- Calyces, Pelvis, Ureter: Inner longitudinal, outer circular (ILOC).
- Bladder (Detrusor): Inner longitudinal, middle circular, outer longitudinal (IL-MC-OL).
- Adventitia/Serosa: Outer CT.
- Mucosa:
- Ureter: Star-shaped lumen (mucosal folds).
- Urinary Bladder: Urothelium thins when distended; rugae when empty. Trigone is smooth.
- Urethra (Epithelium):
- Prostatic: Urothelium.
- Membranous: Stratified/pseudostratified columnar.
- Spongy: Pseudostratified columnar → stratified squamous distally.
⭐ The ureter's muscularis: inner longitudinal, outer circular smooth muscle - opposite to GIT.
High‑Yield Points - ⚡ Biggest Takeaways
- Podocytes form filtration slits crucial for the glomerular filtration barrier.
- Juxtaglomerular apparatus (JGA) includes macula densa and renin-secreting JG cells.
- PCT has a brush border for maximal reabsorption.
- Thick ascending limb of Loop of Henle actively reabsorbs Na-K-2Cl.
- Principal cells in collecting ducts respond to ADH for water reabsorption.
- Intercalated cells in collecting ducts manage acid-base balance.
- Urothelium (transitional epithelium) lines most of the urinary tract, allowing distension.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

