Foot and Ankle Surgery

On this page
🏗️ Foot and Ankle Surgery: The Foundation Architecture
The foot and ankle form a remarkable 26-bone architectural system that bears your entire body weight while enabling complex motion from simple walking to athletic performance. You'll master how this foundation's anatomy translates into biomechanics, learn to recognize pathology patterns through systematic clinical detective work, and build the diagnostic and surgical decision frameworks that separate routine cases from complex reconstructions. This lesson transforms isolated facts into an integrated clinical reasoning system, equipping you to evaluate any foot or ankle complaint with the precision of an engineer and the insight of a master clinician.
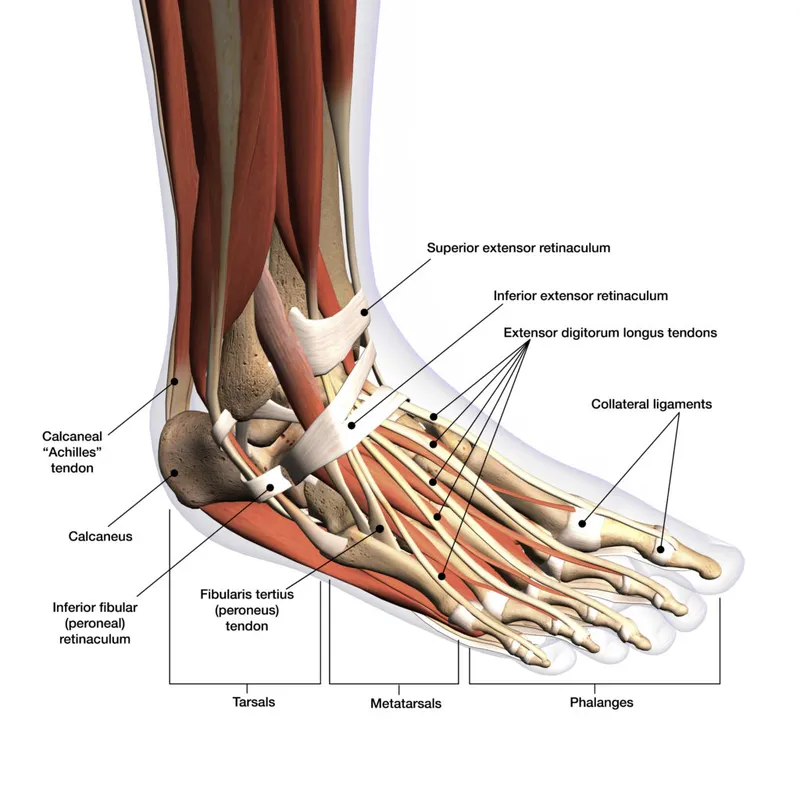
The foot functions as three integrated units: the hindfoot (talus and calcaneus), midfoot (navicular, cuboid, and cuneiforms), and forefoot (metatarsals and phalanges). This tripartite division guides surgical approaches and determines weight-bearing restrictions post-operatively.
📌 Remember: "Some Lovers Try Positions That They Cannot Handle" - Scaphoid, Lunate, Triquetrum, Pisiform, Trapezium, Trapezoid, Capitate, Hamate (carpal bones) - but for foot: "Tiger Cubs Need Meat In Every Meal" - Talus, Calcaneus, Navicular, Medial/Middle/Lateral cuneiforms, Metatarsals
The ankle joint proper involves three bones forming a mortise-and-tenon configuration. The tibial plafond and fibular malleolus create a socket receiving the talar dome. Normal ankle dorsiflexion ranges 15-20° while plantarflexion achieves 45-50°. Surgical restoration must preserve these ranges to prevent compensatory deformities.
