Computer-Assisted Surgery

On this page
🤖 Computer-Assisted Surgery: The Digital Revolution in Orthopaedics
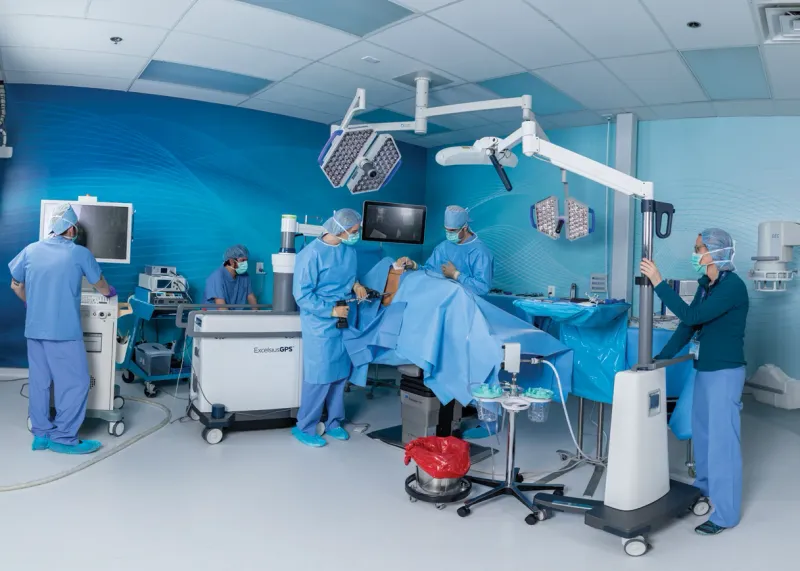
Computer-assisted surgery transforms the operating room into a precision-guided environment where digital intelligence amplifies human expertise. You'll explore how navigation systems function as a surgeon's compass, master their clinical applications across joint replacement and trauma, and compare robotic versus navigation platforms to choose optimal tools for specific cases. We'll examine multi-modal integration strategies, tackle real-world implementation challenges, and peer into the future of AI-enhanced surgical intelligence. This journey equips you to harness technology that measurably improves alignment, reduces complications, and elevates patient outcomes.
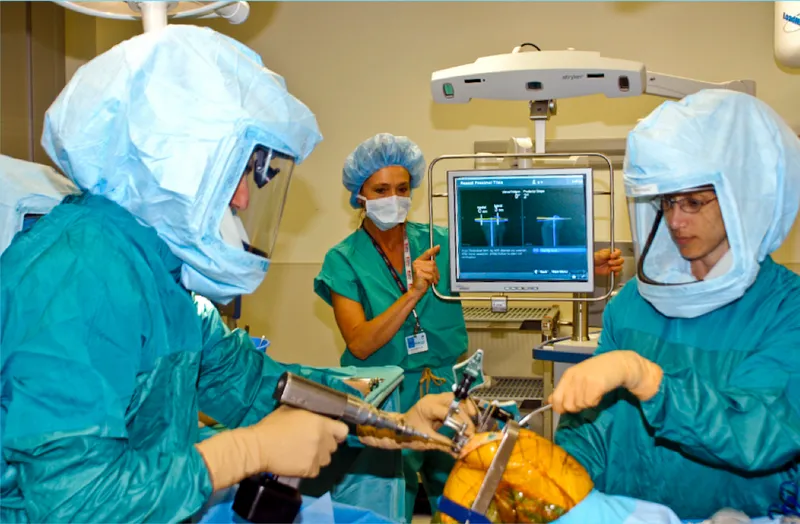
Computer-assisted surgery represents the convergence of imaging technology, computational power, and surgical expertise. Unlike traditional surgery that relies on anatomical landmarks and surgeon experience, CAS provides real-time navigation with sub-millimeter accuracy, transforming complex procedures into precisely guided interventions.
