Food Microbiology

On this page
🔬 Microbial Ecosystem Mastery: The Hidden Food Universe
Food is never sterile-it's a dynamic battlefield where beneficial microbes preserve nutrients while pathogens threaten public health at every stage from farm to table. You'll master the microbial ecosystems that colonize our food supply, engineer environmental controls that halt pathogen growth, recognize the clinical fingerprints of foodborne outbreaks, and deploy multi-barrier prevention systems that protect populations. By integrating classical microbiology with modern surveillance technology, you'll think like both detective and defender, transforming food safety from reactive crisis management into proactive disease prevention.
Food microbiology encompasses the study of microorganisms that inhabit, grow, or contaminate food. These microscopic entities include bacteria (10⁻⁶ meters), viruses (10⁻⁸ meters), fungi (10⁻⁵ meters), and parasites that influence food safety, quality, and nutritional value. The field examines both beneficial microorganisms used in fermentation and pathogenic species causing foodborne illness.
📌 Remember: BVFP - Bacteria, Viruses, Fungi, Parasites - The four kingdoms of food microbiology, each requiring different detection methods and control strategies
-
Beneficial Microorganisms
- Lactic acid bacteria: Lactobacillus species (pH reduction to 3.5-4.0)
- Yeasts: Saccharomyces cerevisiae (alcohol production 12-15% by volume)
- Fermentation rate: 2-4 grams glucose/hour
- Optimal temperature: 25-30°C
- Molds: Aspergillus oryzae (enzyme production 500+ units/gram)
-
Pathogenic Microorganisms
- Bacterial pathogens: Salmonella (infective dose 10-100 cells)
- Viral agents: Norovirus (infective dose <10 particles)
- Survival on surfaces: weeks to months
- Heat resistance: survives 60°C for 30 minutes
- Parasitic forms: Cyclospora (oocyst survival months in environment)
| Microorganism Type | Size Range | Growth Temperature | pH Tolerance | Oxygen Requirement | Clinical Significance |
|---|---|---|---|---|---|
| Bacteria | 0.5-5.0 μm | 4-60°C | 4.0-9.0 | Variable | 90% foodborne illness |
| Viruses | 20-300 nm | Host-dependent | 2.0-12.0 | None | 15% outbreak cases |
| Yeasts | 3-15 μm | 10-35°C | 2.0-8.5 | Facultative | Spoilage + fermentation |
| Molds | 2-10 μm | 10-35°C | 1.5-11.0 | Aerobic | Mycotoxin production |
| Parasites | 5-50 μm | 15-40°C | 6.0-8.0 | Variable | 5% foodborne disease |
The microbial load in food varies dramatically by type and processing. Fresh vegetables carry 10⁴-10⁶ CFU/gram, while processed foods maintain <10² CFU/gram. Raw meat harbors 10⁵-10⁷ CFU/gram, with pathogenic bacteria comprising 0.1-1% of total microflora.
💡 Master This: Microbial competition creates natural preservation - beneficial bacteria produce bacteriocins and organic acids that inhibit pathogens. Understanding this principle enables biopreservation strategies that reduce chemical preservative dependence by 60-80%
Environmental factors controlling microbial growth follow the FATTOM principle: Food (nutrients), Acidity (pH), Temperature, Time, Oxygen, Moisture. Each factor provides control points for food safety management.
📌 Remember: FATTOM controls microbial destiny - manipulate any factor to prevent pathogen growth and ensure food safety
Connect these foundational microbial principles through systematic growth factor analysis to understand how environmental manipulation creates the cornerstone of food preservation strategies.
🔬 Microbial Ecosystem Mastery: The Hidden Food Universe
⚙️ Growth Factor Engineering: The Environmental Control Matrix
Temperature Control Mechanisms
Temperature represents the most critical growth factor, with 10°C changes altering microbial growth rates by 2-3 fold. Pathogenic bacteria exhibit optimal growth between 35-40°C, while refrigeration (<4°C) reduces growth rates by 90-95%.
