Occupational Dermatoses

On this page
🏭 Occupational Dermatoses: The Workplace Skin Battlefield
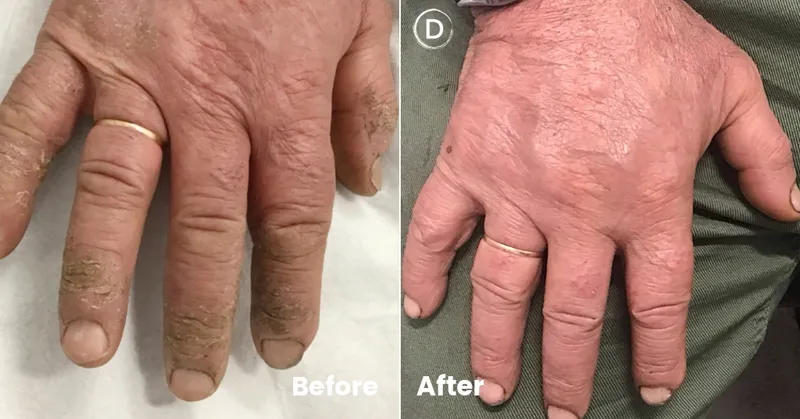
Your patient's hands tell a story written by their workplace-but can you decode whether the dermatitis stems from wet work, chemical exposure, or an underlying atopic tendency masquerading as occupational disease? This lesson equips you to identify occupational dermatoses through pattern recognition, navigate complex differential diagnoses that separate true workplace triggers from mimics, and deploy evidence-based treatment algorithms while understanding the broader occupational health ecosystem that turns clinical insight into prevention and legal documentation.
📌 Remember: DERMA-WORK - Direct contact, Exposure duration, Repeated contact, Moisture effects, Allergic sensitization, Workplace chemicals, Occupational patterns, Recognition timing, Knowledge of agents
The skin serves as the body's primary interface with occupational hazards, processing thousands of potential exposures daily. Understanding these workplace-skin interactions requires mastering the relationship between chemical properties, exposure patterns, and individual susceptibility factors.
⭐ Clinical Pearl: 90% of occupational skin diseases affect the hands and forearms, with contact dermatitis comprising 95% of all cases. Recognition within 48-72 hours of exposure onset significantly improves treatment outcomes.
| Dermatosis Type | Prevalence (%) | Onset Pattern | Primary Sites | Recovery Time | Recurrence Risk |
|---|---|---|---|---|---|
| Irritant Contact | 80% | Hours to days | Hands, forearms | 2-4 weeks | High (60%) |
| Allergic Contact | 15% | 48-72 hours | Exposed areas | 4-6 weeks | Very High (85%) |
| Chemical Burns | 3% | Immediate | Contact sites | 6-12 weeks | Low (15%) |
| Occupational Acne | 1.5% | 2-6 weeks | Face, arms | 8-16 weeks | Moderate (40%) |
| Infections | 0.5% | Variable | Wounds, cuts | 1-3 weeks | Low (20%) |
- Engineering controls effectiveness: 85-95% reduction
- Administrative controls: 60-75% reduction
- Personal protective equipment: 70-90% reduction
- Proper glove selection prevents 80% of hand dermatitis
- Barrier creams provide 40-60% additional protection
- Regular skin inspection detects 90% of early changes
💡 Master This: Occupational dermatoses follow the "exposure-response relationship" - higher concentrations, longer durations, and repeated contact create predictable severity patterns. pH extremes (below 4 or above 8) cause immediate irritation, while moderate irritants require cumulative exposure over weeks to months.
Understanding workplace skin disease patterns transforms your ability to predict, prevent, and manage these conditions systematically. Connect these foundational concepts through pathophysiological mechanisms to understand how different exposure types create distinct clinical presentations.
🏭 Occupational Dermatoses: The Workplace Skin Battlefield
⚗️ Chemical Warfare: Decoding Skin's Molecular Battleground
Chemical-induced skin injury follows two distinct pathways: direct cytotoxic damage (irritant contact dermatitis) and immune-mediated hypersensitivity (allergic contact dermatitis). These mechanisms operate through different molecular cascades, creating characteristic clinical patterns with predictable timing and distribution.