📌 Remember: CAS = Computer + Assisted + Surgery - Digital precision meets surgical expertise for enhanced patient outcomes
The technology encompasses multiple modalities working in seamless integration:
-
Navigation Systems
- Optical tracking with 0.1mm accuracy
- Electromagnetic guidance systems
- Inertial measurement units
- Real-time position feedback
- 360-degree spatial awareness
- Drift compensation algorithms
-
Imaging Integration
- Pre-operative CT/MRI fusion
- Intraoperative fluoroscopy
- 3D reconstruction capabilities
- Volumetric rendering
- Multi-planar visualization
- Virtual surgical planning
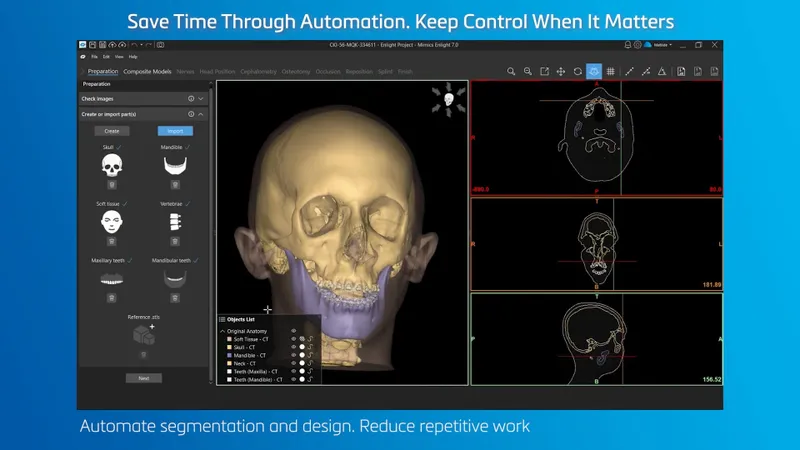
| Technology Type | Accuracy | Setup Time | Cost Factor | Learning Curve | Clinical Applications |
|---|---|---|---|---|---|
| Optical Navigation | ±0.1mm | 15-20 min | High | 6-8 weeks | Spine, Joint Replacement |
| Electromagnetic | ±0.5mm | 5-10 min | Medium | 3-4 weeks | Trauma, Arthroscopy |
| Robotic Systems | ±0.05mm | 25-30 min | Very High | 12-16 weeks | Joint Replacement |
| PSI Templates | ±1.0mm | 2-5 min | Low | 1-2 weeks | Knee/Hip Replacement |
| Fluoroscopy-based | ±2.0mm | 3-7 min | Medium | 2-3 weeks | Trauma Surgery |
The fundamental principle underlying all CAS systems involves spatial registration - the process of correlating virtual anatomical models with actual patient anatomy. This registration achieves accuracy through multiple reference points, typically requiring 4-6 anatomical landmarks for optimal precision.
💡 Master This: Every CAS system depends on accurate registration - master this concept, and you understand why 90% of navigation errors stem from registration problems
Understanding CAS technology unlocks the logic behind modern orthopaedic precision, setting the foundation for exploring specific navigation principles and clinical applications.
🤖 Computer-Assisted Surgery: The Digital Revolution in Orthopaedics
🧭 Navigation Fundamentals: The Surgeon's Digital Compass
![]()
Computer navigation transforms surgical orientation from anatomical estimation to mathematical certainty. The system creates a virtual coordinate system overlaying the patient's anatomy, providing real-time feedback on instrument position and trajectory.
The navigation workflow follows precise sequential steps, each building upon previous accuracy achievements:
-
Image Acquisition Phase
- CT scan with 1mm slice thickness
- MRI sequences for soft tissue definition
- DICOM format standardization
- 512 x 512 pixel resolution minimum
- 16-bit grayscale depth
- Isotropic voxel reconstruction
-
Registration Methodologies
- Point-based registration using anatomical landmarks
- Surface-based registration with 100+ points
- Hybrid techniques combining both approaches
- Accuracy improvement: 40-60%
- Registration time: 8-12 minutes
- Error reduction: 0.5-1.5mm
📌 Remember: TRACK = Tracking + Registration + Accuracy + Calibration + Kinematic feedback - Five pillars of surgical navigation
| Navigation Type | Tracking Method | Workspace | Accuracy | Interference Factors | Setup Complexity |
|---|---|---|---|---|---|
| Optical | Infrared cameras | 2m³ volume | ±0.1mm | Line-of-sight | High |
| Electromagnetic | Magnetic field | 50cm radius | ±0.5mm | Metal objects | Medium |
| Mechanical | Articulated arm | 1.5m reach | ±0.2mm | Physical constraints | Low |
| Inertial | Gyroscopes/accelerometers | Unlimited | ±1.0mm | Drift accumulation | Medium |
| Hybrid | Combined systems | Variable | ±0.05mm | Multiple factors | Very High |
The tracking accuracy depends on multiple technical factors working in precise coordination. Sampling frequency of 20-60 Hz ensures smooth real-time updates, while latency must remain below 50 milliseconds for optimal surgeon feedback.
⭐ Clinical Pearl: Navigation accuracy degrades by 15-25% when tracking volume exceeds optimal range - maintain instruments within 1.2 meters of tracking cameras for best results
Calibration procedures establish the relationship between virtual and physical spaces. Tool calibration requires 5-point verification with accuracy confirmation within ±0.2mm. Patient registration typically involves 6-8 anatomical landmarks for optimal spatial correlation.
💡 Master This: Registration accuracy determines surgical precision - a 1mm registration error translates to 2-3mm surgical deviation at the target site
The navigation interface provides multiple visualization modes: axial, sagittal, and coronal views with real-time instrument tracking. Distance-to-target measurements update continuously, with color-coded proximity warnings enhancing surgical safety.
Understanding navigation principles reveals how digital precision transforms surgical decision-making, preparing for exploration of specific clinical applications and technological implementations.