-
Psychrophiles (cold-loving): -5 to 20°C
- Listeria monocytogenes: grows at 0°C, doubling time 13 hours
- Spoilage significance: 60% of refrigerated food deterioration
- Enzyme activity: remains 20-30% at refrigeration temperatures
- Membrane fluidity: maintains function through unsaturated fatty acids
-
Mesophiles (moderate temperature): 20-45°C
- Salmonella species: optimal 37°C, doubling time 20 minutes
- E. coli O157:H7: growth range 7-46°C
- Heat sensitivity: D₆₀°C = 0.5-1.0 minutes
- Cold survival: >100 days in refrigerated foods
-
Thermophiles (heat-loving): 45-80°C
- Clostridium perfringens: survives 100°C for 1-4 hours
- Spore resistance: D₁₂₁°C = 0.1-1.5 minutes
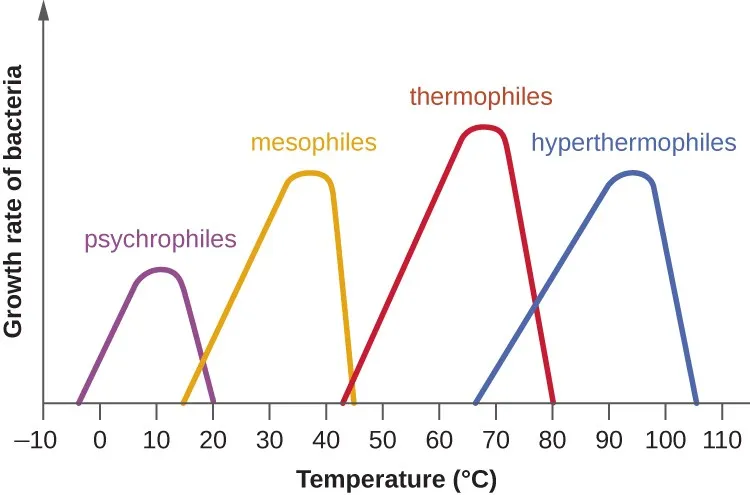
⭐ Clinical Pearl: The "2-hour rule" prevents pathogen multiplication - foods held in the danger zone (4-60°C) for >2 hours allow bacterial populations to reach infectious doses (10⁵-10⁶ CFU/gram)
pH and Acidity Barriers
pH manipulation creates powerful antimicrobial barriers through acid stress and membrane disruption. Most pathogenic bacteria require pH 6.0-8.0 for optimal growth, while pH <4.6 prevents Clostridium botulinum spore germination.
| pH Range | Food Examples | Dominant Microflora | Preservation Strategy | Pathogen Risk |
|---|---|---|---|---|
| >7.0 | Egg whites, fish | Spoilage bacteria | Refrigeration + time | High |
| 6.0-7.0 | Meat, vegetables | Mixed populations | Heat + refrigeration | Very High |
| 4.6-6.0 | Cheese, bread | Lactic acid bacteria | Fermentation control | Moderate |
| 3.7-4.6 | Tomatoes, wine | Yeasts, molds | Acid preservation | Low |
| <3.7 | Citrus, vinegar | Acid-tolerant yeasts | Natural preservation | Very Low |
Water Activity Engineering
Water activity (aᵨ) measures available water for microbial growth, distinct from total moisture content. Most bacteria require aᵨ >0.95, while molds tolerate aᵨ 0.70-0.80. Reducing water activity below 0.85 prevents most pathogenic bacteria growth.