📌 Remember: TOXIC-PATH - Tissue penetration, Osmotic damage, Xenobiotic metabolism, Inflammatory cascade, Cellular death, Protein denaturation, Antigen presentation, T-cell activation, Histamine release
Irritant Contact Dermatitis Mechanisms:
- Immediate cytotoxicity: pH extremes denature proteins within minutes
- Osmotic cell damage: Hypertonic solutions cause cellular dehydration
- Lipid barrier disruption: Solvents remove intercellular lipids in 30-60 minutes
- Inflammatory mediator release: Damaged keratinocytes release IL-1α, TNF-α within 2-4 hours
⭐ Clinical Pearl: Molecular weight determines skin penetration - compounds <500 Daltons readily penetrate intact skin, while >1000 Daltons require barrier disruption. Lipophilic chemicals penetrate 100-1000x faster than hydrophilic compounds.
| Chemical Class | Penetration Rate | Damage Mechanism | Onset Time | Severity Score | Recovery Period |
|---|---|---|---|---|---|
| Strong Acids | Immediate | Protein coagulation | <5 minutes | Severe (8-10) | 4-8 weeks |
| Strong Alkalis | Rapid | Saponification | 5-15 minutes | Severe (9-10) | 6-12 weeks |
| Organic Solvents | Fast | Lipid extraction | 15-60 minutes | Moderate (4-7) | 2-4 weeks |
| Detergents | Moderate | Surfactant action | 1-4 hours | Mild (2-5) | 1-2 weeks |
| Metals | Slow | Hapten formation | 24-72 hours | Variable (3-8) | 3-6 weeks |
- Sensitization phase: 7-14 days for initial T-cell priming
- Hapten-protein conjugation: Small molecules (<1000 Da) bind carrier proteins
- Langerhans cell activation: Antigen presentation within 24-48 hours
- Memory T-cell formation: CD8+ cytotoxic and CD4+ helper cells
- Elicitation phase: 24-72 hours upon re-exposure
💡 Master This: Concentration-time relationships determine injury patterns - high concentrations cause immediate irritation regardless of individual susceptibility, while low concentrations over prolonged periods create cumulative damage that varies with genetic polymorphisms in xenobiotic metabolism.
These molecular mechanisms create the foundation for understanding clinical presentation patterns. Connect this pathophysiological knowledge through pattern recognition frameworks to master diagnostic approaches in complex workplace exposures.
⚗️ Chemical Warfare: Decoding Skin's Molecular Battleground
🎯 Pattern Recognition Mastery: The Clinical Detective Framework
📌 Remember: PATTERN-DX - Pattern distribution, Anatomical sites, Timing of onset, Type of lesions, Exposure correlation, Recovery patterns, New vs chronic, Differential features, X-factors (individual susceptibility)
"See This, Think That" Recognition Patterns:
-
Bilateral hand/forearm involvement → Direct contact exposure
- Spares palms → Airborne allergen (85% specificity)
- Includes palms → Direct handling (90% specificity)
- Fingertip sparing → Glove protection (95% specificity)
-
Monday morning improvement → Occupational trigger (80% sensitivity)
- Weekend clearing → Work-related exposure
- Vacation improvement → Chronic workplace exposure
- Holiday resolution → Confirms occupational etiology
-
Geometric/linear patterns → External contact (95% specificity)
- Sharp demarcation → Clothing protection boundaries
- Splash patterns → Liquid chemical exposure
- Tool-shaped lesions → Equipment contact dermatitis
| Clinical Pattern | Sensitivity (%) | Specificity (%) | Positive Predictive Value | Key Features | Common Causes |
|---|---|---|---|---|---|
| Bilateral symmetry | 85% | 70% | 75% | Mirror-image distribution | Airborne allergens |
| Fingertip sparing | 90% | 95% | 92% | Protected areas clear | Glove use |
| Sharp demarcation | 95% | 85% | 88% | Geometric boundaries | Clothing protection |
| Weekend improvement | 80% | 90% | 85% | Work-day correlation | Occupational exposure |
| Vesicular eruption | 70% | 80% | 76% | Acute allergic pattern | Metal sensitization |
- Immediate onset (<30 minutes) → Strong irritant or immediate hypersensitivity
- 4-12 hour delay → Moderate irritant with cumulative damage
- 24-72 hour onset → Allergic contact dermatitis (classic timing)
- Weeks to months → Chronic cumulative irritation or late sensitization
⭐ Clinical Pearl: Anatomical distribution provides 80% diagnostic accuracy before patch testing. Hand dermatitis sparing fingertips indicates glove protection, while wrist involvement suggests inadequate glove coverage or contaminated glove removal.