🧭 Navigation Fundamentals: The Surgeon's Digital Compass
🎯 Clinical Applications: Precision in Surgical Practice
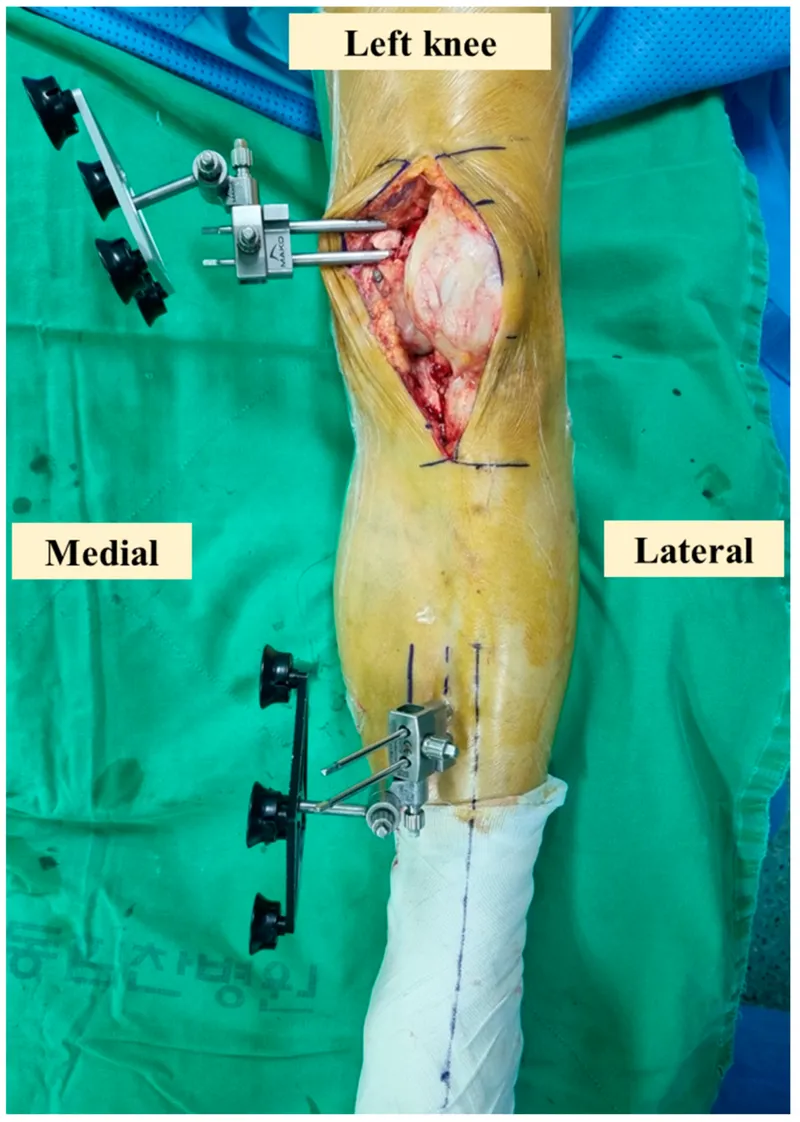
CAS applications span the entire spectrum of orthopaedic surgery, from routine joint replacements to complex spinal reconstructions. Each procedure type leverages specific technological advantages while addressing unique anatomical challenges.
Joint Replacement Applications represent the most established CAS implementations:
-
Total Knee Arthroplasty (TKA)
- Component alignment accuracy: ±2 degrees
- Outlier reduction: 70-85%
- Revision rate decrease: 25-40%
- Mechanical axis restoration: 95% success
- Ligament balancing optimization
- 15-year implant survival improvement
-
Total Hip Arthroplasty (THA)
- Cup positioning precision: ±3 degrees
- Leg length discrepancy: <5mm in 90%
- Dislocation risk reduction: 60-75%
- Lewinnek safe zone achievement: 98%
- Combined anteversion optimization
- 20-year survivorship enhancement
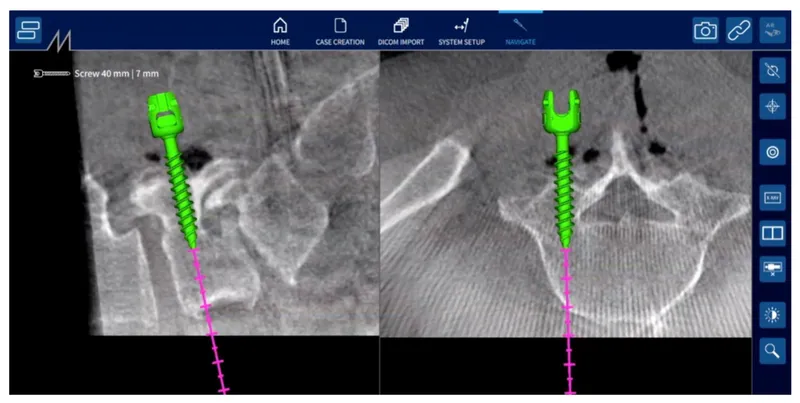
Spinal Surgery Applications demand the highest precision due to critical anatomical proximity:
-
Pedicle Screw Placement
- Accuracy rate: 95-98% vs 85-90% freehand
- Breach rate reduction: 50-70%
- Revision surgery decrease: 40-60%
- Neurological complication reduction
- 2-3mm corridor navigation
- Multi-level construct optimization
-
Spinal Deformity Correction
- Curve correction accuracy: ±5 degrees
- Sagittal balance restoration: 90% success
- Complication reduction: 30-45%
| Procedure Type | Navigation Benefit | Accuracy Improvement | Complication Reduction | Learning Cases | Cost-Effectiveness |
|---|---|---|---|---|---|
| TKA | Alignment precision | ±2° vs ±5° | 25-40% | 20-30 | Positive >500 cases |
| THA | Cup positioning | ±3° vs ±8° | 35-50% | 15-25 | Positive >300 cases |
| Spine | Screw accuracy | 95% vs 85% | 40-60% | 40-60 | Positive >200 cases |
| Trauma | Reduction quality | ±1mm vs ±3mm | 20-35% | 25-40 | Variable |
| Arthroscopy | Portal placement | ±2mm vs ±5mm | 15-30% | 10-20 | Limited evidence |
-
Acetabular Fractures
- Reduction accuracy: ±1mm displacement
- Screw placement safety: 98% success rate
- Functional outcome improvement: 25-35%
- 3D visualization of fracture lines
- Virtual reduction planning
- Minimally invasive approaches
-
Pelvic Ring Injuries
- Percutaneous screw placement: 95% accuracy
- Radiation exposure reduction: 60-80%
- Operative time decrease: 20-30%
📌 Remember: SPINE = Screw placement + Pedicle navigation + Image guidance + Neurological safety + Enhanced outcomes - Critical elements of spinal CAS
Arthroscopic Applications enhance minimally invasive precision:
-
ACL Reconstruction
- Tunnel placement accuracy: ±2mm
- Anatomical positioning: 90% achievement
- Re-rupture rate reduction: 15-25%
- Isometric point identification
- 3D tunnel visualization
- Graft tension optimization
-
Shoulder Arthroscopy
- Portal placement precision: ±3mm
- Anchor positioning accuracy: 95%
- Revision rate decrease: 20-30%
