Geriatrics

On this page
🧬 The Aging Blueprint: Cellular Foundations of Geriatric Medicine
Aging transforms every physiological system through predictable cellular and molecular mechanisms, creating unique clinical patterns that demand specialized recognition and management strategies. You'll master how senescence reshapes organ function, learn to distinguish normal aging from pathology, and develop systematic approaches to optimize treatment in older adults where polypharmacy, frailty, and multi-system interactions complicate every decision. This foundation equips you to deliver precision care for the fastest-growing patient population, where standard protocols often fail and clinical expertise makes the difference between independence and decline.

Primary Aging Theories and Mechanisms
-
Programmed Aging Theory
- Genetic clock hypothesis: 50-70 cell divisions maximum (Hayflick limit)
- Telomere shortening: 50-200 base pairs lost per division
- Hormonal regulation: ↓25% growth hormone after age 40
- IGF-1 levels decline 1-2% annually after age 30
- Thyroid function decreases 6-10% per decade
- Sex hormones drop 1-3% yearly after menopause/andropause
-
Damage Accumulation Theory
- Free radical damage: 10,000+ DNA hits per cell daily
- Protein misfolding increases 2-3 fold by age 80
- Lipofuscin accumulation: 0.3% cell volume per decade
- Particularly prominent in cardiac and neural tissue
- Correlates with functional decline in affected organs
📌 Remember: AGING - Accumulated damage, Genetic programming, Inflammation, Neural decline, Growth factor reduction

Cellular Hallmarks of Aging
| Hallmark | Mechanism | Timeline | Clinical Impact | Intervention Target |
|---|---|---|---|---|
| Genomic Instability | DNA repair ↓40% | Age 50+ | Cancer risk ↑300% | Antioxidants, DNA repair enhancers |
| Telomere Attrition | 50-200bp loss/division | Lifelong | Cellular senescence | Telomerase activators |
| Epigenetic Alterations | Methylation changes 15% | Age 40+ | Gene expression shifts | Epigenetic modulators |
| Proteostasis Loss | Chaperone function ↓30% | Age 60+ | Protein aggregation | Autophagy enhancers |
| Nutrient Sensing Dysregulation | mTOR hyperactivation 200% | Age 45+ | Metabolic dysfunction | Caloric restriction mimetics |
| Mitochondrial Dysfunction | ATP production ↓25% | Age 50+ | Energy deficit | Mitochondrial boosters |
Inflammatory Aging (Inflammaging)
The chronic low-grade inflammatory state characterizing aging drives multiple geriatric syndromes:
-
Cytokine Profile Changes
- IL-6 levels increase 2-4 fold after age 70
- TNF-α elevation correlates with 15% increased frailty risk
- CRP baseline rises 50-100% in healthy elderly
- Values >3.0 mg/L predict cardiovascular events
- Correlates with cognitive decline progression
-
Cellular Senescence Burden
- Senescent cells accumulate at 0.5-2% annually
- SASP (senescence-associated secretory phenotype) affects neighboring cells
- Senolytic interventions show 20-30% improvement in healthspan
💡 Master This: Inflammaging explains why elderly patients develop multi-organ dysfunction patterns - chronic IL-6 elevation simultaneously affects cardiovascular, cognitive, and musculoskeletal systems, creating the interconnected geriatric syndromes.
Understanding these aging fundamentals transforms your approach to geriatric assessment, revealing why comprehensive evaluation must address cellular-level changes that manifest as complex clinical presentations requiring integrated management strategies.