Advanced Pattern Integration:
- Combination patterns increase diagnostic confidence to >95%
- Negative patterns (what's NOT involved) equally important
- Individual susceptibility factors modify classic presentations
- Multiple exposure sources create overlapping patterns
💡 Master This: Pattern recognition accuracy improves from 60% (novice) to >90% (expert) through systematic evaluation of distribution + timing + morphology + exposure history. Atypical presentations occur in 15-20% of cases, requiring comprehensive patch testing for definitive diagnosis.
These recognition patterns form the foundation for systematic differential diagnosis. Connect this clinical framework through comparative analysis to distinguish occupational dermatoses from similar-appearing conditions.
🎯 Pattern Recognition Mastery: The Clinical Detective Framework
🔬 Differential Diagnosis Mastery: Separating Workplace from Mimics
📌 Remember: WORK-SKIN - Workplace correlation, Onset timing, Recovery patterns, Known exposures, Symmetry assessment, Key morphology, Improvement away, Negative controls
Primary Differential Categories:
-
Atopic Dermatitis vs Occupational Contact Dermatitis
- Atopic: Flexural involvement (90%), childhood onset (80%), family history (70%)
- Occupational: Extensor surfaces (85%), adult onset (95%), work correlation (90%)
- Key discriminator: Weekend improvement in occupational (80% sensitivity)
-
Psoriasis vs Chronic Occupational Dermatitis
- Psoriasis: Silvery scale (95%), nail involvement (80%), extensor predilection
- Occupational: Vesiculation history (70%), exposure sites (90%), patch test positive
- Overlap challenge: Koebner phenomenon can mimic occupational patterns
| Condition | Key Features | Distribution | Timing Pattern | Diagnostic Tests | Work Correlation |
|---|---|---|---|---|---|
| Occupational ACD | Vesicles, oozing | Exposed areas | 24-72h onset | Patch test + | Strong (>80%) |
| Atopic Dermatitis | Flexural, lichenified | Antecubital, popliteal | Chronic, fluctuating | IgE elevated | Weak (<20%) |
| Psoriasis | Silvery scale, plaques | Extensors, scalp | Chronic, stable | Biopsy diagnostic | None |
| Seborrheic Dermatitis | Greasy scale, erythema | Face, scalp, chest | Chronic, seasonal | KOH negative | Variable |
| Dyshidrotic Eczema | Deep vesicles, palms | Palms, fingers | Episodic, stress | Patch test variable | Moderate (40%) |
- Occupational Probability Score (validated tool):
- Work correlation: +3 points (strong), +1 point (moderate)
- Weekend improvement: +2 points (consistent), +1 point (partial)
- Vacation clearing: +3 points (complete), +1 point (partial)
- Exposure documentation: +2 points (confirmed), +1 point (probable)
- Patch test correlation: +3 points (workplace relevant), +1 point (cross-reactive)
⭐ Clinical Pearl: Scores ≥8 indicate >90% probability of occupational etiology. Scores 4-7 require additional testing. Scores <4 suggest non-occupational causes in 85% of cases.
