Regional Anesthesia Anatomy: Foundations - Nerve Navigators' Map
- Nerve Layers:
- Epineurium: Tough outer connective tissue sheath.
- Perineurium: Surrounds nerve fascicles; primary diffusion barrier for LAs.
- Endoneurium: Within fascicles, surrounds individual axons.
- Fascial Planes: Connective tissue layers guiding LA spread; crucial for plane blocks.
- Neurovascular Bundles: Nerves, arteries, veins often travel together; aspiration essential to avoid intravascular injection.
- Anatomical Variation: Common; necessitates careful technique, often ultrasound-guided.
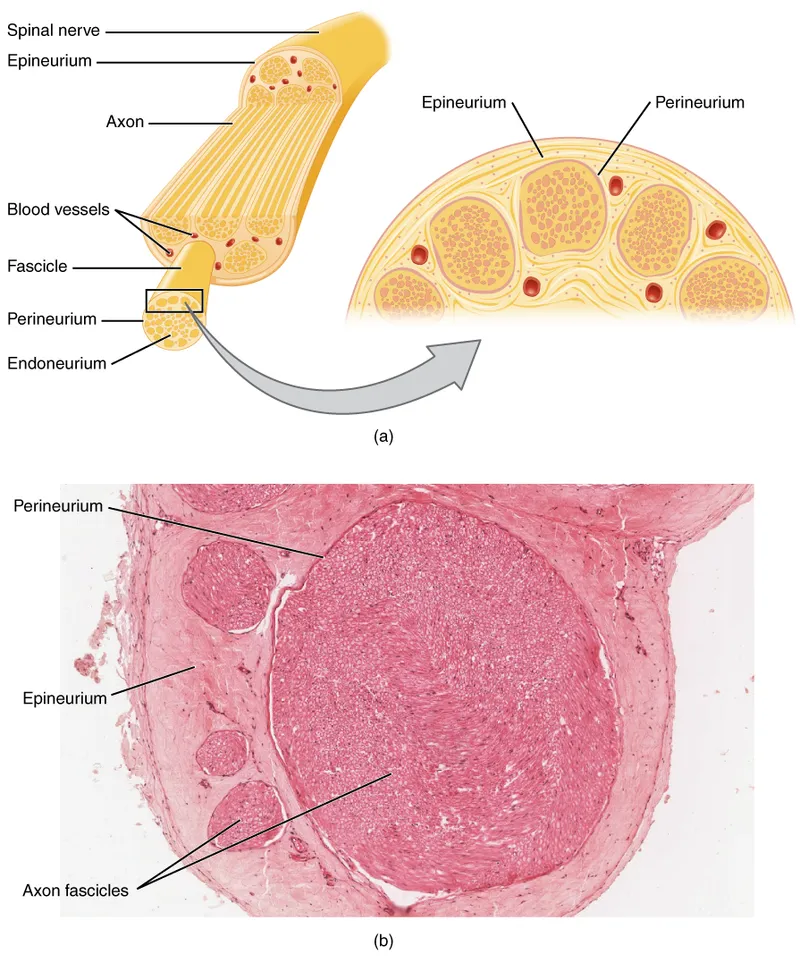
⭐ The perineurium is the principal barrier to local anesthetic diffusion into the nerve fiber, significantly influencing onset time and block quality.
Regional Anesthesia Anatomy: Upper Limb Blocks - Arm's Reach Relief
- Brachial Plexus (C5-T1): Foundation for upper limb sensation/motor function. 📌 RTDCB: Read That Damn Cadaver Book. Key nerves: Musculocutaneous, Axillary, Radial, Median, Ulnar (📌 MARMU).
- Common Blocks & Primary Coverage:
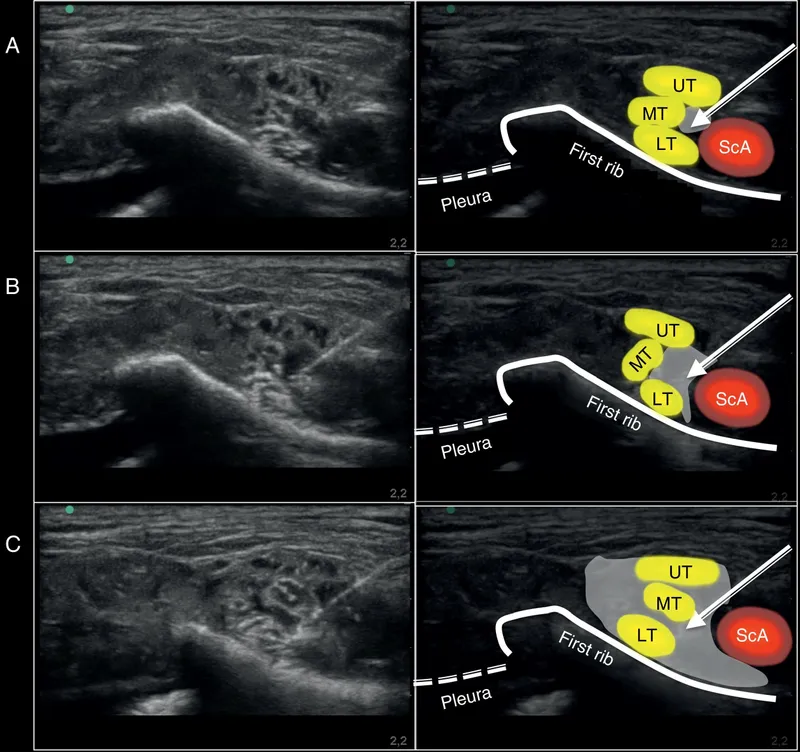
- Interscalene: Targets trunks/roots. For shoulder, clavicle, lateral arm.
- Supraclavicular: Targets divisions/trunks. "Spinal of the arm" - dense block for arm, forearm, hand.
- Infraclavicular: Targets cords. For elbow, forearm, hand; phrenic sparing.
- Axillary: Targets terminal branches. For forearm, hand. Often requires separate musculocutaneous block.
- Ultrasound guidance is standard for visualizing nerves, needle, and local anesthetic spread, enhancing safety.
⭐ Phrenic nerve palsy (ipsilateral diaphragmatic paresis) is a common (~100% transiently) complication of interscalene block due to proximity of phrenic nerve (C3,C4,C5 roots).

