Bony Orbit & Openings - Socket Science
- Cavity: Pyramidal, 4 walls.
- Bones (7): Frontal, Sphenoid, Zygomatic, Maxillary, Palatine, Lacrimal, Ethmoid.
- Walls:
- Roof: Frontal, Sphenoid (Lesser W).
- Floor: Maxillary, Zygomatic, Palatine.
⭐ Orbital floor (Maxillary, Zygomatic, Palatine) = weakest; common blow-out fracture site. Risks Inf. Rectus / Infraorbital N. entrapment.
- Medial: Maxillary, Lacrimal, Ethmoid (Lamina Papyracea: thinnest), Sphenoid (Body).
- Lateral: Zygomatic, Sphenoid (Greater W: strongest).
- Key Openings:
- Optic Canal: CN II, Ophthalmic A.
- SOF: CN III, IV, V1, VI, Sup. Ophthalmic V.
- IOF: CN V2, Inf. Ophthalmic V, Infraorbital A/N.

Extraocular Muscles - Eye Gymnastics
- Muscles: 4 Recti (Superior, Inferior, Medial, Lateral) & 2 Obliques (Superior, Inferior).
- Origin:
- Common Tendinous Ring (Annulus of Zinn): SR, IR, MR, LR, SO.
- Orbital surface of maxilla: IO.
- Innervation: 📌 LR6SO4R3 (Lateral Rectus: CN VI; Superior Oblique: CN IV; Rest: CN III).
- Primary Actions (Muscle):
- Adduction (MR), Abduction (LR).
- Elevation (SR + IO), Depression (IR + SO).
- Intorsion (SO + SR), Extorsion (IO + IR).
⭐ All extraocular muscles originate from the common tendinous ring (Annulus of Zinn) except the inferior oblique, which originates from the orbital surface of the maxilla near the lacrimal fossa.

Orbital Nerves & Vessels - Wire & Pipe Works
- Nerves:
- CN II (Optic): Vision; via optic canal.
- CN III (Oculomotor): Motor to most EOMs, LPS; parasympathetic (miosis).
- CN IV (Trochlear): Motor to SO.
- CN V1 (Ophthalmic): Sensory. Branches: Lacrimal, Frontal, Nasociliary (eye sensation, pupil dilation sympathetics).
- CN VI (Abducens): Motor to LR.
- 📌 SOF Mnemonic: "Live Frankly To See Absolutely No Insult" (Lacrimal, Frontal, Trochlear, Sup.CNIII, Abducens, Nasociliary, Inf.CNIII).
- Vessels:
- Ophthalmic Artery (from ICA): Main supply; via optic canal.
- Central Retinal Artery (CRA): Inner retina; end artery.
- Ophthalmic Veins (S&I): To cavernous sinus.
- Ophthalmic Artery (from ICA): Main supply; via optic canal.

⭐ The central retinal artery, a branch of the ophthalmic artery, is an end artery; its occlusion leads to sudden, painless, and usually permanent loss of vision in the affected eye.
Orbital Contents & Lacrimal Path - Globe & Tears
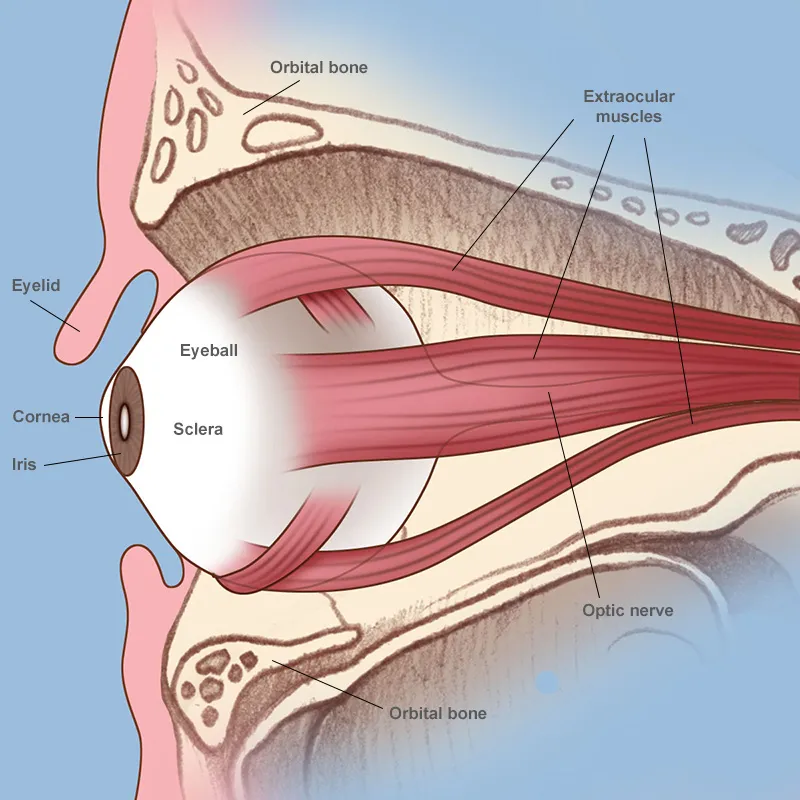
- Globe (Eyeball): Primary orbital structure; cushioned by orbital fat.
- Coats: Outer (Sclera, Cornea); Middle/Uvea (Iris, Ciliary body, Choroid); Inner (Retina).
⭐ Tenon's capsule (fascia bulbi) envelops the eyeball from the optic nerve to the corneoscleral junction, forming a socket that facilitates eye movements and provides sheaths for the extraocular muscles.
- Lacrimal System: Tear production & drainage.
- Gland: Lacrimal gland (superolateral orbit).
- Drainage Path: 📌 Puncta → Canaliculi → Lacrimal Sac → Nasolacrimal Duct → Inferior meatus.

Clinical Quick Hits - Orbit Ouchies
- Orbital Cellulitis: Posterior to septum. Proptosis, ↓vision, painful EOMs.
⭐ Orbital cellulitis, an infection posterior to the orbital septum, is a medical emergency often secondary to ethmoidal sinusitis, requiring prompt IV antibiotics to prevent vision loss or cavernous sinus thrombosis.
- Preseptal Cellulitis: Anterior to septum. Lid swelling; vision, EOMs normal.
- Blowout Fracture: Inferior wall common. Diplopia (upgaze), infraorbital numbness.
- Thyroid Eye Disease: Proptosis, lid lag. EOMs: IR > MR > SR > LR. 📌 I'M SLOW (Inferior, Medial, Superior, Lateral recti).
High-Yield Points - ⚡ Biggest Takeaways
- Orbit: Formed by 7 bones. Orbital floor (maxilla) is weakest, common site for blowout fractures.
- Optic Canal: Transmits CN II & ophthalmic artery.
- Superior Orbital Fissure: Transmits CN III, IV, V1, VI & superior ophthalmic vein.
- Muscles: Innervation by LR6SO4R3. Annulus of Zinn is origin for recti muscles.
- Cavernous sinus thrombosis: A risk from orbital infections via valveless ophthalmic veins.
- Central Retinal Artery: An end artery from ophthalmic artery; occlusion leads to sudden blindness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

