Back
How to Study Respiratory Medicine for NEET PG 2026: High-Yield Topics, TB, COPD, ILD and Exam Checklist
Master NEET PG respiratory medicine with this comprehensive 2026 study guide covering TB, COPD, asthma, ILD, pleural effusion and high-yield exam topics with proven study strategies.

How to Study Respiratory Medicine for NEET PG 2026: High-Yield Topics, TB, COPD, ILD and Exam Checklist
You are probably staring at your respiratory medicine syllabus wondering where to even start. Here's the reality: NEET PG 2026 will test you on 8-12 respiratory questions out of 200 total. That's roughly 4-6% of your exam score riding on how well you know TB drug regimens, COPD staging, and ILD patterns.
Most students make the mistake of treating respiratory as "just another system" and spread their time equally across all topics. Wrong move. NEET PG respiratory has clear high-yield areas that repeat every year. Master these 7 core topics and you will nail 80% of respiratory questions: TB (all forms), COPD staging and management, asthma phenotypes, ILD classification, pleural effusion causes, lung cancer differentials, and pneumonia patterns.
This guide breaks down exactly how to study respiratory medicine for NEET PG 2026. No fluff, just the strategy that works.
Understanding NEET PG Respiratory Medicine Weightage
Respiratory medicine consistently appears with 8-12 questions in NEET PG. The National Board of Examinations focuses heavily on clinical scenarios rather than basic physiology. Here's what the data shows from recent exams:
Topic | Question Frequency | Weightage |
|---|---|---|
Tuberculosis (all forms) | 3-4 questions | 35% |
COPD & Asthma | 2-3 questions | 25% |
Interstitial Lung Disease | 1-2 questions | 15% |
Pleural Effusion | 1-2 questions | 15% |
Pneumonia & Infections | 1 question | 10% |
TB dominates respiratory questions. Master TB and you have secured one-third of respiratory marks. The key insight: NEET PG tests TB in every possible form — pulmonary, extrapulmonary, drug-resistant, and complications.
High-Yield Respiratory Topics for NEET PG 2026
1. Tuberculosis Mastery Framework
TB appears in 3-4 questions every year. You need to know TB inside out:
Pulmonary TB patterns:
Classic upper lobe involvement with cavitation
Primary vs. secondary TB presentations
TB-HIV coinfection patterns
Miliary TB chest X-ray findings
Extrapulmonary TB hotspots:
CNS TB (meningitis patterns, CSF findings)
Abdominal TB (peritoneal, intestinal)
Skeletal TB (Pott's spine, joints)
Genitourinary TB
Drug regimens you must memorize:
RIPE regimen: Rifampicin, Isoniazid, Pyrazinamide, Ethambutol
First-line drug side effects and monitoring
MDR-TB and XDR-TB drug options
Treatment durations for different sites
Pro tip: Oncourse organizes its TB and mycobacterial disease lessons by clinical presentation, making it easier to tackle case-based questions that NEET PG loves.
2. COPD Staging and Management
COPD questions focus on staging, exacerbation management, and spirometry interpretation:
GOLD staging system:
Stage 1: FEV1 ≥80% predicted
Stage 2: 50% ≤ FEV1 <80%
Stage 3: 30% ≤ FEV1 <50%
Stage 4: FEV1 <30%
Exacerbation management:
Mild: Increase bronchodilators
Moderate: Add oral corticosteroids
Severe: Hospitalize, consider NIV
Antibiotic indications in exacerbations
Pharmacotherapy stepwise approach:
Group A: Short-acting bronchodilator
Group B: Long-acting bronchodilator
Group C: LABA + ICS or LAMA
Group D: Triple therapy (LABA + LAMA + ICS)
For quick COPD staging recall, use the mnemonic "8-5-3" for the FEV1 cutoffs (80%, 50%, 30%). This type of clinical decision-making mnemonic is exactly what you'll find in Oncourse's high-yield flashcards for respiratory pharmacology.