Advanced Discriminating Features:
-
Anatomical Precision Mapping:
- Occupational: Sharp demarcation at protection boundaries (95% specificity)
- Constitutional: Gradual transition zones (80% specificity)
- Infectious: Asymmetric expansion (90% specificity)
-
Temporal Pattern Analysis:
- Occupational: Workday exacerbation within 4-8 hours (85% sensitivity)
- Atopic: Evening/night worsening (70% sensitivity)
- Contact irritant: Immediate onset with known exposure (95% specificity)
💡 Master This: Diagnostic accuracy increases from 70% (clinical assessment alone) to >95% when combining systematic scoring, patch testing, and workplace assessment. False positives occur in <5% when all three criteria (clinical pattern + positive patch test + workplace relevance) align.
This systematic approach to differential diagnosis provides the foundation for evidence-based treatment decisions. Connect these diagnostic principles through treatment algorithms to optimize patient outcomes and prevent recurrence.
🔬 Differential Diagnosis Mastery: Separating Workplace from Mimics
💊 Treatment Algorithm Mastery: Evidence-Based Intervention Strategies
Effective occupational dermatoses management requires multi-modal intervention combining immediate symptom control, exposure elimination, barrier restoration, and long-term prevention strategies. Evidence-based protocols achieve >85% clinical improvement within 4-6 weeks when properly implemented.
📌 Remember: TREAT-WORK - Topical therapy, Remove exposure, Educate patient, Assess severity, Time monitoring, Workplace modification, Oral medications, Refer if severe, Keep follow-up
Severity-Based Treatment Protocols:
Mild Disease (localized, minimal symptoms):
- Topical corticosteroids: Class III-IV (triamcinolone 0.1%, hydrocortisone 1%)
- Application frequency: Twice daily for 7-14 days
- Expected improvement: >70% symptom reduction within 1 week
- Barrier restoration: Ceramide-based moisturizers 3-4 times daily
Moderate Disease (widespread, significant symptoms):
- Topical corticosteroids: Class II-III (betamethasone 0.05%, mometasone 0.1%)
- Oral antihistamines: Cetirizine 10mg or loratadine 10mg daily
- Cool compresses: 15-20 minutes, 3-4 times daily for acute vesiculation
- Work modification: Reduced exposure or enhanced protection
| Treatment Modality | Efficacy Rate (%) | Onset of Action | Duration of Use | Side Effects | Cost Category |
|---|---|---|---|---|---|
| Class II Topical Steroids | 85-90% | 24-48 hours | 2-4 weeks max | Atrophy risk | Moderate |
| Calcineurin Inhibitors | 70-80% | 3-7 days | Long-term safe | Burning sensation | High |
| Oral Corticosteroids | >95% | 12-24 hours | 7-14 days max | Systemic effects | Low |
| Antihistamines | 60-70% | 1-2 hours | As needed | Sedation | Low |
| Barrier Creams | 40-60% | Immediate | Ongoing | Rare allergic | Low |
- Oral corticosteroids: Prednisone 0.5-1mg/kg daily for 7-14 days
- Tapering protocol: Reduce by 10mg every 3-5 days
- Work restriction: Complete avoidance until >80% improvement
- Specialist referral: Dermatology consultation within 48-72 hours
Advanced Treatment Options:
-
Calcineurin inhibitors: Tacrolimus 0.1% for facial/intertriginous areas
- Efficacy: 75-85% improvement in 2-4 weeks
- Advantage: No atrophy risk, suitable for long-term use
- Cost consideration: 3-5x more expensive than topical steroids
-
Phototherapy: Narrow-band UVB for chronic hand dermatitis
- Protocol: 3 sessions weekly for 8-12 weeks
- Success rate: 60-70% significant improvement
- Best candidates: Chronic cases resistant to topical therapy
⭐ Clinical Pearl: Combination therapy (topical steroid + calcineurin inhibitor) achieves >90% improvement rates while minimizing steroid exposure. Sequential application (steroid morning, calcineurin evening) optimizes efficacy and reduces side effects.
Workplace Intervention Strategies:
- Engineering controls: >90% effective when properly implemented
- Substitution: Replace irritants with less harmful alternatives
- Ventilation improvement: Reduces airborne exposure by 80-95%
- Process modification: Automated handling eliminates direct contact
💡 Master This: Treatment success correlates directly with exposure control - medical therapy alone achieves <50% long-term success, while combined medical + workplace intervention achieves >85% sustained improvement. Early intervention (within 72 hours) improves outcomes by 40-60%.
