Gastroenterology — Flashcards

On this page
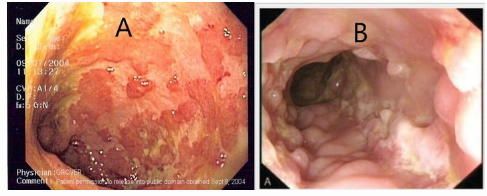
A- _____- Continuous involvement B - _____ - Cobblestone appearence
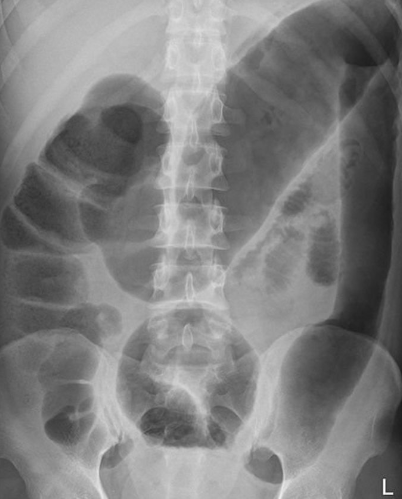
Toxic megacolon is defined as the dilatation of the transverse colon to a diameter of more than _____ cm
Discriminant function (DF), also known as _____ score is calculated using prothrombin time and bilirubin level
Ulcerative colitis always involves the _____ and can extend proximally up to the cecum
One cause of vitamin _____ deficiency is (SIBO) small intestinal bacterial overgrowth
In high resolution esophageal manometry, pressure sensors are no more than _____ cm apart and are upto 36 in number
_____ is the presence of gallstones in the common bile duct, often leading to elevated ALP, GGT, direct bilirubin, and/or AST/ALT
Zollinger-Ellison syndrome is characterized by acid hypersecretion, causing recurrent _____ in the duodenum and jejunum
Physiological test for pancreatic _____ocrine insufficiency is done using a test meal, called as Lundh test
Hint: end/ex
The first line mx of short bowel syndrome is the use of _____ and bile acid sequesterants
Study by Chapter
Esophageal Disorders
Flashcards
Peptic Ulcer Disease
Flashcards
Inflammatory Bowel Disease
Flashcards
Irritable Bowel Syndrome
Flashcards
Malabsorption Syndromes
Flashcards
Pancreatitis (Acute and Chronic)
Flashcards
Gastrointestinal Bleeding
Flashcards
Liver Diseases and Cirrhosis
Flashcards
Viral Hepatitis
Flashcards
Biliary Tract Disorders
Flashcards
Gastrointestinal Motility Disorders
Flashcards
Gastrointestinal Malignancies
Flashcards
About Gastroenterology Flashcards for NEET-PG
These Gastroenterology flashcards are designed for NEET-PG Internal Medicine preparation, using active recall to help you retain high-yield concepts, clinical correlations, and commonly tested facts. Each card prompts you to retrieve information from memory rather than passively reviewing notes, which research shows leads to significantly better exam performance.
The 211 cards in this deck cover the most important topics in Gastroenterology, including key mechanisms, diagnostic criteria, treatment protocols, and clinical pearls that frequently appear in NEET-PG examinations. Cards are organised by chapter so you can focus on specific areas or work through the entire topic systematically.
For personalised spaced repetition scheduling that adapts to your performance, unlimited flashcards, and detailed progress analytics, download the Oncourse app.
Frequently Asked Questions
Are Gastroenterology flashcards free on Oncourse?
How do flashcards help with NEET-PG preparation?
How many Gastroenterology flashcards are available?
Can I study Gastroenterology flashcards by chapter?
What topics do these Internal Medicine flashcards cover?
Want unlimited flashcards?
Get full access to all flashcards, spaced repetition, and progress tracking.
Start For Free