🧬 The Aging Blueprint: Cellular Foundations of Geriatric Medicine
⚙️ The Aging Engine: Physiological System Decline Patterns

Cardiovascular Aging Cascade
-
Structural Cardiovascular Changes
- Left ventricular wall thickness increases 25-30% by age 80
- Arterial compliance decreases 1% annually after age 30
- Pulse wave velocity increases 10 cm/sec per decade
- Normal young adult: 4-6 m/sec
- Elderly (>70): 12-15 m/sec
- Values >12 m/sec predict cardiovascular events
-
Functional Cardiac Decline
- Maximum heart rate: 220 - age (beats/minute)
- Cardiac output decreases 1% annually after age 30
- Diastolic dysfunction present in 50% of adults >65
- E/A ratio reversal: <0.8 indicates impaired relaxation
- Deceleration time >240 msec suggests stiffness
📌 Remember: HEART aging - Hypertrophy, Elasticity loss, Arterial stiffening, Relaxation impairment, Threshold changes
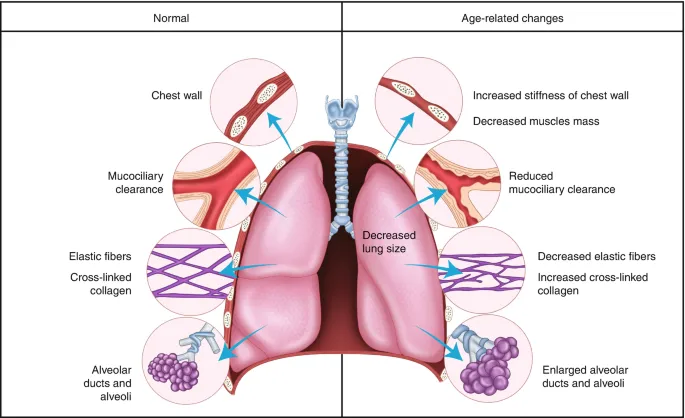
Respiratory System Deterioration
| Parameter | Age 30 Baseline | Age 70 Value | % Decline | Clinical Threshold |
|---|---|---|---|---|
| FEV1 | 4.0L | 2.8L | 30% | <2.5L impairs ADLs |
| Vital Capacity | 5.0L | 3.5L | 30% | <3.0L increases pneumonia risk |
| Residual Volume | 1.2L | 1.8L | ↑50% | >2.0L suggests air trapping |
| Chest Wall Compliance | 100% | 65% | 35% | <60% limits cough effectiveness |
| Alveolar Surface Area | 70m² | 50m² | 29% | <45m² affects gas exchange |
- Alveolar wall destruction: 1-2% surface area loss annually
- Chest wall stiffening reduces compliance 35% by age 70
- Respiratory muscle strength declines 20% per decade after 50
- Diaphragmatic strength particularly affected
- Accessory muscle compensation increases work of breathing
⭐ Clinical Pearl: Elderly patients require 20-30% longer recovery time from respiratory infections due to impaired mucociliary clearance (50% reduction) and decreased cough reflex sensitivity.
Neurological System Aging
-
Structural Brain Changes
- Brain volume decreases 0.5% annually after age 60
- Ventricular enlargement: 3-4% yearly expansion
- White matter lesions present in 90% of adults >65
- Periventricular lesions affect executive function
- Deep white matter changes correlate with processing speed
-
Neurotransmitter System Decline
- Dopamine receptors decrease 6-10% per decade
- Acetylcholine synthesis reduces 15-20% by age 80
- GABA-ergic inhibition weakens 25% in frontal cortex
- Explains increased susceptibility to delirium
- Contributes to sleep architecture changes
💡 Master This: The "cognitive reserve" concept explains why patients with higher education tolerate 30-40% more brain pathology before showing clinical symptoms - understanding this guides realistic prognosis discussions.

These physiological aging patterns create the foundation for understanding why geriatric patients develop characteristic syndrome clusters and require age-adjusted treatment approaches that account for predictable system vulnerabilities.
⚙️ The Aging Engine: Physiological System Decline Patterns
🎯 The Geriatric Recognition Matrix: Clinical Pattern Mastery
Atypical Presentation Recognition Framework
-
Infection Presentations in Elderly
- Classic fever present in only 30-40% of elderly with serious infections
- Delirium as primary manifestation in 60% of UTIs in patients >80
- Falls may be the only sign of pneumonia in 25% of cases
- Temperature elevation <1°C still significant
- White count may remain normal in 40% of elderly infections
- Functional decline often precedes other symptoms by 24-48 hours
-
Cardiac Event Recognition
- Silent MI occurs in 40-60% of elderly patients
- Dyspnea more common than chest pain (70% vs 50%)
- Cognitive changes may be primary presentation in 20%
- New confusion in previously stable patient = rule out MI
- Fatigue and weakness often predominate over pain
📌 Remember: GERIATRIC presentations - General decline, Emotional changes, Reduced function, Incontinence, Atypical symptoms, Thinking problems, Recurrent falls, Immobility, Confusion
Medication-Related Pattern Recognition
| Clinical Presentation | Suspect Drug Class | Prevalence in >65 | Key Discriminators |
|---|---|---|---|
| New-onset confusion | Anticholinergics | 15-25% | Dry mouth, constipation, urinary retention |
| Recurrent falls | Psychotropics | 20-30% | Sedation, orthostasis, gait instability |
| Functional decline | Polypharmacy (>5 drugs) | 40-50% | Gradual onset, multiple systems affected |
| Delirium | Benzodiazepines | 10-15% | Paradoxical agitation, sleep-wake cycle disruption |
| Bradycardia/syncope | Beta-blockers/CCBs | 8-12% | Exercise intolerance, cold extremities |
- Beers Criteria medications used in 40% of community-dwelling elderly
- Drug-drug interactions present in 20% of patients taking >5 medications
- Inappropriate dosing occurs in 25% due to age-related pharmacokinetic changes
- Creatinine clearance overestimated in 60% of elderly
- Hepatic metabolism reduced 30-40% by age 80
⭐ Clinical Pearl: Any new symptom in an elderly patient taking >5 medications should trigger medication review before extensive workup - 30-40% of geriatric complaints are medication-related.