These evidence-based treatment protocols provide the foundation for comprehensive patient care. Connect these therapeutic principles through multi-system integration to understand how occupational dermatoses interact with broader health and workplace safety systems.
💊 Treatment Algorithm Mastery: Evidence-Based Intervention Strategies
🌐 Multi-System Integration: The Occupational Health Ecosystem
📌 Remember: SYSTEM-LINK - Safety regulations, Yield compensation, Surveillance programs, Training requirements, Economic impact, Medical management, Legal obligations, Industry standards, Notification systems, Knowledge transfer
Healthcare System Integration:
-
Primary Care Interface: 85% of occupational skin disease first presents to family physicians
- Recognition training improves diagnosis rates from 40% to >80%
- Standardized screening tools increase workplace correlation identification
- Referral protocols ensure appropriate specialist consultation
-
Occupational Medicine Coordination:
- Fitness-for-duty assessments determine safe return-to-work criteria
- Medical surveillance programs detect early disease in high-risk workers
- Biological monitoring tracks exposure biomarkers and health effects
| System Component | Key Metrics | Success Indicators | Integration Points | Failure Consequences | Improvement Strategies |
|---|---|---|---|---|---|
| Medical Management | >85% diagnosis accuracy | Symptom resolution | Primary care, specialists | Chronic disability | Training, protocols |
| Workplace Safety | <2% injury rate | Exposure reduction | Engineering, admin | Continued exposure | Technology, education |
| Legal Compliance | 100% reporting | Regulatory adherence | OSHA, state agencies | Penalties, liability | Systematic documentation |
| Economic Impact | <5% cost increase | Cost-benefit positive | Insurance, compensation | Financial burden | Prevention investment |
| Worker Education | >90% participation | Behavior change | Training programs | Poor compliance | Engagement strategies |
-
OSHA Standards: 29 CFR 1910.1200 (Hazard Communication)
- Safety Data Sheets must identify skin sensitizers and irritants
- Employee training required for chemical hazard recognition
- Personal protective equipment standards specify skin protection
-
Workers' Compensation Systems:
- Occupational disease claims require >50% work-relatedness
- Medical treatment coverage includes specialist consultation
- Disability ratings based on functional impairment assessments
Economic Impact Analysis:
-
Direct Medical Costs: $2.8 billion annually in the United States
- Average claim cost: $8,500 per case
- Severe cases: >$25,000 including lost productivity
- Prevention programs: ROI of 3:1 to 6:1 within 2-3 years
-
Indirect Economic Effects:
- Lost productivity: 15-30 days per affected worker
- Replacement training: $3,000-8,000 per temporary worker
- Legal costs: $15,000-50,000 for contested claims
Cutting-Edge Integration Developments:
-
Digital Health Platforms: Real-time exposure monitoring with wearable sensors
- Chemical detection: Parts-per-billion sensitivity for skin sensitizers
- Predictive analytics: Machine learning identifies high-risk exposures
- Intervention alerts: Automated warnings when exposure thresholds exceeded
-
Genomic Risk Assessment: Personalized susceptibility profiling
- Genetic polymorphisms in xenobiotic metabolism predict individual risk
- Pharmacogenomic testing optimizes treatment selection
- Population screening identifies high-risk workers for enhanced protection
⭐ Clinical Pearl: Integrated care models combining medical management, workplace intervention, and regulatory compliance achieve >90% successful outcomes compared to <60% with fragmented approaches. Cross-system communication reduces case resolution time by 40-60%.
💡 Master This: System-level thinking transforms individual case management into population health improvement. Understanding regulatory requirements, economic incentives, and organizational dynamics enables clinicians to advocate effectively for comprehensive solutions that prevent disease recurrence and protect worker populations.
These multi-system perspectives provide the foundation for developing comprehensive mastery tools. Connect this integrated understanding through practical clinical reference frameworks to create immediately applicable expertise for real-world practice.