- Hindfoot Joints
- Tibiotalar (ankle): 15-20° dorsiflexion, 45-50° plantarflexion
- Subtalar: 30° inversion, 15° eversion
- Critical for uneven terrain adaptation
- 85% of hindfoot motion occurs here
- Midfoot Joints
- Talonavicular: Primary midfoot motion center
- Calcaneocuboid: Lateral column stability
- Combined motion: 15° dorsiflexion/plantarflexion
- 7° inversion/eversion capability
- Forefoot Joints
- Metatarsophalangeal: 70° dorsiflexion required for push-off
- Interphalangeal: 30° dorsiflexion for toe clearance
| Joint Complex | Primary Motion | Range (Degrees) | Clinical Significance | Surgical Priority |
|---|---|---|---|---|
| Tibiotalar | Sagittal plane | 65° total arc | Weight acceptance | Highest |
| Subtalar | Triplanar | 45° total arc | Terrain adaptation | High |
| Midfoot | Multiplanar | 22° combined | Shock absorption | Moderate |
| MTP Joints | Sagittal | 70° dorsiflexion | Push-off power | Variable |
| IP Joints | Sagittal | 30° dorsiflexion | Toe clearance | Low |
The longitudinal arch system comprises medial, lateral, and transverse components. The medial longitudinal arch bears 80% of body weight and includes the calcaneus, talus, navicular, cuneiforms, and first three metatarsals. Plantar fascia tension provides 60% of arch support, while the posterior tibial tendon contributes 25%.
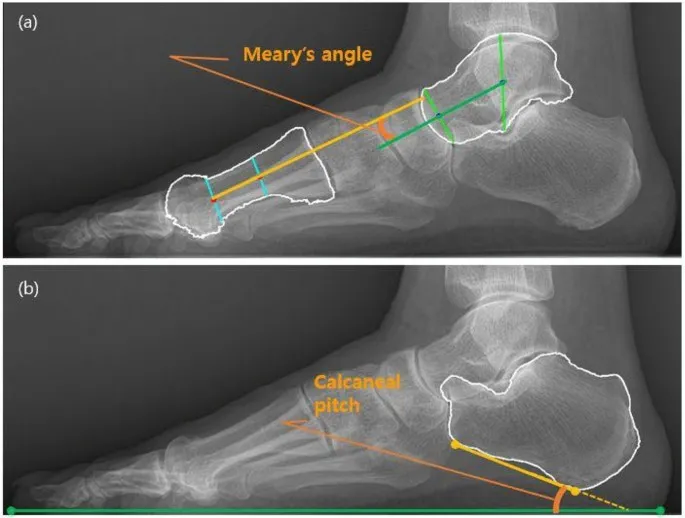
💡 Master This: The Meary's line (talar-first metatarsal angle) should measure 0-4° on lateral radiographs. Values >15° indicate significant flatfoot deformity requiring surgical correction. This single measurement predicts 90% of surgical outcomes in adult acquired flatfoot deformity.
📌 Remember: "LAMP" for lateral ankle ligament complex - Lateral talocalcaneal, ATFL, CFL, PTFL (Anterior talofibular, Calcaneofibular, Posterior talofibular). ATFL tears occur in 85% of ankle sprains, while CFL involvement indicates Grade III injury requiring 6-8 weeks immobilization.
Understanding this foundational architecture enables precise surgical planning where each intervention must preserve or restore the delicate balance between stability and mobility that defines normal foot function.
🏗️ Foot and Ankle Surgery: The Foundation Architecture
⚙️ Biomechanical Engineering: The Motion Mastery System
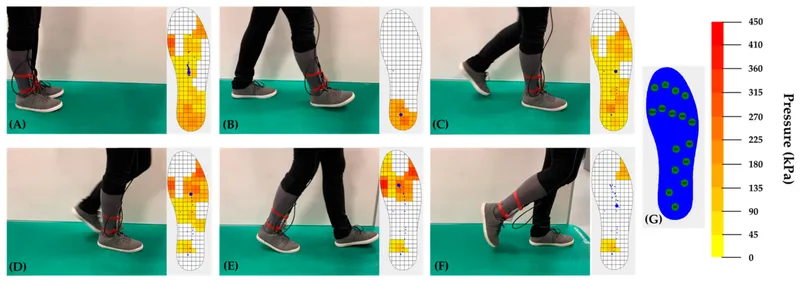
The heel strike phase initiates with the calcaneus contacting the ground at 15-20° of inversion. Ground reaction forces reach 120% of body weight within 50 milliseconds. The subtalar joint immediately begins pronation (eversion, dorsiflexion, abduction) to unlock the midfoot and accommodate terrain irregularities.
