Oral Cavity & Pharynx - Mouthful Marvels
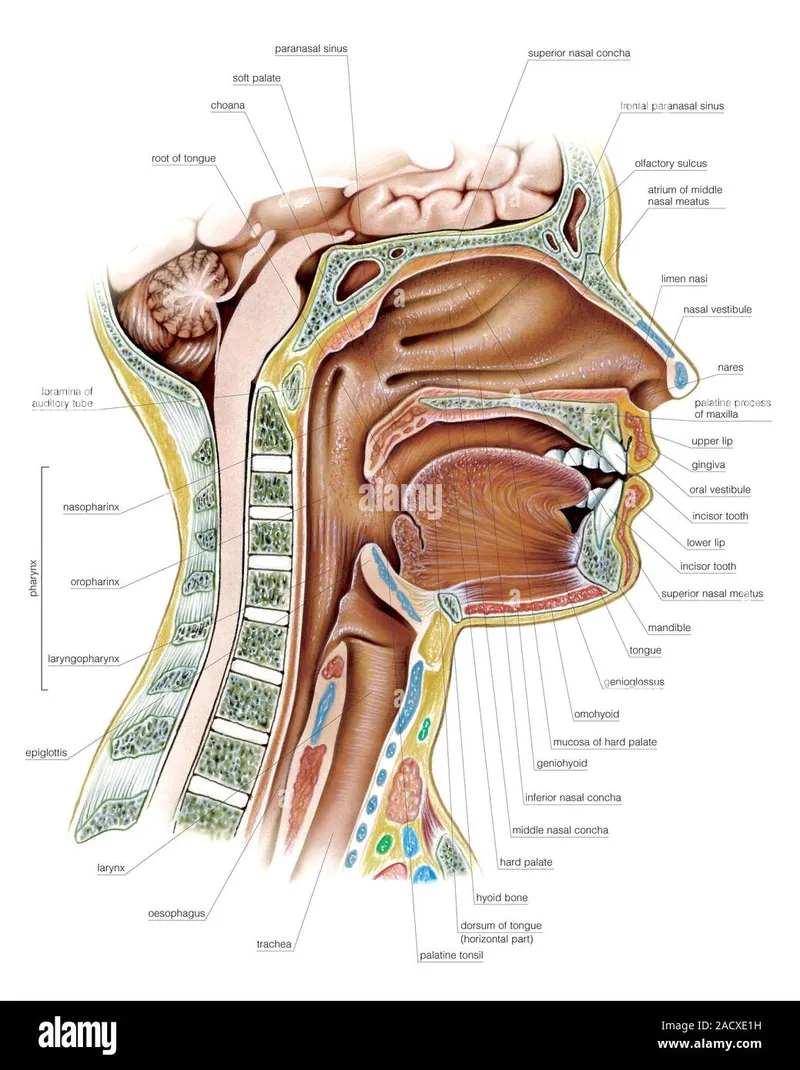
- Salivary Glands: Parotid (Stensen's), Submandibular (Wharton's), Sublingual (Rivinus).
- Teeth (Function): Incisors (cutting), Canines (tearing), Premolars & Molars (grinding).
- Tongue: Papillae: Filiform (touch), Fungiform, Circumvallate, Foliate (taste). Taste buds present.
- Muscles of Mastication: 📌 MaTe MeLa: Masseter, Temporalis, Medial & Lateral pterygoids (CN V3).
- Swallowing (Deglutition):
⭐ Tongue Innervation (Sensory): Ant. 2/3: Lingual (general, V3), Chorda tympani (taste, VII). Post. 1/3: Glossopharyngeal (general & taste, IX). Motor: Hypoglossal (XII) except Palatoglossus (X).
Esophagus & Stomach - Gut's Gateway Grub
- Esophagus: Muscular tube; non-keratinized stratified squamous epithelium.
- Constrictions (4): Cricoid, Aortic arch, L. main bronchus, Diaphragmatic hiatus. 📌 Cars Are Big Danger.
- Sphincters: UES; LES (physiological, pressure 10-25 mmHg). ↓LES tone → GERD.
