Introduction to Reproductive Histology - Tiny Tubes & Tissues
- Focuses on microscopic organization: tubules, follicles, specialized cells.
- Germ Cells are fundamental:
- Spermatogonia (♂): Line seminiferous tubules, become sperm.
- Oogonia (♀): In ovarian follicles, become oocytes.
- Essential Supporting Cells:
- Sertoli cells (testis): Nourish sperm, form blood-testis barrier.
- Granulosa cells (ovary): Support oocyte, produce estrogen.
⭐ Sertoli cells secrete Anti-Müllerian Hormone (AMH), vital for male sexual differentiation.
Male: Testis & Spermatogenesis - Sperm Factory Secrets

- Testis Microanatomy:
- Seminiferous Tubules: Coiled; site of sperm production. Lined by spermatogenic epithelium (Sertoli & germ cells).
- Sertoli Cells: Columnar; form blood-testis barrier; nourish germ cells; secrete ABP, inhibin. 📌 Sertoli Supports Spermatogenesis.
- Leydig Cells: Interstitial; produce testosterone (LH-stimulated). Eosinophilic; may contain Reinke crystals.
- Spermatogenesis: Spermatogonia to spermatozoa; ~74 days.
* Spermiogenesis: Metamorphosis of spermatids (no division). Acrosome formation, nuclear condensation, flagellum development.
⭐ The blood-testis barrier, by Sertoli cell tight junctions, protects developing sperm (antigenically foreign) from autoimmune attack.
Male: Ducts & Glands - The Delivery Network
- Epididymis: Pseudostratified columnar epithelium with stereocilia (non-motile microvilli); sperm maturation & storage.
- Vas Deferens: Pseudostratified columnar epithelium; thick 3-layered muscularis (L-C-L) for peristalsis.
- Seminal Vesicles: Pseudostratified columnar; secrete alkaline, viscous fluid (~70% semen volume) rich in fructose.
- Prostate Gland: Tubuloalveolar glands; secretes milky, acidic fluid with PSA, acid phosphatase. Corpora amylacea common.
- Bulbourethral Glands: Mucous secretion (pre-ejaculate) for lubrication.

⭐ Corpora amylacea are characteristic calcified glycoproteins found in the prostate gland, increasing with age.
Female: Ovary & Oogenesis - Eggcellent Adventures
- Ovary: Cortex (follicles, germinal epithelium, tunica albuginea), Medulla (vasculature).
- Oogenesis: Oogonia ($2n$) → Primary Oocyte ($2n$, Prophase I arrest) → Secondary Oocyte ($n$, Metaphase II arrest post-Meiosis I) → Ovum ($n$, post-Meiosis II if fertilized).
- Folliculogenesis & Corpus Luteum:
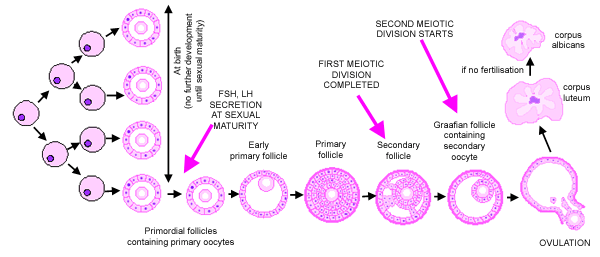
⭐ Primary oocytes arrest in Diplotene (Prophase I) until puberty; Secondary oocytes arrest in Metaphase II until fertilization.
Female: Uterus, Tubes & Vagina - Womb With A View
- Fallopian Tubes (Salpinx): Mucosa: ciliated columnar (transport), peg cells (secretory). Ampulla: fertilization site.
- Uterus:
- Endometrium: Simple columnar. Stratum functionalis (spiral arteries, sheds), Stratum basalis (regenerates).
- Myometrium: Thick smooth muscle; hypertrophy in pregnancy.
- Perimetrium: Outer serosa.
- Cervix: Endocervix (columnar, mucus), Ectocervix (strat. squamous NK). Transformation Zone (SCJ): dysplasia risk.
- Vagina: Strat. squamous NK epithelium, glycogen-rich (acidic pH via lactobacilli). No glands.

⭐ Arias-Stella reaction: nuclear atypia & cytoplasmic clearing in endometrial glands; benign, seen in pregnancy or with progestins.
High‑Yield Points - ⚡ Biggest Takeaways
- Sertoli cells: form blood-testis barrier, secrete ABP (Androgen Binding Protein), inhibin, and MIF (Müllerian Inhibiting Factor).
- Leydig cells: located in testicular interstitium, produce testosterone in response to LH (Luteinizing Hormone).
- Ovarian follicles: progress from primordial → primary → secondary → Graafian follicle (mature, pre-ovulatory).
- Corpus luteum: formed post-ovulation, secretes progesterone and estrogen, vital for early pregnancy.
- Endometrium: stratum functionalis (sheds during menstruation) and stratum basalis (regenerative layer).
- Cervix: transformation zone (squamocolumnar junction) is a key site for HPV infection and dysplasia.
- Placenta: Syncytiotrophoblast produces hCG & hPL; cytotrophoblast is the proliferative stem cell layer of villi.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