Geriatric Syndrome Recognition Patterns
-
Falls Pattern Recognition
- Multifactorial in 85% of cases (average 4-5 risk factors)
- Medication-related in 60% (sedatives, antihypertensives, diuretics)
- Environmental factors contribute to 30-50%
- Poor lighting, loose rugs, bathroom hazards
- Home safety assessment reduces falls by 20-30%
-
Frailty Identification Patterns
- Fried Criteria: Weight loss, exhaustion, low activity, slow gait, weak grip
- Frailty Index: Accumulation of 30+ deficits
- Clinical Frailty Scale: 9-point visual assessment tool
- Scores 1-3: Fit to managing well
- Scores 4-6: Vulnerable to mildly frail
- Scores 7-9: Severely frail to terminally ill
💡 Master This: Geriatric syndromes share common risk factors - identifying one syndrome should trigger screening for others, as 70% of frail elderly have 2+ concurrent syndromes.
These recognition patterns enable rapid identification of age-specific presentations and guide appropriate comprehensive assessment rather than narrow diagnostic pursuits that miss the multifactorial nature of geriatric conditions.
🎯 The Geriatric Recognition Matrix: Clinical Pattern Mastery
🔍 The Differential Decoder: Systematic Geriatric Discrimination
Delirium vs Dementia vs Depression Discrimination Matrix
| Feature | Delirium | Dementia | Depression |
|---|---|---|---|
| Onset | Hours to days | Months to years | Weeks to months |
| Course | Fluctuating | Progressive decline | Episodic/persistent |
| Attention | Severely impaired | Preserved early | Mildly impaired |
| Consciousness | Altered | Clear | Clear |
| Hallucinations | 60-70% visual | 20-30% late stage | 5-10% auditory |
| Reversibility | 80-90% if treated | Irreversible | 70-80% treatable |
- CAM (Confusion Assessment Method): 94% sensitivity, 89% specificity
- 4AT Score: Rapid 2-minute screening tool
- Richmond Agitation-Sedation Scale: Quantifies severity
- Hyperactive delirium: 25% of cases, easily recognized
- Hypoactive delirium: 50% of cases, often missed
- Mixed type: 25% of cases, alternating patterns
- Dementia Subtype Discrimination
- Alzheimer's Disease: 60-70% of dementia cases
- Memory loss predominant early symptom
- Gradual onset over 2-3 years
- Vascular Dementia: 15-20% of cases
- Stepwise decline pattern
- Executive dysfunction prominent
- Lewy Body Dementia: 10-15% of cases
- Visual hallucinations in 80%
- Parkinsonism features present
- Alzheimer's Disease: 60-70% of dementia cases
📌 Remember: DELIRIUM features - Disturbed consciousness, Emotional lability, Language incoherent, Inattention, Rapid onset, Illusions/hallucinations, Unstable course, Memory impaired
Heart Failure Phenotype Discrimination
| HF Type | Prevalence >65 | Key Features | Treatment Response | Prognosis |
|---|---|---|---|---|
| HFpEF | 60-70% | HTN, DM, obesity | Limited ACE-I benefit | 5-year mortality 50% |
| HFmrEF | 15-20% | Transitional state | Moderate GDMT response | 5-year mortality 45% |
| HFrEF | 15-25% | CAD, cardiomyopathy | Strong GDMT benefit | 5-year mortality 40% |
- H2FPEF Score: 9-point clinical prediction tool
- Elevated BNP despite preserved EF: >100 pg/mL
- E/e' ratio >15 indicates elevated filling pressures
- Diastolic stress testing reveals exercise intolerance
- Left atrial enlargement present in 80%
⭐ Clinical Pearl: HFpEF accounts for 60-70% of heart failure in patients >75 years, but standard HF medications show limited benefit - focus on comorbidity management and symptom control.
