CT Overview - Body's Scaffolding
- Origin: Derived from mesenchyme (embryonic connective tissue).
- Primary Components:
- Cells: Diverse (e.g., fibroblasts, chondrocytes, osteocytes, adipocytes, immune cells).
- Extracellular Matrix (ECM):
- Fibers: Collagen (tensile strength), Elastic (elasticity), Reticular (delicate support).
- Ground Substance: Hydrated, amorphous gel (proteoglycans, GAGs, glycoproteins); facilitates diffusion.
- General Functions: Binding & support, protection, insulation, transport (blood), repair.
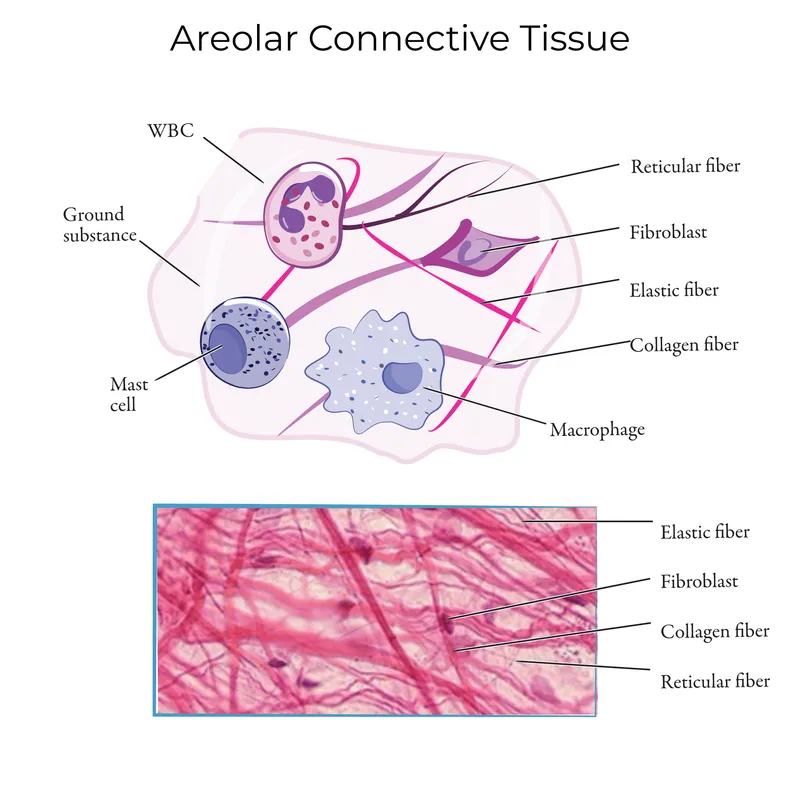
⭐ Collagen is the most abundant protein in the human body, forming the main structural protein of various connective tissues. 📌 Mnemonic: Connective Tissue = Cells + Threads (Fibers) + Ground Substance (Matrix).
CT Cells - The Busy Builders
- Resident (Fixed) Cells:
- Fibroblasts: Most common. Spindle-shaped. Synthesize ECM (collagen, elastin, GAGs). Fibrocytes are inactive.
- Adipocytes: Store lipids. Unilocular (white fat): signet-ring. Multilocular (brown fat): multiple droplets.
- Macrophages (Histiocytes): Phagocytic; kidney-bean nucleus.
- Mast Cells: Oval; granules (histamine, heparin) show metachromasia. Allergic reactions.
- Mesenchymal Stem Cells: Undifferentiated, multipotent.
- Transient (Wandering) Cells:
- Plasma Cells: Antibody production. Eccentric "clock-face" nucleus, basophilic cytoplasm, perinuclear halo (Golgi).
- Leukocytes: Neutrophils, eosinophils, lymphocytes. Migrate from blood.

⭐ Plasma cells: eccentric, "clock-face" nucleus; basophilic cytoplasm; perinuclear halo (Golgi).
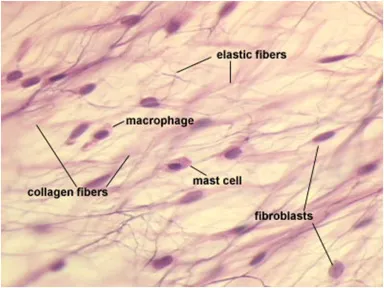
CT Fibers - Threads of Life
Essential for tissue strength, elasticity, and structural support. Three main types:
- Collagen: Most abundant protein; provides tensile strength. Triple helix (Gly-Pro-X).
