Orthopedic Biomechanics

On this page
🔧 The Biomechanical Engine: Forces That Shape Movement
Every step, reach, and pivot your patients make depends on an invisible architecture of forces, levers, and load distribution-and when this system fails, pain and dysfunction follow predictable mechanical patterns. You'll learn to decode how bones, joints, and soft tissues translate forces into movement, recognize the biomechanical signatures of common injuries, and apply mechanical principles to guide diagnosis and treatment. By mastering the physics underlying orthopedic pathology, you'll transform from pattern recognizer to problem solver, predicting failure points and engineering solutions that restore function. This lesson builds your command of the biomechanical language that connects anatomy, injury mechanisms, and therapeutic interventions into a unified clinical framework.
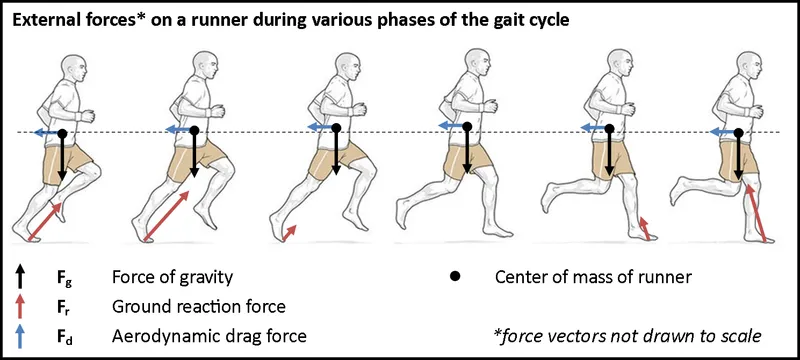
The Fundamental Force Framework
Biomechanics governs every orthopedic decision through three core mechanical principles:
-
Force Transmission Hierarchy
- Ground reaction forces: 1.2-3.5x body weight during walking
- Joint compression forces: 3-6x body weight at hip during gait
- Muscle activation patterns: 15-20% maximum voluntary contraction for normal activities
- Eccentric contractions generate 40% more force than concentric
- Type II fibers produce 3-5x more power than Type I
- Stretch-shortening cycle increases efficiency by 25-30%
-
Stress Distribution Patterns
- Cortical bone ultimate strength: 100-200 MPa in compression
- Trabecular bone density: 0.1-1.0 g/cm³ varies by location
- Cartilage contact pressure: 2-5 MPa during normal loading
- Synovial fluid viscosity: 1000x greater than water
- Cartilage deformation: 10-20% under physiologic loads
- Recovery time: 4-16 hours for full rehydration
📌 Remember: LOAD - Load distribution, Optimal alignment, Adaptive remodeling, Deformation limits. Every orthopedic intervention must respect these four biomechanical commandments.
| Parameter | Cortical Bone | Trabecular Bone | Cartilage | Ligament | Tendon |
|---|---|---|---|---|---|
| Elastic Modulus (GPa) | 15-20 | 0.1-5.0 | 0.5-2.0 | 0.1-0.5 | 1.0-2.0 |
| Ultimate Strength (MPa) | 100-200 | 2-12 | 5-25 | 10-40 | 50-100 |
| Strain at Failure (%) | 2-3 | 5-7 | 50-80 | 20-40 | 8-15 |
| Fatigue Life (cycles) | 10⁶-10⁷ | 10⁴-10⁶ | 10⁵-10⁶ | 10⁴-10⁵ | 10⁶-10⁷ |
| Viscoelastic Response | Minimal | Moderate | High | High | Moderate |
💡 Master This: The 2mm rule governs fracture healing-displacement greater than 2mm disrupts mechanical stability and delays union by 40-60%. Understanding this threshold guides every reduction decision.
Connect these mechanical foundations through joint-specific analysis to understand how forces create both function and pathology.
