Neurons & Neuroglia - Brain's Building Blocks
- Neurons: Excitable cells; functional units.
- Soma (perikaryon): Nissl bodies (RER), nucleus.
- Dendrites: Receive signals.
- Axon: Transmits signals; axon hillock. Nodes of Ranvier (saltatory conduction).
- Myelin: ↑ conduction. Schwann (PNS, 1 axon), Oligodendrocytes (CNS, many axons).
- Neuroglia (Glial Cells): Support neurons. More numerous.
- CNS Glia:
- Astrocytes: Largest, star-shaped. Blood-Brain Barrier (BBB), K+ buffer, GFAP+.
- Oligodendrocytes: Myelinate CNS axons (many). Damaged in MS.
- Microglia: Phagocytic (macrophage-like). Monocyte-derived.
- Ependymal cells: Line ventricles, central canal. CSF production (choroid plexus).
- PNS Glia:
- Schwann cells: Myelinate PNS axon (1). Aid regeneration. Damaged in GBS.
- Satellite cells: Support ganglia neurons.
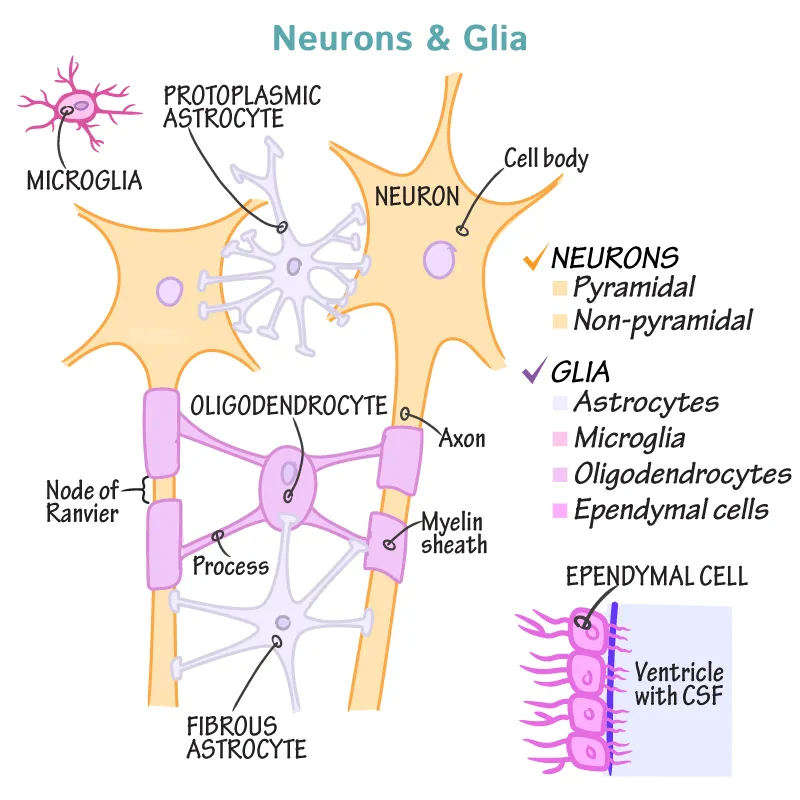
- CNS Glia:
⭐ Microglia are of mesodermal origin; other glial cells are neuroectodermal.
Myelin & Fibers - Speedy Signal Conduits
- Myelin Sheath: Insulates axons; ↑ conduction velocity.
- PNS: Schwann Cells (myelinate 1 axon segment; aid regeneration).
- CNS: Oligodendrocytes (myelinate multiple axons; no significant regeneration).
- Nodes of Ranvier: Myelin gaps; high Na+ channel density.
- Saltatory Conduction: AP "jumps" node to node; ↑ speed, conserves energy.
- Nerve Fibers (Erlanger-Gasser Classification):
- Type A: Large, myelinated (e.g., Aα: proprioception, motor). Fastest.
- Type B: Smaller, myelinated (e.g., preganglionic autonomic).
- Type C: Smallest, unmyelinated (e.g., pain, temperature, postganglionic autonomic). Slowest. 📌 Always Be Careful (A>B>C)
⭐ Oligodendrocytes in CNS myelinate multiple axons, while Schwann cells in PNS myelinate a single axon segment and aid in regeneration.
Synapses & Ganglia - Neural Network Hubs
- Synapse: Junction for neuronal communication.
