Pharyngeal Apparatus Overview - Neck's Early Sketch
- Transient structures appearing in 4th-5th weeks, forming head/neck.
- Components:
- Pharyngeal Arches: 6 pairs (5th rudimentary/absent), mesenchymal core.
- Pharyngeal Pouches: 5 pairs, endodermal outpocketings.
- Pharyngeal Grooves (Clefts): 4 pairs, ectodermal invaginations.
- Pharyngeal Membranes: Ecto-endodermal contact points.
- Germ Layers:
- Ectoderm: External lining, grooves.
- Mesoderm (paraxial, lateral plate) & Neural Crest Cells (NCCs): Arch core (muscles, arteries, cartilage).
- Endoderm: Internal lining, pouches.

⭐ Neural Crest Cells are pivotal for craniofacial skeletal and connective tissues; defects cause syndromes like DiGeorge or Treacher Collins.
Pharyngeal Arch Derivatives - Arch's Mighty Minions
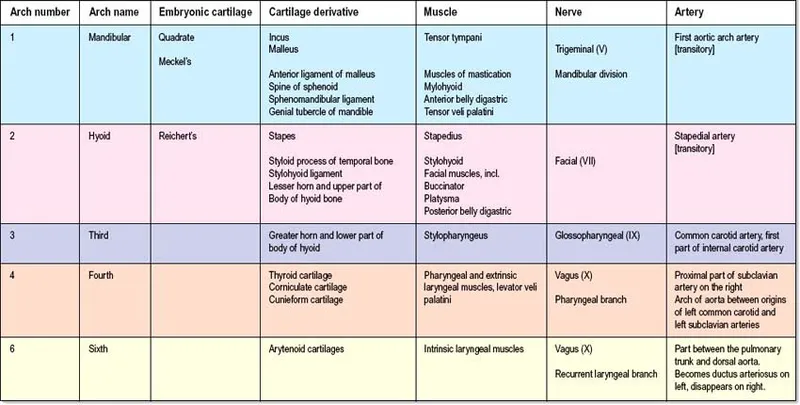
📌 Nerves: Tall Fairies Go Vaping. (Trigeminal, Facial, Glossopharyngeal, Vagus for arches 1,2,3,4/6 respectively).
| Arch | Nerve (N) | Artery (A) | Muscles (M) | Skeletal/Cartilage (S) |
|---|---|---|---|---|
| 1 | Trigeminal (V) | Maxillary | Mastication, Mylohyoid, Ant.Dig, TT, TVP | Malleus, Incus, Mandible (Meckel's), Maxilla, Zygoma |
| 2 | Facial (VII) | Stapedial | Facial Exp, Stapedius, Stylohyoid, Post.Dig | Stapes, Styloid, Lesser Hyoid (Reichert's) |
| 3 | Glossopharyngeal (IX) | Common/Internal Carotid | Stylopharyngeus | Greater Hyoid |
| 4 | Vagus (X) - Sup. Laryng. | Aortic Arch (L), R. Subclavian (prox.) | Pharynx constrictors, Cricothyroid | Thyroid, Epiglottis, Sup. Laryngeal cartilages |
| 6 | Vagus (X) - Rec. Laryng. | Pulmonary a., Ductus Art. | Intrinsic Larynx (exc. Cricothyroid) | Inf. Laryngeal cartilages (Cricoid, Arytenoids) |
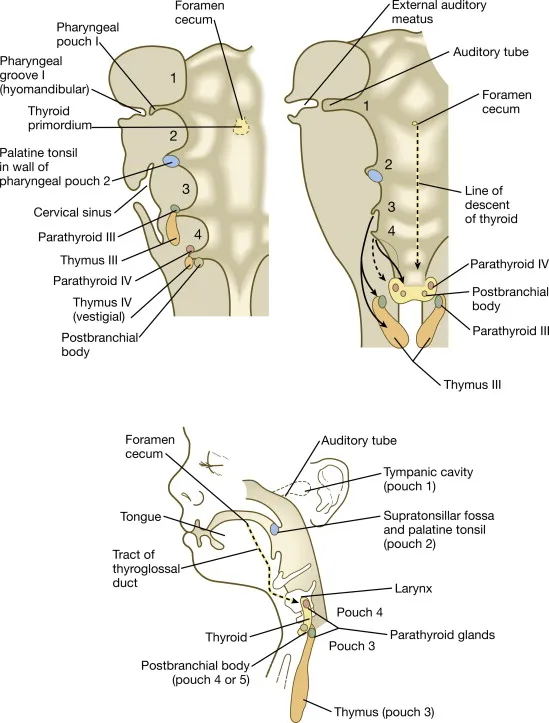
Pouches, Grooves & Membranes - Gulp & Groove Goodies
- Pharyngeal Pouches (Endoderm): 📌 "PET CAT" (Palatine, Eustachian, Thymus, C cells, Parathyroids)
- 1st: Middle ear cavity, Eustachian tube, mastoid antrum.