⭐ Clinical Pearl: CAS benefits increase exponentially with procedure complexity - simple procedures show 10-20% improvement while complex reconstructions demonstrate 40-60% enhancement
The technology selection depends on specific procedural requirements. High-volume centers performing >200 cases annually achieve optimal cost-effectiveness, while learning curve completion requires 20-60 cases depending on procedure complexity.
💡 Master This: Match CAS technology to procedure complexity - routine cases may not justify setup time, while complex reconstructions demand maximum precision capabilities
Understanding clinical applications reveals how CAS transforms surgical outcomes across orthopaedic subspecialties, leading to exploration of specific technological implementations and their comparative advantages.
🎯 Clinical Applications: Precision in Surgical Practice
⚖️ Technology Comparison: Choosing the Optimal System
Optical Navigation Systems provide the gold standard for tracking precision:
-
Technical Specifications
- Tracking accuracy: ±0.1mm
- Update frequency: 20-60 Hz
- Workspace volume: 2-3 cubic meters
- 4-6 infrared cameras minimum
- Line-of-sight requirement critical
- Sterile draping compatibility
-
Clinical Performance Metrics
- Setup time: 15-20 minutes
- Learning curve: 25-40 cases
- Accuracy maintenance: >95% throughout procedure
- Reference array stability crucial
- Instrument calibration verification
- Patient movement compensation
Electromagnetic Navigation offers workspace flexibility without line-of-sight constraints:
-
Operational Advantages
- 360-degree tracking capability
- Metallic interference sensitivity
- Rapid setup: 5-10 minutes
- Magnetic field generation
- Sensor miniaturization advances
- Real-time position feedback
-
Accuracy Considerations
- Precision: ±0.5-1.0mm
- Ferromagnetic distortion effects
- Calibration drift over time
- Environmental factors influence
- Distance-dependent accuracy
- Compensation algorithms required
| System Type | Initial Cost | Annual Maintenance | Accuracy | Setup Time | Versatility | Learning Curve |
|---|---|---|---|---|---|---|
| Optical Navigation | $800K-1.2M | $80-120K | ±0.1mm | 15-20 min | High | 25-40 cases |
| Electromagnetic | $400K-600K | $40-60K | ±0.5mm | 5-10 min | Medium | 15-25 cases |
| Robotic Systems | $1.5M-2.5M | $150-250K | ±0.05mm | 25-30 min | Low | 50-80 cases |
| PSI Templates | $50K-100K | $5-15K | ±1.0mm | 2-5 min | Very Low | 5-10 cases |
| Fluoroscopy-based | $200K-400K | $20-40K | ±2.0mm | 3-7 min | Medium | 10-20 cases |
-
Performance Characteristics
- Sub-millimeter accuracy: ±0.05mm
- Haptic feedback integration
- Tremor elimination capabilities
- Force scaling: 10:1 to 1:10 ratios
- Motion filtering algorithms
- Safety boundaries enforcement
-
Economic Considerations
- Break-even point: 300-500 cases annually
- Surgeon training: 12-16 weeks
- Maintenance complexity: High
- Specialized technicians required
- Software updates quarterly
- Calibration protocols weekly