📌 Remember: "PAID" for pronation components - Plantarflexion, Adduction, Inversion, Dorsiflexion (actually Plantarflexion, Abduction, Inversion, Dorsiflexion - the mnemonic helps remember the complex triplanar motion where subtalar eversion creates midfoot unlocking)
- Gait Phase Mechanics
- Heel Strike (0-15% of cycle): 120% body weight loading
- Subtalar pronation: 4-6° eversion
- Ankle dorsiflexion: 5° from neutral
- Midstance (15-50% of cycle): 100% body weight sustained
- Maximum pronation: 8-10° total
- Ankle progression: 10° dorsiflexion
- Midfoot unlocking allows 15° total motion
- Heel Rise (50-65% of cycle): 80% body weight transition
- Subtalar supination begins: 2-4° inversion
- Midfoot locking initiates rigid lever
- Push-off (65-100% of cycle): 200% body weight peak
- Maximum supination: 6-8° inversion
- MTP dorsiflexion: 65-70° required
- Ankle plantarflexion: 20-25° for clearance
- Heel Strike (0-15% of cycle): 120% body weight loading
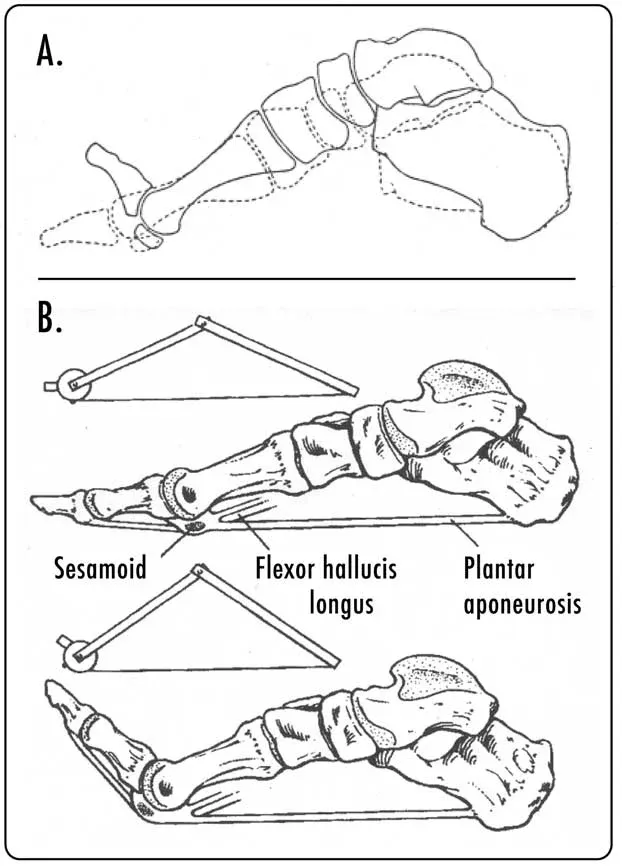
The windlass mechanism represents the foot's most elegant biomechanical feature. During push-off, MTP dorsiflexion tightens the plantar fascia like a windlass, elevating the arch 8-12mm and converting the foot into a rigid lever. This mechanism generates 60% of the foot's propulsive force.
| Biomechanical Phase | Joint Position | Muscle Activity | Force Distribution | Clinical Relevance |
|---|---|---|---|---|
| Heel Strike | Ankle neutral, STJ inverted | Eccentric dorsiflexors | Lateral heel 100% | Calcaneal fractures |
| Foot Flat | Ankle 5° DF, STJ pronating | Isometric stabilizers | Whole foot 80% | Plantar fasciitis |
| Midstance | Ankle 10° DF, STJ pronated | Concentric supinators | Medial forefoot 60% | PTTD progression |
| Heel Rise | Ankle 5° DF, STJ supinating | Concentric plantarflexors | Forefoot 40% | Hallux rigidus |
| Push-off | Ankle 20° PF, STJ supinated | Explosive plantarflexors | Great toe 20% | Sesamoid pathology |
The triple joint complex (subtalar, talonavicular, calcaneocuboid) functions as the foot's universal joint, allowing triplanar motion while maintaining structural integrity. Subtalar axis orientation varies ±15° between individuals, explaining why identical injuries produce different clinical presentations.
