Maternal Physiological Changes - Heart's Big Load
- Cardiac Output (CO): ↑ 30-50%; peaks 20-24 wks.
- Early: ↑ Stroke Volume (SV).
- Later: ↑ Heart Rate (HR) by 15-20 bpm.
- Blood Volume: ↑ 40-50%.
- Plasma volume ↑ 40-50% > RBC mass ↑ 20-30% → physiological anemia.
- Systemic Vascular Resistance (SVR): ↓ (progesterone, PGs).
- Blood Pressure (BP):
- Systolic: Slight ↓ or stable.
- Diastolic: ↓ (nadir mid-preg), then ↑.
- Heart Sounds: Wide S1 split, S3. Systolic ejection murmur (flow, ~90%). Diastolic = PATHOLOGY.
- ECG: Left axis deviation.
- Supine Hypotension: IVC compression → ↓CO. Use left lateral position.
- 📌 Mnemonic: CO ↑, Blood Volume ↑, SVR ↓, Diastolic BP ↓.
⭐ Cardiac output increases by 30-50% during pregnancy, peaking around 20-24 weeks.
 oka
oka
Maternal Physiological Changes - Breathing & Peeing
Respiratory System:
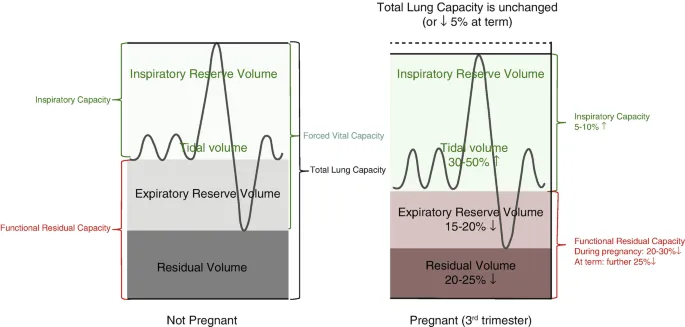
- Diaphragm: Elevated ~4 cm; Thoracic cage circumference ↑.
- Tidal Volume (TV) & Minute Ventilation (MV): ↑ 30-50%.
- Functional Residual Capacity (FRC) & Residual Volume (RV): ↓ 20%. Total Lung Capacity (TLC) slightly ↓.
- $PaCO_2$: ↓ to 27-32 mmHg (progesterone effect) → compensated respiratory alkalosis.
- Physiological dyspnea common.
Renal System:
- Kidneys: ↑ size; Glomerular Filtration Rate (GFR) & Renal Plasma Flow (RPF) ↑ by ~50%.
- Serum Creatinine & Blood Urea Nitrogen (BUN): ↓.
- Physiological hydronephrosis & hydroureter (Right > Left common).
- Glycosuria: Common (↓ tubular reabsorption of glucose).
- Urinary frequency & nocturia. Renin-Angiotensin-Aldosterone System (RAAS) activity ↑.
⭐ Progesterone is the primary stimulant for increased minute ventilation, leading to chronic compensated respiratory alkalosis with renal bicarbonate excretion.
Maternal Physiological Changes - Blood & Guts Shifts
- Blood Volume & Composition:
- Plasma volume ↑ by 40-50%; Red Blood Cell (RBC) mass ↑ by 20-30%.
- Physiological anemia: Hemoglobin (Hb) ↓ (e.g., < 11 g/dL in 1st trimester, < 10.5 g/dL in 2nd).
- White Blood Cell (WBC) count (leukocytosis) ↑; Platelets may slightly ↓.
- Hypercoagulable state: Fibrinogen ↑, Clotting Factors (VII, VIII, X) ↑. Erythrocyte Sedimentation Rate (ESR) ↑.
- Iron requirement ↑ significantly (total ~1000 mg).
- Gastrointestinal System:
- Nausea & Vomiting of Pregnancy (NVP): Common, linked to hCG.
- ↓ Lower Esophageal Sphincter (LES) tone → Heartburn/GERD (progesterone effect).
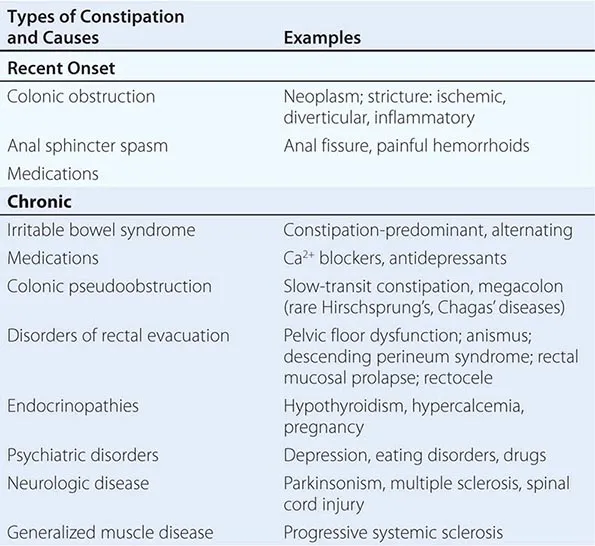
- ↓ GI motility → Constipation, ↑ nutrient absorption time.
- Gallbladder: Stasis, ↓ contractility → ↑ risk of cholesterol gallstones.
- Liver: Alkaline Phosphatase (ALP) ↑ (placental origin); serum albumin ↓ (hemodilution).
⭐ Plasma volume expansion significantly exceeds red cell mass increase, causing physiological hemodilution and a decrease in hemoglobin concentration, hematocrit, and red blood cell count.
Maternal Physiological Changes - Hormones & Body Mods
- Hormones:
- hCG: Peaks 8-10 wks; maintains corpus luteum.
- Progesterone (↑): Smooth muscle relaxation; supports pregnancy.
- Estrogen (E3) (↑): Uterine/breast growth.
- hPL/hCS (↑): Anti-insulin (↑ maternal glucose); lipolysis.
- Relaxin (↑): Softens cervix, ligaments.
- Prolactin (↑): Prepares lactation.
- Cortisol (↑), Aldosterone (↑).
- Thyroid: ↑TBG → ↑Total T4/T3. hCG may ↓TSH (1st trim).
- Body Modifications:
- Weight Gain: Avg. 11-16 kg.
- BMR: ↑ 15-20%.
- Insulin Resistance: hPL, progesterone, cortisol driven.
- Breast: ↑Size, tenderness; Montgomery's tubercles; colostrum (~16 wks).
- Skin: Hyperpigmentation (linea nigra, melasma); striae; spider angiomata.

⭐ hPL (Human Placental Lactogen) is key for diabetogenic state of pregnancy, ensuring fetal glucose supply.
High‑Yield Points - ⚡ Biggest Takeaways
- Cardiac output ↑ 30-50%; SVR ↓; supine hypotension common.
- Plasma volume ↑ more than RBC mass, causing physiological anemia; hypercoagulable state.
- Tidal volume & minute ventilation ↑; PaCO2 ↓ (compensated respiratory alkalosis).
- GFR & renal plasma flow ↑ by 50%; mild proteinuria & glycosuria can be normal.
- ↑ Estrogen, progesterone, hCG, hPL; progressive insulin resistance.
- Uterine blood flow ↑ dramatically.
- Diaphragm elevated, AP chest diameter ↑; thoracic breathing predominates.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