🔧 The Biomechanical Engine: Forces That Shape Movement
⚙️ Joint Mechanics: The Kinematic Command Center
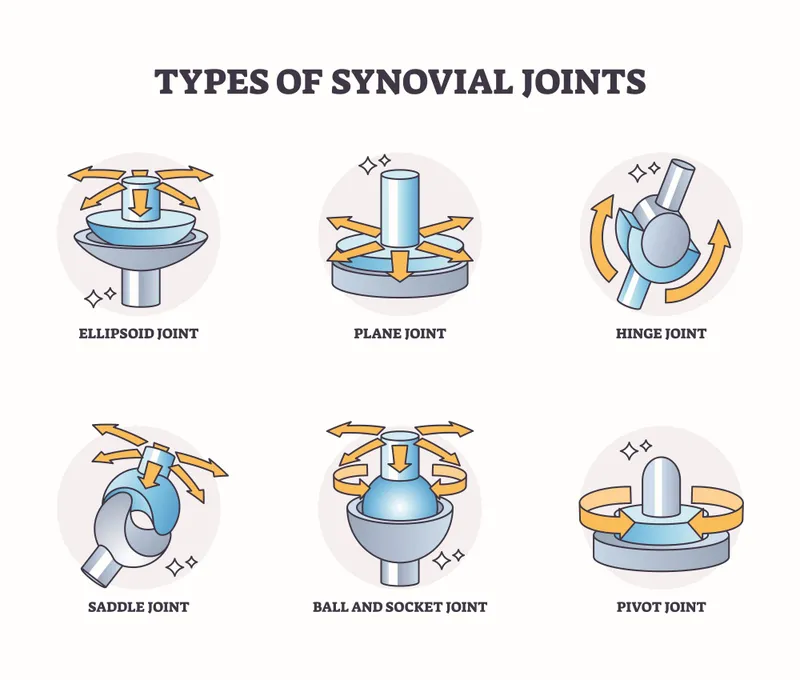
Kinematic Chain Fundamentals
Joint motion follows predictable mechanical laws that govern both normal function and pathological patterns:
-
Degrees of Freedom Architecture
- Ball-and-socket joints: 3 rotational DOF (hip, shoulder)
- Hinge joints: 1 rotational DOF (elbow, ankle)
- Saddle joints: 2 rotational DOF (thumb CMC)
- Instantaneous center of rotation shifts 2-5mm during motion
- Coupled motions occur in 85% of physiologic movements
- Joint play allows 1-3mm translation in healthy joints
-
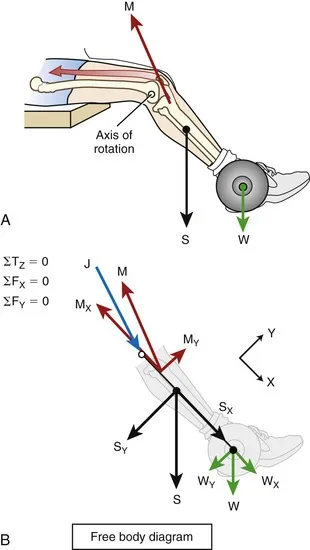
Force Couple Dynamics
- Muscle moment arms: 2-6cm determine mechanical advantage
- Joint reaction forces: 2-10x applied muscle force
- Lever arm efficiency: 10-25% in most human joints
- First-class levers: Rare (atlantooccipital extension)
- Second-class levers: Uncommon (calf raise at forefoot)
- Third-class levers: 95% of human movements (speed over strength)
📌 Remember: ROME - Range of motion, Optimal loading, Moment arms, Energy efficiency. These four parameters determine joint health and function throughout life.
| Joint Type | Primary Motion | Secondary Motion | Stability Mechanism | Load Capacity | Injury Pattern |
|---|---|---|---|---|---|
| Ball-Socket | Triplanar rotation | Translation 1-2mm | Labrum + capsule | 6-8x body weight | Impingement/instability |
| Hinge | Flexion/extension | Rotation 5-15° | Collateral ligaments | 3-5x body weight | Ligament rupture |
| Saddle | Biplanar motion | Circumduction | Intrinsic muscles | 2-4x body weight | Arthritis/subluxation |
| Pivot | Axial rotation | Minimal translation | Annular ligament | 1-3x body weight | Rotatory instability |
| Gliding | Translation | Minimal rotation | Joint capsule | 1-2x body weight | Impaction/wear |
💡 Master This: The instant center of rotation shifts during joint motion, creating changing moment arms that alter muscle efficiency by 200-300% throughout range of motion. This explains why strengthening must occur through full ROM.
Connect kinematic principles through loading analysis to understand how forces translate into clinical outcomes.