-
High Water Activity (aᵨ 0.95-1.00)
- Fresh meats, vegetables, dairy products
- Bacterial growth: optimal conditions
- Salmonella: minimum aᵨ 0.94
- E. coli: minimum aᵨ 0.95
-
Intermediate Water Activity (aᵨ 0.85-0.95)
- Cured meats, aged cheeses
- Selective microbial growth: yeasts and molds predominate
- Staphylococcus aureus: minimum aᵨ 0.86
- Toxin production: requires aᵨ >0.93
-
Low Water Activity (aᵨ <0.85)
- Dried foods, honey, nuts
- Microbial stability: extended shelf life
- Aspergillus species: minimum aᵨ 0.70
- Xerophilic yeasts: minimum aᵨ 0.65

📌 Remember: "Dry Means Die" - reducing water activity below 0.85 eliminates >99% of pathogenic bacteria, while maintaining food nutritional value and extending shelf life by months to years
Connect these environmental control principles through systematic pathogen identification to understand how specific microorganisms exploit growth factor combinations in clinical food safety scenarios.
⚙️ Growth Factor Engineering: The Environmental Control Matrix
🦠 Pathogen Profiling Arsenal: The Clinical Recognition Matrix
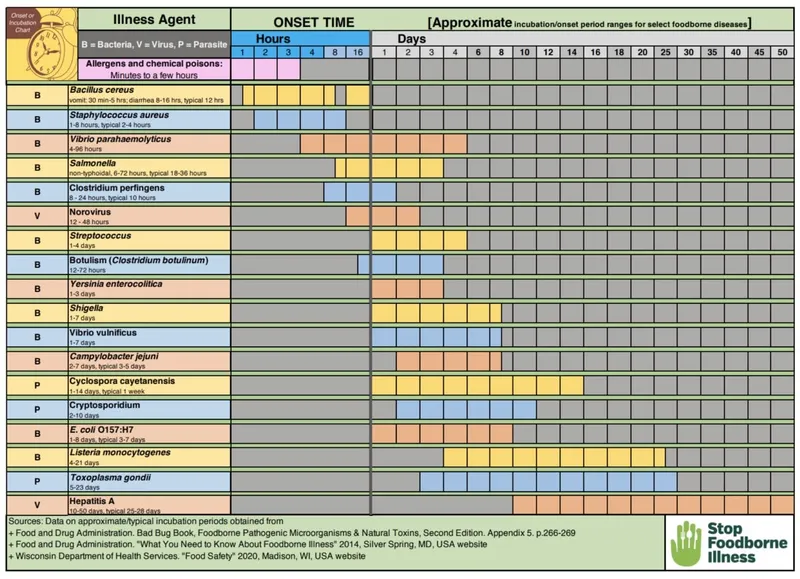
Bacterial Pathogen Recognition Patterns
Bacterial foodborne pathogens cause >80% of identified foodborne illness outbreaks, with distinct clinical presentations based on pathogenic mechanisms. Invasive pathogens penetrate intestinal mucosa, while toxigenic bacteria produce enterotoxins causing rapid symptom onset.
-
Rapid-Onset Toxigenic Pathogens (<6 hours)
-
Staphylococcus aureus: preformed enterotoxin
- Incubation: 1-6 hours (median 3 hours)
- Symptoms: violent vomiting (>10 episodes), cramping
- Infectious dose: 10⁵-10⁶ CFU or 1-5 μg toxin
- Food association: dairy products, salads, bakery items
-
Bacillus cereus (emetic form): preformed cereulide toxin
- Incubation: 1-6 hours
- Symptoms: severe nausea, vomiting (rice syndrome)
- Heat stability: toxin survives 126°C for 90 minutes
-
-
Intermediate-Onset Invasive Pathogens (6-72 hours)
-
Salmonella species: invasive enterocolitis
- Incubation: 12-36 hours (range 6-72 hours)
- Symptoms: fever (38-40°C), diarrhea (>6 stools/day)
- Infectious dose: 10-100 organisms (highly variable)
- Complications: bacteremia (5-10% cases), typhoid fever
-
Campylobacter jejuni: mucosal invasion
- Incubation: 2-5 days (range 1-10 days)
- Symptoms: bloody diarrhea, severe cramping
- Infectious dose: <500 organisms
- Sequelae: Guillain-Barré syndrome (1:1000 cases)
-
⭐ Clinical Pearl: Symptom timing provides diagnostic clues - <6 hours suggests preformed toxins, 6-24 hours indicates bacterial multiplication, >24 hours suggests invasive pathogens or parasites
Viral and Parasitic Recognition Frameworks
Viral pathogens cause >50% of foodborne illness cases but <20% of identified outbreaks due to diagnostic challenges. Parasitic infections show prolonged incubation periods and chronic symptoms distinguishing them from bacterial causes.
