Introduction to Variations - What Lurks Beneath
- Variation: Common deviation from typical anatomy; often asymptomatic.
- Anomaly: Significant congenital structural defect; functional impact likely. Rarer.
- Embryological Basis: Errors in morphogenesis (e.g., differentiation, migration, apoptosis).
- Types of Anomalies:
- Agenesis: No organ.
- Aplasia: Primordium present, no development.
- Hypoplasia: Underdeveloped organ.
- Dysplasia: Disorganized cells/tissues.
- Duplication: Extra organ/part.
- Ectopia: Misplaced organ.
- Atresia: No normal opening.
- Stenosis: Narrowed passage.
📌 Mnemonic (Key Types): All Animals Have Distinct Ears (Agenesis, Aplasia, Hypoplasia, Dysplasia, Ectopia).
⭐ Anatomical variations are far more common than true anomalies and often discovered incidentally during surgery or imaging.
System-Specific Variations - Danger Zones Unveiled
| System | Variation | Surgical Implication/Risk |
|---|---|---|
| Vascular | Cystic Artery (Calot's Δ) | Injury in cholecystectomy (e.g., Moynihan's hump). 📌 Calot's Δ: Boundaries - Cystic Duct, CHD, Inf. Liver Border. Contents: Cystic A., Lund's Node. |
| Aberrant Renal Arteries | Bleeding/ischemia in renal surgery/transplant. | |
| Arteria Lusoria (Aberrant R. Subclavian A.) | Dysphagia Lusoria; injury in thoracic/esophageal surgery. | |
| Biliary | Biliary Duct Variations (accessory/aberrant) | Bile duct injury/leak post-cholecystectomy/liver resection. |
| Nervous | Recurrent Laryngeal N. (RLN) Variations | Voice change post-thyroidectomy (esp. non-recurrent RLN on R. with aberrant subclavian a.). |
| GI | Meckel's Diverticulum (Rule of 2s) | Bleeding, obstruction, perforation; often missed. |
| Urogenital | Horseshoe Kidney | Injury to isthmus/aberrant vessels (aortic/renal surgery); ↑ Ureteropelvic Junction (UPJ) obstruction. |
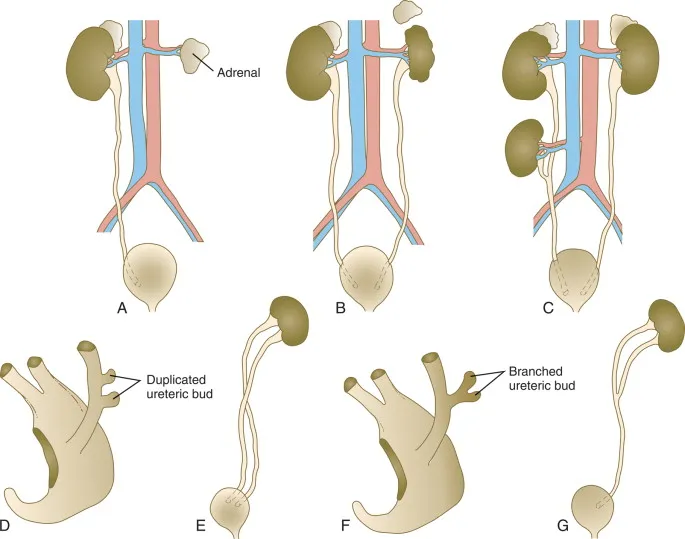
| Duplicated Ureter (Weigert-Meyer rule) | Injury during pelvic surgery; complications like reflux/obstruction. |
בוודאי, הנה התוכן המבוקש בפורמט JSON:
{
"markdown": "## System-Specific Variations - Danger Zones Unveiled\n\n| System | Variation | Surgical Implication/Risk |\n|------------|-------------------------------------------------|--------------------------------------------------------------------------------------------------------|\n| Vascular | Cystic Artery (Calot's Δ) | Injury in cholecystectomy (e.g., Moynihan's hump). 📌 Calot's Δ: Boundaries - Cystic Duct, CHD, Inf. Liver Border. Contents: Cystic A., Lund's Node. |\n| | Aberrant Renal Arteries | Bleeding/ischemia in renal surgery/transplant. |\n| | Arteria Lusoria (Aberrant R. Subclavian A.) | Dysphagia Lusoria; injury in thoracic/esophageal surgery. |\n| Biliary | Biliary Duct Variations (accessory/aberrant) | Bile duct injury/leak post-cholecystectomy/liver resection. |\n| Nervous | Recurrent Laryngeal N. (RLN) Variations | Voice change post-thyroidectomy (esp. non-recurrent RLN on R. with aberrant subclavian a.). |\n| GI | Meckel's Diverticulum (Rule of **2s**) | Bleeding, obstruction, perforation; often missed. |\n| Urogenital | Horseshoe Kidney | Injury to isthmus/aberrant vessels (aortic/renal surgery); ↑ Ureteropelvic Junction (UPJ) obstruction. |\n| | Duplicated Ureter (Weigert-Meyer rule) | Injury during pelvic surgery; complications like reflux/obstruction. |\n\n> ⭐ Cystic artery variations (e.g., Moynihan's hump - tortuous right hepatic or cystic artery crossing anterior to the common hepatic duct) are a major cause of iatrogenic injury during cholecystectomy.\n\n(image)[b5b665cc-811f-4ec0-aa26-2e744bff1326]"
}
Preoperative & Intraoperative Strategies - Navigating the Maze
- Preoperative Detection: Key for surgical planning.
- Advanced Imaging: CT (angio), MRI (e.g., MRCP for biliary tree), Angiography (vascular mapping), USG (Doppler for vessels).
- Intraoperative Identification: Vigilance & meticulous technique.
- Careful dissection: Layer-by-layer, identify structures before division.
- Specific maneuvers: Kocher (mobilize duodenum/pancreas), Pringle (control hepatic inflow), Intraoperative Cholangiography (IOC) for biliary anatomy.
- General Surgical Principles:
- Constant awareness of potential variations.
- Modify techniques based on findings.
- Prioritize safety: Convert to open if variant anatomy poses risk.
⭐ Routine identification of the recurrent laryngeal nerve is crucial in thyroid surgery to prevent voice changes, irrespective of its typical or variant course.
High‑Yield Points - ⚡ Biggest Takeaways
- Aberrant vessels (e.g., hepatic/cystic arteries) risk iatrogenic bleeding or ischemia.
- Nerve variations (e.g., recurrent laryngeal) increase post-op deficits like hoarseness.
- Anomalous biliary anatomy (e.g., cystic duct insertion) heightens bile duct injury risk.
- Organ positional variations (e.g., horseshoe kidney) demand altered surgical access.
- Accessory structures (e.g., accessory spleen) can lead to failed surgery if unaddressed.
- Situs inversus necessitates mirror-image surgical planning and execution.
- Pre-op imaging is key to identify variations, reducing intraoperative complications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