- Chemical: Neurotransmitters (e.g., ACh, GABA); unidirectional; synaptic delay. Key: presynaptic terminal, cleft, postsynaptic membrane.
- Electrical: Gap junctions; rapid, bidirectional flow.
- Ganglia: Neuronal cell body clusters outside CNS.
- Sensory (e.g., DRG): Pseudounipolar neurons. Satellite cells. No synapses.
⭐ Dorsal root ganglia (sensory) contain pseudounipolar neurons with centrally located nuclei and surrounding satellite cells, and NO synapses.
- Autonomic (Symp/Parasymp): Multipolar neurons. Synapses present. Fewer satellite cells.

- Sensory (e.g., DRG): Pseudounipolar neurons. Satellite cells. No synapses.
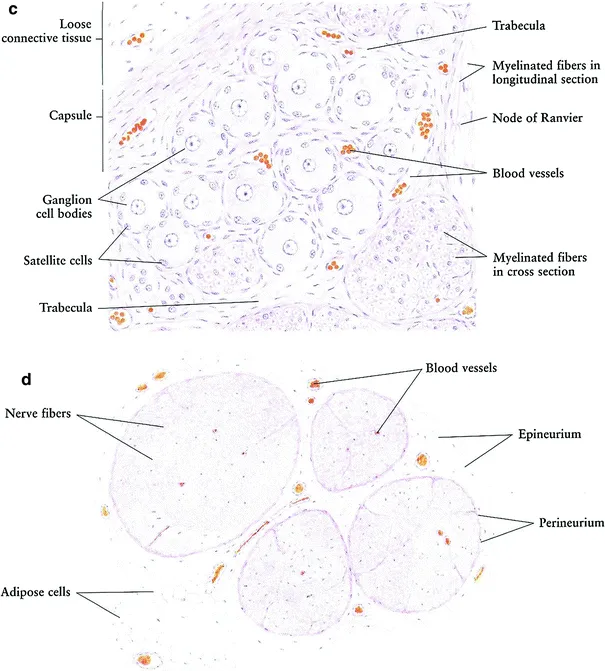
Nerve Coverings - Protective Nerve Wraps
- Peripheral nerves: wrapped in three connective tissue (CT) layers:
- Epineurium: Outermost; dense irregular CT; surrounds entire nerve; contains vasa nervorum.
- Perineurium: Middle; surrounds nerve fascicles; specialized CT.
⭐ The perineurium, composed of layers of flattened fibroblast-like cells with tight junctions, forms the blood-nerve barrier.
- Endoneurium: Innermost; loose CT; surrounds individual nerve fibers & Schwann cells; contains capillaries.
- 📌 Mnemonic: Eat Pizza Everyday (Epineurium, Perineurium, Endoneurium - from out to in).

Nerve Injury & Repair - Damage & Fix Crew
- Seddon's Classification (📌 NAP for severity ↑):
- Neuropraxia: Myelin damage, temporary conduction block. Full, rapid recovery.
- Axonotmesis: Axon severed, endoneurium intact. Wallerian degeneration distally. Regeneration (1-4 mm/day) via Büngner bands.
- Neurotmesis: Complete nerve transection (axon, sheaths). Surgery essential. Poor prognosis.
- Key Processes:
- Wallerian Degeneration: Distal axon/myelin breakdown, macrophage cleanup.
- Chromatolysis: Proximal cell body changes.
- Regeneration: Axonal sprouting, Schwann cell guidance (Bands of Büngner).
⭐ Chromatolysis (central chromatolysis) involves swelling of the neuron cell body, eccentric displacement of the nucleus, and dispersal of Nissl substance, occurring after axonal injury.
High‑Yield Points - ⚡ Biggest Takeaways
- Neurons: functional units; Neuroglia: support (Astrocytes, Oligodendrocytes, Microglia, Ependymal cells).
- Nissl bodies (RER): in soma/dendrites; absent in axon hillock/axon.
- Myelin: Schwann cells (PNS), Oligodendrocytes (CNS); for saltatory conduction at Nodes of Ranvier.
- Astrocytes: largest glia, form blood-brain barrier, structural/metabolic support.
- Microglia: CNS macrophages (mesodermal origin), phagocytic.
- Ependymal cells: line ventricles/central canal, CSF production/circulation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