| Pathogen Category | Incubation Period | Primary Symptoms | Diagnostic Features | Attack Rate |
|---|---|---|---|---|
| Preformed Toxins | 1-6 hours | Vomiting, cramping | Rapid onset, short duration | >50% |
| Bacterial Multiplication | 8-24 hours | Diarrhea, cramping | Moderate onset, 2-3 days | 25-50% |
| Invasive Bacteria | 12-72 hours | Fever, bloody diarrhea | Systemic symptoms | 10-25% |
| Viral Agents | 24-48 hours | Vomiting, diarrhea | Person-to-person spread | >75% |
| Parasitic Agents | 1-4 weeks | Chronic diarrhea | Prolonged symptoms | <10% |
- Incubation: 24-48 hours (range 12-72 hours)
- Symptoms: projectile vomiting, watery diarrhea
- Duration: 24-72 hours (self-limiting)
- Attack rate: >75% in closed populations
- Secondary transmission: >30% household contacts
- Environmental persistence: weeks on surfaces
- Parasitic Pattern Recognition
-
Cyclospora cayetanensis: 7-14 day incubation
- Symptoms: watery diarrhea (>10 stools/day)
- Duration: weeks to months without treatment
- Food association: fresh produce (berries, herbs)
-
Cryptosporidium parvum: 2-10 day incubation
- Symptoms: profuse watery diarrhea (>20 L/day)
- High-risk groups: immunocompromised patients
- Chlorine resistance: survives standard water treatment
-
💡 Master This: Food vehicle identification narrows pathogen possibilities - poultry suggests Salmonella/Campylobacter, dairy indicates Staphylococcus, shellfish points to Norovirus/Vibrio, enabling targeted testing and treatment
📌 Remember: "VOMIT" for rapid-onset toxins - Violent onset, Outbreak pattern, Minimal fever, Immediate symptoms, Toxin-mediated (Staph aureus, B. cereus emetic)
Connect these pathogen recognition patterns through systematic outbreak investigation principles to understand how epidemiological analysis transforms individual cases into population-level food safety interventions.
🦠 Pathogen Profiling Arsenal: The Clinical Recognition Matrix
🔍 Outbreak Investigation Mastery: The Epidemiological Detective Framework
Case Definition and Verification Protocols
Outbreak investigation begins with precise case definitions that distinguish outbreak-related illness from background disease. Confirmed cases meet laboratory criteria, while probable cases satisfy clinical and epidemiological criteria without laboratory confirmation.
- Case Definition Components
-
Clinical criteria: specific symptom combinations
- Gastroenteritis: diarrhea (≥3 loose stools/24 hours) OR vomiting
- Severity markers: fever (>38°C), blood in stool, dehydration
- Duration thresholds: symptoms lasting >12 hours
-
Epidemiological criteria: exposure linkages
- Time boundaries: illness onset within incubation period
- Place connections: common venue or food source
- Person characteristics: demographic patterns
-
Laboratory criteria: pathogen confirmation
- Stool culture: isolation of outbreak strain
- Serological testing: specific antibody responses
- Molecular typing: PFGE, WGS strain matching
-
⭐ Clinical Pearl: Attack rates >15% suggest common source outbreaks, while <5% indicates person-to-person transmission. Secondary attack rates >30% in households confirm highly contagious agents like Norovirus
Analytical Study Design and Implementation
Outbreak investigations employ case-control or cohort study designs to identify food vehicles and risk factors. Odds ratios >2.0 with confidence intervals excluding 1.0 indicate significant associations requiring immediate control measures.