💡 Master This: The center of pressure travels from lateral heel to medial forefoot during normal gait, covering 85% of foot length. Abnormal pressure patterns indicate specific pathologies: lateral forefoot pressure suggests cavus deformity, while medial midfoot pressure indicates flatfoot collapse.
Muscle timing coordination requires precise neuromuscular control with ±50 millisecond accuracy. The posterior tibial muscle fires 200 milliseconds before heel strike, pre-tensioning the medial arch. Peroneal muscles activate 150 milliseconds after heel strike to control excessive inversion.
Understanding these biomechanical principles guides surgical decision-making where procedures must restore normal motion patterns while preserving the intricate timing relationships that enable efficient locomotion.
⚙️ Biomechanical Engineering: The Motion Mastery System
🎯 Pattern Recognition Mastery: The Clinical Detective Framework
The pain pattern matrix provides the foundation for rapid diagnosis. Medial ankle pain in patients >50 years suggests posterior tibial tendon dysfunction in 75% of cases. Lateral ankle pain following inversion injury indicates peroneal tendon pathology in 60% of chronic cases.
📌 Remember: "PAIN" location guide - Posterior (Achilles), Anterior (impingement), Inferior (plantar fascia), Navicular (PTTD). Each location has 3-4 primary differentials with specific provocative tests achieving >90% sensitivity.
- Systematic Pain Assessment Framework
- Medial Pain Patterns
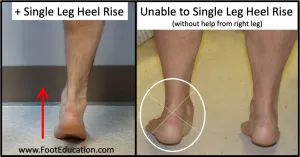
- Posterior tibial tendon: Medial malleolar pain, single heel rise inability
- Tarsal tunnel: Burning/tingling distribution, positive Tinel's sign
- Spring ligament: Plantar medial pain, arch collapse visible
- Lateral Pain Patterns
- Peroneal tendinopathy: Posterior fibular pain, resisted eversion weakness
- Sinus tarsi syndrome: Lateral hindfoot pain, subtalar stiffness
- Cuboid syndrome: Lateral midfoot pain, cuboid mobility loss
- Posterior Pain Patterns
- Achilles tendinopathy: 2-6cm proximal to insertion, morning stiffness
- Haglund's deformity: Posterosuperior heel pain, shoe irritation
- Retrocalcaneal bursitis: Deep posterior pain, dorsiflexion aggravation
- Medial Pain Patterns
The deformity recognition system enables rapid surgical planning. Hallux valgus angles >30° require proximal metatarsal osteotomy in 90% of cases. Hindfoot valgus >15° indicates subtalar arthritis requiring fusion rather than soft tissue reconstruction.
| Clinical Pattern | Key Finding | Diagnostic Test | Sensitivity | Surgical Indication |
|---|---|---|---|---|
| PTTD Stage II | Single heel rise failure | MRI tendon signal | 95% | Tendon reconstruction |
| Ankle impingement | Anterior ankle pain | Forced dorsiflexion | 88% | Arthroscopic debridement |
| Plantar fasciitis | First step pain | Heel tenderness | 92% | Conservative first |
| Achilles rupture | Palpable gap | Thompson test | 96% | Surgical repair |
| Peroneal subluxation | Lateral snapping | Dynamic ultrasound | 85% | Retinacular repair |
Functional assessment patterns reveal surgical urgency. Patients unable to walk 2 blocks or climb 10 stairs without pain demonstrate functional disability requiring surgical intervention in 85% of cases when conservative treatment fails after 6 months.
💡 Master This: The "first ray mobility test" predicts hallux valgus recurrence with 90% accuracy. >8mm of dorsal translation indicates hypermobility requiring Lapidus fusion rather than distal osteotomy to prevent recurrence rates >40%.
Imaging pattern recognition accelerates diagnosis. Talar beaking on lateral radiographs indicates >5 years of ankle arthritis. Subchondral cysts >5mm predict failed conservative treatment in 85% of ankle arthritis cases.
The surgical timing matrix guides intervention decisions. Acute Achilles ruptures within 48 hours achieve 95% excellent outcomes with surgery. Delayed presentation >6 weeks requires augmentation procedures with 20% higher complication rates.
Understanding these recognition patterns enables rapid, accurate diagnosis while avoiding the analysis paralysis that delays appropriate surgical intervention in time-sensitive conditions.