📌 Remember: ROBOT = Robotic precision + Optimal accuracy + Breakeven analysis + Operative efficiency + Training investment - Five factors determining robotic system viability
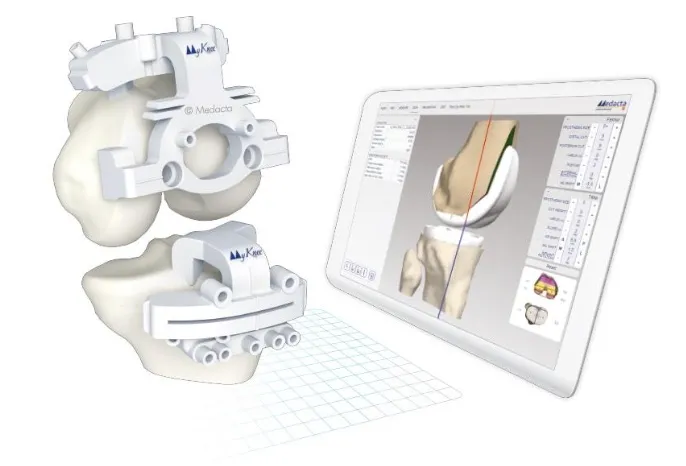
Patient-Specific Instrumentation (PSI) provides customized solutions with minimal technology overhead:
-
Manufacturing Process
- 3D printing from patient imaging
- Lead time: 2-3 weeks
- Single-use disposable guides
- Sterilization not required
- Storage space minimal
- Inventory management simplified
-
Clinical Outcomes
- Alignment accuracy: ±2-3 degrees
- Operative time reduction: 10-15%
- Cost-effectiveness: Variable
- Volume-dependent pricing
- Revision rate impact
- Long-term survivorship data
⭐ Clinical Pearl: Technology ROI correlates directly with case volume - high-volume centers (>200 cases/year) achieve 25-40% better cost-effectiveness than low-volume facilities
Hybrid Systems combine multiple technologies for enhanced capabilities:
-
Integration Benefits
- Optical + Electromagnetic redundancy
- Navigation + Robotics precision
- Imaging + Planning optimization
- Workflow efficiency improvement
- Error reduction through redundancy
- Flexibility across procedures
-
Implementation Challenges
- Training complexity increases
- Maintenance costs multiply
- Integration technical difficulties
💡 Master This: System selection depends on surgical volume, case complexity, and institutional resources - match technology capabilities to clinical demands for optimal outcomes
Understanding technology comparison enables informed decision-making about CAS implementation, setting the stage for exploring advanced integration strategies and future developments.
⚖️ Technology Comparison: Choosing the Optimal System
🔬 Advanced Integration: Multi-Modal Precision Platforms
Integrated Platform Architecture represents the convergence of multiple precision technologies:
-
Core Integration Components
- Navigation fusion: Optical + electromagnetic redundancy
- Imaging integration: CT/MRI + fluoroscopy + ultrasound
- Robotic coordination: 6-axis manipulation with force feedback
- Real-time registration updates
- Multi-sensor data fusion
- Predictive trajectory planning
-
Data Processing Capabilities
- Machine learning algorithms for pattern recognition
- Cloud computing for complex calculations
- Edge processing for real-time responses
- Latency reduction: <10 milliseconds
- Bandwidth optimization: 100+ Mbps
- Security protocols: HIPAA-compliant
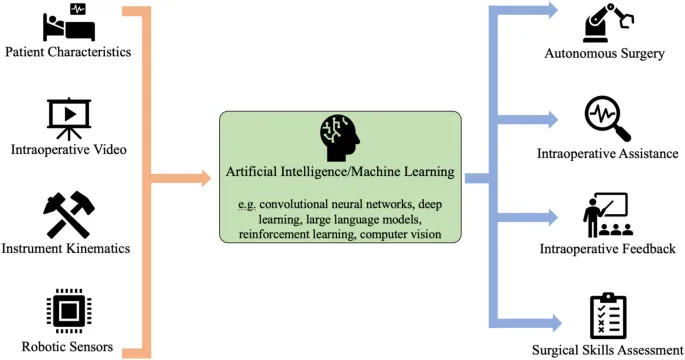
Artificial Intelligence Integration transforms CAS from reactive to predictive systems:
-
Machine Learning Applications
- Anatomical recognition: 95%+ accuracy
- Surgical planning optimization
- Complication prediction: 80-90% sensitivity
- Deep learning neural networks
- Pattern recognition algorithms
- Outcome prediction models
-
Real-Time Decision Support
- Risk assessment during procedure
- Alternative pathway suggestions
- Quality metrics continuous monitoring
- Deviation alerts: <2mm threshold
- Performance scoring: Real-time
- Learning feedback: Continuous