Syncope Etiology Discrimination Framework
-
Cardiovascular Syncope (25-30% in elderly)
- Structural heart disease: AS, HCM, PE
- Arrhythmic: VT, complete heart block, sick sinus
- Orthostatic hypotension: 20 mmHg systolic drop
- Medication-induced in 40% of cases
- Dehydration contributes to 30%
-
Neurally-Mediated Syncope (15-20% in elderly)
- Carotid sinus hypersensitivity: >3 second pause
- Situational syncope: Cough, micturition, defecation
- Vasovagal response: Less common with aging
-
Unexplained Syncope (30-40% in elderly)
- Implantable loop recorder diagnostic yield: 70%
- Tilt table testing less reliable in elderly
- Electrophysiology study indicated if structural heart disease
💡 Master This: Elderly syncope requires aggressive evaluation - 30-day mortality is 8-10% in patients >65 years with unexplained syncope, compared to <1% in younger patients.
These discrimination frameworks enable precise diagnosis in elderly patients where overlapping presentations can lead to misdiagnosis and inappropriate treatment cascades that worsen outcomes in this vulnerable population.
🔍 The Differential Decoder: Systematic Geriatric Discrimination
⚖️ The Treatment Optimization Engine: Evidence-Based Geriatric Therapeutics
Age-Adjusted Pharmacotherapy Algorithm
-
Renal Dose Adjustment Principles
- Cockcroft-Gault equation overestimates function in 60% of elderly
- CKD-EPI equation more accurate for GFR >60 mL/min/1.73m²
- Serum creatinine normal despite 50% GFR reduction
- Age-related muscle mass loss masks kidney dysfunction
- Cystatin C more reliable marker in elderly
-
High-Risk Medication Dosing Adjustments
- Digoxin: Reduce dose 50%, target level 0.8-1.2 ng/mL
- Warfarin: Start 2.5 mg daily (vs 5 mg in younger patients)
- ACE inhibitors: Begin 25-50% standard dose
- Monitor for hyperkalemia (risk increased 3-fold)
- Acute kidney injury occurs in 15-20% of elderly
📌 Remember: START LOW principles - Start low dose, Titrate slowly, Assess response, Review regularly, Taper when stopping, Limit polypharmacy, Optimize timing, Watch for interactions
Cardiovascular Treatment Optimization
| Condition | Standard Dose | Elderly Dose | Monitoring Parameter | Target Goal |
|---|---|---|---|---|
| Hypertension | Lisinopril 10mg | 5mg start | BP, K+, Cr | <140/90 (>80 years) |
| Heart Failure | Metoprolol 50mg BID | 25mg BID start | HR, BP, symptoms | HR 60-70 |
| Atrial Fibrillation | Warfarin 5mg | 2.5mg start | INR, bleeding | INR 2.0-2.5 |
| CAD | Atorvastatin 40mg | 20mg start | LFTs, CK, symptoms | LDL <100 |
| DVT/PE | Rivaroxaban 20mg | 15mg if CrCl 30-50 | Bleeding, renal function | No dose adjustment |
- DOAC preferred over warfarin in patients >75 years
- Bleeding risk increases 2-3 fold after age 75
- HAS-BLED score >3 indicates high bleeding risk
- Apixaban lowest bleeding risk among DOACs
- Dabigatran requires dose reduction if CrCl 15-30
⭐ Clinical Pearl: Statin therapy in patients >80 years reduces cardiovascular events by 20% but increases diabetes risk by 15% - individualize based on life expectancy and functional status.
Deprescribing Systematic Approach
-
Deprescribing Priority Targets
- Proton pump inhibitors: Taper after 8-12 weeks unless high-risk
- Benzodiazepines: Reduce 25% weekly to prevent withdrawal
- Anticholinergics: Discontinue immediately if cognitive impairment
- Anticholinergic burden score >3 increases dementia risk 50%
- Common culprits: diphenhydramine, oxybutynin, amitriptyline
-
Successful Deprescribing Outcomes
- Falls reduction: 20-30% decrease with psychotropic withdrawal
- Cognitive improvement: 15-25% enhancement after anticholinergic removal
- Mortality benefit: 10-15% reduction with inappropriate medication cessation
- Number needed to treat: 8-12 patients for one prevented adverse event
💡 Master This: Deprescribing is as important as prescribing in elderly patients - systematic medication review every 6 months prevents 40% of medication-related hospitalizations and improves quality of life scores by 20-30%.
