Introduction & Classification - Anomaly ABCs
- Congenital Anomaly: Structural/functional defect present at birth.
- Primary Types (📌 MDDD):
- Malformation: Intrinsic developmental error (e.g., NTD). 📌 Made wrong.
- Disruption: Extrinsic breakdown of normal tissue (e.g., amniotic bands). 📌 Destroyed.
- Deformation: Abnormal form from mechanical force (e.g., clubfoot). 📌 Distorted.
- Dysplasia: Abnormal cell organization in tissue (e.g., achondroplasia). 📌 Disorganized.
- Multiple Anomalies:
- Syndrome: Pattern of anomalies, known common cause (e.g., Down syndrome).
- Sequence: Single primary defect leads to cascade (e.g., Potter sequence).
- Association: Non-random co-occurrence, unknown cause (e.g., VACTERL).
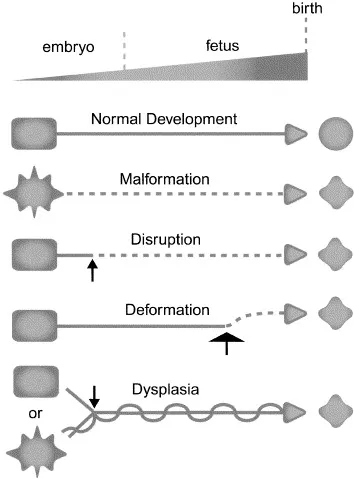
⭐ Most major congenital anomalies arise during the embryonic period (3rd-8th week).
Etiological Factors - Culprit Countdown
- Genetic (~30-40%):
- Chromosomal:
- Numerical: Aneuploidy (Trisomy 21, 18, 13; Monosomy 45,XO Turner's)
- Structural: Deletions (Cri-du-chat $5p-$), Translocations
- Single Gene (Mendelian):
- AD (Achondroplasia), AR (Cystic Fibrosis), X-L (Hemophilia)
- Chromosomal:
- Environmental (Teratogens; ~10%):
- Drugs: Thalidomide (limbs), Valproate (NTDs), Alcohol (FAS), Warfarin, ACEi
- Infections: 📌 TORCHES-Z (Toxoplasma, Other [Syphilis, VZV, Parvo B19], Rubella, CMV, Herpes, Zika)
- Maternal: Diabetes (cardiac, NTDs), PKU (CNS), Hypothyroidism
- Radiation: Ionizing (>0.05 Gy); CNS/skeletal defects; dose/timing critical
- Multifactorial (~20-25%):
- Genes + Environment interaction
- E.g., Cleft lip/palate, NTDs, most CHDs, Pyloric stenosis
- Unknown (~25-40%): Significant proportion.

⭐ The critical period for teratogenic insult is weeks 3-8 of gestation (embryonic period), when organogenesis is at its peak.
Timing is Everything - Susceptibility Windows
- Teratogen impact varies critically with gestational timing.
- All-or-None Period (0-2 weeks post-conception):
- Exposure causes embryo death or full recovery; no anomalies.
- Embryonic Period (Weeks 3-8): Organogenesis
- Maximum susceptibility to major structural defects.
- Specific critical windows:
- CNS: Weeks 3-16+
- Heart: Weeks 3-6
- Limbs: Weeks 4-7
- Palate: Weeks 6-9
- Fetal Period (Week 9 - Birth):
- Leads to functional defects, minor anomalies, growth issues.
- CNS remains vulnerable.

⭐ Neural tube defects (NTDs) arise from failed neural tube closure between days 21-28 post-conception (critical in weeks 3-4).
Mechanisms & Examples - Defect Detectives
- Teratogenesis Principles:
- Critical Periods: Organogenesis (wk 3-8) most sensitive.
- < wk 3: "All-or-none" effect.
-
wk 8: Growth/functional issues.
- Dose-Response: ↑ dose → ↑ effect.
- Genetic Susceptibility: Modifies risk.
- Mechanisms: e.g., impaired cell migration, apoptosis.
- Critical Periods: Organogenesis (wk 3-8) most sensitive.
- Examples (Anomaly: Cause / Teratogen):
- NTDs (Anencephaly, Spina Bifida): Failed neural tube closure (wk 3-4) / Folate deficiency, Valproate.
⭐ Folic acid (0.4 mg/day) preconceptionally & early pregnancy drastically ↓ NTD risk.
- CHDs (VSD, ASD, ToF): Faulty heart development (wk 3-8) / Rubella, Lithium, maternal diabetes.
- Limb Defects (Phocomelia): Disrupted limb bud (wk 4-8) / Thalidomide.
- Cleft Lip/Palate: Failed facial fusion (wk 5-12) / Anticonvulsants, smoking.
- NTDs (Anencephaly, Spina Bifida): Failed neural tube closure (wk 3-4) / Folate deficiency, Valproate.

High-Yield Points - ⚡ Biggest Takeaways
- Teratogens cause defects, most critical during organogenesis (3-8 weeks).
- Key TORCH infections are major infectious teratogens.
- Folic acid deficiency strongly linked to Neural Tube Defects (NTDs).
- Maternal alcohol (FAS) & drugs (e.g., thalidomide, valproate) are potent teratogens.
- Chromosomal abnormalities (e.g., Trisomy 21) & single gene defects are key genetic causes.
- Multifactorial inheritance underlies anomalies like cleft lip/palate.
- Anomalies: Malformations, Disruptions, Deformations, Dysplasias.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