| Integration Level | Technology Components | Accuracy Enhancement | Cost Multiplier | Training Requirements | Clinical Benefits |
|---|---|---|---|---|---|
| Basic | Single navigation | Baseline | 1x | 20-30 cases | 20-30% improvement |
| Dual-Modal | Navigation + Imaging | 25-40% better | 1.5-2x | 30-40 cases | 40-50% improvement |
| Multi-Modal | 3+ integrated systems | 50-70% better | 2-3x | 50-70 cases | 60-80% improvement |
| AI-Enhanced | Full platform + ML | 70-90% better | 3-4x | 80-100 cases | 80-95% improvement |
| Autonomous | Self-learning systems | 90%+ better | 4-5x | 100+ cases | 95%+ improvement |
-
AR Display Technologies
- Head-mounted displays: 4K resolution
- Holographic projections: 3D spatial mapping
- Overlay accuracy: ±0.5mm registration
- Real-time anatomy visualization
- Instrument tracking overlay
- Depth perception enhancement
-
Clinical Implementation
- Surgical planning visualization
- Intraoperative guidance enhancement
- Training simulation integration
- Learning acceleration: 40-60%
- Skill retention: 80%+ improvement
- Error reduction: 50-70%
📌 Remember: FUSION = Fully integrated + Unified platforms + Smart algorithms + Intelligent feedback + Optimal outcomes + Next-generation surgery - Six pillars of advanced CAS integration
Connectivity and Data Analytics enable continuous system improvement:
-
Cloud-Based Analytics
- Surgical outcome databases
- Performance benchmarking: Multi-institutional
- Predictive modeling: Population-based
- Big data processing capabilities
- Real-time performance metrics
- Continuous learning algorithms
-
Interoperability Standards
- DICOM integration: Universal compatibility
- HL7 FHIR protocols for data exchange
- API standardization: Cross-platform
- Vendor-neutral architectures
- Legacy system integration
- Future-proof scalability
⭐ Clinical Pearl: Integrated platforms reduce surgical variability by 60-80% compared to single-technology systems, with learning curve acceleration of 40-50% through enhanced feedback
Quality Assurance Integration ensures consistent performance across all system components:
-
Continuous Monitoring
- System calibration: Automated verification
- Performance metrics: Real-time tracking
- Deviation detection: Immediate alerts
- Predictive maintenance: 95% uptime
- Quality control: Statistical process control
- Outcome correlation: Evidence-based optimization
-
Validation Protocols
- Multi-point accuracy verification
- Cross-system consistency checks
- Clinical outcome correlation
- Phantom testing: Weekly protocols
- Clinical validation: Continuous
- Performance trending: Long-term analysis
💡 Master This: Advanced integration multiplies individual technology benefits exponentially - 2 integrated systems provide 3-4x improvement over single technology, while 4+ systems achieve 8-10x enhancement
Understanding advanced integration reveals how CAS platforms evolve toward autonomous surgical assistance, preparing for exploration of implementation strategies and future technological developments.