-
Cohort Study Applications
- Defined populations: wedding receptions, conferences, schools
- Attack rate calculations: (ill persons/total exposed) × 100
- Food-specific attack rates: compare exposed vs. unexposed groups
- Relative risk >2.0: suggests causal association
- Attributable risk >50%: indicates major contributing factor
-
Case-Control Study Methods
- Undefined populations: restaurant patrons, community outbreaks
- Control selection: 2-4 controls per case, matched by demographics
- Odds ratio interpretation:
- OR 1.0: no association
- OR >2.0: positive association (risk factor)
- OR <0.5: negative association (protective factor)
| Study Design | Population Type | Primary Measure | Interpretation Threshold | Control Implementation |
|---|---|---|---|---|
| Cohort | Defined group | Attack Rate | >15% difference | Immediate food removal |
| Case-Control | Undefined population | Odds Ratio | >2.0 with CI>1.0 | Source investigation |
| Cross-Sectional | Survey-based | Prevalence Ratio | >1.5 with significance | Risk communication |
| Ecological | Population-level | Correlation | r>0.7 with p<0.05 | Policy intervention |
Environmental investigation identifies contamination sources, critical control point failures, and transmission pathways. Traceback investigations follow food distribution chains to identify common suppliers and production facilities.
-
Food Safety Assessment
- Temperature logs: verify cold chain maintenance (<4°C)
- HACCP records: identify critical control point deviations
- Employee health: screen for asymptomatic carriers
- Stool testing: food handlers with GI symptoms
- Exclusion criteria: positive cultures, 48-hour symptom-free
-
Laboratory Investigation
- Food sampling: collect ≥100g samples for testing
- Environmental sampling: surfaces, equipment, water sources
- Molecular subtyping: PFGE, MLST, whole genome sequencing
- Genetic relatedness: ≥95% similarity suggests common source
- Outbreak strain definition: ≤2 SNP differences (WGS)
💡 Master This: Dose-response relationships guide control measures - high-attack rate foods (>50%) with low infectious doses (<100 organisms) require immediate removal and supplier notification to prevent continued exposure
- Control Measure Implementation
- Immediate actions: food embargo, facility closure
- Communication strategies: public notification, media coordination
- Follow-up monitoring: continued surveillance, 14-day post-exposure
- Epidemic curve monitoring: declining case numbers
- Secondary prevention: household contact screening
📌 Remember: "STEP" for outbreak investigation - Suspect cases, Test hypotheses, Environmental assessment, Prevent continued exposure
Connect these investigation principles through systematic prevention and control strategies to understand how outbreak lessons transform into comprehensive food safety management systems.
🔍 Outbreak Investigation Mastery: The Epidemiological Detective Framework
⚖️ Prevention Protocol Engineering: The Multi-Barrier Defense System
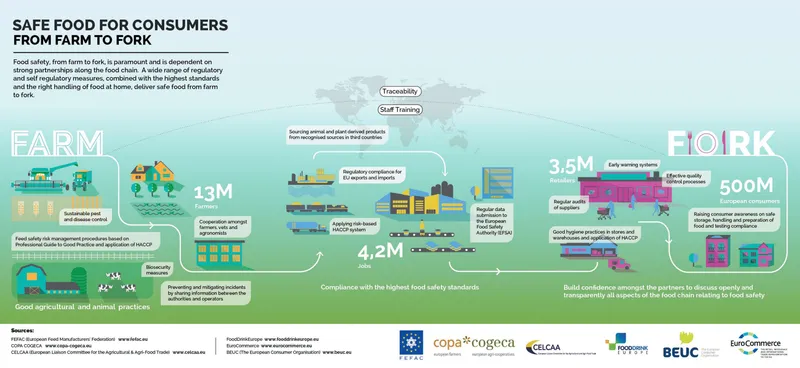
HACCP Implementation and Critical Control Points
Hazard Analysis Critical Control Points (HACCP) provides systematic methodology for biological, chemical, and physical hazard control. Critical Control Points (CCPs) represent process steps where preventive measures eliminate or reduce hazards to acceptable levels.