3. Asthma Phenotyping and Management
NEET PG tests asthma through clinical scenarios requiring phenotype recognition:
Key asthma phenotypes:
Allergic asthma (early onset, atopic)
Non-allergic asthma (late onset, intrinsic)
Exercise-induced asthma
Aspirin-exacerbated respiratory disease (AERD)
Severe asthma with fungal sensitization
Step therapy approach:
Step 1: Short-acting β2-agonist PRN
Step 2: Low-dose ICS
Step 3: ICS + LABA or medium-dose ICS
Step 4: High-dose ICS + LABA
Step 5: Add omalizumab, mepolizumab, or oral steroids
Acute exacerbation management:
Mild: Increase SABA frequency
Moderate: SABA + oral prednisolone
Severe: SABA + high-dose ICS + systemic steroids
Life-threatening: IV magnesium, consider aminophylline
4. Interstitial Lung Disease Classification
ILD questions test pattern recognition on HRCT and clinical correlation:
Major ILD patterns:
Usual Interstitial Pneumonia (UIP): Honeycombing, basilar
Non-specific Interstitial Pneumonia (NSIP): Ground glass, symmetric
Hypersensitivity pneumonitis: Upper lobe predominance
Sarcoidosis: Hilar lymphadenopathy with reticulonodular pattern
Diagnostic approach:
HRCT chest is the key imaging modality
Bronchoalveolar lavage for cell counts
Transbronchial vs. surgical biopsy indications
Pulmonary function testing patterns
Drug-induced ILD triggers:
Bleomycin, methotrexate, amiodarone
Nitrofurantoin, sulfonamides
Anti-TNF agents
After practicing ILD cases, Oncourse's adaptive weak-area detection will flag whether you struggle more with pattern recognition or drug causality — then create targeted practice sessions accordingly.
5. Pleural Effusion Analysis
Pleural effusion questions revolve around fluid analysis and underlying causes:
Light's criteria for exudate:
Pleural fluid protein/serum protein >0.5
Pleural fluid LDH/serum LDH >0.6
Pleural fluid LDH >2/3 upper limit of normal serum LDH
Transudate causes:
Heart failure (most common)
Hepatic hydrothorax
Nephrotic syndrome
Hypoproteinemia
Exudate causes:
Malignancy (lung, breast, lymphoma)
Pneumonia and parapneumonic effusion
TB pleuritis
Connective tissue disorders