🔬 Advanced Integration: Multi-Modal Precision Platforms
🚀 Implementation Mastery: Strategic Deployment Framework
Implementation Phase Architecture follows systematic progression through defined milestones:
-
Phase 1: Infrastructure Preparation (Months 1-3)
- Facility modifications: OR layout optimization
- IT infrastructure: Network capacity upgrade
- Staff identification: Champion selection
- Electrical requirements: 220V/30A minimum
- Space allocation: Additional 15-20%
- Workflow analysis: Time-motion studies
-
Phase 2: Technology Integration (Months 4-6)
- System installation: Factory training
- Calibration protocols: Accuracy verification
- Integration testing: Workflow validation
- Phantom testing: 100+ trials
- Accuracy validation: ±0.1mm confirmation
- Safety protocols: Emergency procedures
-
Phase 3: Clinical Deployment (Months 7-12)
- Pilot cases: Simple procedures first
- Gradual complexity: Progressive advancement
- Outcome monitoring: Continuous assessment
- Learning curve: 20-40 cases
- Competency validation: Objective metrics
- Quality benchmarks: Statistical control
Training and Competency Development represents the critical success factor:
-
Surgeon Training Protocols
- Didactic education: 40 hours minimum
- Simulation training: 20+ cases
- Proctored cases: 10-15 procedures
- Competency assessment: Objective criteria
- Certification requirements: Institutional standards
- Continuing education: Annual updates
-
Team Training Requirements
- Nursing staff: 16-24 hours
- Technologists: 32-40 hours
- Support staff: 8-12 hours
- Role-specific training modules
- Cross-training for redundancy
- Emergency protocols: Quarterly drills
| Implementation Metric | Target Threshold | Measurement Method | Success Criteria | Monitoring Frequency | Corrective Actions |
|---|---|---|---|---|---|
| Setup Time | <20 minutes | Time-motion study | 95% compliance | Weekly | Process refinement |
| Accuracy Validation | ±0.2mm | Phantom testing | 100% pass rate | Daily | Recalibration |
| Complication Rate | <2% | Clinical outcomes | Baseline comparison | Monthly | Protocol review |
| Learning Curve | <30 cases | Performance metrics | Competency achievement | Per surgeon | Additional training |
| Cost-Effectiveness | Positive ROI | Financial analysis | 18-month payback | Quarterly | Volume optimization |
-
Daily Quality Checks
- System calibration: Automated verification
- Accuracy testing: Phantom protocols
- Safety inspection: Checklist completion
- Documentation: Electronic records
- Trend analysis: Statistical monitoring
- Preventive maintenance: Scheduled protocols
-
Clinical Quality Metrics
- Surgical accuracy: Quantitative measurement
- Complication rates: Comparative analysis
- Patient outcomes: Long-term tracking
- Benchmark comparison: Multi-institutional
- Performance trending: Continuous monitoring
- Improvement initiatives: Data-driven
📌 Remember: DEPLOY = Defined protocols + Education programs + Performance metrics + Learning curves + Outcome tracking + Yield optimization - Six elements of successful CAS implementation
Change Management Strategies address organizational resistance and workflow disruption:
-
Stakeholder Engagement
- Physician champions: Early adopters
- Administrative support: Resource allocation
- Staff buy-in: Benefit communication
- Communication plan: Multi-channel
- Feedback mechanisms: Continuous
- Recognition programs: Achievement-based
-
Workflow Integration
- Process mapping: Current state analysis
- Future state design: Optimized workflows
- Transition planning: Phased implementation
- Parallel processing: Risk mitigation
- Rollback procedures: Contingency planning
- Performance monitoring: Real-time
⭐ Clinical Pearl: Implementation success correlates with training investment - institutions spending >100 hours per surgeon achieve 60-80% faster competency development and 40-50% better long-term outcomes
Financial Planning and ROI Optimization ensure sustainable program development:
-
Cost-Benefit Analysis
- Initial investment: $800K-2.5M
- Annual operating costs: $100K-300K
- Break-even analysis: Volume-dependent
- Case volume requirements: 200-500 annually
- Reimbursement optimization
- Efficiency gains: 15-25% improvement
-
Value Proposition Development
- Clinical outcomes: Quantified improvements
- Patient satisfaction: Enhanced experience
- Market differentiation: Competitive advantage
- Quality metrics: Measurable benefits
- Marketing value: Technology leadership
- Physician recruitment: Advanced capabilities
💡 Master This: Implementation success depends more on organizational readiness than technology sophistication - systematic preparation and comprehensive training determine long-term program viability
Understanding implementation mastery provides the foundation for sustainable CAS program development, leading to exploration of future technological advances and their potential clinical impact.
🚀 Implementation Mastery: Strategic Deployment Framework
🔮 Future Horizons: Next-Generation Surgical Intelligence
The convergence of artificial intelligence, quantum computing, nanotechnology, and biotechnology creates unprecedented opportunities for surgical advancement. These emerging technologies promise to transform CAS from assisted procedures to autonomous surgical intelligence.