- Critical Control Point Identification
-
Thermal processing: 71°C for 15 seconds (poultry)
- Critical limit: core temperature ≥71°C
- Monitoring: continuous temperature recording
- Corrective action: reprocess or discard product
-
Refrigerated storage: ≤4°C maintenance
- Critical limit: storage temperature <4°C
- Monitoring: hourly temperature checks
- Corrective action: temperature adjustment, product evaluation
-
pH control: acidified foods pH ≤4.6
- Critical limit: pH 4.6 or below
- Monitoring: pH measurement each batch
- Corrective action: acid addition, product rework
-
| Process Step | Hazard Type | Critical Limit | Monitoring Frequency | Corrective Action | Verification Method |
|---|---|---|---|---|---|
| Receiving | Biological | Temperature ≤4°C | Each delivery | Reject product | Supplier audits |
| Cooking | Biological | 71°C × 15 sec | Continuous | Recook/discard | Calibration checks |
| Cooling | Biological | 21°C in 2 hours | Every 30 min | Rapid cooling | Temperature logs |
| Storage | Biological | ≤4°C | Hourly | Adjust temperature | Equipment validation |
| Packaging | Chemical | Metal detection | Each package | Remove/rework | Detector testing |
Good Manufacturing Practices and Sanitation Standards
Good Manufacturing Practices (GMPs) establish baseline sanitary conditions supporting HACCP effectiveness. Sanitation Standard Operating Procedures (SSOPs) define cleaning and sanitizing protocols maintaining hygienic processing environments.
-
Personnel Hygiene Requirements
-
Hand washing: 20-second soap and water protocol
- Frequency: before work, after breaks, after contamination
- Hand sanitizer: 70% alcohol minimum concentration
- Glove usage: change every 2 hours or after contamination
-
Health monitoring: exclude ill employees
- Symptom screening: fever, vomiting, diarrhea
- Return criteria: 24-48 hours symptom-free
- Medical clearance: negative stool cultures for food handlers
-
-
Environmental Sanitation
-
Cleaning protocols: remove visible soil and debris
- Detergent selection: appropriate for soil type
- Contact time: minimum 30 seconds for effectiveness
- Rinse procedures: potable water removal of residues
-
Sanitizing procedures: reduce microbial populations
- Chemical sanitizers: 200 ppm chlorine, 25 ppm quaternary ammonium
- Heat sanitization: 82°C for 10 seconds
- Contact time: minimum 30 seconds chemical contact
-
💡 Master This: Sanitation effectiveness requires 4-log reduction (99.99%) in microbial populations. ATP bioluminescence testing provides real-time verification with <10 RLU indicating adequate cleaning
Supplier Verification and Traceability Systems
Supply chain control extends food safety responsibility to raw material sources and ingredient suppliers. Traceability systems enable rapid product recall and contamination source identification during outbreak investigations.
-
Supplier Approval Programs
-
Facility audits: annual on-site inspections
- HACCP verification: system implementation and effectiveness
- GMP compliance: sanitation and personnel practices
- Testing programs: pathogen and indicator organism monitoring
-
Certificate of Analysis (COA): batch-specific testing results
- Microbiological criteria: pathogen absence, indicator limits
- Chemical specifications: pesticide residues, heavy metals
- Physical parameters: foreign material absence
-
-
Traceability Documentation
-
Lot identification: unique codes linking products to sources
- Forward traceability: distribution records to customers
- Backward traceability: ingredient sources and suppliers
- Internal traceability: processing records and transformations
-
Record retention: minimum 2 years for most products
- High-risk products: extended retention periods
- Electronic systems: backup and recovery procedures
- Recall simulation: quarterly mock recalls within 2 hours
-
📌 Remember: "TRACE" for supply chain control - Track sources, Record movements, Audit suppliers, Certify quality, Enable rapid recall
Connect these prevention strategies through advanced detection and monitoring technologies to understand how modern food safety systems integrate traditional principles with cutting-edge analytical capabilities.