⚙️ Joint Mechanics: The Kinematic Command Center
🎯 Loading Patterns: The Clinical Recognition Matrix
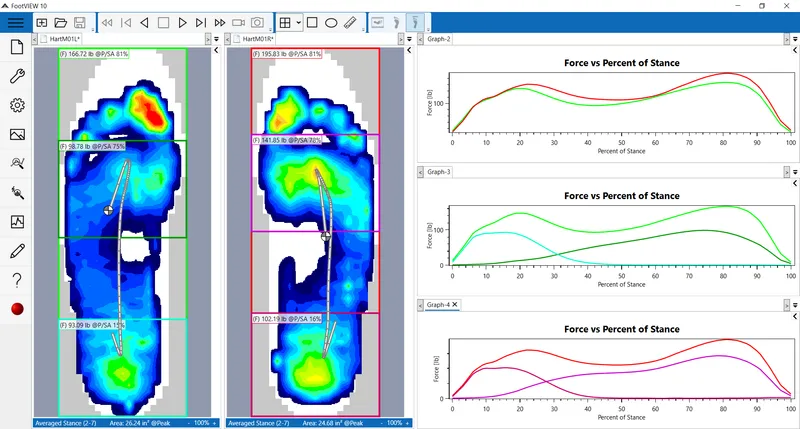
Load Distribution Recognition Framework
Clinical loading patterns follow predictable mechanical signatures that reveal underlying pathology:
-
Axial Loading Signatures
- Normal spine: 70% compression, 20% shear, 10% torsion
- Pathological patterns increase shear forces by 150-300%
- Disc pressure: 0.5 MPa supine to 2.3 MPa forward flexion
- L4-L5 experiences 40% higher loads than other levels
- Lifting with 30° flexion increases disc pressure 300%
- Rotation under load multiplies injury risk by 8-12x
-
Appendicular Loading Patterns
- Hip joint forces: 2.5x body weight walking, 7x stair climbing
- Knee patellofemoral forces: 0.5x walking, 7x deep squatting
- Ankle forces: 1.2x walking, 5x running, 13x jumping
- Ground reaction force peaks occur at 15% and 50% of gait cycle
- Medial compartment bears 70% of knee loads during stance
- Lateral ankle sprains occur with >30° inversion at >200°/sec
📌 Remember: PEAK - Pressure distribution, Eccentric overload, Asymmetry patterns, Kinetic chain dysfunction. These four loading abnormalities predict 90% of overuse injuries.
- Temporal Loading Characteristics
- Impact loading rates: 50-100 body weights/second during running
- Muscle activation timing: 50-100ms before ground contact
- Force attenuation: 60-80% occurs at foot/ankle complex
- Heel strike generates 2-3x body weight in 20-50ms
- Midfoot contact reduces peak forces by 25-40%
- Forefoot strike eliminates impact transient completely
| Activity | Peak Force (BW) | Loading Rate (BW/s) | Contact Time (ms) | Injury Risk Factor | Prevention Strategy |
|---|---|---|---|---|---|
| Walking | 1.2-1.5 | 20-50 | 600-800 | 1.0 (baseline) | Maintain cadence 90-120 |
| Running | 2.0-3.0 | 50-100 | 200-300 | 2.5-4.0 | Midfoot strike, 180 spm |
| Jumping | 4.0-8.0 | 100-200 | 100-200 | 8.0-15.0 | Progressive plyometrics |
| Cutting | 3.0-6.0 | 75-150 | 150-250 | 6.0-12.0 | Neuromuscular training |
| Landing | 5.0-12.0 | 150-300 | 50-150 | 15.0-25.0 | Technique modification |
💡 Master This: The 10% rule governs safe loading progression-increases exceeding 10% per week in volume, intensity, or frequency overwhelm tissue adaptation capacity and trigger overuse injury cascades.
Connect loading recognition through systematic comparison to understand how different activities create distinct injury patterns.