- Key Types: I (Bone, Skin, Tendon - Osteogenesis Imperfecta), II (Cartilage), III (Reticular, Vessels - Ehlers-Danlos), IV (Basement Membrane - Alport Syndrome).
- Elastic Fibers: Elastin core + Fibrillin microfibrils. Enable tissue recoil.
- Defects: Marfan Syndrome (Fibrillin-1 defect), Emphysema (α1-antitrypsin deficiency).
- Reticular Fibers: Delicate Type III collagen network. Argyrophilic (silver stain).
- Forms stroma in lymphoid organs, liver, bone marrow.
⭐ Vitamin C is crucial for collagen synthesis (proline/lysine hydroxylation). Deficiency causes Scurvy: poor wound healing, bleeding gums, petechiae.
Ground Substance - The Matrix Gel
- Amorphous, hydrated, gel-like component of the Extracellular Matrix (ECM); resists compression.
- Key Components:
- Glycosaminoglycans (GAGs): e.g., Hyaluronic acid, Chondroitin sulfate. Highly negatively charged, attract $H_2O$.
- Proteoglycans: Core protein + GAGs (e.g., Aggrecan). Form large hydrated complexes.
- Adhesive Glycoproteins: e.g., Fibronectin, Laminin. Link cells to ECM components.
- Primary Functions:
- Medium for diffusion of nutrients & waste.
- Lubrication and shock absorption.
- Regulates cell adhesion, migration, and proliferation.

⭐ Hyaluronic acid is a unique GAG: it's exceptionally long, non-sulfated, and not covalently bound to a core protein, playing a key role in tissue hydration and lubrication.
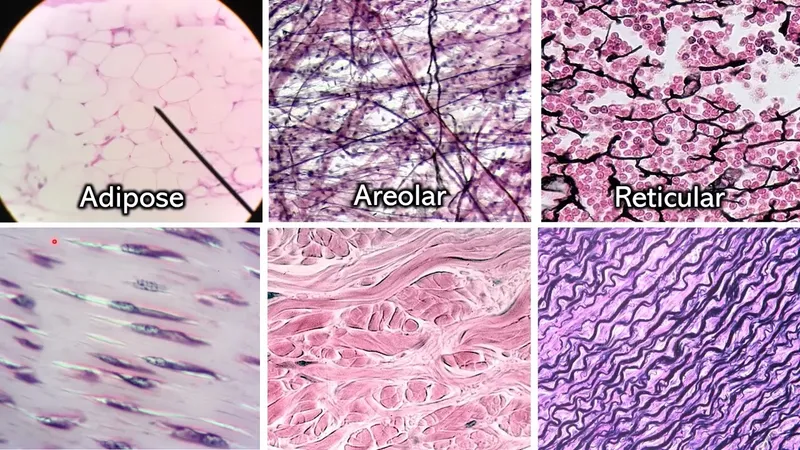
CT Proper Types - Diverse & Diffuse
- Loose CT: ↑Ground substance, ↓Fibers.
- Areolar: All 3 fibers; widespread; lamina propria.
- Adipose: Adipocytes; energy storage, insulation.
- Reticular: Reticular fibers (collagen III); stroma (spleen, lymph nodes).
- Dense CT: ↓Ground substance, ↑Fibers.
- Dense Regular: Parallel collagen I; tendons, ligaments.
- Dense Irregular: Multidirectional collagen I; dermis, capsules.
- Elastic: Elastic fibers; recoil (aorta, lung).
⭐ Keloids: excessive scar tissue from overgrowth of dense irregular CT (collagen I & III).
High‑Yield Points - ⚡ Biggest Takeaways
- Connective tissue = Cells + Fibers + Ground Substance.
- Collagen Type I: Most abundant; in bone, skin, tendon, dentin, cornea.
- Reticular fibers (Type III collagen): Support soft tissues like liver, spleen, lymph nodes.
- Elastic fibers (elastin, fibrillin): Provide recoil; fibrillin-1 defect causes Marfan syndrome.
- Mast cells: Granules contain histamine & heparin; key in allergic reactions.
- Ground substance: Composed of GAGs, proteoglycans, and adhesive glycoproteins.
- Fibroblasts: Synthesize collagen, elastin, and ground substance components.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