Specific fluid characteristics:
Empyema: pH <7.30, glucose <60 mg/dL
Malignant: Low pH, low glucose, high LDH
TB: Lymphocyte predominance, low glucose
6. Lung Cancer Differential Diagnosis
Lung cancer questions focus on histological subtypes and staging:
Histological types and characteristics:
Adenocarcinoma: Peripheral, glandular pattern, K-RAS mutations
Squamous cell: Central, cavitation common, smoking-related
Small cell: Central, early metastasis, neuroendocrine markers
Large cell: Peripheral, poorly differentiated
Staging basics:
TNM staging system
Small cell: Limited vs. extensive stage
Non-small cell: Stage I-IV with resectability assessment
Treatment approaches:
Stage I-II: Surgical resection
Stage III: Combined chemoradiotherapy
Stage IV: Systemic therapy, targeted agents
Small cell: Chemotherapy regardless of stage
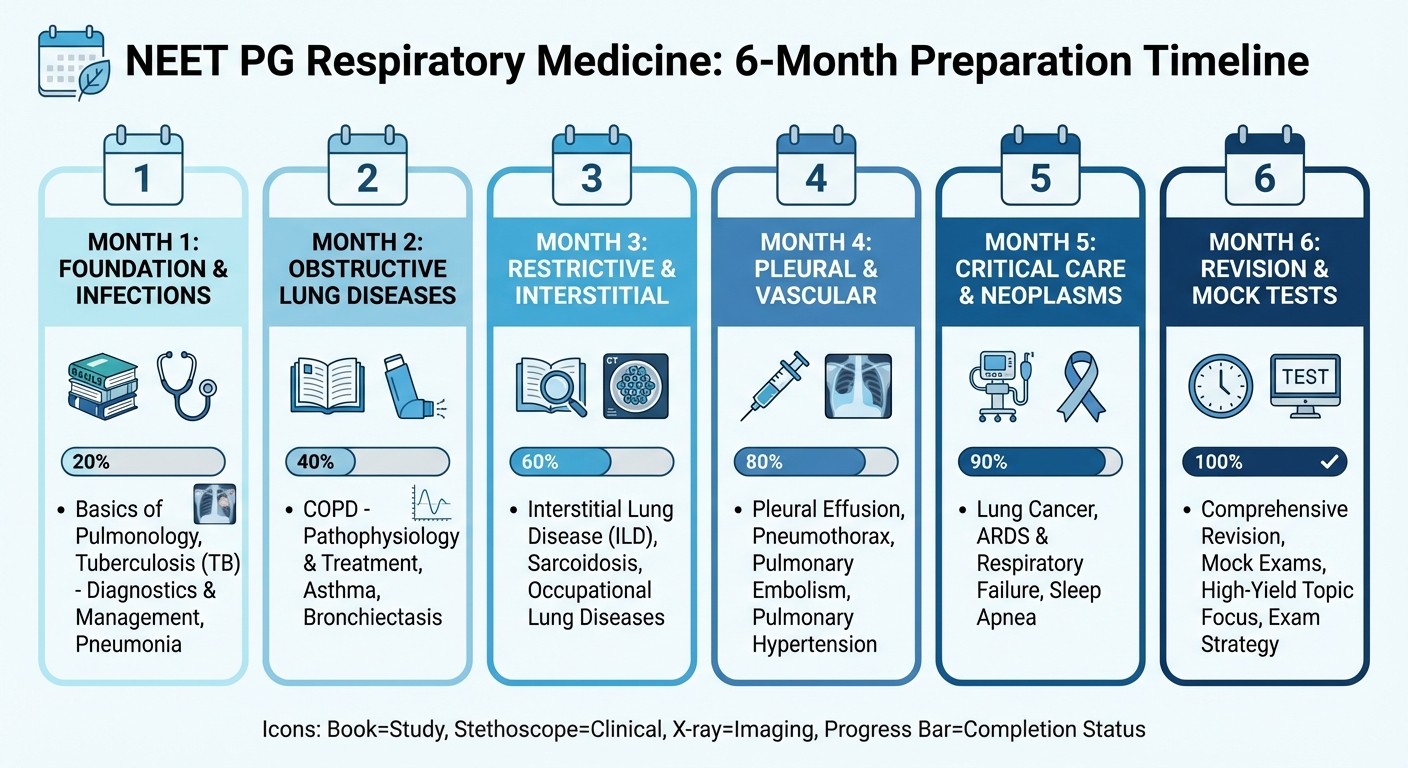
Creating Your NEET PG Respiratory Study Schedule
Month 1-2: Foundation Building
Week 1-2: TB Deep Dive
Complete all TB topic areas: pulmonary, extrapulmonary, drug-resistant
Memorize RIPE regimen and side effects
Practice 50+ TB questions daily using Oncourse's topic-wise question bank — the platform filters questions by specific TB subtopics so you can drill weak areas
Week 3-4: COPD and Asthma
Master GOLD staging criteria
Learn step therapy approaches
Focus on exacerbation management protocols
Month 3-4: Advanced Topics and Integration
Week 1-2: ILD and Pleural Diseases
Study HRCT pattern recognition
Memorize Light's criteria
Practice pleural fluid analysis cases
Week 3-4: Lung Cancer and Infections
Learn histological differentiation
Study pneumonia classification and treatment
Review lung abscess and bronchiectasis
Month 5-6: Intensive Practice and Revision
Daily routine:
30 respiratory MCQs with detailed explanations
Review one high-yield topic daily
Weekly full-length respiratory mock tests
The key is spaced repetition. Instead of cramming all topics in one go, cycle through them weekly. For example, review TB drug regimens using Oncourse's Synapses mnemonics every Monday, COPD staging every Tuesday, and so on.