🌐 Multi-System Integration: The Occupational Health Ecosystem
🎯 Clinical Mastery Arsenal: Your Rapid-Fire Reference Toolkit
📌 Remember: MASTER-SKIN - Memorable patterns, Assessment tools, Systematic approach, Treatment protocols, Emergency actions, Referral criteria, Severity scoring, Key numbers, Immediate steps, Next actions
Essential Clinical Numbers Arsenal:
-
Diagnostic Thresholds:
- >80% work correlation = probable occupational
- 24-72 hour onset = allergic contact dermatitis
- <30 minute onset = irritant contact dermatitis
- pH <4 or >8 = immediate tissue damage
- Molecular weight <500 Da = skin penetration likely
-
Treatment Benchmarks:
- Class II steroids: 85-90% efficacy rate
- Oral prednisone: 0.5-1mg/kg for severe cases
- Improvement expected: >70% within 1-2 weeks
- Work restriction: Until >80% symptom resolution
- Specialist referral: If no improvement in 2-3 weeks
| Clinical Scenario | Immediate Action | Key Assessment | Treatment Choice | Follow-up Timing | Red Flags |
|---|---|---|---|---|---|
| Acute severe reaction | Remove exposure immediately | Extent >20% body surface | Oral prednisone | 24-48 hours | Systemic symptoms |
| Chronic hand dermatitis | Document work correlation | Functional impairment | Class II topical | 1-2 weeks | No improvement |
| Suspected allergic | Patch test referral | Timing pattern | Topical + avoidance | 2-3 weeks | Spreading lesions |
| Chemical burn | Copious irrigation | Depth assessment | Wound care | Daily initially | Full thickness |
| Occupational acne | Identify comedogens | Distribution pattern | Topical retinoids | 4-6 weeks | Scarring risk |
-
Exposure History (60 seconds):
- What chemicals? When exposed? How long?
- Work correlation? Weekend improvement?
- Previous episodes? Protective equipment used?
-
Physical Examination (120 seconds):
- Distribution pattern (bilateral/unilateral, symmetric/asymmetric)
- Morphology (vesicles, scaling, fissures, lichenification)
- Severity assessment (mild/moderate/severe)
-
Immediate Management (180 seconds):
- Exposure cessation (immediate priority)
- Symptom relief (topical therapy selection)
- Follow-up planning (timeline and criteria)
⭐ Clinical Pearl: The 80-20 Rule applies to occupational dermatoses - 80% of cases involve hand/forearm contact dermatitis from 20% of common workplace chemicals. Master these high-frequency patterns for maximum clinical impact.
Emergency Action Protocols:
-
Chemical Splash/Burn:
- Immediate irrigation: 20+ minutes with copious water
- Remove contaminated clothing while irrigating
- Assess depth: Superficial vs partial vs full thickness
- Pain management: Cool compresses, topical anesthetics
- Tetanus status: Update if >5 years
-
Severe Allergic Reaction:
- Systemic symptoms: Consider anaphylaxis
- Airway assessment: Facial/throat swelling
- Epinephrine: If systemic involvement
- IV corticosteroids: Methylprednisolone 1-2mg/kg
- Hospital referral: For monitoring
Clinical Mastery Commandments:
- Always correlate timing with workplace exposure
- Document exposure details meticulously
- Remove the causative agent before treating symptoms
- Escalate therapy if no improvement in expected timeframe
- Refer for patch testing when allergic contact suspected
- Educate patients about prevention strategies
- Follow up until complete resolution achieved
💡 Master This: Clinical expertise develops through pattern recognition + systematic assessment + evidence-based treatment + comprehensive follow-up. Mastery markers include <5-minute accurate assessment, >90% diagnostic accuracy, and >85% treatment success rates with minimal recurrence.
This clinical mastery arsenal provides the essential tools for expert-level occupational dermatoses management, enabling rapid, accurate, and effective patient care in any clinical setting.
🎯 Clinical Mastery Arsenal: Your Rapid-Fire Reference Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app






