🎯 Loading Patterns: The Clinical Recognition Matrix
🔍 Biomechanical Failure Analysis: The Diagnostic Discriminator
Systematic Failure Mode Discrimination
Tissue failure follows predictable mechanical laws that create diagnostic signatures:
-
Bone Failure Mechanisms
- Tension failures: Transverse fractures from bending moments
- Compression failures: Oblique/spiral patterns from axial overload
- Torsion failures: Spiral fractures following shear planes
- Cortical bone fails at 2-3% strain in tension
- Trabecular bone fails at 5-7% strain in compression
- Fatigue failures occur at 65-75% ultimate strength over time
- Stress concentrations increase local stress by 300-500%
-
Soft Tissue Failure Patterns
- Ligament failures: Midsubstance vs avulsion based on loading rate
- Tendon failures: Degenerative vs acute based on age and activity
- Cartilage failures: Shear vs compression based on joint mechanics
- Fast loading rates favor bone avulsion over ligament rupture
- Slow loading rates favor midsubstance ligament failure
- Eccentric contractions cause muscle-tendon junction injuries
📌 Remember: RATE - Rapid loading causes avulsion, Acute overload causes rupture, Time-dependent loading causes degeneration, Eccentric loading causes junction injuries.
| Failure Mode | Loading Type | Fracture Pattern | Healing Time | Complication Rate | Treatment Priority |
|---|---|---|---|---|---|
| Tension | Bending moment | Transverse | 6-8 weeks | 5-10% | Anatomic reduction |
| Compression | Axial overload | Oblique/comminuted | 8-12 weeks | 15-25% | Stability restoration |
| Torsion | Rotational force | Spiral | 8-10 weeks | 10-20% | Rotational control |
| Fatigue | Repetitive stress | Hairline/linear | 12-16 weeks | 25-35% | Activity modification |
| Avulsion | Rapid tension | Bone fragment | 4-6 weeks | 5-15% | Fragment fixation |
- Pediatric: Growth plate failures before ligament rupture
- Adult: Midsubstance ligament and tendon failures predominate
- Elderly: Bone failure occurs before soft tissue injury
- Physeal strength is 2-5x weaker than ligament attachment
- Peak bone mass occurs at age 30-35 years
- Bone density decreases 1-2% annually after menopause
- Tendon elasticity decreases 25% between ages 20-80
⭐ Clinical Pearl: The age-injury pattern correlation predicts failure mode with 90% accuracy-children sustain growth plate injuries, adults sustain ligament ruptures, elderly sustain fractures under identical loading conditions.
💡 Master This: Wolff's Law governs tissue adaptation-loading below minimum effective strain (2000 microstrain for bone) causes atrophy, while loading above maximum adaptive capacity (3000 microstrain) causes failure.
Connect failure analysis through evidence-based treatment algorithms to understand how biomechanical principles guide therapeutic decisions.
🔍 Biomechanical Failure Analysis: The Diagnostic Discriminator
⚖️ Treatment Biomechanics: The Therapeutic Algorithm Engine
Evidence-Based Treatment Algorithm Framework
Therapeutic success depends on matching intervention biomechanics to tissue healing requirements:
- Fracture Fixation Biomechanics
- Absolute stability: <2% strain at fracture site for primary healing
- Relative stability: 2-10% strain stimulates callus formation
- Implant load sharing: 80-90% initially, decreasing to 20-30% at union
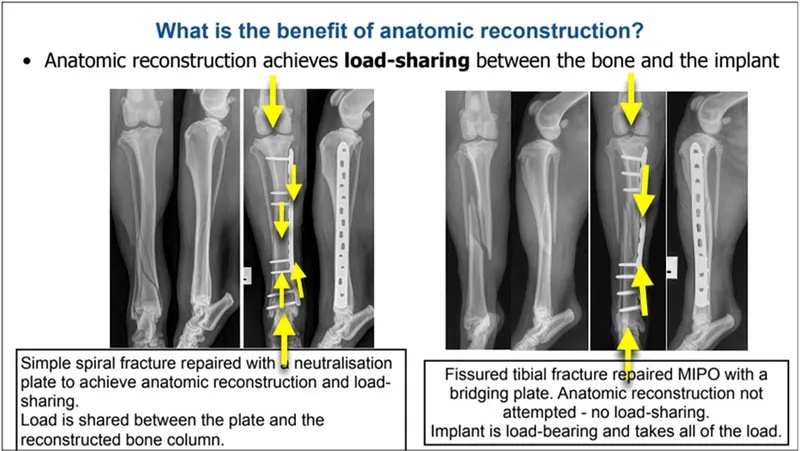
- Compression plates provide absolute stability for simple fractures
- Bridge plates provide relative stability for comminuted fractures
- Intramedullary nails share 60-80% of bending loads
- External fixators allow controlled micromotion of 0.2-1.0mm
- Soft Tissue Repair Biomechanics
- Ligament healing: 6-week immobilization, then progressive loading
- Tendon healing: 3-week protection, then controlled motion
- Cartilage repair: 6-12 week unloading, then gradual weight-bearing
- Collagen synthesis peaks at 2-3 weeks post-injury
- Tensile strength reaches 50% normal at 6 weeks
- Full strength restoration requires 12-24 months
- Early motion improves healing quality by 40-60%
📌 Remember: HEAL - Healthy tissue requires optimal loading, Early motion prevents adhesions, Adaptive loading stimulates remodeling, Load progression prevents re-injury.