Essential Mnemonics and Memory Aids
TB Drug Side Effects (RIPE)
Rifampicin: Red-orange discoloration
Isoniazid: Interferes with vitamin B6 (peripheral neuropathy)
Pyrazinamide: Painful joints (hyperuricemia)
Ethambutol: Eyes affected (optic neuritis)
COPD Exacerbation Severity
MINT: Mild (outpatient), Intermediate (oral steroids), Needs hospitalization, Threatening (ICU)
ILD Pattern Recognition
UIP: Under (basilar) In Patches (honeycombing)
NSIP: No Specific Involvement Pattern (diffuse)
Pleural Fluid Analysis
PLEURAL: Protein ratio >0.5, LDH ratio >0.6, LDH >2/3 ULN = Exudate, Under these = transudate, Remember All Light's criteria
These memory aids become second nature with regular practice. Whenever you encounter a tricky scenario question, your brain automatically recalls the mnemonic and guides you to the right answer.
Common NEET PG Respiratory Question Patterns
Pattern 1: TB Case Scenarios
Typical stem: "45-year-old male with 3-month history of evening fever, weight loss, and productive cough. Chest X-ray shows right upper lobe cavitation." What they're testing: TB diagnosis and management Key approach: Identify TB risk factors → imaging pattern → confirm with AFB/GeneXpert → start RIPE regimen
Pattern 2: COPD Staging
Typical stem: "62-year-old smoker with dyspnea on exertion. Spirometry shows FEV1 45% of predicted, FEV1/FVC ratio 0.65." What they're testing: GOLD staging and treatment step Key approach: FEV1% determines stage → stage determines treatment group → match to appropriate therapy
Pattern 3: ILD Pattern Recognition
Typical stem: "55-year-old with progressive dyspnea. HRCT shows honeycombing and traction bronchiectasis with basilar predominance." What they're testing: ILD subtype identification Key approach: HRCT pattern → clinical context → specific ILD diagnosis
Pattern 4: Pleural Effusion Analysis
Typical stem: "Pleural fluid analysis: protein 4.2 g/dL (serum 6.8), LDH 180 U/L (serum 240). What is the next step?" What they're testing: Light's criteria application Key approach: Calculate ratios → transudate vs. exudate → investigate underlying cause
NEET PG Respiratory Medicine Exam Checklist
One Month Before Exam
Must-know drug regimens:
[ ] RIPE regimen for TB (doses and durations)
[ ] COPD step therapy protocol
[ ] Asthma step therapy protocol
[ ] Pneumonia antibiotic choices by pathogen
Must-know criteria and scores:
[ ] Light's criteria for pleural effusion
[ ] GOLD staging for COPD
[ ] TNM staging for lung cancer
[ ] CURB-65 score for pneumonia severity
Must-know imaging patterns:
[ ] TB patterns on chest X-ray and CT
[ ] ILD patterns on HRCT
[ ] Lung cancer appearances by histology
[ ] Pleural effusion on chest X-ray
One Week Before Exam
Final revision topics:
[ ] TB drug resistance patterns and treatment
[ ] COPD exacerbation management algorithm
[ ] Asthma phenotypes and targeted therapy
[ ] ILD diagnostic approach and treatment
Practice focus areas:
[ ] Complete 100+ respiratory MCQs
[ ] Review all incorrect answers
[ ] Time yourself: 45 seconds per question maximum
[ ] Focus on clinical decision-making rather than factual recall
Day Before Exam
Quick review only:
[ ] Skim through mnemonics
[ ] Review drug side effects
[ ] Go through staging criteria one last time
[ ] Get adequate sleep — dont cram new material
Advanced Study Strategies for High Scorers
Integration Across Systems
Respiratory medicine doesnt exist in isolation. NEET PG loves questions that combine respiratory with other systems:
Cardio-pulmonary integration:
Heart failure causing pleural effusion
Pulmonary edema vs. ARDS differentiation
Cor pulmonale secondary to COPD
Rheumatology-respiratory overlap:
SLE causing pleuritis
Rheumatoid arthritis with ILD
Scleroderma pulmonary involvement
Infectious diseases correlation:
HIV-associated respiratory infections
Immunocompromised pneumonia patterns