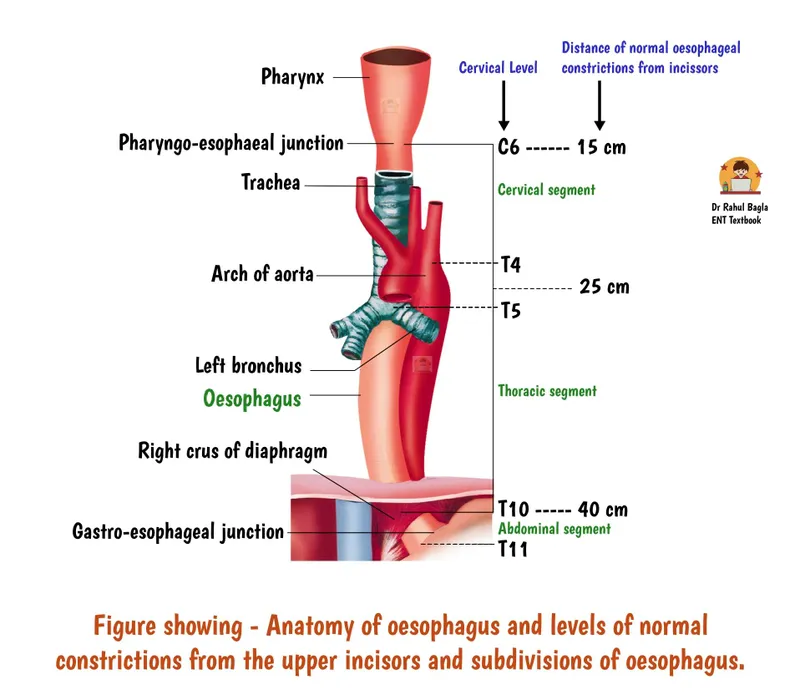
- Stomach: J-shaped; regions (Cardia, Fundus, Body, Antrum, Pylorus); rugae for expansion.
- Gastric Glands & Cells:
Cell Secretion(s) Stimulants Parietal HCl (pH 1.5-3.5), Intrinsic Factor ACh, Gastrin, Histamine Chief Pepsinogen, Gastric Lipase ACh, Gastrin, Secretin Mucous Neck Mucus, Bicarbonate Vagal, Prostaglandins G-cells Gastrin Peptides, AAs, Vagal
⭐ Left gastric artery (from celiac trunk) supplies stomach's lesser curvature, a common site for ulcers and bleeding.
- Gastric Glands & Cells:
Small Intestine - Absorb All Action
Primary site for digestion & absorption. 📌 "Dow Jones Industrial" (Duodenum, Jejunum, Ileum).
Comparative Features:
| Feature | Duodenum | Jejunum | Ileum |
|---|---|---|---|
| Length | ~25 cm | ~2.5 m | ~3.5 m |
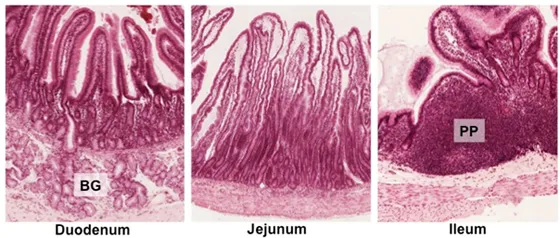
| Glands/Tissue | Brunner's (submucosa, alkaline) | - (Maximal absorption) | Peyer's Patches (MALT) |
| Villi | Broad, leaf-shaped | Long, finger-shaped | Short, club-shaped |
| Plicae Circulares | Tall, numerous | Large, prominent | Low, sparse |
| Key Absorption | Fe, Ca | Most nutrients | Vit B12, Bile Salts |
- Plicae circulares (valves of Kerckring): ↑ 3x
- Villi: ↑ 10x
- Microvilli (brush border): ↑ 20x (Total ↑ ~600x)
Key Cells:
- Enterocytes: Absorption (brush border enzymes)
- Goblet cells: Mucus
- Paneth cells: Lysozyme, defensins (crypts)
Carbohydrate Absorption Pathway:
⭐ Duodenum is the primary site for iron (Fe²⁺ via DMT1) and calcium absorption.