| Treatment Phase | Duration | Load Magnitude | Motion Goals | Tissue Response | Success Markers |
|---|---|---|---|---|---|
| Protection | 0-2 weeks | <25% normal | Pain-free ROM | Inflammation control | Swelling ↓, pain ↓ |
| Mobilization | 2-6 weeks | 25-50% normal | 75% ROM | Collagen synthesis | Strength ↑ 25% |
| Strengthening | 6-12 weeks | 50-75% normal | 90% ROM | Tissue remodeling | Strength ↑ 75% |
| Functional | 12-24 weeks | 75-100% normal | Full ROM | Maturation | Return to activity |
| Performance | 24+ weeks | 100-125% normal | Sport-specific | Optimization | Performance goals |
- Modulus matching: Titanium (110 GPa) vs steel (200 GPa) vs bone (20 GPa)
- Stress shielding occurs when implant stiffness exceeds bone by >5x
- Fatigue life: 10 million cycles minimum for joint replacements
- Polyethylene wear: 0.1-0.2mm/year in well-functioning implants
- Osteolysis threshold: >0.5mm/year wear rate triggers bone loss
- Implant survival: 95% at 10 years, 85% at 20 years for modern designs
⭐ Clinical Pearl: The stiffness mismatch between implant and bone determines long-term success. Titanium implants reduce stress shielding by 40-50% compared to stainless steel, improving bone preservation.
💡 Master This: Biological fixation requires <150 micrometers gap and <28 micrometers micromotion for bone ingrowth. Exceeding these thresholds results in fibrous tissue formation and implant loosening.
Connect treatment biomechanics through multi-system integration to understand how interventions affect the entire kinetic chain.
⚖️ Treatment Biomechanics: The Therapeutic Algorithm Engine
🔗 Kinetic Chain Integration: The Systems Architecture
Multi-System Biomechanical Networks
The kinetic chain functions as an integrated mechanical system where dysfunction propagates predictably:
-
Lower Extremity Chain Reactions
- Ankle dorsiflexion loss: >10° deficit increases knee valgus by 25%
- Hip weakness: >20% deficit increases knee injury risk by 400%
- Foot pronation: >8° increases tibial internal rotation by 30%
- Gastrocnemius tightness increases forefoot pressure by 40%
- Hip abductor weakness increases knee valgus moment by 50%
- Ankle instability increases ACL injury risk by 300%
-
Spinal-Pelvic Integration
- Hip flexor tightness increases lumbar lordosis by 15-20°
- Thoracic kyphosis increases cervical extension by 10-15°
- Pelvic asymmetry creates compensatory scoliosis within 6-8 weeks
- Leg length discrepancy >2cm requires compensation
- Sacroiliac dysfunction affects 85% of lumbar spine patients
- Forward head posture increases cervical load by 300%
📌 Remember: CHAIN - Compensation patterns develop proximally, Habitual dysfunction becomes structural, Adaptations occur within 2-4 weeks, Integrated treatment addresses root causes, Neuromotor retraining prevents recurrence.