These evidence-based treatment optimization strategies enable safe and effective therapeutics in elderly patients while minimizing the iatrogenic complications that disproportionately affect this vulnerable population.
⚖️ The Treatment Optimization Engine: Evidence-Based Geriatric Therapeutics
🔗 The Geriatric Integration Network: Multi-System Orchestration
Biopsychosocial Integration Framework
-
Biological Domain Interactions
- Cardiovascular-Renal axis: Heart failure affects 60% of CKD patients >75
- Metabolic-Cognitive coupling: Diabetes increases dementia risk 2-fold
- Musculoskeletal-Cardiovascular link: Sarcopenia correlates with 40% increased cardiac mortality
- Muscle mass loss >20% predicts heart failure progression
- Exercise capacity directly relates to cardiac reserve
-
Psychological-Physical Interconnections
- Depression-Frailty cycle: Depression increases frailty risk 3-fold
- Cognitive-Functional relationship: MMSE <24 predicts ADL dependence
- Pain-Mood-Sleep triangle: Chronic pain affects 50% of elderly
- Sleep disruption in 80% of chronic pain patients
- Depression prevalence 40% in persistent pain conditions
📌 Remember: COMPLEX elderly care - Cognitive assessment, Optimize function, Medication review, Psychosocial support, Living environment, Exercise prescription, X-ray social determinants
Geriatric Syndrome Clustering Patterns
| Primary Syndrome | Co-occurring Syndromes | Prevalence | Shared Risk Factors |
|---|---|---|---|
| Frailty | Falls (70%), Cognitive impairment (50%) | 15-20% community | Inflammation, sarcopenia, polypharmacy |
| Falls | Incontinence (60%), Depression (40%) | 30-35% annually | Medications, mobility, environment |
| Delirium | Functional decline (80%), Pressure ulcers (30%) | 15-25% hospitalized | Acute illness, medications, immobility |
| Incontinence | Cognitive impairment (45%), Social isolation (35%) | 25-30% women | Mobility, cognition, medications |
- Early mobility protocols reduce delirium by 40%
- Medication reconciliation prevents 25% of adverse drug events
- Comprehensive discharge planning decreases readmissions 20%
- Multidisciplinary team involvement essential
- 72-hour post-discharge contact reduces complications
⭐ Clinical Pearl: Geriatric syndromes cluster in 70% of frail elderly - identifying one syndrome should trigger systematic screening for others using validated assessment tools.

Advanced Care Integration Models
-
Transitional Care Innovations
- Geriatric Emergency Departments: 30% reduction in readmissions
- Hospital at Home programs: 25% cost reduction, improved satisfaction
- Acute Care for Elders (ACE) units: 15% shorter stays, better function
- Specialized nursing protocols
- Environmental modifications
- Early discharge planning
-
Technology-Enhanced Integration
- Remote monitoring reduces hospitalizations 20-30%
- Telemedicine improves access for 40% of homebound elderly
- Electronic health records with geriatric modules enhance care coordination
- Automated medication interaction checking
- Fall risk stratification algorithms
- Cognitive screening reminders
💡 Master This: Successful geriatric care requires team-based approaches - studies show 30-40% better outcomes when physicians, nurses, pharmacists, social workers, and therapists collaborate using structured protocols.
Cutting-Edge Geriatric Research Integration
-
Precision Geriatrics Emerging
- Genetic testing for medication metabolism: CYP2D6 variants affect 25% of elderly
- Biomarker-guided therapy: NT-proBNP levels guide heart failure management
- Frailty phenotyping using wearable technology: Gait speed predicts mortality
- <0.8 m/sec indicates high mortality risk
- Grip strength <16 kg (women), <27 kg (men) predicts disability
-
Innovative Intervention Strategies
- Prehabilitation before surgery reduces complications 40%
- Multimodal exercise programs improve cognition 15-20%
- Social prescribing addresses loneliness affecting 35% of elderly
- Community engagement reduces healthcare utilization 25%
- Peer support programs improve medication adherence 30%

These integration frameworks enable comprehensive care that addresses the complex, interconnected needs of elderly patients, moving beyond single-disease management to holistic approaches that optimize function, independence, and quality of life.