Regional Anesthesia Anatomy: Lower Limb Blocks - Leg Up On Pain
- Lumbar Plexus (L1-L4):
- Key Nerves: Femoral, Lateral Femoral Cutaneous (LFCN), Obturator.
- Femoral Nerve Block: Anterior thigh, knee, medial leg/foot (saphenous).
- 📌 Mnemonic (Lumbar Plexus): "I Invariably Get Lazy On Fridays" (Iliohypogastric, Ilioinguinal, Genitofemoral, LFCN, Obturator, Femoral).

⭐ Femoral nerve is lateral to the femoral artery (VAN: Vein-Artery-Nerve from medial to lateral in femoral triangle).
- Sciatic Nerve (L4-S3):
- Branches: Tibial & Common Peroneal.
- Innervates: Posterior thigh, most of leg & foot.
- Popliteal Block: Sciatic nerve at popliteal fossa.

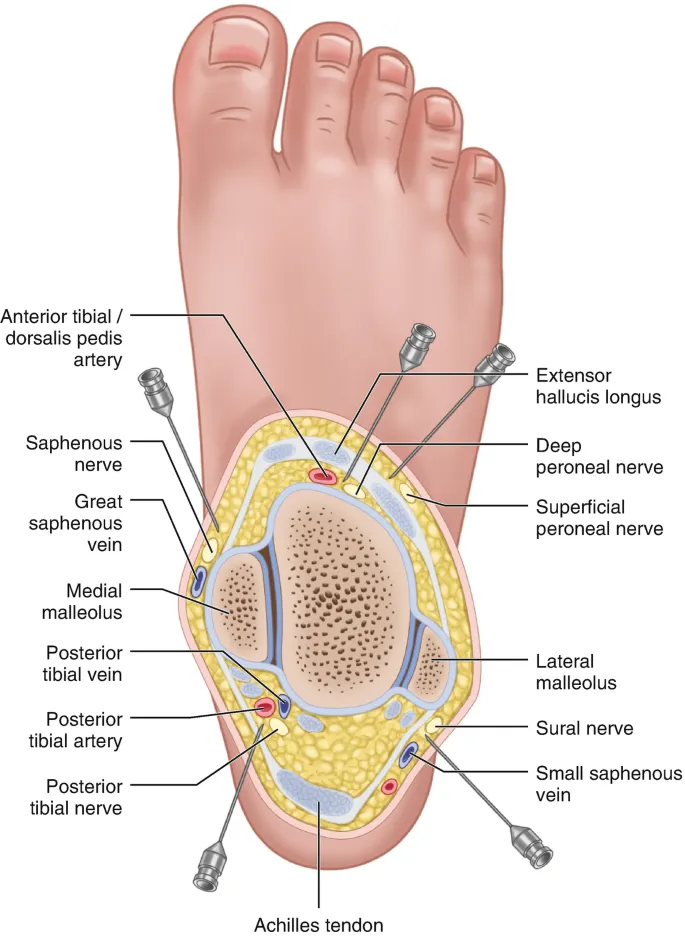
- Ankle Block:
- Nerves: Saphenous, Sural, Deep Peroneal, Superficial Peroneal, Posterior Tibial.
- Targets all sensory innervation to the foot.
Regional Anesthesia Anatomy: Axial & Truncal Blocks - Core Comfort Zone
- Central Neuraxial Blocks (CNB):
- Targets epidural/subarachnoid space.
- 📌 Layers (midline): Skin → Subcutaneous → Supraspinous lig. → Interspinous lig. → Ligamentum flavum → Epidural space → Dura → Arachnoid → Subarachnoid space.
- Site: Below conus medullaris (L1-L2 adults, L3 kids); dural sac to S2.
- Dermatomes: T4 (C-section), T6 (umbilicus), T10 (lower limb).

- Truncal Blocks (e.g., TAP):
- TAP Block: Targets T6-L1 nerves between internal oblique & transversus abdominis.

⭐ The conus medullaris typically ends at L1-L2 in adults; spinal needles are inserted below this level, usually at L3-L4 or L4-L5 interspace.
Regional Anesthesia Anatomy: High‑Yield Points - ⚡ Biggest Takeaways
- Brachial Plexus: Interscalene (roots/trunks); Supraclavicular (trunks/divisions, highest pneumothorax risk); Infraclavicular (cords); Axillary (terminal nerves).
- Lower Limb Nerves: Femoral (L2-L4, anterior thigh); Sciatic (L4-S3, posterior thigh/leg/foot).
- Neuraxial Blocks: Spinal in subarachnoid space (below L1-L2 adult cord); Epidural in epidural space (landmark: ligamentum flavum).
- Interscalene Block: High phrenic nerve palsy risk; often spares ulnar nerve.
- TAP Block: Abdominal wall analgesia; between internal oblique & transversus abdominis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