🎯 Pattern Recognition Mastery: The Clinical Detective Framework
🔬 Differential Mastery: The Diagnostic Discrimination Engine
The posterior heel pain differential matrix demonstrates systematic discrimination. Insertional Achilles tendinopathy shows bone marrow edema on MRI in 85% of cases, while non-insertional tendinopathy demonstrates fusiform thickening 2-6cm proximal to insertion in 90% of cases.
📌 Remember: "SHARP" for posterior heel differentials - Sever's disease, Haglund's deformity, Achilles tendinopathy, Retrocalcaneal bursitis, Plantar fasciitis (posterior extension). Each has specific age demographics and imaging signatures with >85% diagnostic accuracy.
- Systematic Posterior Heel Discrimination
- Insertional Achilles Tendinopathy
- Age: >40 years in 75% of cases
- Location: Direct insertion tenderness
- Imaging: Bone marrow edema, calcific deposits
- Treatment response: Poor to conservative care (<30% success)
- Non-insertional Achilles Tendinopathy
- Age: 30-50 years peak incidence
- Location: 2-6cm proximal to insertion
- Imaging: Fusiform thickening, intratendinous signal
- Treatment response: Good to conservative care (70% success)
- Haglund's Deformity
- Age: Young adults with rigid shoes
- Location: Posterosuperior calcaneal prominence
- Imaging: Parallel pitch lines, prominent tuberosity
- Treatment response: Moderate to shoe modification (50% success)
- Insertional Achilles Tendinopathy
The medial ankle pain discrimination system separates posterior tibial tendon dysfunction from tarsal tunnel syndrome using specific provocative tests. PTTD demonstrates inability to perform single heel rise in 95% of Stage II cases, while tarsal tunnel syndrome shows positive Tinel's sign in 80% of cases.
| Condition | Age Peak | Pain Character | Physical Finding | Imaging Hallmark | Conservative Success |
|---|---|---|---|---|---|
| PTTD Stage I | 50-60 years | Activity-related ache | Tendon tenderness | Tendon thickening | 60% |
| PTTD Stage II | 55-65 years | Constant medial pain | Single heel rise failure | Hindfoot valgus | 20% |
| Tarsal Tunnel | 40-50 years | Burning/tingling | Positive Tinel's | Nerve compression | 40% |
| Spring Ligament | 45-55 years | Plantar medial sharp | Arch collapse | Ligament tear | 30% |
| PTT Tenosynovitis | 35-45 years | Swelling/stiffness | Tendon sheath fluid | Fluid around tendon | 70% |
Lateral ankle pain discrimination requires understanding chronic instability patterns. Functional instability demonstrates normal stress radiographs but positive anterior drawer in 70% of cases. Mechanical instability shows >10mm anterior translation on stress views in 85% of cases.
💡 Master This: Peroneal tendon subluxation occurs in 15% of acute ankle sprains but is missed initially in 60% of cases. Dynamic ultrasound during active eversion demonstrates tendon displacement with 90% sensitivity, while static MRI shows normal findings in 40% of cases.
The forefoot pain differential engine distinguishes Morton's neuroma from metatarsalgia using specific compression tests. Mulder's click appears in 85% of neuromas >5mm diameter, while metatarsal squeeze test reproduces metatarsalgia in 90% of cases.
Imaging discrimination protocols provide definitive diagnosis. T2 hyperintensity in posterior tibial tendon indicates >50% fiber disruption requiring surgical reconstruction. Subchondral cysts >5mm in ankle arthritis predict failed conservative treatment in 85% of cases.
Understanding these discrimination frameworks eliminates diagnostic uncertainty and enables confident surgical planning based on evidence-based criteria rather than clinical intuition alone.
🔬 Differential Mastery: The Diagnostic Discrimination Engine
⚖️ Surgical Decision Mastery: The Treatment Algorithm Engine
The hallux valgus algorithm demonstrates evidence-based decision-making. Mild deformities (HVA <30°, IMA <13°) achieve 95% satisfaction with distal osteotomies. Severe deformities (HVA >40°, IMA >20°) require proximal procedures to prevent recurrence rates >40%.