🔗 The Geriatric Integration Network: Multi-System Orchestration
🎯 The Geriatric Mastery Arsenal: Clinical Excellence Toolkit
Essential Clinical Assessment Arsenal
| Tool | Purpose | Time Required | Sensitivity/Specificity | Clinical Threshold |
|---|---|---|---|---|
| Mini-Cog | Cognitive screening | 3 minutes | 76%/89% | <3/5 abnormal |
| Timed Up & Go | Fall risk assessment | 2 minutes | 87%/87% | >12 seconds high risk |
| FRAIL Scale | Frailty screening | 1 minute | 94%/86% | ≥3/5 frail |
| PHQ-2 | Depression screening | 1 minute | 83%/92% | ≥3/6 positive |
| AUDIT-C | Alcohol screening | 30 seconds | 95%/78% | ≥4 (men), ≥3 (women) |
- Clock Drawing Test: 30-second screening, 85% sensitivity for dementia
- Montreal Cognitive Assessment (MoCA): 10-minute comprehensive evaluation
- AD8 Questionnaire: 2-minute informant-based screening
- ≥2 positive responses suggest cognitive impairment
- Particularly useful when patient cannot cooperate
- Functional Status Evaluation
- Katz ADL Scale: 6 basic activities, predicts nursing home placement
- Lawton IADL Scale: 8 instrumental activities, detects early decline
- Short Physical Performance Battery: 4-meter walk, chair stands, balance
- Scores <8/12 predict disability and mortality
- Gait speed <0.8 m/sec indicates high mortality risk
📌 Remember: GERIATRIC toolkit - Gait assessment, Emotional screening, Risk stratification, IADL evaluation, Alcohol screening, Timed tests, Rapid cognition, Instrument selection, Clinical thresholds
High-Yield Clinical Pearls Compendium
-
Medication Management Pearls
- "Start low, go slow": Begin at 25-50% standard dose in patients >75
- Anticholinergic burden: Score >3 increases dementia risk 50%
- Polypharmacy threshold: >5 medications increases adverse events exponentially
- Drug-drug interactions occur in 40% of patients taking >8 medications
- Potentially inappropriate medications present in 50% of elderly
-
Cardiovascular Optimization Pearls
- Blood pressure targets: <140/90 in patients >80 years (less aggressive)
- Statin therapy: Benefits persist until age 85, then individualize
- Anticoagulation: DOAC preferred over warfarin in patients >75
- Bleeding risk doubles every 10 years after age 65
- Time in therapeutic range <60% with warfarin suggests DOAC switch
⭐ Clinical Pearl: Orthostatic hypotension affects 30% of elderly and increases fall risk 2.4-fold - measure BP supine and after 1 and 3 minutes standing in all geriatric assessments.
Rapid Decision-Making Frameworks
-
Emergency Department Geriatric Protocols
- Silver Alert criteria: Age >65 + cognitive impairment + missing >24 hours
- Geriatric ED assessment: ISAR score predicts 6-month outcomes
- Discharge planning: 72-hour follow-up reduces readmissions 25%
- Medication reconciliation essential
- Home safety evaluation recommended
-
Hospitalization Optimization Strategies
- HOSPITAL score: Predicts 30-day readmission risk
- Mobility protocols: Early ambulation reduces delirium 40%
- Sleep hygiene: Quiet hours and lighting protocols improve outcomes
- Avoid tethering: Minimize catheters, monitors, restraints
- Family involvement reduces confusion and agitation
💡 Master This: Comprehensive Geriatric Assessment (CGA) improves outcomes in 85% of elderly patients when implemented systematically - the number needed to treat is 17 to prevent one death or nursing home admission.
Evidence-Based Quick Reference
-
Prognosis Estimation Tools
- ePrognosis calculators: 1, 4, and 10-year mortality predictions
- Palliative Performance Scale: Functional decline trajectory
- Surprise Question: "Would you be surprised if this patient died in the next year?"
- Positive response indicates need for advance care planning
- Triggers goals of care discussions
-
Preventive Care Guidelines (Age-Adjusted)
- Mammography: Continue until age 75 if life expectancy >10 years
- Colonoscopy: Stop at age 85 or life expectancy <10 years
- Bone density: Screen women >65, men >70
- FRAX score guides treatment decisions
- 10-year fracture risk >20% warrants intervention
This comprehensive toolkit enables rapid, evidence-based decision-making in geriatric care, ensuring optimal outcomes while avoiding the common pitfalls that lead to iatrogenic complications in elderly patients.
🎯 The Geriatric Mastery Arsenal: Clinical Excellence Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