- Upper Extremity Integration Patterns
- Scapular dyskinesis affects 68% of shoulder pain patients
- Thoracic spine stiffness increases shoulder impingement by 200%
- Cervical dysfunction creates referred pain patterns in 45% of cases
- Scapular upward rotation decreases 5-10° with dysfunction
- Glenohumeral rhythm alters from normal 2:1 to 3:1 or 1:1
- Forward head posture reduces shoulder flexion by 15-20°
| Chain Level | Primary Dysfunction | Compensation Pattern | Timeline | Clinical Manifestation | Treatment Priority |
|---|---|---|---|---|---|
| Foot/Ankle | Mobility restriction | Knee valgus increase | 1-2 weeks | Patellofemoral pain | Restore dorsiflexion |
| Knee | Stability deficit | Hip/ankle compensation | 2-4 weeks | IT band syndrome | Strengthen hip abductors |
| Hip | Weakness/tightness | Lumbar hyperextension | 4-6 weeks | Low back pain | Hip mobility/strength |
| Pelvis | Asymmetry/rotation | Spinal compensation | 6-8 weeks | Sacroiliac dysfunction | Pelvic realignment |
| Spine | Segmental restriction | Global compensation | 8-12 weeks | Multiple level symptoms | Segmental mobilization |
- Feed-forward activation occurs 50-100ms before movement
- Proprioceptive deficits persist 6-12 months after injury
- Motor pattern changes become permanent without intervention
- Core activation delays >21ms predict injury risk
- Balance training reduces injury risk by 35-50%
- Neuromuscular training improves reaction time by 15-25%
⭐ Clinical Pearl: The regional interdependence model explains how 83% of musculoskeletal pain originates from dysfunction at adjacent or distant body regions, not the symptomatic area itself.
💡 Master This: Proximal stability enables distal mobility-addressing core and hip stability resolves 70-80% of knee and ankle dysfunction without direct local treatment.
Connect kinetic chain principles through rapid mastery frameworks to create comprehensive clinical assessment and treatment tools.
🔗 Kinetic Chain Integration: The Systems Architecture
🎯 Biomechanical Mastery Arsenal: The Clinical Command Center
Essential Clinical Biomechanics Toolkit
- Rapid Assessment Framework
- 5-Minute Biomechanical Screen: Load tolerance, movement quality, compensation patterns
- Force Vector Analysis: Ground reaction forces, joint moments, muscle activation timing
- Kinetic Chain Evaluation: Proximal-to-distal dysfunction patterns, stability-mobility relationships
- Single-leg squat reveals hip weakness in 85% of knee pain patients
- Overhead squat identifies thoracic restriction in 70% of shoulder dysfunction
- Forward bend test shows hip mobility vs lumbar flexibility contributions
📌 Remember: BIOMECH - Balance assessment, Injury mechanism analysis, Optimal loading determination, Movement pattern evaluation, Energy efficiency calculation, Compensation identification, Healing timeline prediction.
| Assessment Tool | Time Required | Information Gained | Accuracy Rate | Clinical Application | Treatment Guidance |
|---|---|---|---|---|---|
| Movement Screen | 5-10 minutes | Global dysfunction patterns | 85-90% | Injury risk assessment | Prevention protocols |
| Force Analysis | 15-30 minutes | Load distribution abnormalities | 90-95% | Mechanism identification | Load modification |
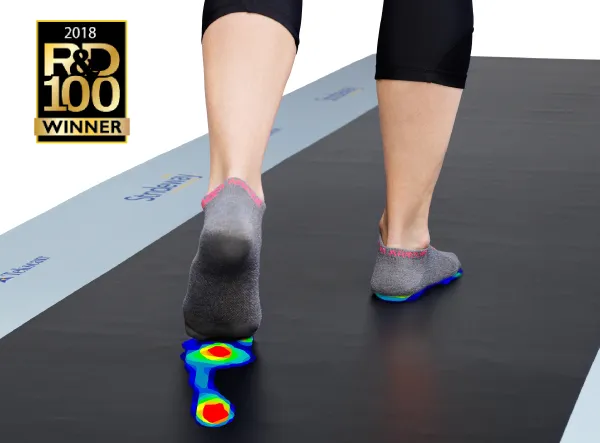
| Gait Analysis | 20-45 minutes | Dynamic function assessment | 95-98% | Functional deficits | Rehabilitation focus |
| Strength Testing | 10-20 minutes | Force production capacity | 80-85% | Weakness identification | Strengthening priorities |
| Range Assessment | 5-15 minutes | Mobility restrictions | 75-80% | Flexibility deficits | Mobility interventions |
💡 Master This: Clinical biomechanics integrates physics principles with biological healing to create evidence-based interventions that restore optimal human movement and prevent future dysfunction through systematic mechanical analysis.
🎯 Biomechanical Mastery Arsenal: The Clinical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