⚖️ Prevention Protocol Engineering: The Multi-Barrier Defense System
🔗 Technology Integration Nexus: The Smart Safety Ecosystem
Rapid Detection and Molecular Diagnostics
Molecular detection methods reduce pathogen identification from days to hours, enabling real-time decision making and immediate corrective actions. PCR-based systems detect single organisms in complex food matrices with >99% specificity.
-
Real-Time PCR Applications
-
Pathogen detection: 2-4 hour results vs. 24-72 hours culture
- Sensitivity: 1-10 CFU/25g sample detection
- Specificity: >99% accuracy with <1% false positives
- Multiplexing: simultaneous detection of 5-10 pathogens
-
Quantitative analysis: viable cell enumeration
- Dynamic range: 10¹-10⁸ CFU/mL quantification
- Precision: ±0.3 log units reproducibility
- Speed: <30 minutes sample-to-result time
-
-
Next-Generation Sequencing (NGS)
-
Whole genome sequencing: strain-level identification
- Resolution: single nucleotide polymorphism detection
- Outbreak investigation: <24 hours strain comparison
- Source attribution: phylogenetic analysis of contamination routes
-
Metagenomics: total microbiome analysis
- Community profiling: species-level identification
- Functional analysis: virulence gene detection
- Antimicrobial resistance: resistance gene screening
-
| Detection Method | Time to Result | Sensitivity | Specificity | Cost per Test | Applications |
|---|---|---|---|---|---|
| Traditional Culture | 24-72 hours | 10²-10³ CFU/g | >95% | $5-15 | Regulatory compliance |
| Real-Time PCR | 2-4 hours | 1-10 CFU/g | >99% | $15-30 | Rapid screening |
| Isothermal Amplification | 30-60 minutes | 10-100 CFU/g | >98% | $10-20 | Point-of-use testing |
| Immunoassays | 15-30 minutes | 10³-10⁴ CFU/g | 90-95% | $3-8 | Field testing |
| Biosensors | <15 minutes | 10²-10³ CFU/g | 85-95% | $1-5 | Continuous monitoring |
Smart Sensor Networks and IoT Integration
Internet of Things (IoT) sensors create continuous monitoring networks tracking temperature, humidity, pH, and microbial indicators throughout food production and distribution. Wireless sensor networks provide real-time alerts when critical limits are exceeded.
-
Environmental Monitoring Systems
-
Temperature sensors: ±0.1°C accuracy with wireless transmission
- Monitoring frequency: every 1-5 minutes
- Alert thresholds: >4°C for refrigerated products
- Data logging: continuous recording with cloud storage
-
Humidity control: ±2% RH precision monitoring
- Critical limits: <85% RH for mold prevention
- Automated responses: dehumidification system activation
- Trend analysis: predictive maintenance scheduling
-
-
Predictive Analytics and Machine Learning
-
Risk modeling: algorithm-based contamination prediction
- Input variables: temperature, time, pH, water activity
- Output predictions: pathogen growth probability
- Decision support: automated recommendations for interventions
-
Pattern recognition: anomaly detection in sensor data
- Baseline establishment: normal operating ranges
- Deviation alerts: statistical significance thresholds
- Root cause analysis: correlation analysis of multiple variables
-
💡 Master This: Predictive modeling prevents contamination before it occurs - machine learning algorithms analyzing temperature abuse patterns predict pathogen growth with >90% accuracy, enabling proactive interventions
Blockchain Traceability and Supply Chain Transparency
Blockchain technology creates immutable records of food movement from farm to fork, enabling instant traceability and rapid recall execution. Smart contracts automate quality verification and compliance monitoring throughout supply chains.
