Neurology — Flashcards

On this page
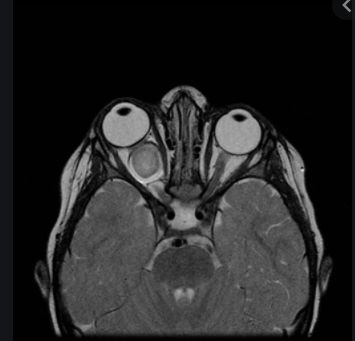
Optic nerve glioma (15–40%), a pilocytic astrocytoma, is commonly seen in _____
Hint: inherited condition
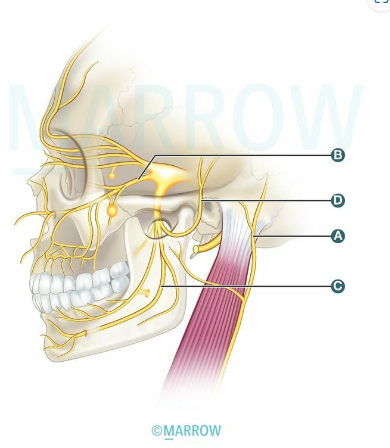
_____ nerve marked as "D" is involved in Frey's syndrome
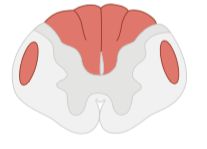
What disease is associated with this spinal cord lesion? _____
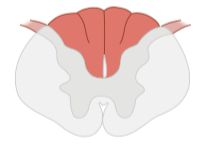
What disease is associated with this spinal cord lesion? _____
_____ is most affected in neurolathyrism
jerky steps are seen in _____ stage of neurolathyrism
Reversible dementia may occur with deficiencies in vitamins _____, B3, and B12
Internuclear ophthalmoplegia results in _____ of the contra-lateral eye
_____ and Breast cancers can produce anti-Yo antibodies which can cause Paraneoplastic Cerebellar Degeneration
Carpal tunnel syndrome is associated with - _____ (due to edema)- rheumatoid arthritis- hypothyroidism- diabetes mellitus- acromegaly- dialysis-related amyloidosis. It may also be associated with repetitive use
Hint: reproductive circumstance
Study by Chapter
Cerebrovascular Diseases
Flashcards
Seizure Disorders and Epilepsy
Flashcards
Headache Disorders
Flashcards
Movement Disorders
Flashcards
Demyelinating Diseases
Flashcards
Neurodegenerative Disorders
Flashcards
Neuromuscular Junction Disorders
Flashcards
Peripheral Neuropathies
Flashcards
CNS Infections
Flashcards
Neuro-oncology
Flashcards
Dementia and Cognitive Disorders
Flashcards
Neurological Emergencies
Flashcards
About Neurology Flashcards for NEET-PG
These Neurology flashcards are designed for NEET-PG Internal Medicine preparation, using active recall to help you retain high-yield concepts, clinical correlations, and commonly tested facts. Each card prompts you to retrieve information from memory rather than passively reviewing notes, which research shows leads to significantly better exam performance.
The 207 cards in this deck cover the most important topics in Neurology, including key mechanisms, diagnostic criteria, treatment protocols, and clinical pearls that frequently appear in NEET-PG examinations. Cards are organised by chapter so you can focus on specific areas or work through the entire topic systematically.
For personalised spaced repetition scheduling that adapts to your performance, unlimited flashcards, and detailed progress analytics, download the Oncourse app.
Frequently Asked Questions
Are Neurology flashcards free on Oncourse?
How do flashcards help with NEET-PG preparation?
How many Neurology flashcards are available?
Can I study Neurology flashcards by chapter?
What topics do these Internal Medicine flashcards cover?
Want unlimited flashcards?
Get full access to all flashcards, spaced repetition, and progress tracking.
Start For Free