📌 Remember: "MILD, MODERATE, SEVERE" for hallux valgus surgery - Metatarsal head procedures (HVA <30°), Intermediate shaft osteotomies (HVA 30-40°), Lapidus fusion (HVA >40°), Double procedures for severe cases. Recurrence rates increase exponentially with inappropriate procedure selection.
- Hallux Valgus Surgical Algorithm
- Mild Deformity (HVA <30°, IMA <13°)
- Procedure: Chevron/Austin osteotomy
- Success rate: 95% satisfaction at 2 years
- Recurrence: <5% with proper technique
- Return to activity: 6-8 weeks full weight-bearing
- Moderate Deformity (HVA 30-40°, IMA 13-20°)
- Procedure: Scarf/Ludloff osteotomy
- Success rate: 90% satisfaction at 2 years
- Recurrence: 8-12% with adequate correction
- Return to activity: 8-10 weeks protected weight-bearing
- Severe Deformity (HVA >40°, IMA >20°)
- Procedure: Lapidus arthrodesis
- Success rate: 85% satisfaction at 2 years
- Recurrence: <3% with solid fusion
- Return to activity: 12-16 weeks non-weight-bearing
- Mild Deformity (HVA <30°, IMA <13°)
The ankle arthritis treatment algorithm guides intervention timing. Early arthritis with >5° motion and minimal cysts achieves 80% improvement with arthroscopic debridement. End-stage arthritis with <5° motion requires arthrodesis for predictable pain relief in 90% of cases.
| Arthritis Stage | Joint Space | Motion Arc | Cyst Size | Recommended Treatment | Success Rate |
|---|---|---|---|---|---|
| Early | >2mm | >15° | <3mm | Arthroscopic debridement | 80% |
| Moderate | 1-2mm | 5-15° | 3-5mm | Distraction arthroplasty | 70% |
| Severe | <1mm | <5° | >5mm | Ankle arthrodesis | 90% |
| End-stage | Bone-on-bone | 0° | Multiple | Tibiotalocalcaneal fusion | 85% |
| Salvage | Collapse | Fixed deformity | Extensive | Amputation consideration | Variable |
Achilles tendon rupture algorithms depend on timing and patient factors. Acute ruptures within 48 hours in active patients <60 years achieve 95% strength return with surgical repair. Chronic ruptures >6 weeks require augmentation procedures with 20% higher complication rates.
💡 Master This: Posterior tibial tendon dysfunction staging determines surgical approach with 95% accuracy. Stage I (tendinopathy) responds to debridement in 80% of cases. Stage II (deformity) requires reconstruction with 85% success. Stage III (arthritis) needs fusion for predictable outcomes.
The flatfoot reconstruction algorithm considers deformity flexibility. Flexible deformities with >50% correction on heel rise achieve 90% satisfaction with soft tissue procedures. Rigid deformities require bony correction with osteotomies or fusions for reliable outcomes.
Revision surgery algorithms address failed primary procedures. Hallux valgus recurrence with maintained correction suggests soft tissue failure requiring lateral release revision. Loss of correction indicates inadequate bony procedure requiring proximal osteotomy or Lapidus conversion.
Understanding these algorithmic approaches ensures optimal procedure selection based on evidence-based criteria rather than technical familiarity, leading to predictable outcomes and high patient satisfaction rates.
⚖️ Surgical Decision Mastery: The Treatment Algorithm Engine
🌐 Integration Mastery: The Multi-System Orchestration Network
The kinetic chain integration model reveals how foot pathology creates ascending dysfunction. Ankle arthritis with <5° dorsiflexion forces knee hyperextension during midstance, increasing patellofemoral stress by 40% and creating secondary knee pain in 65% of patients within 2 years.
📌 Remember: "CHAIN" for kinetic integration - Calcaneus position affects Hindfoot alignment, Ankle motion influences Intermediate joints, Navicular drop creates forefoot compensation. Each 5° of hindfoot valgus increases forefoot abduction by 3° and medial column stress by 25%.