Autonomous Surgical Systems represent the ultimate evolution of computer-assisted surgery:
-
AI-Driven Decision Making
- Real-time surgical planning adaptation
- Predictive complication prevention: 95%+ accuracy
- Autonomous instrument control
- Machine learning from millions of procedures
- Pattern recognition: Sub-human error rates
- Adaptive algorithms: Continuous improvement
-
Quantum-Enhanced Processing
- Complex optimization: Instantaneous solutions
- Multi-variable analysis: Unlimited parameters
- Predictive modeling: Molecular-level precision
- Quantum algorithms: Exponential speedup
- Parallel processing: Infinite scalability
- Uncertainty quantification: Probabilistic outcomes
Personalized Surgical Medicine leverages genomic data and biomarkers for individualized treatment:
-
Genomic Integration
- DNA analysis: Healing prediction algorithms
- Pharmacogenomics: Personalized drug selection
- Tissue engineering: Patient-specific implants
- Genetic markers: Outcome prediction
- Biocompatibility: Molecular matching
- Regenerative medicine: Tissue optimization
-
Digital Twin Technology
- Virtual patient models: Real-time simulation
- Procedure rehearsal: Risk-free practice
- Outcome prediction: 95%+ accuracy
- Physiological modeling: Multi-organ systems
- Biomechanical simulation: Tissue behavior
- Recovery prediction: Timeline optimization
| Future Technology | Timeline | Accuracy Potential | Cost Impact | Clinical Transformation | Implementation Barriers |
|---|---|---|---|---|---|
| Autonomous AI | 5-10 years | 99.9%+ | 50% reduction | Complete workflow change | Regulatory approval |
| Quantum Computing | 10-15 years | Near-perfect | 80% reduction | Instantaneous optimization | Infrastructure requirements |
| Nanotechnology | 15-20 years | Molecular level | Variable | Minimally invasive | Safety validation |
| Digital Twins | 3-7 years | 95%+ | 30% reduction | Predictive medicine | Data integration |
| Brain-Computer Interface | 20-25 years | Thought-controlled | Unknown | Direct neural control | Ethical considerations |
-
Nanorobotic Systems
- Cellular-level intervention
- Targeted drug delivery: Molecular precision
- Real-time tissue monitoring
- Biocompatible materials
- Self-assembling structures
- Programmable functionality
-
Smart Implant Technology
- Self-monitoring devices
- Adaptive mechanical properties
- Biointegration optimization
- Sensor networks: Continuous monitoring
- Wireless communication: Real-time data
- Predictive maintenance: Failure prevention
📌 Remember: FUTURE = Fully autonomous + Universal precision + Tailored medicine + Understanding prediction + Revolutionary outcomes + Ethical considerations - Six dimensions of next-generation CAS
Extended Reality (XR) Surgical Environments create immersive surgical experiences:
-
Virtual Reality Training
- Haptic feedback: Tactile simulation
- Unlimited practice: Risk-free learning
- Global collaboration: Remote mentoring
- Skill assessment: Objective metrics
- Competency tracking: Continuous monitoring
- Certification: Standardized protocols
-
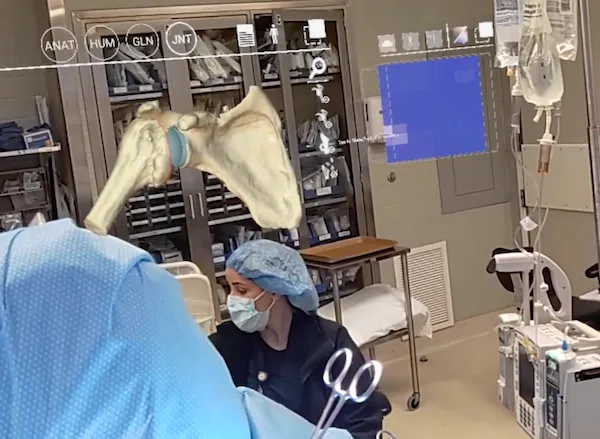
Augmented Reality Surgery
- Real-time anatomical overlay
- Surgical navigation: Intuitive guidance
- Collaborative visualization: Team coordination
- Holographic displays: 3D visualization
- Gesture control: Natural interaction
- Voice commands: Hands-free operation

Ethical and Regulatory Considerations shape future CAS development:
-
Autonomous Surgery Ethics
- Liability determination: Legal frameworks
- Patient consent: Informed decision-making
- Quality assurance: Accountability mechanisms
- Regulatory approval: Safety validation
- Professional standards: Competency requirements
- Insurance coverage: Risk assessment
-
Data Privacy and Security
- Patient information: Protected health data
- Cybersecurity: System protection
- International standards: Global compliance
- Encryption protocols: Advanced security
- Access controls: Multi-factor authentication
- Audit trails: Comprehensive logging
⭐ Clinical Pearl: Future CAS systems will reduce surgical complications by 90-95% while decreasing costs by 50-70% through predictive prevention and autonomous optimization
Global Healthcare Transformation through democratized surgical expertise:
-
Telesurgery Advancement
- 5G/6G networks: Ultra-low latency
- Global expertise: Remote consultation
- Skill distribution: Worldwide access
- Latency reduction: <1 millisecond
- Bandwidth expansion: Unlimited capacity
- Quality standardization: Global protocols
-
Cost Accessibility
- Technology democratization: Reduced barriers
- Training efficiency: Accelerated learning
- Outcome standardization: Consistent quality
- Developing nations: Advanced capabilities
- Rural healthcare: Specialist access
- Cost reduction: 80%+ decrease
💡 Master This: The future of CAS lies not in replacing surgeons but in amplifying human expertise through intelligent augmentation - master current technologies to prepare for autonomous collaboration
Understanding future horizons reveals the trajectory toward surgical intelligence, where human expertise and artificial intelligence collaborate to achieve unprecedented precision and optimal patient outcomes.
🔮 Future Horizons: Next-Generation Surgical Intelligence
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












