Autoimmune Diseases — Flashcards

_____ amyloidosis is characterized by systemic deposition of AA amyloid, which is derived from serum amyloid-associated protein (SAA)
Deficiency of _____ protein causes autoimmune polyendocrine syndrome-1
_____ are involved in the recognition and clearance of necrotic cells.
_____ is a IHC marker seen with Breast carcinoma, urothelial carcinoma, salivary duct carcinoma and choriocarcinoma
PTLD has a variety of symptoms; ranging from symptoms that resemble _____ to malignancy induced dysfunction of the transplanted organ
The most common antibodies associated with TRALI are those that bind particularly _____ antigens
_____ amyloidosis is characterized by systemic deposition of AL amyloid, which is derived from Ig light chain
Biopsy for IgG4 disease will demonstrate dense _____ infiltrate
LE cell is a phagocytic _____ or _____ that has engulfed the denatured nucleus of an injured cell
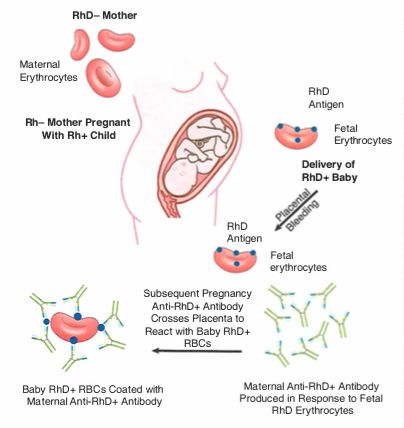
--- Do with heme --- Type II Hypersensitivity Disorders - Cytotoxic: Transfusion Reaction - Antibody against _____ - IgM isohemagglutinins formed naturally in response to bacterial flora cause opsonization and complement activation - Leads to hemolysis **Hemolytic Disease of the Newborn (Erythroblastosis fetalis) Antibody = _____ - Formed in _____ mother carrying _____ child - First pregnancy _____ (doesn't have to be viable pregnancy) - Antibody crosses placenta and injures subsequent fetuses - Prevent with _____ (anti-Rh, binds fetal red cells and prevents mothers immune system from reacting) ABO blood typing and screening for other preformed Abs; always done in case of transplants. Universal donor: type _____ Universal recipient: type _____ (Ex) Type A can donate to _____ and _____. Type A can receive donations from _____ and _____. - Anti-B antibodies prevent donation from type B and type AB. HLA Typing - Microcytotoxicity test Tests for MHC _____ Test hundreds of different haplotypes to find a potential match. Cells recognized by antibody will be attacked by complement and thus become leaky and take up dye. HLA Typing - Mixed lymphocyte reaction Tests for MHC class _____ Take donor cells and irradiate them (prevent proliferation). Irradiated cells are mixed with donor cells to see if proliferation occurs. Higher radioactivity (thymidine) signifies _____ compatibility.
Autoimmune Diseases Flashcards for NEET-PG
Study 10 flashcards on Autoimmune Diseases for NEET-PG Pathology. These active recall cards cover the key concepts, clinical associations, and high-yield facts from this chapter of Immunopathology. Each card is designed to test your understanding rather than just recognition, building stronger and more durable memories for exam day.
For personalised spaced repetition scheduling and unlimited flashcards, download the Oncourse app.
Frequently Asked Questions
Are Autoimmune Diseases flashcards free?
How many flashcards does this chapter have?
How should I use these flashcards for NEET-PG?
Are there more flashcards for Immunopathology?
Want unlimited flashcards?
Get full access to all flashcards, spaced repetition, and progress tracking.
Start For Free