- Multi-System Integration Patterns
- Hindfoot-Forefoot Coupling
- Hindfoot valgus creates forefoot abduction and first ray elevation
- Ratio: 3:1 forefoot to hindfoot compensation
- Clinical significance: Isolated hindfoot correction fails in 40% without forefoot addressing
- Ankle-Subtalar Interaction
- Ankle arthritis increases subtalar motion by 150% as compensation
- Progression: 65% develop subtalar arthritis within 5 years
- Surgical implication: Isolated ankle fusion creates adjacent joint stress
- Muscle-Tendon Integration
- Posterior tibial dysfunction affects 6 different muscle groups
- Compensation patterns: Peroneal overactivity in 80% of cases
- Treatment requirement: Multi-tendon balancing for optimal outcomes
- Hindfoot-Forefoot Coupling
The deformity progression cascade demonstrates system-wide effects. Adult acquired flatfoot begins with posterior tibial tendon dysfunction but progresses to involve spring ligament failure, subtalar arthritis, and ankle valgus in predictable sequence over 5-10 years.
| Integration Level | Primary Pathology | Secondary Effects | Tertiary Complications | Surgical Complexity |
|---|---|---|---|---|
| Single Joint | Isolated arthritis | Adjacent stiffness | Muscle weakness | Simple |
| Regional | Multi-joint arthritis | Kinetic chain dysfunction | Gait abnormalities | Moderate |
| Systemic | Neuromuscular disease | Global deformity | Functional disability | Complex |
| Compensatory | Failed surgery | Overcorrection | New pain patterns | Revision |
| Degenerative | Age-related changes | Multiple joint involvement | Activity limitation | Salvage |
Neuromuscular integration affects surgical planning in complex deformities. Cerebral palsy patients with spastic equinovarus require multi-level correction addressing gastrocnemius contracture, posterior tibial overactivity, and peroneal weakness simultaneously for functional improvement.
💡 Master This: Charcot foot reconstruction requires understanding diabetes pathophysiology, neuropathic bone changes, and wound healing impairment. Success rates drop from 85% in normal patients to 60% in diabetics due to multi-system involvement requiring specialized protocols.
The surgical timing integration considers multiple factors simultaneously. Adolescent bunion correction must account for growth remaining, family history, activity level, and deformity progression rate to optimize timing and procedure selection for long-term success.
Revision surgery integration addresses failed primary procedures through systematic analysis. Recurrent hallux valgus requires evaluating initial procedure adequacy, healing complications, patient compliance, and biomechanical factors to select appropriate revision strategy.
Understanding multi-system integration enables comprehensive surgical planning that addresses root causes rather than isolated symptoms, leading to durable corrections and improved long-term outcomes through systematic orchestration of all contributing factors.
🌐 Integration Mastery: The Multi-System Orchestration Network
🎯 Clinical Mastery Arsenal: The Rapid-Fire Reference Engine
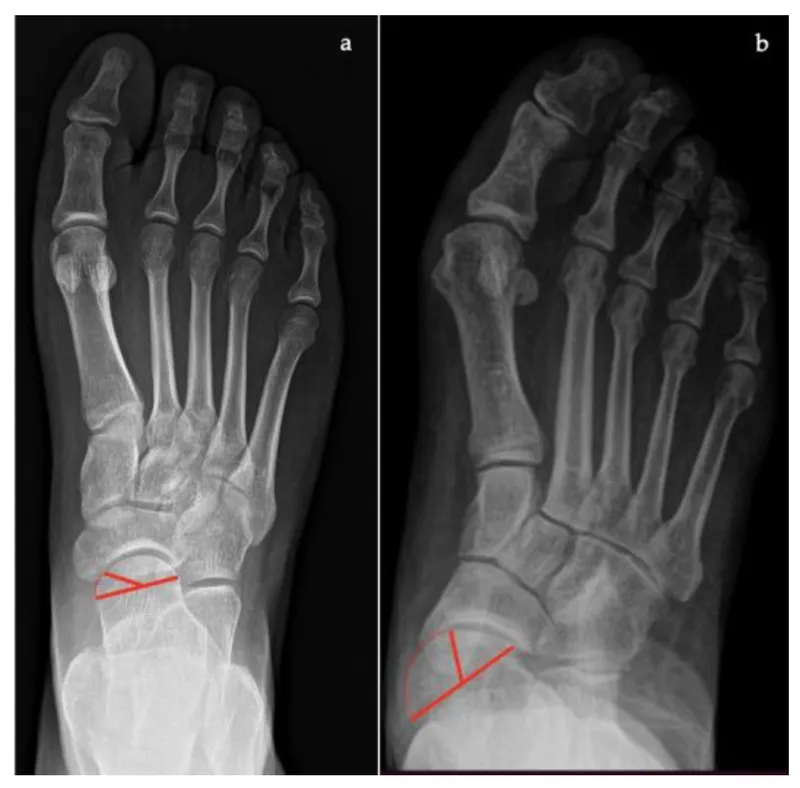