Large Intestine Complex - Colon Cleanup Crew
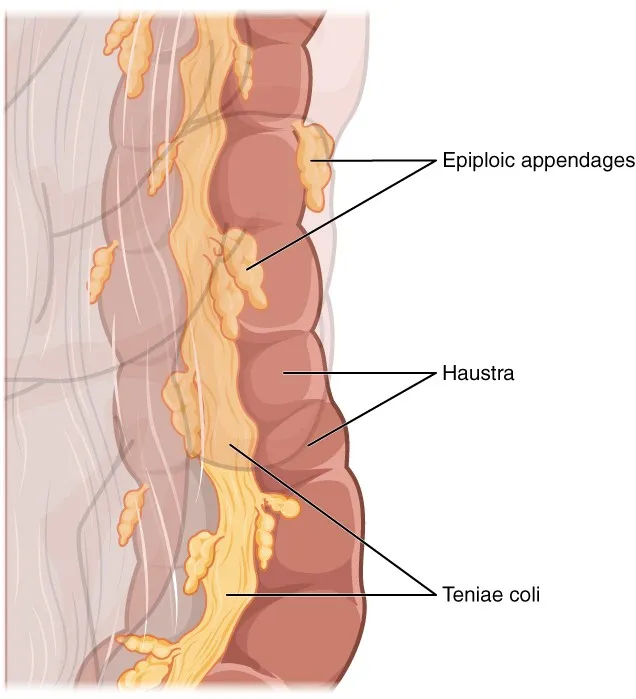
- Parts: Cecum, appendix, colon (ascending, transverse, descending, sigmoid), rectum, anal canal.
- Hallmarks: Taeniae coli (3 muscle bands), haustra (sacculations), epiploic appendages (fat sacs).
- Microscopy: Abundant goblet cells; no villi.
- Supply: Arterial: Superior Mesenteric Artery (SMA), Inferior Mesenteric Artery (IMA). Innervation: Enteric NS, Vagus (proximal), Pelvic splanchnics (S2-S4, distal parasympathetic).
- Roles: Water/electrolyte absorption. Bacterial Vit K, B synthesis. Feces formation, storage, expulsion.
⭐ Exam Favourite: Watershed areas prone to ischemia: Griffith's point (splenic flexure: SMA-IMA junction) & Sudeck's point (rectosigmoid junction: IMA-superior rectal artery).
Defecation Reflex Pathway:
Accessory Digestive Organs - Gland Grandeur Guides
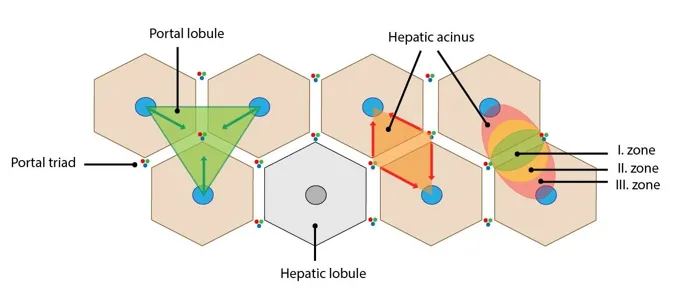
- Liver: Portal triad (Bile Duct, Hepatic Artery, Portal Vein 📌 DAVE). Functional unit: hepatic acinus (vs classic lobule). Synthesizes bile.
⭐ Portal triad contents: Portal vein, Hepatic artery, Bile duct.
- Gallbladder: Stores & concentrates bile. Cholecystokinin (CCK) stimulates contraction & bile release.
- Pancreas (Exocrine): Acini secrete enzymes; ducts secrete bicarbonate ($HCO_3^-$).
- Regulation: Secretin → ↑$HCO_3^-$; CCK → ↑enzymes.
- Regulation: Secretin → ↑$HCO_3^-$; CCK → ↑enzymes.
Pancreatic Enzymes:
| Enzyme | Activator | Substrate |
|---|---|---|
| Trypsinogen | Enterokinase | Proteins |
| Chymotrypsinogen | Trypsin | Proteins |
| Amylase | - | Carbohydrates |
| Lipase | Colipase | Fats |
High‑Yield Points - ⚡ Biggest Takeaways
- Meissner's plexus (submucosal) governs secretions/blood flow; Auerbach's plexus (myenteric) controls motility.
- Interstitial Cells of Cajal (myenteric plexus) are pacesetter cells generating slow waves.
- Brunner's glands (duodenum) secrete alkaline mucus to neutralize chyme.
- Peyer's patches (lymphoid aggregates) are most numerous in the ileum.
- Taeniae coli contraction forms haustra in the large intestine.
- Sphincter of Oddi controls bile/pancreatic juice flow into the duodenum.
- G cells (gastric antrum) secrete gastrin, stimulating HCl secretion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