- 2nd: Palatine tonsil crypts, tonsillar fossa.
- 3rd: Inferior parathyroid gland, thymus.
- 4th: Superior parathyroid gland, ultimobranchial body (→ C cells).
- Pharyngeal Grooves/Clefts (Ectoderm):
- 1st Groove: External acoustic meatus.
- 2nd-4th Grooves: Overgrown by 2nd arch, form cervical sinus (obliterates). Failure → Branchial (cervical) cyst/fistula.
- Pharyngeal Membranes (Ecto/Endoderm):
- 1st Membrane: Tympanic membrane. Others disappear.
- Anomalies:
- Branchial Cysts/Fistulas: Lateral cervical cysts, anterior to SCM.
- DiGeorge Syndrome (22q11.2 deletion): Failure of 3rd & 4th pouch development. Thymic/parathyroid aplasia. 📌 CATCH-22.
⭐ DiGeorge syndrome results from failure of neural crest cell migration to the 3rd and 4th pharyngeal pouches and arches.
Face, Palate & Tongue Dev. - Face-Making Fiesta

-
Face (4th-8th wks): 5 prominences:
- 1 Frontonasal: Forehead, nose bridge, medial/lateral nasal prominences.
- 2 Maxillary: Cheeks, lat. upper lip, secondary palate.
- 2 Mandibular: Lower lip, jaw.
- 📌 Maxillary + Medial nasal prom. → Upper lip. Failure → Cleft Lip.
-
Palate (6th-12th wks):
- Primary: Intermaxillary segment (fused medial nasal prom.).
- Secondary: Palatal shelves (from maxillary prom.). Fusion crucial.
-
Tongue:
- Ant. ⅔ (Oral): 1st arch (2 lat. lingual swellings, 1 tuberculum impar). Sensory: CN V3; Taste: CN VII (chorda tympani).
- Post. ⅓ (Pharyngeal): 3rd & 4th arches (copula/hypobranchial eminence). Sensory & Taste: CN IX; CN X (epiglottis).
- Muscles: Occipital somites (CN XII).
-
Anomalies:
- Cleft Lip (CL): Maxillary prom. fails to fuse with medial nasal prom.
- Cleft Palate (CP): Palatal shelves fail to fuse.
⭐ Isolated cleft palate is more common in females (approx. 2:1), while cleft lip ± cleft palate is more common in males (approx. 2:1).
High-Yield Points - ⚡ Biggest Takeaways
- 1st Arch (Mandibular): CN V3, mastication muscles, Meckel's. Treacher Collins.
- 2nd Arch (Hyoid): CN VII, facial expression muscles, Reichert's.
- Pouches: 3rd (inferior parathyroids, thymus), 4th (superior parathyroids). DiGeorge syndrome.
- Tongue: Ant ⅔ (Arch 1: CN V3 sensory, CN VII taste); Post ⅓ (Arch 3: CN IX).
- Thyroid: From foramen cecum. Thyroglossal duct cyst (midline).
- Clefts: Lip (maxillary + medial nasal prominence fusion failure); Palate (palatal shelf fusion failure).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