📌 Remember: "ANGLES" for critical measurements - Anterior distal tibial angle (93±2°), Normal calcaneal pitch (20-30°), Great toe hallux valgus (<15°), Lateral distal metatarsal angle (<8°), Expected correction (70-80% of deformity), Subtalar motion (30° inversion, 15° eversion)
- Essential Surgical Thresholds
- Hallux Valgus Correction
- Mild: HVA <30°, IMA <13° → Distal osteotomy
- Moderate: HVA 30-40°, IMA 13-20° → Shaft osteotomy
- Severe: HVA >40°, IMA >20° → Proximal fusion
- Recurrence risk: >40% if undercorrected by >5°
- Flatfoot Reconstruction
- Stage I: Tendinopathy only → Debridement (80% success)
- Stage II: <40% talar uncoverage → Reconstruction (85% success)
- Stage III: Subtalar arthritis → Triple fusion (90% success)
- Stage IV: Ankle valgus → Tibiotalocalcaneal fusion
- Ankle Arthritis Management
- Early: >5° motion, <3mm cysts → Arthroscopy (80% improvement)
- Moderate: 2-5° motion → Distraction (70% improvement)
- Severe: <2° motion → Fusion (90% pain relief)
- Replacement criteria: Age <70, >5° motion, intact ligaments
- Hallux Valgus Correction
| Procedure | Success Rate | Return to Activity | Complication Rate | Revision Rate | Key Predictor |
|---|---|---|---|---|---|
| Chevron Osteotomy | 95% | 6-8 weeks | 5% | 3% | Proper indication |
| Lapidus Fusion | 85% | 12-16 weeks | 15% | 8% | Fusion healing |
| Ankle Arthrodesis | 90% | 16-20 weeks | 20% | 10% | Bone quality |
| Triple Arthrodesis | 85% | 20-24 weeks | 25% | 15% | Alignment correction |
| Achilles Repair | 95% | 12-16 weeks | 10% | 5% | Timing of repair |
Rapid Assessment Protocol for emergency presentations:
- Achilles rupture: Thompson test (96% sensitivity), palpable gap, inability to plantarflex
- Ankle fracture: Ottawa rules (99% sensitivity), weight-bearing ability, bone tenderness
- Compartment syndrome: Pain out of proportion, passive stretch pain, pressure >30mmHg
- Open fracture: Gustilo classification, tetanus status, antibiotic timing (<6 hours)
💡 Master This: First ray mobility predicts hallux valgus recurrence with 90% accuracy. >8mm dorsal translation requires Lapidus fusion rather than osteotomy to prevent recurrence rates >40%. This single test changes surgical approach in 25% of cases.
Critical Complication Avoidance:
- Nerve injury rates: Superficial peroneal (3% in ankle arthroscopy), Sural (2% in lateral approaches), Medial plantar (1% in bunion surgery)
- Nonunion risks: Smoking increases risk 4x, diabetes increases risk 2x, NSAIDs delay healing 30%
- Infection prevention: Antibiotic prophylaxis within 60 minutes, glucose <200mg/dL, normothermia maintenance
Outcome Optimization Factors:
- Patient selection: Realistic expectations (95% satisfaction), compliance (90% success), medical optimization (85% healing)
- Surgical technique: Anatomic reduction (90% outcomes), stable fixation (85% union), soft tissue handling (80% wound healing)
- Postoperative care: Protected weight-bearing (95% union), early motion (90% function), gradual progression (85% return to activity)
This clinical arsenal enables confident decision-making under time pressure while maintaining evidence-based standards that optimize patient outcomes through systematic application of proven principles.
🎯 Clinical Mastery Arsenal: The Rapid-Fire Reference Engine
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