-
Distributed Ledger Applications
-
Transaction recording: tamper-proof documentation
- Block creation: cryptographic hashing ensures integrity
- Consensus mechanisms: network validation of transactions
- Audit trails: complete history of product movement
-
Smart contract automation: conditional execution of agreements
- Quality gates: automatic approval based on test results
- Payment triggers: performance-based compensation
- Compliance verification: regulatory requirement checking
-
-
Supply Chain Integration
-
Multi-stakeholder platforms: farmer to retailer connectivity
- Data standardization: common formats for information exchange
- Permission management: role-based access to sensitive data
- Interoperability: cross-platform communication protocols
-
Consumer transparency: QR code access to product history
- Origin verification: farm location and production date
- Quality certifications: organic, safety standards compliance
- Recall notifications: immediate consumer alerts
-
📌 Remember: "SMART" technology integration - Sensors monitor continuously, Machine learning predicts risks, Automation responds instantly, Rapid detection identifies threats, Traceability enables quick response
Connect these technology integration principles through comprehensive mastery frameworks to understand how modern food safety professionals synthesize traditional knowledge with cutting-edge tools for optimal protection outcomes.
🔗 Technology Integration Nexus: The Smart Safety Ecosystem
🎯 Clinical Mastery Command Center: The Expert Practitioner's Arsenal
Essential Clinical Arsenal - Rapid Reference Tools
⭐ Master This: Temperature-Time Relationships - Every 10°C increase doubles microbial growth rates; 2-hour rule at danger zone (4-60°C) prevents infectious dose accumulation
- Critical Temperature Thresholds
- Refrigeration: ≤4°C (pathogen growth inhibition)
- Cooking: 71°C × 15 seconds (vegetative cell destruction)
- Hot holding: ≥60°C (growth prevention)
- Reheating: 74°C (spore activation prevention)
💡 Clinical Pearl: pH-Pathogen Matrix - pH <4.6 prevents C. botulinum growth; pH <4.0 inhibits most pathogens; pH <3.5 provides multi-log reduction
- Rapid Pathogen Recognition
- <6 hours onset: Preformed toxins (Staph, B. cereus)
- 6-24 hours: Bacterial multiplication (C. perfringens)
- >24 hours: Invasive pathogens (Salmonella, Campylobacter)
📌 Remember: "HACCP-TRACE-SMART" - Hazard analysis, Assess risks, Control points, Correct deviations, Prevent recurrence; Track products, Record data, Audit systems, Certify suppliers, Enable recalls; Sensors, Modeling, Automation, Rapid detection, Technology
| Risk Category | Immediate Actions | Investigation Priority | Prevention Focus | Technology Tools |
|---|---|---|---|---|
| High Risk | Product recall, facility closure | <24 hours | Source elimination | Real-time PCR, WGS |
| Moderate Risk | Product hold, enhanced testing | 24-72 hours | Process improvement | Rapid tests, sensors |
| Low Risk | Increased monitoring | <1 week | System optimization | Trend analysis |
⭐ Clinical Pearl: Outbreak Signatures - Attack rates >50% with <6 hour onset indicate preformed toxins; Secondary transmission >30% suggests viral etiology
- Food-Pathogen Associations
- Poultry: Salmonella (25% prevalence), Campylobacter (>50%)
- Ground beef: E. coli O157:H7 (<1% but high severity)
- Dairy: Listeria (ready-to-eat), Staphylococcus (temperature abuse)
- Produce: Norovirus (contaminated water), Parasites (imported)
💡 Master This: Risk Assessment Integration - Combine hazard severity × exposure probability × population vulnerability = Risk Priority Number for resource allocation
Advanced Integration Protocols
- Multi-System Risk Analysis
- Ingredient risk: supplier history, geographic origin
- Process risk: critical control point effectiveness
- Environmental risk: facility design, sanitation adequacy
- Human risk: training level, compliance culture
📌 Remember: "PREVENT" - Predict risks, Recognize patterns, Evaluate evidence, Verify controls, Enforce standards, Navigate technology, Train continuously
Food safety mastery represents the synthesis of microbiological knowledge, epidemiological thinking, technological capability, and clinical judgment into comprehensive protection systems that safeguard human health through every stage of food production and consumption.
🎯 Clinical Mastery Command Center: The Expert Practitioner's Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app























