Gametogenesis Overview - Germ Cell Genesis
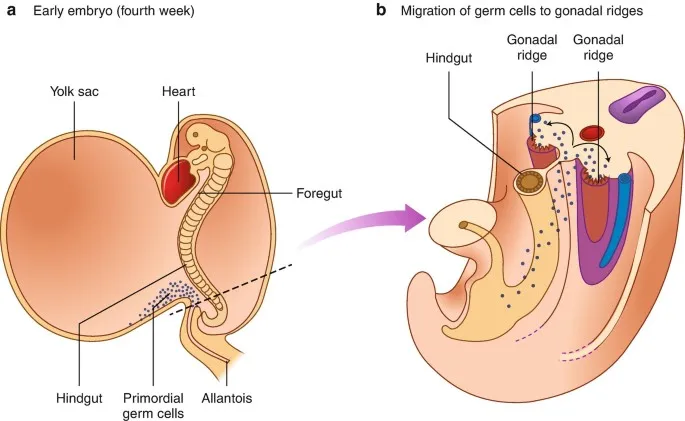
- Primordial Germ Cells (PGCs): Epiblast origin (2nd wk); migrate via yolk sac to gonadal ridge (4th-6th wk).
- Gametogenesis: PGCs form gametes. Involves mitosis (proliferation) & meiosis (maturation).
- Mitosis: Diploid (2n) cell → two identical diploid (2n) cells. For PGC proliferation.
- Meiosis: Diploid (2n, 4c) cell → four haploid (1n, 1c) gametes. Two stages:
- Meiosis I (Reductional): Homologous chromosomes separate. (2n, 4c → 1n, 2c)
- Meiosis II (Equational): Sister chromatids separate. (1n, 2c → 1n, 1c)
⭐ PGCs are visible in the yolk sac wall by the 3rd week.
Spermatogenesis - Sperm Squadron
Spermatozoa formation in seminiferous tubules from puberty. Duration: ~74 days.
- Stages:
- Spermatogonia (2n) → Primary Spermatocyte (2n)
- Meiosis I: Primary Spermatocyte → 2 Secondary Spermatocytes (n)
- Meiosis II: Secondary Spermatocytes → 4 Spermatids (n)
- Spermiogenesis (Spermatid → Spermatozoon):
- Acrosome formation (enzymes)
- Nuclear condensation, flagellum development, cytoplasm shed.
- Hormonal Control:
- GnRH → LH (Leydig cells: Testosterone↑) & FSH (Sertoli cells: ABP, Inhibin↓FSH)
- Testosterone: essential. ABP: concentrates testosterone.
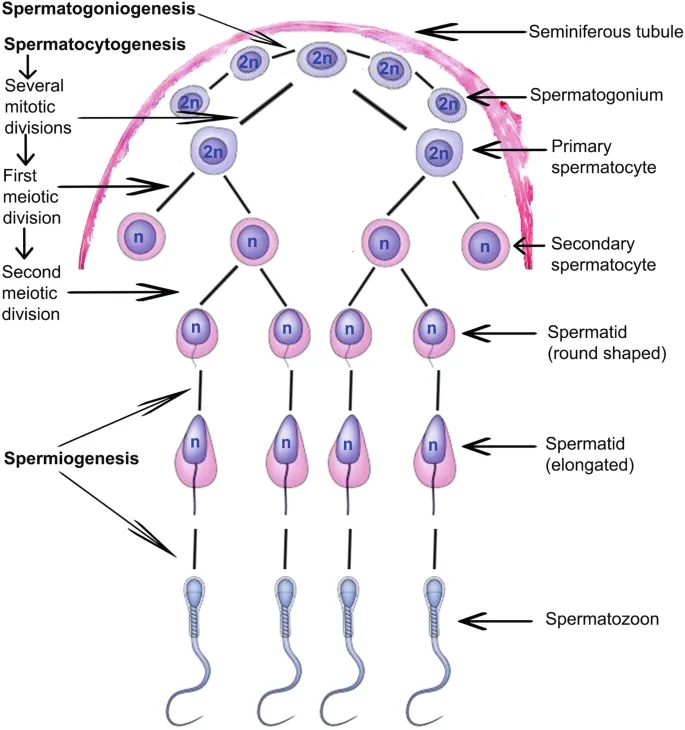
⭐ Spermatogenesis results in four functional spermatozoa from each primary spermatocyte.
- Sperm: Head (acrosome, nucleus), Midpiece (mitochondria), Tail (flagellum).