Post-infectious bronchiectasis
Clinical Correlation Techniques
Instead of memorizing isolated facts, build clinical reasoning:
Case-based learning approach:
1. Present with chief complaint
2. Gather relevant history and examination
3. Order appropriate investigations
4. Interpret results systematically
5. Formulate differential diagnosis
6. Choose best treatment option
Example workflow for dyspnea:
History → smoking, occupational exposure, family history
Examination → clubbing, wheeze, crackles, chest wall deformity
Basic tests → chest X-ray, ABG, spirometry
Advanced tests → HRCT, echocardiography, bronchoscopy
Diagnosis → COPD vs. asthma vs. ILD vs. heart failure
This systematic approach prevents tunnel vision and helps you tackle complex scenario questions confidently.
Question Analysis Strategy
After solving respiratory MCQs, spend equal time analyzing your mistakes:
For incorrect answers:
Why did I choose the wrong option?
What knowledge gap caused the error?
How can I recognize this pattern next time?
For correct answers:
Did I guess or know the answer confidently?
What clues in the stem led me to the right choice?
Are there alternate ways to ask the same concept?
This meta-analysis approach rapidly improves your question-solving accuracy. Track your performance by topic — if you consistently miss TB drug resistance questions, dedicate extra time to that area.
Frequently Asked Questions
How many respiratory questions typically appear in NEET PG?
NEET PG consistently includes 8-12 respiratory medicine questions out of 200 total questions. This represents approximately 4-6% of your total score, making respiratory a moderately weighted subject that deserves focused preparation.
Which respiratory topic has the highest weightage in NEET PG?
Tuberculosis dominates respiratory questions with 3-4 questions every year, representing 35% of respiratory content. Master all forms of TB — pulmonary, extrapulmonary, drug-resistant, and complications — to secure maximum respiratory marks.
How much time should I spend daily on respiratory medicine preparation?
Allocate 45-60 minutes daily to respiratory medicine during your dedicated preparation phase. This should include 30 minutes for topic review and 15-30 minutes for MCQ practice with detailed explanation analysis.
Should I memorize drug doses for NEET PG respiratory topics?
Yes, memorize standard drug regimens and doses for TB (RIPE regimen), COPD exacerbations (prednisolone 30-40mg), and asthma attacks. NEET PG frequently tests specific dosing in clinical scenarios, especially for TB treatment protocols.
What's the best way to remember COPD GOLD staging criteria?
Use the "8-5-3" mnemonic for FEV1 cutoffs: Stage 1 (≥80%), Stage 2 (50-80%), Stage 3 (30-50%), Stage 4 (<30%). Practice spirometry interpretation questions daily to internalize these values through repetition.
How important are chest X-ray and HRCT interpretations for NEET PG?
Imaging interpretation is crucial — about 60% of respiratory questions include chest X-ray or HRCT findings. Focus on classic patterns: TB cavitation, ILD honeycombing, pneumonia consolidation, and pleural effusion appearances.
---
Respiratory medicine rewards systematic preparation over random studying. Master the high-yield topics — TB, COPD, asthma, ILD, and pleural diseases — through active practice and spaced repetition. Build clinical reasoning skills alongside factual knowledge to tackle complex scenario questions confidently.
Remember, respiratory questions in NEET PG test practical clinical decision-making more than theoretical knowledge. Practice systematically, review mistakes thoroughly, and integrate respiratory concepts with other systems for comprehensive understanding.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for NEET PG. Download free on Android and iOS.