Oogenesis & Ovulation - Ovum Odyssey
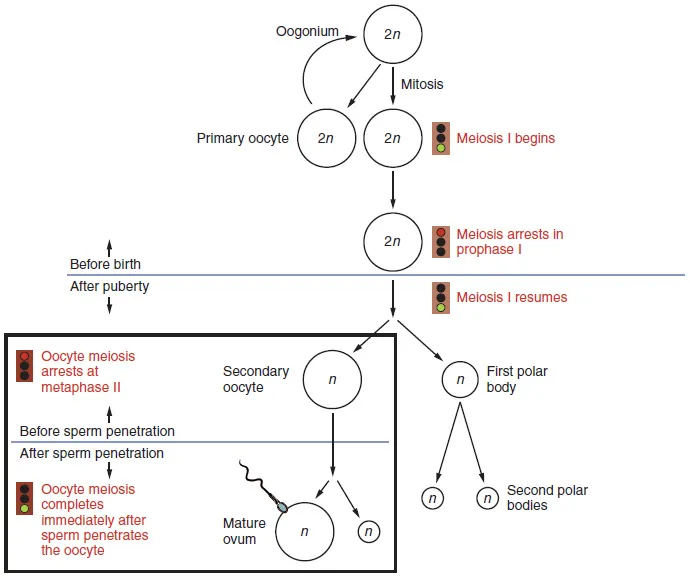
- Prenatal Start: Oogonia → primary oocytes, arrested in Prophase I (diplotene) until puberty.
- Follicular Development: Primordial → Primary → Secondary → Graafian (mature) follicle under hormonal influence.
- Puberty Onset: FSH stimulates maturation. Primary oocyte completes Meiosis I → secondary oocyte (arrested Metaphase II) + 1st polar body.
- Ovulation Trigger: LH surge ~24-36h prior → Graafian follicle rupture, releasing secondary oocyte.
- Fertilization: If sperm penetrates, Meiosis II completes → mature ovum + 2nd polar body.
⭐ LH surge is essential for final oocyte maturation, resumption of meiosis, and ovulation.
Fertilization - Zygote Zeal
- Sperm Journey & Maturation:
- Capacitation: Hyperactivation in female tract; cholesterol removal, ↑Ca$^{2+}$ influx.
- Penetration of Barriers:
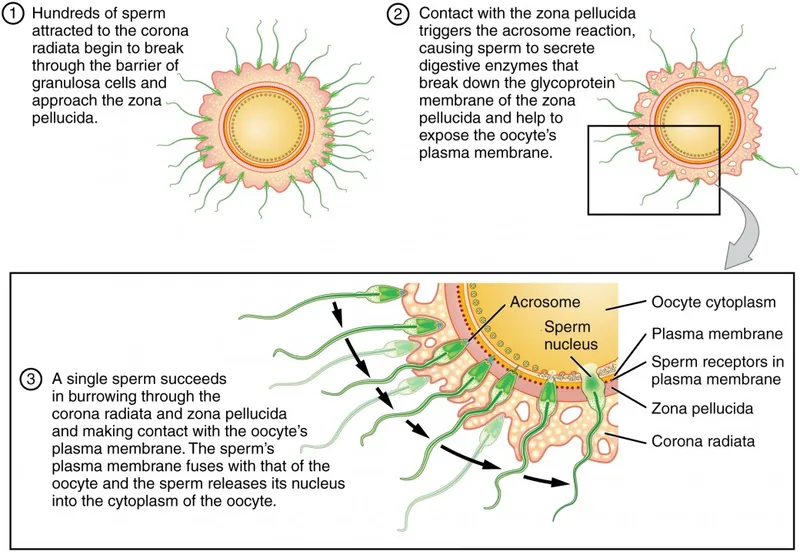
- Corona Radiata: Dispersed by sperm hyaluronidase & tubal enzymes.
- Zona Pellucida (ZP):
- Acrosome Reaction: Triggered by ZP3 binding; exocytosis of acrosomal enzymes (acrosin, hyaluronidase).
- Sperm binds ZP2, penetrates ZP via acrosin digestion.
- Gamete Fusion & Oocyte Activation:
- Sperm fuses oocyte membrane (oolemma); integrins, CD9 involved.
- Cortical Reaction: Oocyte cortical granule release → Zona block (ZP hardening, ZP3 inactivation), prevents polyspermy.
- Oocyte completes Meiosis II → mature ovum + 2nd polar body.
- Zygote Formation:
- Male & female pronuclei (haploid) form.
- Syngamy: Pronuclei fuse → Zygote (diploid, $2n$).
⭐ Fertilization typically occurs in the ampulla of the fallopian tube.
High‑Yield Points - ⚡ Biggest Takeaways
- Spermatogenesis begins at puberty; Oogenesis initiates in fetal life, arresting in Prophase I (Diplotene stage).
- Oocyte Meiosis I completes just before ovulation; Meiosis II completes only after fertilization.
- Spermiogenesis is the morphological transformation of spermatids into spermatozoa (no cell division).
- Sperm capacitation (in female tract) and acrosome reaction (near oocyte) are essential for fertilization.
- Fertilization most commonly occurs in the ampulla of the fallopian tube.
- The cortical reaction leads to the zona reaction, preventing polyspermy.
- ZP3 glycoprotein of the zona pellucida acts as the primary sperm receptor site.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more